Abstract
Organic anion transporting polypeptides (OATPs) mediate the uptake of a broad range of compounds into cells. Substrates for members of the OATP family include bile salts, hormones, and steroid conjugates as well as drugs like the HMG-CoA-reductase inhibitors (statins), cardiac glycosides, anticancer agents like methotrexate, and antibiotics like rifampicin. OATPs are expressed in a variety of different tissues, including intestine, liver, kidney, and brain, suggesting that they play a critical role in drug absorption, distribution, and excretion. The identification and functional characterisation of naturally occurring variations in genes encoding human OATP (SLCO) family members is in the focus of transporter research. As a result of their broad substrate spectrum and their wide tissue distribution, altered transport characteristics or protein localisation can contribute significantly to interindividual variations of drug effects. The analysis of the consequences of genetic variations in genes encoding transport proteins may, therefore, contribute to a better understanding of interindividual differences in drug effects and to individualise treatment regimens with drugs that are substrates for human OATP proteins. In this review, we summarise the current knowledge on genetic variations in transporter genes encoding human OATP family members and their functional consequences analysed by in vitro and in vivo studies.
Similar content being viewed by others
The OATP family of uptake transporters
Uptake transporters belonging to the superfamily of solute carriers (SLC) (Hagenbuch and Meier 2004; Hediger et al. 2004), and efflux pumps belonging to the ATP-binding cassette transporter (ABC transporter) superfamily (Borst and Elferink 2002; Fromm 2004; König et al. 1999; Kruh and Belinsky 2003), have an impact on the absorption, distribution and elimination of drugs. Genes encoding organic anion transporting polypeptides form a large family within this superfamily of solute carriers. Their genes are classified within the solute carrier family SLCO (Hagenbuch and Meier 2004). OATP1A2 (formerly termed OATP or OATP-A) was described in 1995 (Kullak-Ublick et al. 1995) and followed by the discovery of the second member OATP1B1 (formerly termed OATP2, OATP-C, or LST1) (Abe et al. 1999; Hsiang et al. 1999; König et al. 2000a). Today, the human OATP family consists of 11 members (Hagenbuch and Meier 2003; Mikkaichi et al. 2004a) including 10 OATPs and the prostaglandin transporter OATP2A1 (formerly termed PGT). Due to the fact that trivial names for individual proteins do not correspond to the continuous numbering based on the chronology of protein identification, and because many mouse/rat Oatps have no direct human orthologue, Hagenbuch and Meier (Hagenbuch and Meier 2004) introduced a new nomenclature for the OATP family. In this review, we will follow this new nomenclature and designate all proteins and genes according to this denomination.
According to computer based hydropathy analysis, all OATPs share a very similar transmembrane domain organisation, with 12 predicted transmembrane domains and a large 5th extracellular loop (Hagenbuch and Meier 2003). Additional conserved features of all OATP proteins are N-glycosylation sites in the extracellular loops 2 and 5 and the OATP ‘superfamily signature’ at the border between the extracellular loop 3 and transmembrane domain 6 (Hagenbuch and Meier 2003). While most of the OATP proteins are expressed in multiple tissues, OATP1B1 (OATP2 / OATP-C) and OATP1B3 (OATP8) are predominantly if not exclusively expressed in liver (Hsiang et al. 1999; König et al. 2000a,b). OATP1A2 shows highest expression in brain and testis (Kullak-Ublick et al. 1995), whereas OATP2B1 (OATP-B) and OATP4A1 (OATP-E) are ubiquitously expressed in all tissues investigated so far (Hagenbuch and Meier 2003). Almost all OATP family members are localised to the basolateral membrane of polarised cells. OATP1B1, OATP1B3 and OATP2B1 have been localised to the basolateral membrane of human hepatocytes (Hsiang et al. 1999; König et al. 2000a,b), whereas OATP2A1 has been localised to the basolateral membrane of brain endothelial cells (Lee et al. 2005a). Interestingly, in addition to its basolateral localisation in liver and placenta (St-Pierre et al. 2002), OATP2B1 has been detected in the apical membrane of enterocytes (Kobayashi et al. 2003). OATP4A1 (formerly termed OATP-E) is predominantly expressed at the apical surface of the syncytiotrophoblast in placenta (Sato et al. 2003) and, together with OATP1C1 (formerly termed OATP-F) and OATP3A1 (formerly termed OATP-D), in the basolateral plasma membrane of the non-pigmented human ciliary body epithelium (Gao et al. 2005). OATP4C1 has been found to be highly expressed at mRNA level in human kidney (Mikkaichi et al. 2004b) and the rat Oatp4c1 protein has been localised to the basolateral membrane of kidney proximal tubular cells (Mikkaichi et al. 2004b). The expression and subcellular localisation of human OATP5A1 and OATP6A1 remains to be clarified.
Originally, human OATP1A2 was cloned based on its homology to rat Oatp1a1 (Jacquemin et al. 1994) as a sodium-independent transporter for bile salts and bromosulfophthalein in human liver (Kullak-Ublick et al. 1995). Further studies investigating the substrate spectrum in more detail have shown that OATP1A2 is capable of transporting a wide range of amphipathic organic anions (Table 1), including bile salts (Kullak-Ublick et al. 1995; Meier et al. 1997), thyroid hormones (Friesema et al. 1999), steroid hormones and their conjugates (Bossuyt et al. 1996a), as well as organic cations like N-methyl-quinidine and others (van Montfoort et al. 1999).
Determining the substrate spectrum of other human OATP family members demonstrated that most of them have a similarly broad substrate spectrum partially overlapping with the substrate spectrum defined for OATP1A2 (Table 1). In addition to endogenous compounds, OATPs are capable of transporting various xenobiotics and drugs and, therefore, play an important role in drug absorption, disposition, and excretion. Especially OATP1B1 and OATP1B3, both highly expressed in human liver and involved in the uptake of endogenous substances and of xenobiotics into hepatocytes, are able to transport various drugs, including HMG-CoA-reductase inhibitors like pravastatin (Hsiang et al. 1999; Nakai et al. 2001) and pitavastatin (Hirano et al. 2004), the endothelin receptor antagonist BQ123 (Kullak-Ublick et al. 2001), and the antibiotic rifampicin (Tirona et al. 2003; Vavricka et al. 2002) (Table 1). Since expression and substrates for all human OATP family members have not been completely characterised, additional functional studies and investigations of protein localisations are required to determine the specific role of each OATP family member in drug disposition.
Pharmacogenomics of OATP1B1
In vitro analysis of polymorphisms and haplotypes
Polymorphisms in genes encoding transport proteins may play an important role in the interindividual variability of drug disposition and drug response. A considerable effort has been made to identify single nucleotide polymorphisms (SNPs) or haplotypes, to determine their frequency, and to establish their potential functional consequences on protein localisation and transport function. A summary of so far reported non-synonymous SLCO polymorphisms, haplotypes, alleles, and their allelic frequencies is shown in Table 2 and the localisation of the respective amino acid exchanges is indicated in Fig. 1.
Localisation of amino acid exchanges caused by mutations and polymorphisms in genes encoding human members of the OATP family. A two-dimensional model of human OATP proteins is shown based on several transmembrane analysis programs. Amino acid exchanges caused by mutations in the SLCO1A2 gene encoding human OATP1A2 are shown in grey, by mutations in the SLCO1B1 gene encoding human OATP1B1 are shown in red, by mutations in the SLCO1B3 gene encoding human OATP1B3 are shown in blue, and by mutations in the SLCO2B1 geneencoding human OATP2B1 are shown in green
Tirona et al. (2001) investigated 14 non-synonymous polymorphisms in the SLCO1B1 gene identified in a population of African and European Americans and discovered that some polymorphisms or haplotypes can affect localisation or transport function of the respective protein. In particular, the exchange 217T>C (OATP1B1*2; see Table 2), alone or together with the exchange 1964A>G (haplotype OATP1B1*12), increased the Km value for [3H]estrone-3-sulfate from 0.54 μM to 5.9 and 8.1 μM, respectively. Furthermore, reduced transport of the substrates estrone-3-sulfate, rifampicin, and estradiol-17β-glucuronide was observed for the variants OATP1B1*3, *5, *6, *9, and *13. Interestingly, many of these amino acid exchanges are located within the transmembrane-spanning domains or in the 2nd and 5th extracellular loop (Fig. 1). These results suggest that these protein regions are involved in substrate recognition and transport.
Michalski et al. (2002) analysed 81 human liver samples originating from Caucasians and identified one haplotype containing 5 base pair exchanges resulting in 3 amino acid substitutions. Two of them corresponded to the previously analysed, frequent polymorphisms OATP1B1*1b and OATP1B1*4 (Tirona et al. 2001). The third exchange could be analysed as the first naturally occurring, rare mutation (OATP1B1-Leu193Arg) within the SLCO1B1 gene with a frequency below 0.3%. Using stably transfected MDCKII cells and bromosulfophthalein, estradiol-17β-glucuronide, and taurocholate as substrates, the functional consequences of these 3 exchanges have been analysed (Michalski et al. 2002). Whereas bromosulfophthalein was transported from OATP1B1*1b and OATP1B1*4 according to transport rates determined for the OATP1B1 protein, transport of estradiol-17β-glucuronide was significantly reduced by OATP1B1*4. Using taurocholate as substrate, the transport by OATP1B1*1b was reduced and totally abolished by OATP1B1*4. Furthermore, none of the tested substrates was transported by a protein containing the mutation Leu193Arg. In addition, a pronounced change in protein localisation was observed after expression of the mutant OATP1B1-Leu193Arg protein, which was hardly detectable in the lateral membrane of MDCKII cells and mainly retained intracellularly. These investigations demonstrated that alterations in the extracellular loop 2, where the polymorphisms OATP1B1*1b and OATP1B1*4 are localised (Fig. 1), could influence the substrate spectrum whereas the mutation OATP1B1-Leu193Arg totally abolishes the transport function of the protein.
Nozawa et al. (2002) investigated several polymorphisms in the Japanese population and found that the previously identified OATP1B1*1c allele could not be detected in 267 healthy Japanese subjects, whereas OATP1B1*1b and OATP1B1*5 were present with 54% and 0.7%, respectively. In addition, they identified a novel allele, termed OATP1B1*15 (Table 2), possessing the two SNPs Asn130Asp and Val174Ala simultaneously. The allelic frequency of OATP1B1*15 in the investigated population was 3.0%. Using transfected HEK293 cells, they also investigated the functional consequences of these polymorphisms and found no significant alteration in Km or Vmaxvalues of the [3H]estrone-3-sulfate uptake. These results were confirmed in a second study investigating the same haplotypes (Iwai et al. 2004) and estradiol-17ß-glucuronide as substrate. Interestingly, the authors did not find a change in Km values for any of the three haplotypes. However, the Vmax value for OATP1B1*15 was decreased to less than 30% compared with OATP1B1*1a. Furthermore, Nozawa et al. (2004b) demonstrated that this haplotype exhibits decreased transport activities for SN-38, the active metabolite of the topoisomerase inhibitor topotecan as well as for the HMG-CoA-reductase inhibitor pravastatin. Therefore, the haplotype OATP1B1*15 could contribute to the known interindividual variability in disposition of these two drugs.
OATP1B1 polymorphisms and drug disposition and effects in humans
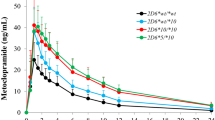
Based on the in vitro findings described above, various groups tested the hypothesis whether polymorphisms in the SLCO1B1 gene have an impact on pharmacokinetics and the effects of drugs in humans. The data currently available on this issue are summarised in Table 3. In spite of the fact that the HMG-CoA-reductase inhibitor pravastatin is not significantly metabolised in humans, pharmacokinetic studies in humans reported a large interindividual variability in pravastatin plasma concentrations (Neuvonen et al. 1998). Kobayashi et al. (2003) reported a pH-dependent OATP2B1-mediated transport of pravastatin. In addition, in vitro data indicate that pravastatin is also a substrate of OATP1B1 (Hsiang et al. 1999; Nakai et al. 2001), thereby mediating pravastatin uptake into hepatocytes. One would expect that genetic variations or haplotypes associated with a reduced OATP1B1 function would limit the access of pravastatin into the hepatocytes and thereby result in increased systemic exposure to pravastatin. Indeed, several publications highlight the relevance of genetic variations in the SLCO1B1 gene for pravastatin disposition (Table 3, Fig. 2) (Mwinyi et al. 2004; Niemi et al. 2004; Nishizato et al. 2003). For example, Niemi et al. (2004) reported that individuals with the 521TC genotype have on average a 106% higher pravastatin plasma concentration compared to the 521TT group (Fig. 2a), which is in accordance with previous in vitro studies showing reduced transport activity for 521T>C (OATP1B1*5; see Table 2) (Tirona et al. 2001, 2003). Based on these pharmacokinetic findings, it was tempting to speculate whether the pravastatin effect on hepatic HMG-CoA-reductase is reduced in individuals with the 521C genotype. In accordance with the underlying hypothesis, Niemi et al. (2005c) reported significantly smaller effects of pravastatin on cholesterol synthesis (determined by plasma lathosterol concentration and lathosterol to cholesterol concentration ratio) in heterozygous carriers of the SCLO1B1*17 (containing -11187G, 388A and 521C) haplotype compared with non-carriers (Fig. 2a) (Niemi et al. 2005c).
Impact of SLCO1B1 polymorphisms and haplotypes on the disposition and effects of pravastatin and repaglinide. a Left panels: effect of SLCO1B1 polymorphism 521 and of haplotype OATP1B1*17 on pharmacokinetics of orally administered prava-statin (1×40 mg) to healthy volunteers of both genders (with permission from Niemi et al. 2004); right panel: reduced pravastatin effect on cholesterol synthesis in carriers with haplotype OATP1B1*17 (with permission from Niemi et al. 2005c). b Effect of SLCO1B1 polymorphisms 521 and -11187 on repaglinide pharmacokinetics and effects on blood glucose studied in healthy volunteers of both genders (1×0.25 mg p. o.). (With permission from Niemi et al. 2005a; American Society for Clinical Pharmacology and Therapeutics)
Recently, the effect of OATP variant alleles on the pharmacokinetic of pitavastatin, another HMG-CoA-reductase inhibitor, has been analysed in healthy Korean subjects (Chung et al. 2005). This group characterised the effect of the alleles OATP1B1*1a, *1b, and *15 (Table 2) and found that the OATP1B1*15 allele is associated with increased pitavastatin plasma concentrations. Similar to pravastatin, the H1-receptor antagonist fexofenadine is not metabolised in humans and is excreted mainly via the biliary route. In a study with healthy volunteers, fexofenadine plasma concentrations were (similar to the observations with pravastatin) highest in individuals with the 521CC genotype, intermediate in the 521TC group and lowest in the 521TT group (Table 3) (Niemi et al. 2005b). Interestingly, fexofenadine has been established to be a substrate for P-glycoprotein and several OATP transporters (OATP1A2, OATP1B3, OATP2B1) (Cvetkovic et al. 1999; Nozawa et al. 2004a; Shimizu et al. 2005). However, one recent in vitro study reported no significant fexofenadine transport by OATP1B1 (Shimizu et al. 2005). This discrepancy between in vivo and in vitro findings deserves further studies.
Finally, there are recently published data indicating a relevance of polymorphisms in the SLCO1B1 gene for pharmacokinetics and effects of a drug which is eliminated completely by metabolism, namely for the antidiabetic drug repaglinide. Similar to the in vivo findings with pravastatin and fexofenadine, the AUC for repaglinide in subjects with the 521CC genotype was 107% and 188% higher, respectively, than in individuals with 521TC and 521CC genotype (Table 3, Fig. 2b) (Niemi et al. 2005a). Accordingly, the 521CC group had the largest changes in blood glucose levels, which were, however, not statistically significant (Niemi et al. 2005a). In addition, the effect of repaglinide on blood glucose was significantly associated with the SCLO1B1 polymorphism - 11187G>A (Fig. 2b).
In addition to this data on the influence of OATP1B1 polymorphisms on drug disposition and effects, Huang et al. (2005) reported an increased risk for unconjugated hyperbilirubinemia in Taiwanese patients with the two frequent polymorphisms at nucleotide position 388 and 521.
Pharmacogenomics of OATP1A2, OATP1B3, and OATP2B1
OATP1A2 (also known as OATP-A) was the first human OATP family member to be cloned and characterised (Kullak-Ublick et al. 1995). Substrates for this uptake transporter include endogenous compounds like steroid hormones and bile salts, but also drugs such as fexofenadine (Table 1). SLCO1A2 mRNA has been detected in various tissues with a high expression in brain (Kullak- Ublick et al. 1995). There, the protein has been localised to the capillary endothelium (Lee et al. 2005a) suggesting that OATP1A2 may play a critical role in the constitution of the blood-brain barrier. Thus, genetic variations in the SLCO1A2 gene encoding human OATP1A2 may have significant pharmacological consequences. Lee et al. (2005a) identified and analysed 6 non-synonymous polymorphisms in the SLCO1A2 gene and found that the allelic frequencies appear to be ethnicity-dependent (Table 2). To investigate the functional consequences of these polymorphisms, they used transiently transfected HeLa cells expressing the respective mutant OATP1A2 protein. They found that the two alleles OATP1A2*3 (516A>C; Glu172Asp) and OATP1A2*6 (404A>T; Asn135Ile) had a markedly reduced transport capacity for deltorphin II and for estrone-3-sulfate. The reason for this reduced transport could be due to an altered plasma membrane localisation of mutated OATP1A2 proteins as demonstrated by surface biotinylation experiments. Furthermore, the authors found that the variants OATP1A2*4 (559G>A; Ala185Thr) and OATP1A2*7 (2003C>G; Thr668Ser) exhibit a substrate-dependent change in transport activity as shown by altered Vmax values only for selected substrates.
Besides OATP1B1, OATP1B3 seems to be the second liver-specific member of the human OATP family (König et al. 2000b). OATP1B3 has 80% amino acid identity with OATP1B1 and both have an overlapping substrate spectrum. Interestingly, literature on the pharmacogenetics of OATP1B3 is relatively sparse in comparison with OATP1B1. The first identification of SNPs in the SLCO1B3 gene was published by Iida et al. (2001) without analysing the functional consequences of the base pair alterations. They found several SNPs in the noncoding region of the SLCO1B3 gene and the non-synonymous SNP 334T>G resulting in the amino acid exchange Ser112Ala. This exchange, as well as one additional frequent polymorphism (699G>A; Met233Ile; allelic frequency of 71%), one rare polymorphism (1564C>T; Gly522Cys; allelic frequency of 1.9%) and the artificial mutation 1748G>A (Gly583Glu), have been analysed in detail by Letschert et al. (2004) with respect to functional consequences on protein localisation and transport characteristics. These investigations demonstrated that both frequent polymorphisms showed localisation and transport properties corresponding to the protein encoded by the reference sequence. In contrast, the rare polymorphism and the artificial mutation abolish the transport function of the protein for the bile salt taurocholate, whereas other substrates like estradiol-17β-glucuronide and estrone-3-sulfate were transported with transport rates according to the protein encoded by the reference sequence. These results support the hypothesis that the 5th extracellular loop of the OATP1B3 protein is involved in substrate recognition, as has also been suggested for the OATP1B1 protein (Tirona et al. 2001). Interestingly, depending on the cell system used for analysis, the rare polymorphism and the mutation showed different glycosylation patterns as demonstrated by immunoblot analysis.
Like OATP1B1 and OATP1B3, OATP2B1 is also expressed in human liver and, therefore, may contribute to the hepatic elimination of endogenous substances and drugs. In addition, OATP2B1 is expressed in various other tissues including placenta (St-Pierre et al. 2002) and small intestine (Kobayashi et al. 2003). As for OATP1A2 and OATP1B3, the knowledge of the functional consequences of variations in the SLCO2B1 gene is limited. Nozawa et al. (2002) described the two variants OATP2B1*2 (1175C>T; Thr392Ile) and OATP2B1*3 (1457C>T; Ser486Phe) (Table 2) with an allelic frequency of 30.9% for OATP2B1*3, whereas the OATP2B1*2 allele could not be detected in additional 267 Japanese subjects. The functional consequences of both variations compared to the OATP2B1*1 protein have been analysed in HEK293 cells. These experiments demonstrated that the Km values for estrone-3-sulfate used as model substrate are in a comparable range for all three OATP2B1 proteins. In addition, no change in the cellular distribution of all different OATP2B1 proteins could be detected (Nozawa et al. 2002).
In conclusion, uptake transporters are increasingly recognised as important factors in the absorption of drugs into the body, the distribution of drugs, and the directed elimination out of the body. In addition, modification of transport rates by drug competition is a new, additional mechanism of drug-drug interactions. Variations in genes encoding uptake transporters can cause interindividual variations of drug effects. Studies regarding the detailed analysis of the consequences of genetic variations, not only limited to single polymorphisms but also to frequent haplotypes of allelic variants, may be of importance to further individualise and optimise treatment regimens involving drugs that are substrates for the respective uptake transporter. Many drugs, however, are substrates for drug metabolising enzymes and efflux transporters in addition to uptake transporters, highlighting the need to characterise the importance of each component for overall drug elimination.
References
Abe T, Kakyo M, Tokui T, Nakagomi R, Nishio T, Nakai D, Nomura H, Unno M, Suzuki M, Naitoh T, Matsuno S, Yawo H (1999) Identification of a novel gene family encoding human liver-specific organic anion transporter LST-1. J Biol Chem 274:17159–17163
Abe T, Unno M, Onogawa T, Tokui T, Kondo TN, Nakagomi R, Adachi H, Fujiwara K, Okabe M, Suzuki T, Nunoki K, Sato E, Kakyo M, Nishio T, Sugita J, Asano N, Tanemoto M, Seki M, Date F, Ono K, Kondo Y, Shiiba K, Suzuki M, Ohtani H, Shimosegawa T, Iinuma K, Nagura H, Ito S, Matsuno S (2001) LST-2, a human liver-specific organic anion transporter, determines methotrexate sensitivity in gastrointestinal cancers. Gastroenterology 120:1689–1699
Borst P, Elferink RO (2002) Mammalian ABC transporters in health and disease. Annu Rev Biochem 71:537–592
Bossuyt X, Müller M, Hagenbuch B, Meier PJ (1996a) Polyspecific drug and steroid clearance by an organic anion transporter of mammalian liver. J Pharmacol Exp Ther 276:891–896
Bossuyt X, Muller M, Meier PJ (1996b) Multispecific amphipathic substrate transport by an organic anion transporter of human liver. J Hepatol 25:733–738
Briz O, Serrano MA, Rebollo N, Hagenbuch B, Meier PJ, Koepsell H, Marin JJ (2002) Carriers involved in targeting the cytostatic bile acid-cisplatin derivatives cis-diammine-chlorocholylglycinate- platinum(II) and cis-diammine-bisursodeoxycholate-platinum(II) toward liver cells. Mol Pharmacol 61:853–860
Briz O, Serrano MA, MacIas RI, Gonzalez-Gallego J, Marin JJ (2003) Role of organic aniontransporting polypeptides, OATP-A, OATP-C and OATP-8, in the human placenta-maternal liver tandem excretory pathway for foetal bilirubin. Biochem J 371:897–905
Chung JY, Cho JY, Yu KS, Kim JR, Oh DS, Jung HR, Lim KS, Moon KH, Shin SG, Jang IJ (2005) Effect of OATP1B1 (SLCO1B1) variant alleles on the pharmacokinetics of pitavastatin in healthy volunteers. Clin Pharmacol Ther 78:342–350
Cui Y, König J, Leier I, Buchholz U, Keppler D (2001) Hepatic uptake of bilirubin and its conjugates by the human organic anion transporter SLC21A6. J Biol Chem 276:9626–9630
Cvetkovic M, Leake B, Fromm MF, Wilkinson GR, Kim RB (1999) OATP and P-glycoprotein transporters mediate the cellular uptake and excretion of fexofenadine. Drug Metab Dispos 27:866–871
Fehrenbach T, Cui Y, Faulstich H, Keppler D (2003) Characterization of the transport of the bicyclic peptide phalloidin by human hepatic transport proteins. Naunyn-Schmiedeberg’s Arch Pharmacol 368:415–420
Fischer WJ, Altheimer S, Cattori V, Meier PJ, Dietrich DR, Hagenbuch B (2005) Organic anion transporting polypeptides expressed in liver and brain mediate uptake of microcystin. Toxicol Appl Pharmacol 203:257–263
Friesema EC, Docter R, Moerings EP, Stieger B, Hagenbuch B, Meier PJ, Krenning EP, Hennemann G, Visser TJ (1999) Identification of thyroid hormone transporters. Biochem Biophys Res Commun 254:497–501
Fromm MF (2004) Importance of P-glycoprotein at blood-tissue barriers. Trends Pharmacol Sci 25:423–429
Fujiwara K, Adachi H, Nishio T, Unno M, Tokui T, Okabe M, Onogawa T, Suzuki T, Asano N, Tanemoto M, Seki M, Shiiba K, Suzuki M, Kondo Y, Nunoki K, Shimosegawa T, Iinuma K, Ito S, Matsuno S, Abe T (2001) Identification of thyroid hormone transporters in humans: different molecules are involved in a tissue-specific manner. Endocrinology 142:2005–2012
Gao B, Hagenbuch B, Kullak-Ublick GA, Benke D, Aguzzi A, Meier PJ (2000) Organic aniontransporting polypeptides mediate transport of opioid peptides across blood-brain barrier. J Pharmacol Exp Ther 294:73–79
Gao B, Huber RD, Wenzel A, Vavricka SR, Ismair MG, Reme C, Meier PJ (2005) Localisation of organic anion transporting polypeptides in the rat and human ciliary body epithelium. Exp Eye Res 80:61–72
Hagenbuch B, Meier PJ (2003) The superfamily of organic anion transporting polypeptides. Biochim Biophys Acta 1609:1–18
Hagenbuch B, Meier PJ (2004) Organic anion transporting polypeptides of the OATP/ SLC21 family: phylogenetic classification as OATP/ SLCO superfamily, new nomenclature and molecular/functional properties. Pflugers Arch 447:653–665
Hediger MA, Romero MF, Peng JB, Rolfs A, Takanaga H, Bruford EA (2004) The ABCs of solute carriers: physiological, pathological and therapeutic implications of human membrane transport proteinsIntroduction. Pflugers Arch 447:465–468
Hirano M, Maeda K, Shitara Y, Sugiyama Y (2004) Contribution of OATP2 (OATP1B1) and OATP8 (OATP1B3) to the hepatic uptake of pitavastatin in humans. J Pharmacol Exp Ther 311:139–146
Hsiang B, Zhu Y, Wang Z, Wu Y, Sasseville V, Yang WP, Kirchgessner TG (1999) A novel human hepatic organic anion transporting polypeptide (OATP2). Identification of a liver-specific human organic anion transporting polypeptide and identification of rat and human hydroxymethylglutaryl-CoA reductase inhibitor transporters. J Biol Chem 274:37161–37168
Huang CS, Huang MJ, Lin MS, Yang SS, Teng HC, Tang KS (2005) Genetic factors related to unconjugated hyperbilirubinemia amongst adults. Pharmacogenet Genomics 15:43–50
Iida A, Saito S, Sekine A, Mishima C, Kondo K, Kitamura Y, Harigae S, Osawa S, Nakamura Y (2001) Catalog of 258 single-nucleotide polymorphisms (SNPs) in genes encoding three organic anion transporters, three organic anion-transporting polypeptides, and three NADH:ubiquinone oxidoreductase flavoproteins. J Hum Genet 46:668–683
Ismair MG, Stieger B, Cattori V, Hagenbuch B, Fried M, Meier PJ, Kullak-Ublick GA (2001) Hepatic uptake of cholecystokinin octapeptide by organic anion-transporting polypeptides OATP4 and OATP8 of rat and human liver. Gastroenterology 121:1185–1190
Iwai M, Suzuki H, Ieiri I, Otsubo K, Sugiyama Y (2004) Functional analysis of single nucleotide polymorphisms of hepatic organic anion transporter OATP1B1 (OATP-C). Pharmacogenetics 14:749–757
Jacquemin E, Hagenbuch B, Stieger B, Wolkoff AW, Meier PJ (1994) Expression cloning of a rat liver Na(+)-independent organic anion transporter. Proc Natl Acad Sci U S A 91:133–137
Kajosaari LI, Laitila J, Neuvonen PJ, Backman JT (2005) Metabolism of repaglinide by CYP2C8 and CYP3A4 in vitro: effect of fibrates and rifampicin. Basic Clin Pharmacol Toxicol 97:249–256
Kameyama Y, Yamashita K, Kobayashi K, Hosokawa M, Chiba K (2005) Functional characterization of SLCO1B1 (OATP-C) variants, SLCO1B1*5, SLCO1B1*15 and SLCO1B1*15+C1007G, by using transient expression systems of HeLa and HEK293 cells. Pharmacogenet Genomics 15:513–522
Kobayashi D, Nozawa T, Imai K, Nezu J, Tsuji A, Tamai I (2003) Involvement of human organic anion transporting polypeptide OATP-B (SLC21A9) in pH-dependent transport across intestinal apical membrane. J Pharmacol Exp Ther 306:703–708
König J, Nies AT, Cui Y, Leier I, Keppler D (1999) Conjugate export pumps of the multidrug resistance protein (MRP) family: localisation, substrate specificity, and MRP2-mediated drug resistance. Biochim Biophys Acta 1461:377–394
König J, Cui Y, Nies AT, Keppler D (2000a) A novel human organic anion transporting polypeptide localized to the basolateral hepatocyte membrane. Am J Physiol Gastrointest Liver Physiol 278:G156–164
König J, Cui Y, Nies AT, Keppler D (2000b) Localization and genomic organization of a new hepatocellular organic anion transporting polypeptide. J Biol Chem 275:23161–23168
Kopplow K, Letschert K, König J, Walter B, Keppler D (2005) Human hepatobiliary transport of organic anions analyzed by quadruple-transfected cells. Mol Pharmacol 68:1031–1038
Kullak-Ublick GA, Hagenbuch B, Stieger B, Schteingart CD, Hofmann AF, Wolkoff AW, Meier PJ (1995) Molecular and functional characterization of an organic anion transporting polypeptide cloned from human liver. Gastroenterology 109:1274–1282
Kullak-Ublick GA, Glasa J, Boker C, Oswald M, Grutzner U, Hagenbuch B, Stieger B, Meier PJ, Beuers U, Kramer W, Wess G, Paumgartner G (1997) Chlorambucil-taurocholate is transported by bile acid carriers expressed in human hepatocellular carcinomas. Gastroenterology 113:1295–1305
Kullak-Ublick GA, Fisch T, Oswald M, Hagenbuch B, Meier PJ, Beuers U, Paumgartner G (1998) Dehydroepiandrosterone sulfate (DHEAS): identification of a carrier protein in human liver and brain. FEBS Lett 424:173–176
Kullak-Ublick GA, Ismair MG, Stieger B, Landmann L, Huber R, Pizzagalli F, Fattinger K, Meier PJ, Hagenbuch B (2001) Organic anion-transporting polypeptide B (OATP-B) and its functional comparison with three other OATPs of human liver. Gastroenterology 120:525– 533
Kruh GD, Belinsky MG (2003) The MRP family of drug efflux pumps. Oncogene 22:7537–7552
Lee W, Glaeser H, Smith LH, Roberts RL, Moeckel GW, Gervasini G, Leake BF, Kim RB (2005a) Polymorphisms in human organic anion-transporting polypeptide 1A2 (OATP1A2): implications for altered drug disposition and central nervous system drug entry. J Biol Chem 280:9610–9617
Lee E, Ryan S, Birmingham B, Zalikowski J, March R, Ambrose H, Moore R, Lee C, Chen Y, Schneck D (2005b) Rosuvastatin pharmacokinetics and pharmacogenetics in white and Asian subjects residing in the same environment. Clin Pharmacol Ther 78:330–341
Letschert K, Keppler D, König J (2004) Mutations in the SLCO1B3 gene affecting the substrate specificity of the hepatocellular uptake transporter OATP1B3 (OATP8). Pharmacogenetics 14:441-452
Meier PJ, Eckhardt U, Schroeder A, Hagenbuch B, Stieger B (1997) Substrate specificity of sinusoidal bile acid and organic anion uptake systems in rat and human liver. Hepatology 26:1667–1677
Meier-Abt F, Faulstich H, Hagenbuch B (2004) Identification of phalloidin uptake systems of rat and human liver. Biochim Biophys Acta 1664:64–69
Michalski C, Cui Y, Nies AT, Nuessler AK, Neuhaus P, Zanger UM, Klein K, Eichelbaum M, Keppler D, König J (2002) A naturally occurring mutation in the SLC21A6 gene causing impaired membrane localisation of the hepatocyte uptake transporter. J Biol Chem 277:43058–43063
Mikkaichi T, Suzuki T, Tanemoto M, Ito S, Abe T (2004a) The organic anion transporter (OATP) family. Drug Metab Pharmacokinet 19:171–179
Mikkaichi T, Suzuki T, Onogawa T, Tanemoto M, Mizutamari H, Okada M, Chaki T, Masuda S, Tokui T, Eto N, Abe M, Satoh F, Unno M, Hishinuma T, Inui K, Ito S, Goto J, Abe T (2004b) Isolation and characterization of a digoxin transporter and its rat homologue expressed in the kidney. Proc Natl Acad Sci U S A 101:3569–3574
Morimoto K, Oishi T, Ueda S, Ueda M, Hosokawa M, Chiba K (2004) A novel variant allele of OATP-C (SLCO1B1) found in a Japanese patient with pravastatin-induced myopathy. Drug Metab Pharmacokinet 19:453–455
Mwinyi J, Johne A, Bauer S, Roots I, Gerloff T (2004) Evidence for inverse effects of OATP-C (SLC21A6) 5 and 1b haplotypes on pravastatin kinetics. Clin Pharmacol Ther 75:415–421
Nakai D, Nakagomi R, Furuta Y, Tokui T, Abe T, Ikeda T, Nishimura K (2001) Human liverspecific organic anion transporter, LST-1, mediates uptake of pravastatin by human hepatocytes. J Pharmacol Exp Ther 297:861–867
Neuvonen PJ, Kantola T, Kivistö KT (1998) Simvastatin but not pravastatin is very susceptible to interaction with the CYP3A4 inhibitor itraconazole. Clin Pharmacol Ther 63:332–341
Niemi M, Schaeffeler E, Lang T, Fromm MF, Neuvonen M, Kyrklund C, Backman JT, Kerb R, Schwab M, Neuvonen PJ, Eichelbaum M, Kivistö KT (2004) High plasma pravastatin concentrations are associated with single nucleotide polymorphisms and haplotypes of organic anion transporting polypeptide-C (OATP-C, SLCO1B1). Pharmacogenetics 14:429–440
Niemi M, Backman JT, Kajosaari LI, Leathart JB, Neuvonen M, Daly AK, Eichelbaum M, Kivistö KT, Neuvonen PJ (2005a) Polymorphic organic anion transporting polypeptide 1B1 is a major determinant of repaglinide pharmacokinetics. Clin Pharmacol Ther 77:468–478
Niemi M, Kivistö KT, Hofmann U, Schwab M, Eichelbaum M, Fromm MF (2005b) Fexofenadine pharmacokinetics are associated with a polymorphism of the SLCO1B1 gene (encoding OATP1B1). Br J Clin Pharmacol 59:602–604
Niemi M, Neuvonen PJ, Hofmann U, Backman JT, Schwab M, Lutjohann D, von Bergmann K, Eichelbaum M, Kivistö KT (2005c) Acute effects of pravastatin on cholesterol synthesis are associated with SLCO1B1 (encoding OATP1B1) haplotype *17. Pharmacogenet Genomics 15:303–309
Nishizato Y, Ieiri I, Suzuki H, Kimura M, Kawabata K, Hirota T, Takane H, Irie S, Kusuhara H, Urasaki Y, Urae A, Higuchi S, Otsubo K, Sugiyama Y (2003) Polymorphisms of OATP-C (SLC21A6) and OAT3 (SLC22A8) genes: consequences for pravastatin pharmacokinetics. Clin Pharmacol Ther 73:554–565
Nozawa T, Nakajima M, Tamai I, Noda K, Nezu J, Sai Y, Tsuji A, Yokoi T (2002) Genetic polymorphisms of human organic anion transporters OATP-C (SLC21A6) and OATP-B (SLC21A9): allele frequencies in the Japanese population and functional analysis. J Pharmacol Exp Ther 302:804–813
Nozawa T, Tamai I, Sai Y, Nezu J, Tsuji A (2003) Contribution of organic anion transporting polypeptide OATP-C to hepatic elimination of the opioid pentapeptide analogue [D-Ala2, D-Leu5]-enkephalin. J Pharm Pharmacol 55:1013–1020
Nozawa T, Imai K, Nezu J, Tsuji A, Tamai I (2004a) Functional characterization of pH-sensitive organic anion transporting polypeptide OATP-B in human. J Pharmacol Exp Ther 308:438–445
Nozawa T, Minami H, Sugiura S, Tsuji A, Tamai I (2004b) Role of Organic Anion Transporter Oatp1b1 (Oatp-C) in Hepatic Uptake of Irinotecan and Its Active Metabolite Sn-38: In Vitro Evidence and Effect of Single Nucleotide Polymorphisms. Drug Metab Dispos
Nozawa T, Sugiura S, Nakajima M, Goto A, Yokoi T, Nezu J, Tsuji A, Tamai I (2004c) Involvement of organic anion transporting polypeptides in the transport of troglitazone sulfate: implications for understanding troglitazone hepatotoxicity. Drug Metab Dispos 32:291–294
Nozawa T, Minami H, Sugiura S, Tsuji A, Tamai I (2005) Role of organic anion transporter OATP1B1 (OATP-C) in hepatic uptake of irinotecan and its active metabolite, 7-ethyl-10- hydroxycamptothecin: in vitro evidence and effect of single nucleotide polymorphisms. Drug Metab Dispos 33:434–439
Pascolo L, Cupelli F, Anelli PL, Lorusso V, Visigalli M, Uggeri F, Tiribelli C (1999) Molecular mechanisms for the hepatic uptake of magnetic resonance imaging contrast agents. Biochem Biophys Res Commun 257:746–752
Pizzagalli F, Hagenbuch B, Stieger B, Klenk U, Folkers G, Meier PJ (2002) Identification of a novel human organic anion transporting polypeptide as a high affinity thyroxine transporter. Mol Endocrinol 16:2283–2296
Sandhu P, Lee W, Xu X, Leake BF, Yamazaki M, Stone JA, Lin JH, Pearson PG, Kim RB (2005) Hepatic uptake of the novel antifungal agent caspofungin. Drug Metab Dispos 33:676–682
Sato K, Sugawara J, Sato T, Mizutamari H, Suzuki T, Ito A, Mikkaichi T, Onogawa T, Tanemoto M, Unno M, Abe T, Okamura K (2003) Expression of organic anion transporting polypeptide E (OATP-E) in human placenta. Placenta 24:144–148
Schneck DW, Birmingham BK, Zalikowski JA, Mitchell PD, Wang Y, Martin PD, Lasseter KC, Brown CD, Windass AS, Raza A (2004) The effect of gemfibrozil on the pharmacokinetics of rosuvastatin. Clin Pharmacol Ther 75:455–463
Shimizu M, Fuse K, Okudaira K, Nishigaki R, Maeda K, Kusuhara H, Sugiyama Y (2005) Contribution of OATP (organic anion-transporting polypeptide) family transporters to the hepatic uptake of fexofenadine in humans. Drug Metab Dispos 33:1477–1481
Shitara Y, Hirano M, Sato H, Sugiyama Y (2004) Gemfibrozil and its glucuronide inhibit the organic anion transporting polypeptide 2 (OATP2/OATP1B1:SLC21A6)-mediated hepatic uptake and CYP2C8-mediated metabolism of cerivastatin: analysis of the mechanism of the clinically relevant drug-drug interaction between cerivastatin and gemfibrozil. J Pharmacol Exp Ther 311:228–236
Smith NF, Acharya MR, Desai N, Figg WD, Sparreboom A (2005) Identification of OATP1B3 as a High-Affinity Hepatocellular Transporter of Paclitaxel. Cancer Biol Ther 4 St-Pierre MV, Hagenbuch B, Ugele B, Meier PJ, Stallmach T (2002) Characterization of an organic anion-transporting polypeptide (OATP-B) in human placenta. J Clin Endocrinol Metab 87:1856–1863
Takada T, Weiss HM, Kretz O, Gross G, Sugiyama Y (2004) Hepatic transport of PKI166, an epidermal growth factor receptor kinase inhibitor of the pyrrolo-pyrimidine class, and its main metabolite, ACU154. Drug Metab Dispos 32:1272–1278
Tamai I, Nezu J, Uchino H, Sai Y, Oku A, Shimane M, Tsuji A (2000) Molecular identification and characterization of novel members of the human organic anion transporter (OATP) family. Biochem Biophys Res Commun 273:251–260
Tirona RG, Leake BF, Merino G, Kim RB (2001) Polymorphisms in OATP-C: identification of multiple allelic variants associated with altered transport activity among European- and African-Americans. J Biol Chem 276:35669–35675
Tirona RG, Leake BF, Wolkoff AW, Kim RB (2003) Human organic anion transporting polypeptide-C (SLC21A6) is a major determinant of rifampin-mediated pregnane X receptor activation. J Pharmacol Exp Ther 304:223–228
van Montfoort JE, Hagenbuch B, Fattinger KE, Müller M, Groothuis GM, Meijer DK, Meier PJ (1999) Polyspecific organic anion transporting polypeptides mediate hepatic uptake of amphipathic type II organic cations. J Pharmacol Exp Ther 291:147–152
Vavricka SR, Van Montfoort J, Ha HR, Meier PJ, Fattinger K (2002) Interactions of rifamycin SV and rifampicin with organic anion uptake systems of human liver. Hepatology 36:164–172
Acknowledgement
This work was supported by grant DFG Ko2120/1-3 of the Deutsche Forschungsgemeinschaft.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
König, J., Seithel, A., Gradhand, U. et al. Pharmacogenomics of human OATP transporters. Naunyn Schmied Arch Pharmacol 372, 432–443 (2006). https://doi.org/10.1007/s00210-006-0040-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-006-0040-y