Abstract
Purpose
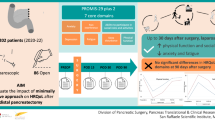
This study was designed to compare quality of life (QoL) among patients who underwent open versus laparoscopic pancreatic resection, including distal pancreatectomy and pancreaticoduodenectomy, and to identify clinical characteristics that are associated with changes in QoL.
Methods
Quality of life (QoL) was assessed in patients undergoing pancreatic resection with the Functional Assessment of Cancer Therapy-Hepatobiliary questionnaire preoperatively and 2 weeks, 1, 3, and 6 months postoperatively. Multilevel regression modeling was used to determine the variability in each QoL domain within the first 2 weeks (postoperative period) and thereafter (recovery period).
Results
Among 159 patients, 60.4% underwent open and 39.6% underwent laparoscopic surgery. Physical, functional, hepatobiliary, and total QoL scores decreased in the postoperative period but returned to baseline levels by 6 months postoperatively. Emotional QoL improved from baseline by 2 weeks after surgery (p < 0.001) and social QoL improved from baseline by 3 months after surgery (p < 0.001). Emotional QoL was the only domain where significant differences were observed in QoL in the postoperative and recovery periods between patients who underwent open and laparoscopic pancreatic resection. Controlling for surgical approach, patients who experienced a grade III or IV complication experienced greater declines in physical, functional, hepatobiliary, and total QoL in the postoperative period. The negative impact of complications on QoL resolved by 6 months postoperatively.
Conclusions
The impact of pancreatic resection on QoL was comparable between patients who underwent laparoscopic versus open pancreatic resection. Complications were strongly associated with changes in postoperative QoL, suggesting that performing a safe operation is the best approach for optimizing patient reported QoL.



Similar content being viewed by others
References
Tran Cao HS, Lopez N, Chang DC, et al. Improved perioperative outcomes with minimally invasive distal pancreatectomy: results from a population-based analysis. JAMA Surg. 2014;149(3):237–43.
Torphy RJ, Friedman C, Halpern A, et al. Comparing short-term and oncologic outcomes of minimally invasive versus open pancreaticoduodenectomy across low and high volume centers. Ann Surg. 2018. https://doi.org/10.1097/SLA.0000000000002810.
Croome KP, Farnell MB, Que FG, et al. Total laparoscopic pancreaticoduodenectomy for pancreatic ductal adenocarcinoma: oncologic advantages over open approaches? Ann Surg. 2014;260(4):633–8; discussion 638–40.
Kendrick ML, Cusati D. Total laparoscopic pancreaticoduodenectomy: feasibility and outcome in an early experience. Arch Surg (Chicago, Ill: 1960). 2010;145(1):19–23.
Nassour I, Wang SC, Christie A, et al. Minimally invasive versus open pancreaticoduodenectomy: a propensity-matched study from a national cohort of patients. Ann Surg. 2018;268(1):151–7.
Nieveen van Dijkum EJ, Kuhlmann KF, Terwee CB, Obertop H, de Haes JC, Gouma DJ. Quality of life after curative or palliative surgical treatment of pancreatic and periampullary carcinoma. Br J Surg. 2005;92(4):471–7.
Schniewind B, Bestmann B, Henne-Bruns D, Faendrich F, Kremer B, Kuechler T. Quality of life after pancreaticoduodenectomy for ductal adenocarcinoma of the pancreatic head. Br J Surg. 2006;93(9):1099–107.
Heerkens HD, Tseng DS, Lips IM, et al. Health-related quality of life after pancreatic resection for malignancy. Br J Surg. 2016;103(3):257–66.
Eaton AA, Gonen M, Karanicolas P, et al. Health-related quality of life after pancreatectomy: results from a randomized controlled trial. Ann Surg Oncol. 2016;23(7):2137–45.
Allen CJ, Yakoub D, Macedo FI, et al. Long-term quality of life and gastrointestinal functional outcomes after pancreaticoduodenectomy. Ann Surg. 2018;268(4):657–64.
Cella D, Butt Z, Kindler HL, et al. Validity of the FACT Hepatobiliary (FACT-Hep) questionnaire for assessing disease-related symptoms and health-related quality of life in patients with metastatic pancreatic cancer. Qual Life Res. 2013;22(5):1105–12.
Heffernan N, Cella D, Webster K, et al. Measuring health-related quality of life in patients with hepatobiliary cancers: the functional assessment of cancer therapy-hepatobiliary questionnaire. J Clin Oncol. 2002;20(9):2229–39.
Webster K, Cella D, Yost K. The Functional Assessment of Chronic Illness Therapy (FACIT) Measurement System: properties, applications, and interpretation. Health Qual Life Outcomes. 2003;1:79.
Scientific Advisory Committee of the Medical Outcomes Trust. Assessing Health Status and Quality-of-Life Instruments: attributes and review criteria. Qual Life Res 2002;11(3):193–205.
Desquilbet L, Mariotti F. Dose-response analyses using restricted cubic spline functions in public health research. Stat Med. 2010;29(9):1037–57.
Cloyd JM, Tran Cao HS, Petzel MQ, et al. Impact of pancreatectomy on long-term patient-reported symptoms and quality of life in recurrence-free survivors of pancreatic and periampullary neoplasms. J Surg Oncol. 2017;115(2):144–50.
Brucker PS, Yost K, Cashy J, Webster K, Cella D. General population and cancer patient norms for the Functional Assessment of Cancer Therapy-General (FACT-G). Evaluation Health Prof. 2005;28(2):192–211.
Heerkens HD, van Berkel L, Tseng DSJ, et al. Long-term health-related quality of life after pancreatic resection for malignancy in patients with and without severe postoperative complications. HPB. 2018;20(2):188–95.
Velanovich V. Laparoscopic vs open surgery: a preliminary comparison of quality-of-life outcomes. Surg Endosc. 2000;14(1):16–21.
Biere SS, van Berge Henegouwen MI, Maas KW, et al. Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet (London, Engl). 2012;379(9829):1887–92.
Weeks JC, Nelson H, Gelber S, Sargent D, Schroeder G. Short-term quality-of-life outcomes following laparoscopic-assisted colectomy vs open colectomy for colon cancer: a randomized trial. JAMA. 2002;287(3):321–8.
Heikkinen TJ, Haukipuro K, Koivukangas P, et al. Comparison of costs between laparoscopic and open Nissen fundoplication: a prospective randomized study with a 3-month followup. J Am Coll Surg. 1999;188(4):368–76.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
DISCLOSURES
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplemental Fig.
1 Study population flow diagram (PDF 7 kb)
Supplemental Fig.
2 Boxplots of FACT-Hep subscale (A-E) and total (F) QoL scores from preop to 6 months following pancreatic resection. In the box plots, the boundary of the box closest to 0 represents the 25th percentile, the line in the box represents the median, and the boundary of the box farthest from 0 represents the 75th percentile. The whiskers represent scores less than 1.5× interquartile range, and the points below the whiskers indicate outliers that are lower than 1.5× interquartile range (TIFF 76733 kb)
Supplemental Fig.
3 Mean trajectories of FACT-Hep subscale and Total QoL scores at 2 weeks, 1 month, 3 months, and 6 months postoperatively by operation and surgical approach (TIFF 76735 kb)
Rights and permissions
About this article
Cite this article
Torphy, R.J., Chapman, B.C., Friedman, C. et al. Quality of Life Following Major Laparoscopic or Open Pancreatic Resection. Ann Surg Oncol 26, 2985–2993 (2019). https://doi.org/10.1245/s10434-019-07449-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-019-07449-x