Abstract
Background:
Increases in Gram-positive infections and infections with Enterobacteriaceae with antimicrobial resistance have been reported in patients with spontaneous bacterial peritonitis (SBP). This study was performed to investigate the rate of treatment failures of recommended empirical therapies and the impact on mortality.
Patients and Methods:
A prospectively collected database comprising 101 patients with SBP (70 nosocomial, 31 community acquired) treated at a university hospital between 2002 and 2006 in Munich, Germany, was analyzed.
Results:
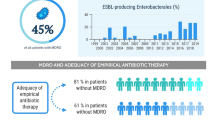
17 patients initially received a broader than recommended antibiotic regimen. Most of these were treated in the intensive care unit because of severe sepsis/septic shock. Hospital mortality in this group was 82%. A modification of therapy was necessary in 24 of the 84 patients receiving one of the published first-line therapies (cefotaxime, ampicillin/clavulanate, or ciprofloxacin). Mortality was significantly higher in these patients than in those with no change in treatment (66.7% vs 30%, p = 0.002). In 29 patients with positive cultures, mortality was also higher in those with an ineffective first-line treatment (90% vs 45%, p = 0.032). In the multivariable analysis, a modification of antibiotic treatment was an independent risk factor for mortality (odds ratio 5.876, 95% confidence interval 1.826–18.910, p = 0.003). In 41 culture-positive cases, the most commonly cultured pathogens were Escherichia coli (n = 17) and Enterococcus faecium (n = 10). Of the encountered bacterial microorganisms, 14 (33.3%) were resistant to cefotaxime, 17 (38.6%) were resistant to amoxicillin/clavulanate, and 19 (45.2%) were resistant to ciprofloxacin. 29 (64.4%) of the isolates were resistant to one of the recommended firstline antibiotic regimens, and 11 (24.4%) of the isolates were resistant to all three.
Conclusion:
Recommended empirical antibiotic regimens fail to achieve the desired effect in a substantial number of hospitalized patients with SBP. This has a negative impact on mortality.
Article PDF
Similar content being viewed by others
References
Such J, Guarner C, Runyon BA: Pathogenesis and clinical features of spontaneous bacterial peritonitis. In: Ginès P, Arroyo V, Rodés J, Schrier RW (eds) Ascites and renal dysfunction in liver disease. 2nd edition Malden Mass, Blackwell 2005, pp 422–433.
Garcia-Tsao G: Bacterial infections in cirrhosis: treatment and prophylaxis. J Hepatol 2005; 42: S85–92.
Sort P, Navasa M, Arroyo V, Aldeguer X, Planas R, Ruiz-del-Arbol L, Castells L, Vargas V, Soriano G, Guevara M, Gines P, Rodes J: Effect of intravenous albumin on renal impairment and mortality in patients with cirrhosis and spontaneous bacterial peritonitis. N Engl J Med 1999; 341: 403–409.
Ricart E, Soriano G, et al. Amoxicillin-clavulanic acid versus cefotaxime in the therapy of bacterial infections in cirrhotic patients. J Hepatol 2000; 32: 596–602.
Terg R, Cobas S, et al. Oral ciprofloxacin after a short course of intravenous ciprofloxacin in the treatment of spontaneous bacterial peritonitis: results of a multicenter, randomized study. J Hepatol 2000; 33: 564–569.
Felisart J, Rimola A, Arroyo V, Perez-Ayuso RM, Quintero E, Gines P, Rodes J: Cefotaxime is more effective than is ampicillin-tobramycin in cirrhotics with severe infections. Hepatology 1985; 5: 456–462.
Runyon BA, McHutchison JG, Antillon MR, Akriviadis EA, Montano AA: Short-course versus long-course antibiotic treatment of spontaneous bacterial peritonitis. A randomized controlled study of 100 patients. Gastroenterology 1991; 100: 1737–1742.
Mercader J, Gomez J, Ruiz J, Garre MC, Valdes M: Use of ceftriaxone in the treatment of bacterial infections in cirrhotic patients. Chemotherapy. 1989; 35: 23–26.
Gómez-Jiménez J, Ribera E, Gasser I, Artaza MA, Del Valle O, Pahissa A, Martínez-Vázquez JM: Randomized trial comparing ceftriaxone with cefonicid for treatment of spontaneous bacterial peritonitis in cirrhotic patients. Antimicrob Agents Chemother 1993; 37: 1587–1592.
Rimola A, García-Tsao G, et al. Diagnosis, treatment and prophylaxis of spontaneous bacterial peritonitis: a consensus document. International Ascites Club. J Hepatol 2000; 32: 142–153.
Grange JD, Amiot X, Grange V, Gutmann L, Biour M, Bodin F, Poupon R: Amoxicillin-clavulanic acid therapy of spontaneous bacterial peritonitis: a prospective study of twenty-seven cases in cirrhotic patients. Hepatology 1990; 11: 360–364.
Fernandez J, Navasa M, Gomez J, Colmenero J, Vila J, Arroyo V, Rodes J: Bacterial infections in cirrhosis: epidemiological changes with invasive procedures and norfloxacin prophylaxis. Hepatology 2002; 35: 140–148.
Singh N, Wagener MM, Gayowski T: Changing epidemiology and predictors of mortality in patients with spontaneous bacterial peritonitis at a liver transplant unit. Clin Microbiol Infect 2003; 9: 531–537.
Campillo BRJ, Kheo T, Dupeyron C: Nosocomial spontaneous bacterial peritonitis and bacteremia in cirrhotic patients: impact of isolate type on prognosis and characteristics of infection. Clin Infect Dis 2002; 35: 1–10.
Performance Standards for Antimicrobial Susceptibility Testing (2005) Fifteenth International Supplement. Clinical and Laboratory Performance Institute/NCCLS, Wayne.
Pedersen G, Schonheyder HC, Steffensen FH, Sorensen HT: Risk of resistance related to antibiotic use before admission in patients with community-acquired bacteraemia. J Antimicrob Chem 1999; 43: 119–126.
Bouchillon SK, Johnson BM, et al. Determining incidence of extended spectrum [beta]-lactamase producing Enterobacteriaceae, vancomycin-resistant Enterococcus faecium and methicillin-resistant Staphylococcus aureus in 38 centres from 17 countries: the PEARLS study 2001–2002. Int J Antimicrob Agents 2004; 24: 119–124.
Navasa MFA, Llovet JM, Clemente G, Vargas V, Rimola A, Marco F, Guarner C, Forne M, Planas R, Banares R, Castells L, De Jimenez Anta MT, Arroyo V, Rodes J: Randomized, comparative study of oral ofloxacin versus intravenous cefotaxime in spontaneous bacterial peritonitis. Gastroenterology 1996; 111: 1011–1017.
Alvarez-Lerma F: Modification of empiric antibiotic treatment in patients with pneumonia acquired in the intensive care unit. ICU-Acquired Pneumonia Study Group. Intensive Care Med 1996; 22: 387–394.
Rello J, Gallego M, Mariscal D, Soñora R, Valles J: The value of routine microbial investigation in ventilator-associated pneumonia. Am J Respir Crit Care Med 1997; 156: 196–200.
Luna CM, Vujacich P, et al. Impact of BAL data on the therapy and outcome of ventilator-associated pneumonia. Chest 1997; 111: 676–685.
Leibovici L, Shraga I, Drucker M, Konigsberger H, Samra Z, Pitlik SD: The benefit of appropriate empirical antibiotic treatment in patients with bloodstream infection. J Intern Med 1998; 244: 379–386.
Behrendt G, Schneider S, Brodt HR, Just-Nübling G, Shah PM: Influence of antimicrobial treatment on mortality in septicemia. J Chemother 1999; 11: 179–186.
MacArthur RD, Miller M, et al. Adequacy of early empiric antibiotic treatment and survival in severe sepsis: experience from the MONARCS trial. Clin Infect Dis 2004; 38: 284–288.
Garnacho-Montero J, Garcia-Garmendia JL, Barrero-Almodovar A, Jimenez-Jimenez FJ, Perez-Paredes C, Ortiz-Leyba C: Impact of adequate empirical antibiotic therapy on the outcome of patients admitted to the intensive care unit with sepsis. Crit Care Med 2003; 31: 2742–2751.
Scarsi KK, Feinglass JM, Scheetz MH, Postelnick MJ, Bolon MK, Noscin GA: Impact of inactive empiric antimicrobial therapy on inpatient mortality and length of stay. Antimicrob Agents Chemother 2006; 50: 3355–3360.
Kollef MH, Sherman G, Ward S, Fraser VJ: Inadequate antimicrobial treatment of infections: a risk factor for hospital mortality among critically ill patients. Chest 1999; 115: 462–474.
Dellinger RP, Carlet JM, Masur H, Gerlach H, Calandra T, Cohen J, Gea-Banacloche J, Keh D, Marshall JC, Parker MM, Ramsay G, Zimmerman JL, Vincent JL, Levy MM: Surviving Sepsis Campaign Management Guidelines Committee. Surviving Sepsis Campaign guidelines for management of severe sepsis and septic shock. Crit Care Med 2004; 23: 858–873.
Cholongitas E, Senzolo M, et al. Risk factors, sequential organ failure assessment and model for end-stage liver disease scores for predicting short term mortality in cirrhotic patients admitted to intensive care unit. Aliment Pharmacol Ther 2006; 23: 883–893.
Blasco A, Navasa M: Treatment and prophylaxis of spontaneous bacterial peritonitis. In: Ginès P, Arroyo V, Rodés J, Schrier RW (eds): Ascites and renal dysfunction in liver disease. 2nd edition Blackwell, Oxford 2005.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Umgelter, A., Reindl, W., Miedaner, M. et al. Failure of Current Antibiotic First-Line Regimens and Mortality in Hospitalized Patients with Spontaneous Bacterial Peritonitis. Infection 37, 2–8 (2009). https://doi.org/10.1007/s15010-008-8060-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-008-8060-9