Abstract
The complexity of handheld steerable laparoscopic instruments (SLI) may impair the learning curve compared to conventional instruments when first utilized. This study aimed to provide the current state of interest in the use of SLI, the current use of these in daily practice and the type of training which is conducted before using SLI in the operating room (OR) on real patients. An online survey was distributed by European Association of Endoscopic Surgery (EAES) Executive Office to all active members, between January 4th and February 3rd, 2020. The survey consisted of 14 questions regarding the usage and training of steerable laparoscopic instruments. A total of 83 members responded, coming from 33 different countries. Twenty three percent of the respondents using SLI, were using the instruments routinely and of these 21% had not received any formal training in advance of using the instruments in real patients. Of all responding EAES members, 41% considered the instruments to potentially compromise patient safety due to their complexity, learning curve and the inexperience of the surgeons. The respondents reported the three most important aspects of a possible steerable laparoscopic instruments training curriculum to be: hands-on training, safe tissue handling and suturing practice. Finally, a major part of the respondents consider force/pressure feedback data to be of significant importance for implementation of training and assessment of safe laparoscopic and robotic surgery. Training and assessment of skills regarding safe implementation of steerable laparoscopic instruments is lacking. The respondents stressed the need for specific hands-on training during which feedback and assessment of skills should be guaranteed before operating on real patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Since the late 1980s, robot-assisted surgery (RAS) has been gaining ground and has become the standard of care for several complex surgical procedures [1,2,3,4,5,6,7]. One of the advantages of RAS is the use of (distally) articulating robotic instruments which increase the degrees of freedom. However, due to the high acquisition and operating costs of RAS, the desire for a more affordable alternative has increased [8,9,10]. These more affordable alternatives should benefit both the patient and the surgeon [11, 12]. Consequently, hand held steerable laparoscopic instruments (SLI) were developed, offering part of the benefits that the robotic instruments have, but with reduction of the overall costs [10, 13, 14]. In recent years, the usage of SLI increased predominantly as a result of the interest in single-incision laparoscopy and the improved ergonomics for the surgeon’s hand compared to conventional laparoscopic instruments [15,16,17,18].
The benefits and drawbacks of steerable instruments have been extensively reported in previous studies [15, 18,19,20]. Steerable instruments improve the range of motion and increase the degrees of freedom. Furthermore, by increasing the degree of freedom the physical strain and musculoskeletal pain of the surgeon’s upper extremities decreased. [15, 21, 22]. Training courses with box trainers and virtual reality trainers using conventional laparoscopic instruments improve surgical skills [23,24,25,26]. However, the complexity of the SLI may result in a more shallow learning curve and, therefore, may require additional training to pursue mastery of skills. The angular amplification of the instrument tip and the more complex handle controls due to the increased degrees of freedom could overwhelm the surgeon and cause an initial longer training process [21, 27].
The aim of this study consisted of surveying members of the European Association of Endoscopic Surgery (EAES) to analyze and provide the current state of interest in the usage of steerable instruments. Moreover, we determined the current perceptions and use of the steerable instruments in daily practice and the type of training which has been conducted prior to using the instruments during laparoscopic surgery.
Methods
An online survey was conducted using a questionnaire designed and distributed by the European Association of Endoscopic Surgery (EAES) Executive Office to all active members of the EAES. The survey was conducted between January 4th and February 3rd, 2020. The survey consisted of 14 questions, presented in Table 1, regarding the usage and training of steerable laparoscopic instruments. Furthermore, the questions were designed to determine the opinion regarding objective assessment of the surgical performance with steerable instruments. GraphPad (Prism 9.0.0, San Diego, California USA) was used for frequency distribution and to generate the graphs. This anonymous survey was exempt from IRB approval.
Results
A total of 83 (out of 3582) active members, of whom 80 were practicing surgeons, responded. The respondents originated from 33 countries, with the highest proportion from the Netherlands (14%), Italy (11%) and the United Kingdom (6%). The respondents held a position either as a surgeon (94%), a fellow (1%), or a resident (5%).
The vast majority of 75 participants (90%) was interested in using SLI during surgery in the OR (Fig. 1). Of the respondents, 61 (74%) had previously utilized a new SLI in the OR, but less than 5 times, 9 (11%) responded 5–10 times, and 12 (15%) confirmed they had used SLI more than 20 times in the OR (Fig. 2).
Of all surgeons who used SLI in the OR, 23% used it routinely, and most commonly to perform colorectal surgery procedures. When asked about the brand and company of the previously used SLI, the members responded with 23 different brands and companies, of which 17% Karl Storz SE & Co. KG (Tuttlingen, Germany), 17% Medtronic plc (Dublin, Ireland), 14% Alphatron Surgical B.V. (Rotterdam, The Netherlands) and 10% Tuebingen Scientific Medical GmbH (Tuebingen, Germany) were the most common (Fig. 3).
Twenty three percent of the respondents using SLI, were using SLI routinely and of this group twenty one percent had not received any specific training in advance of using the SLI in the OR (Fig. 4). If the participant had received training, the three most common types of training consisted of: demonstration by instructor (34%), hands-on box training (31%) and theoretical training (eLearning, instruction form or booklet) (17%) (Fig. 5). Regarding potential risks of SLI concerning patient safety, 46% of the respondents foresaw no risk. Yet, 41% of respondents considered patient safety to be compromised with the introduction of SLI. The most frequent argument given for no risk was that before using SLI training is essential and only a good trained surgeon should perform surgery with steerable instruments and thus reducing the risk. The most common mentioned reason for potential risks consisted of the difficult and shallow learning curve and the lack of experience of the surgeons.
The three most reported aspects of training for steerable laparoscopic instruments were tissue handling, hands-on training and suturing practice. Fifty respondents (60%) reported that force/pressure data, with regard to tissue handling skills, is of significant importance for the assessment of safe laparoscopic surgery in and outside of the OR. In addition, 56 out of 83 respondents (67%) answered that it is necessary to have force/pressure data integrated during robotic surgery for training and/or clinical routine.
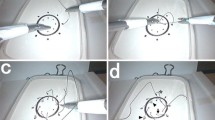
Below listed the most frequently mentioned manufacturers and instruments (Fig. 3), a short example that was provided by the respondents and the number (%) of users.
1. Karl Storz SE & Co. KG (Tuttlingen, Germany) (Fig. 3A), Articulating Needle Holder (17%).
2. Medtronic plc (Dublin, Ireland) (Fig. 3B), Covidien SILS™ Stitch articulating suturing device (17%).
3. Alphatron Surgical B.V. (Rotterdam, The Netherlands) (Fig. 3C), FlexDex system (14%).
4. Tuebingen Scientific Medical GmbH (Tuebingen, Germany) (Fig. 3D), Radius surgical system (10%).
5. B. Braun (Melsungen, Germany) (Fig. 3E), Caiman® 5 Articulating Maryland (3%).
6. Deam Products B.V. (Roden, The Netherlands) (Fig. 3F), LaproFlex (3%).
7. Johnson & Johnson (New Brunswick, New Jersey, United States) (Fig. 3G), ENSEAL G2 Articulating Tissue Sealer (3%).
Discussion
This study, conducted with an questionnaire among EAES members, provided insight and perceptions regarding the implementation and adoption of SLI. Moreover, the results indicate to what extent specific skills for SLI have been trained and assessed before operating on real patients. The vast majority of the respondents had interest in using steerable instruments. However, only a small fraction was using the steerable laparoscopic instruments routinely. Furthermore, twenty one percent of this group did not receive any form of prior training regarding steerable laparoscopic instruments. The respondents that did receive training, replied that the training consisted mainly of demonstration by an instructor or hands-on box training.
The majority of responding EAES members raised concerns on risks for patient safety, due to a shallow learning curve and the inexperience of the surgeon, when introducing the use of SLI. With this in mind the respondents determined the three most important aspects of steerable laparoscopic instruments to be: safe tissue handling, hands-on training and suturing practice. Furthermore, there was consensus among the respondents on the use of force-based feedback on tissue handling skills and its importance for the assessment of safe laparoscopic surgery. This same consensus, regarding the force/pressure data, consists for robotic surgery training.
Previous studies have compared conventional and steerable laparoscopic instruments in performance, ergonomics, learning curve and (the lack of) training [15, 18, 27, 28]. Santos et al. [28] compared two groups of medical students (n = 45) with one group receiving laparoscopic training with conventional instruments, and the other group receiving single-incision laparoscopy training with articulating instruments. The groups performed laparoscopic and single incision laparoscopic peg transfer and pattern cutting tasks. The learning curve for the articulating instruments was longer compared to conventional instruments and the performance with conventional instruments was superior. Besides, Uysal et al. (2020) [27] performed a randomized cross-over study with fifty laparoscopic novices comparing conventional and articulating laparoscopic instruments in completing the European training in basic laparoscopic urological skills (E-BLUS). The conventional laparoscopic instruments group had a better performance, with the longer learning curve of the articulating instruments being one of the possible reasons for this outcome. Corker et al. [18] compared articulating versus conventional instruments and also the combination of both instruments. This study consisted of three groups of surgeons with different combinations of instruments (n = 21): two articulating instruments, two conventional, and a combination of both. The groups performed a peg transfer task and a pattern-cutting task. The group with one articulating and one conventional laparoscopic instrument performed best in the peg transfer task. Finally, Sánchez-Margallo et al. [15] performed a study comparing six laparoscopic surgeons while using both conventional and a handheld motor-driven laparoscopic needle holder during three different suturing tasks. In this study, no significant differences were observed between the instruments regarding performance. However, the SLI did result in better outcomes with regards to ergonomics.
A limitation of this study is possible participation bias. EAES members who are more interested in SLI are more likely to participate in the survey, this also follows from the responses as ninety percent of the respondents was interested in SLI. Furthermore, a relatively small number of EAES members participated in the survey. A strength of this survey is the diversity in the country of origin of the respondents providing a variety in experience. Moreover, the respondents had experience with a large variety of SLI brands and, therefore, contributing to the survey with a more diverse experience.
Mainly driven by the large interest in SLI combined with an indicated uncertainty in the ability to safely control the instruments during complex surgical tasks as tissue manipulation or suturing, it is advisable to develop training initiatives for technical skills training and assessment specific for SLI. This training should allow residents and surgeons to practice with any type of SLI in a realistic setting using for example a physical hands-on trainer to overcome the learning curve for these instruments. Based on our previous results [26, 29, 30] and based on the outcomes of this present study, the training system ideally provides objective performance feedback that reflect safe tissue handling. Doing so, surgeons can train new specific technical skills to control SLI. Adequate assessment of tissue interaction forces and unintentional errors at the end of training may reduce exerted forces and minimize tissue trauma when first utilizing SLI in real patients. [26, 30, 31]
Conclusion
Training and assessment of technical skills for safe use of steerable laparoscopic instruments is lacking. Despite the large interest in these instrument, there are limited training initiatives and few surgeons have been trained sufficiently. According to the responding EAES members in this study, hands-on box trainers must be used for training of specific technical skills. Moreover, the respondents stressed the importance of objective force-based feedback to train safe handling of tissues before operating on real patients.
References
Lane T (2018) A short history of robotic surgery. Ann R Coll Surg Engl 100:5–7. https://doi.org/10.1308/rcsann.supp1.5
George EI, Brand TC, LaPorta A, Marescaux J, Satava RM (2018) Origins of robotic surgery: from skepticism to standard of care. JSLS J Soc Laparoendosc Surg. https://doi.org/10.4293/JSLS.2018.00039
Chopra S, Srivastava A, Tewari A (2012) Robotic radical prostatectomy: the new gold standard, Arab. J Urol 10:23–31. https://doi.org/10.1016/j.aju.2011.12.005
Stafford AT, Walsh RM (2015) Robotic surgery of the pancreas: the current state of the art. J Surg Oncol 112:289–294. https://doi.org/10.1002/jso.23952
Shay SG, Chrin JD, Wang MB, Mendelsohn AH (2019) Initial and long-term retention of robotic technical skills in an otolaryngology residency program. Laryngoscope 129:1380–1385. https://doi.org/10.1002/lary.27425
Health Quality Ontario (2010) Robotic-assisted minimally invasive surgery for gynecologic and urologic oncology: an evidence-based analysis. Ont Health Technol Assess Ser 10: 1–118. http://www.ncbi.nlm.nih.gov/pubmed/23074405 (Accessed January 31, 2021).
Willuth E, Hardon SF, Lang F, Haney CM, Felinska EA, Kowalewski KF, Müller-Stich BP, Horeman T, Nickel F (2021) Robotic-assisted cholecystectomy is superior to laparoscopic cholecystectomy in the initial training for surgical novices in an ex vivo porcine model: a randomized crossover study. Surg Endosc. https://doi.org/10.1007/s00464-021-08373-6
Patel HRH, Linares A, Joseph JV (2009) Robotic and laparoscopic surgery: cost and training. Surg Oncol 18:242–246. https://doi.org/10.1016/j.suronc.2009.02.007
Childers CP, Maggard-Gibbons M (2018) Estimation of the acquisition and operating costs for robotic surgery. JAMA J Am Med Assoc 320:835–836. https://doi.org/10.1001/jama.2018.9219
Lacitignola L, Trisciuzzi R, Imperante A, Fracassi L, Crovace AM, Staffieri F (2020) Comparison of laparoscopic steerable instruments performed by expert surgeons and novices. Vet Sci. https://doi.org/10.3390/VETSCI7030135
Siddaiah-Subramanya M, Tiang K, Nyandowe M (2017) A new era of minimally invasive surgery: progress and development of major technical innovations in general surgery over the last decade. Surg J 03:e163–e166. https://doi.org/10.1055/s-0037-1608651
Buia A, Stockhausen F, Hanisch E (2015) Laparoscopic surgery: a qualified systematic review. World J Methodol 5:238. https://doi.org/10.5662/wjm.v5.i4.238
Anderson PL, Lathrop RA, Webster RJ (2016) Robot-like dexterity without computers and motors: a review of hand-held laparoscopic instruments with wrist-like tip articulation. Expert Rev Med Devices 13:661–672. https://doi.org/10.1586/17434440.2016.1146585
Romanelli JR, Earle DB (2009) Single-port laparoscopic surgery: an overview. Surg Endosc 23:1419–1427. https://doi.org/10.1007/s00464-009-0463-x
Sánchez-Margallo JA, Sánchez-Margallo FM (2017) Initial experience using a robotic-driven laparoscopic needle holder with ergonomic handle: assessment of surgeons’ task performance and ergonomics. Int J Comput Assist Radiol Surg 12:2069–2077. https://doi.org/10.1007/s11548-017-1636-z
Supe AN, Kulkarni GV, Supe PA (2010) Ergonomics in laparoscopic surgery. J Minim Access Surg 6:31–36. https://doi.org/10.4103/0972-9941.65161
Yu D, Lowndes B, Morrow M, Kaufman K, Bingener J, Hallbeck S (2016) Impact of novel shift handle laparoscopic tool on wrist ergonomics and task performance. Surg Endosc 30:3480–3490. https://doi.org/10.1007/s00464-015-4634-7
Corker HP, Singh P, Sodergren MH, Balaji S, Kwasnicki RM, Darzi AW, Paraskeva P (2015) A randomized controlled study to establish the effect of articulating instruments on performance in single-incision laparoscopic surgery. J Surg Educ 72:1–7. https://doi.org/10.1016/j.jsurg.2014.08.004
Chow G, Chiu CJ, Zheng B, Panton ON, Meneghetti AT (2016) Rigid vs articulating instrumentation for task completion in single-port surgery. Am J Surg 211:903–907. https://doi.org/10.1016/j.amjsurg.2016.01.017
Hardon SF, Schilder F, Bonjer J, Dankelman J, Horeman T (2019) A new modular mechanism that allows full detachability and cleaning of steerable laparoscopic instruments. Surg Endosc 33:3484–3493. https://doi.org/10.1007/s00464-019-06849-0
Dewaele F, De Pauw T, Kalmar A, Pattyn P, Van Herzeele I, Mottrie A, Van Nieuwenhove Y, Van Roost D (2019) Is the human brain capable of controlling seven degrees of freedom? J Surg Res 238:1–9. https://doi.org/10.1016/j.jss.2019.01.005
Wee IJY, Kuo LJ, Ngu JCY (2020) A systematic review of the true benefit of robotic surgery: ergonomics. J Med Robot Comput Assist Surg Int. https://doi.org/10.1002/rcs.2113
Dhariwal A, Prabhu R, Dalvi A, Supe A (2007) Effectiveness of box trainers in laparoscopic training. J Minim Access Surg 3:57–63. https://doi.org/10.4103/0972-9941.33274
Mohammadi Y, Lerner MA, Sethi AS, Sundaram CP (2010) Comparison of laparoscopy training using the box trainer versus the virtual trainer. J Soc Laparoendosc Surg 14:205–212. https://doi.org/10.4293/108680810X12785289144115
Willaert W, Van De Putte D, Van Renterghem K, Van Nieuwenhove Y, Ceelen W, Pattyn P (2013) Training models in laparoscopy: a systematic review comparing their effectiveness in learning surgical skills. Acta Chir Belg 113:77–95. https://doi.org/10.1080/00015458.2013.11680892
Hardon SF, Horeman T, Bonjer HJ, Meijerink WJHJ (2018) Force-based learning curve tracking in fundamental laparoscopic skills training. Surg Endosc 32:3609–3621. https://doi.org/10.1007/s00464-018-6090-7
Uysal D, Gasch C, Behnisch R, Nickel F, Müller-Stich BP, Hohenfellner M, Teber D (2020) Evaluation of new motorized articulating laparoscopic instruments by laparoscopic novices using a standardized laparoscopic skills curriculum. Surg Endosc 1:3. https://doi.org/10.1007/s00464-020-08086-2
Santos BF, Reif TJ, Soper NJ, Hungness ES (2011) Effect of training and instrument type on performance in single-incision laparoscopy: results of a randomized comparison using a surgical simulator. Surg Endosc 25:3798–3804. https://doi.org/10.1007/s00464-011-1791-1
Horeman T, Dankelman J, Jansen FW, Van Den Dobbelsteen JJ (2014) Assessment of laparoscopic skills based on force and motion parameters. IEEE Trans Biomed Eng 61:805–813. https://doi.org/10.1109/TBME.2013.2290052
Horeman T, Van Delft F, Blikkendaal MD, Dankelman J, Van Den Dobbelsteen JJ, Jansen FW (2014) Learning from visual force feedback in box trainers: tissue manipulation in laparoscopic surgery. Surg Endosc. https://doi.org/10.1007/s00464-014-3425-x
Smit D, Spruit E, Dankelman J, Tuijthof G, Hamming J, Horeman T (2017) Improving training of laparoscopic tissue manipulation skills using various visual force feedback types. Surg Endosc 31:299–308. https://doi.org/10.1007/s00464-016-4972-0
Acknowledgements
The authors sincerely thank all responding surgeons for their contribution.
Funding
Not applicable.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
Drs. Sem Hardon, Masie Rahimi, Roelf Postema, Estelle Willuth, Yoav Mintz, Alberto Arezzo and Prof. Jenny Dankelman have no conflict of interest or financial ties to disclose. Dr. Felix Nickel reports receiving travel support for conference participation as well as equipment provided for laparoscopic surgery courses by Karl Storz, Johnson & Johnson, Intuitive Surgical, Cambridge Medical Robotics, and Medtronic. Dr. ir. Tim Horeman is founder and shareholder of the TU-Delft MedTech startup Medishield Delft BV.
Ethical approval
Not applicable.
Research involving human participants and/or animals
Not applicable.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hardon, S.F., Rahimi, A.M., Postema, R.R. et al. Safe implementation of hand held steerable laparoscopic instruments: a survey among EAES surgeons. Updates Surg 74, 1749–1754 (2022). https://doi.org/10.1007/s13304-022-01258-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-022-01258-w