Abstract
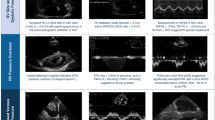
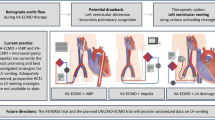
Fulminant myocarditis is one of the most challenging diseases. We sought to examine the outcomes of our multidisciplinary treatment strategy for fulminant myocarditis. A retrospective review of consecutive 30 patients with fulminant myocarditis was conducted. Of the 30 patients, 25 required mechanical circulatory support (MCS). Percutaneous extracorporeal membrane oxygenation (ECMO) was the first-line therapy to rescue the patients and inserted in 23 of them. The other 2 were implanted with temporary ventricular assist device (t-VAD) with extracorporeal centrifugal pump(s). Sixteen of the ECMO-supported patients were later transitioned to t-VAD. Of the 18 patients who underwent t-VAD support, heart function recovered and the VAD was explanted in 10. Four patients were bridged to long-term VAD and the other 4 died on t-VAD. Two patients were directly bridged to long-term VAD by ECMO. Heart function recovered only with ECMO in 4 patients and 1 died on ECMO. Overall survival rate was 83.3%. The duration of ECMO support significantly correlated with total bilirubin level, which was a significant risk factor for mortality. Pathologically, 7 patients (23.3%) had eosinophilic myocarditis and 1 (3.3%) had giant-cell myocarditis, and all the 8 patients underwent immunosuppressive therapy including steroids. Heart function recovered to normal level in 7 of them (87.5%). Timely conversion from the percutaneous ECMO to the temporary VAD before elevation of total bilirubin level is crucial for improving the clinical outcomes. Endomyocardial biopsy is needed to be done as soon as possible, because immunosuppressive therapy carries promising outcomes in certain etiologies.





Similar content being viewed by others
References
Maisch B, Pankuweit S. Standard and etiology-directed evidence-based therapies in myocarditis: state of the art and future perspectives. Heart Fail Rev. 2013;18:761–95.
Heart Failure Society of America. HFSA guidelines for the management of patients with heart failure due to left ventricular systolic dysfunction: pharmacological approaches. Congest Heart Fail. 2000;6:11–39.
Japanese Circulation Society Task Force Committee on Acute and Chronic Myocarditis. Guidelines for diagnosis and treatment of myocarditis (JCS 2009). http://www.j-circ.or.jp/guideline/pdf/JCS 2009_izumi_h.pdf. Accessed 13 Dec 2017.
McCarthy RE 3rd, Boehmer JP, Hruban RH, et al. Long-term outcome of fulminant myocarditis as compared with acute (nonfulminant) myocarditis. N Engl J Med. 2000;342:690–5.
De Robertis F, Birks EJ, Rogers P, Dreyfus G, Repper JR, Khaghani A. Clinical performance with the levitronix centrimag short-term ventricular assist device. J Heart Lung Transpl. 2006;25:181–6.
De Robertis F, Rogers P, Amrani M, et al. Bridge to decision using the levitronix centrimag short-term ventricular assist device. J Heart Lung Transpl. 2008;27:474–8.
Aretz HT, Billingham ME, Edwards WD, et al. Myocarditis: a histopathologic definition and classification. Am J Cardiovasc Pathol. 1987;1:3–14.
Asaumi Y, Yasuda S, Morii I, et al. Favourable clinical outcome in patients with cardiogenic shock due to fulminant myocarditis supported by percutaneous extracorporeal membrane oxygenation. Eur Heart J. 2005;26:2185e92.
Mirabel M, Luyt CE, Leprince P, et al. Outcomes, long-term quality of life, and psychologic assessment of fulminant myocarditis patients rescued by mechanical circulatory support. Crit Care Med. 2011;39:1029e35.
Saito S, Nakatani T, Kobayashi J, et al. Is extracorporeal life support contraindicated in elderly patinets? Ann Thorac Surg. 2007;83:140–5.
Acker MA. Mechanical circulatory support for patientswith acute-fulminant myocarditis. Ann Thorac Surg. 2001;71:S73–6.
Ginsberg F, Parrillo JE. Fulminant myocarditis. Critic Care Clin. 2013;29:465–83.
Mody KP, Takayama H, Landes E, et al. Acute mechanical circulatory support for fulminant myocarditis complicated by cardiogenic shock. J Cardiovasc Trans Res. 2014;7:156–64.
Saito S, Fleischer B, Maeß C, Baraki H, Kutschka I. Minimally invasive implantation of an extracorporeal membrane oxygenation circuit used as a temporary left ventricular assist device: a new concept for bridging to permanent cardiac support. J Artif Organs. 2015;18:95–8.
Mason JW, O’Connell JB, Herskowitz A, et al. A clinical trial of immunosuppressive therapy for myocarditis. The myocarditis treatment trial investigators. N Engl J Med. 1995;333:269–75.
Cooper LT Jr. Myocarditis. N Engl J Med. 2009;360:1526–38.
Kirklin JK, Naftel DC, Pagani FD, et al. Seventh INTERMACS annual report: 15,000 patients and counting. J Heart Lung Transplant 2015;34;1495–504.
Kawano S, Kato J, Kawano N, et al. Clinical features and outcomes of eosinophilic myocarditis patients treated with prednisolone at a single institution over a 27-year period. Intern Med. 2011;50:975–81.
Arima M, Kanoh T. Eosinophilic myocarditis associated with dense deposits of eosinophil cationic protein (ECP) in endomyocardium with high serum ECP. Heart. 1999;81:669–75.
Tai PC, Ackerman SJ, Spry CJF, Dunnette S, Olsen EGJ, Gleich GJ. Deposits of eosinophil granule proteins in cardiac tissues of patients with eosinophilic endomyocardial disease. Lancet. 1987;8534:643–7.
Arima M, Kanoh T, Kawano Y, Oigawa T, Yamagami S, Matsuda S. Serum levels of eosinophilic cationic protein in patients with eosinophilic myocarditis. Int J Cardiol. 2002;84:97–9.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare no conflict of interest associated with this study.
Rights and permissions
About this article
Cite this article
Saito, S., Toda, K., Miyagawa, S. et al. Diagnosis, medical treatment, and stepwise mechanical circulatory support for fulminat myocarditis. J Artif Organs 21, 172–179 (2018). https://doi.org/10.1007/s10047-017-1011-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-017-1011-4