Abstract
Background
There is limited evidence on the transferability of conventional laparoscopic and open surgical skills to robotic-assisted surgery. The primary aim of this study was to evaluate the transferability of expertise in conventional laparoscopy and open surgery to robotic-assisted surgery using the da Vinci Skills Simulator (dVSS). Secondary aims included evaluating the influence of individual participants’ characteristics.
Methods
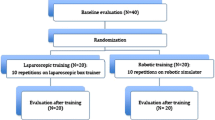
Participants performed four tasks on the dVSS: Peg Board 1 (PB), Pick and Place (PP), Thread the Rings (TR), and Suture Sponge 1 (SS). Participants were classified into three groups (Novice, Intermediate, Experts) according to experience in laparoscopic and open surgery. All tasks were performed twice except for SS. Performance was assessed using the built-in scoring system.
Results
37 medical students and 25 surgeons participated. Experts did not perform significantly better than less experienced participants on the dVSS. Specifically, with regard to laparoscopic experience, total simulator scores were: Novices 68.2 ± 28.8; Intermediates 65.1 ± 31.2; Experts 65.1 ± 30.0; p = 0.611. Regarding open surgical experience, scores were: Novices 68.6 ± 28.7; Intermediates 68.2 ± 30.8; Experts 63.2 ± 30.3; p = 0.305. Although there were some significant differences among groups for single parameters in specific tasks, there was no constant superiority of one group. Laparoscopic and open surgical Novices improved significantly in overall score and time for all three tasks (p < 0.05). Laparoscopic intermediates improved only in PP time (4.64 ± 3.42; p = 0.006), open Intermediates in PB score (11.98 ± 13.01; p = 0.025), and open Experts in PP score (6.69 ± 11.48; p = 0.048). Laparoscopic experts showed no improvement. Participants with gaming experience had better overall scores than non-gamers when comparing all second attempts (Gamer 83.62 ± 7.57; Non-Gamer 76.31 ± 12.78; p = 0.008) as well as first and second attempts together (Gamer 72.08 ± 8.86; Non-Gamer 65.45 ± 11.68; p = 0.039). Musical and sports experience showed no correlation with robotic performance.
Conclusions
Robotic-assisted surgery requires skills distinct from conventional laparoscopy or open surgery. Basic robotic skills training prior to patient contact should be required.






Similar content being viewed by others
References
Himpens J, Leman G, Cadiere GB (1998) Telesurgical laparoscopic cholecystectomy. Surg Endosc 12(8):1091–1091. https://doi.org/10.1007/s004649900788
Sood A, Jeong W, Peabody JO, Hemal AK, Menon M (2014) Robot-assisted radical prostatectomy: inching toward gold standard. Urol Clin North Am 41(4):473–484
Nguyen KT, Zureikat AH, Chalikonda S, Bartlett DL, Moser AJ, Zeh HJ (2011) Technical aspects of robotic-assisted pancreaticoduodenectomy (RAPD). J Gastrointest Surg 15(5):870–875
Hogg ME, Tam V, Zenati M, Novak S, Miller J, Zureikat AH, Zeh HJ 3rd (2017) Mastery-based virtual reality robotic simulation curriculum: the first step toward operative robotic proficiency. J Surg Educ 74(3):477–485. https://doi.org/10.1016/j.jsurg.2016.10.015
Hanly EJ, Talamini MA (2004) Robotic abdominal surgery. Am J Surg 188(4):19–26
Rashid T, Kini M, Ind T (2010) Comparing the learning curve for robotically assisted and straight stick laparoscopic procedures in surgical novices. Int J Med Robot Comput Assist Surg 6(3):306–310
Yohannes P, Rotariu P, Pinto P, Smith AD, Lee BR (2002) Comparison of robotic versus laparoscopic skills: is there a difference in the learning curve? Urology 60(1):39–45
Miskovic D, Ni M, Wyles SM, Parvaiz A, Hanna GB (2012) Observational clinical human reliability analysis (OCHRA) for competency assessment in laparoscopic colorectal surgery at the specialist level. Surg Endosc 26(3):796–803. https://doi.org/10.1007/s00464-011-1955-z
Miskovic D, Ni M, Wyles SM, Kennedy RH, Francis NK, Parvaiz A, Cunningham C, Rockall TA, Gudgeon AM, Coleman MG, Hanna GB (2013) Is competency assessment at the specialist level achievable? A study for the national training programme in laparoscopic colorectal surgery in England. Ann Surg 257(3):476–482. https://doi.org/10.1097/SLA.0b013e318275b72a
Roch PJ, Rangnick HM, Brzoska JA, Benner L, Kowalewski KF, Muller PC, Kenngott HG, Muller-Stich BP, Nickel F (2017) Impact of visual-spatial ability on laparoscopic camera navigation training. Surg Endosc. https://doi.org/10.1007/s00464-017-5789-1
Carter FJ, Schijven MP, Aggarwal R, Grantcharov T, Francis NK, Hanna GB, Jakimowicz JJ (2006) Consensus guidelines for validation of virtual reality surgical simulators. Simul Healthc 1(3):171–179. https://doi.org/10.1097/01.sih.0000244452.43542.47
Hendrie JD, Nickel F, Bruckner T, Kowalewski KF, Garrow CR, Mantel M, Romero P, Muller-Stich BP (2016) Sequential learning of psychomotor and visuospatial skills for laparoscopic suturing and knot tying - study protocol for a randomized controlled trial “The shoebox study”. Trials 17(1):14. https://doi.org/10.1186/s13063-015-1145-8
Nickel F, Kowalewski KF, Rehberger F, Hendrie JD, Mayer BF, Kenngott HG, Bintintan V, Linke GR, Fischer L, Müller-Stich BP (2016) Face validity of the pulsatile organ perfusion trainer for laparoscopic cholecystectomy. Surg Endosc. https://doi.org/10.1007/s00464-016-5025-4
Nickel F, Brzoska JA, Gondan M, Rangnick HM, Chu J, Kenngott HG, Linke GR, Kadmon M, Fischer L, Muller-Stich BP (2015) Virtual reality training versus blended learning of laparoscopic cholecystectomy: a randomized controlled trial with laparoscopic novices. Medicine (Baltimore) 94(20):e764. https://doi.org/10.1097/md.0000000000000764
Kelly DC, Margules AC, Kundavaram CR, Narins H, Gomella LG, Trabulsi EJ, Lallas CD (2012) Face, content, and construct validation of the da Vinci Skills Simulator. Urology 79(5):1068–1072. https://doi.org/10.1016/j.urology.2012.01.028
Finnegan KT, Meraney AM, Staff I, Shichman SJ (2012) da Vinci Skills Simulator construct validation study: Correlation of prior robotic experience with overall score and time score simulator performance. Urology 80(2):330–336. https://doi.org/10.1016/j.urology.2012.02.059
Badurdeen S, Abdul-Samad O, Story G, Wilson C, Down S, Harris A (2010) Nintendo Wii video-gaming ability predicts laparoscopic skill. Surg Endosc 24(8):1824–1828
Madan AK, Frantzides CT, Park WC, Tebbit CL, Kumari NVA, O’Leary PJ (2005) Predicting baseline laparoscopic surgery skills. Surg Endosc Other Interv Tech 19(1):101–104. https://doi.org/10.1007/s00464-004-8123-7
Berkley J (2011) Automated Support for da Vinci Surgical System. DTIC Document
Teishima J, Hattori M, Inoue S, Ikeda K, Hieda K, Miyamoto K, Shoji K, Hayashi T, Kobayashi K, Kajiwara M, Egi H, Ohdan H, Matsubara A (2012) Impact of laparoscopic experience on the proficiency gain of urologic surgeons in robot-assisted surgery. J Endourol 26(12):1635–1638. https://doi.org/10.1089/end.2012.0308
Graafland M, Schraagen JM, Boermeester MA, Bemelman WA, Schijven MP (2015) Training situational awareness to reduce surgical errors in the operating room. Br J Surg 102(1):16–23. https://doi.org/10.1002/bjs.9643
Birkmeyer JD, Finks JF, O’Reilly A, Oerline M, Carlin AM, Nunn AR, Dimick J, Banerjee M, Birkmeyer NJ, Michigan Bariatric Surgery Collaborative (2013) Surgical skill and complication rates after bariatric surgery. N Engl J Med 369 (15):1434–1442. https://doi.org/10.1056/NEJMsa1300625
Francis NK, Hanna GB, Cuschieri A (2002) The performance of master surgeons on the advanced dundee endoscopic psychomotor tester: contrast validity study. Arch Surg 137(7):841–844
Stefanidis D, Hope WW, Scott DJ (2011) Robotic suturing on the FLS model possesses construct validity, is less physically demanding, and is favored by more surgeons compared with laparoscopy. Surg Endosc 25(7):2141–2146. https://doi.org/10.1007/s00464-010-1512-1
Ahlering TE, Skarecky D, Lee D, Clayman RV (2003) Successful transfer of open surgical skills to a laparoscopic environment using a robotic interface: initial experience with laparoscopic radical prostatectomy. J Urol 170(5):1738–1741
Brown DC, Miskovic D, Tang B, Hanna GB (2010) Impact of established skills in open surgery on the proficiency gain process for laparoscopic surgery. Surg Endosc 24(6):1420–1426. https://doi.org/10.1007/s00464-009-0792-9
Szold A, Bergamaschi R, Broeders I, Dankelman J, Forgione A, Lango T, Melzer A, Mintz Y, Morales-Conde S, Rhodes M, Satava R, Tang CN, Vilallonga R, European Association of Endoscopic Surgery (2015) European Association of Endoscopic Surgeons (EAES) consensus statement on the use of robotics in general surgery. Surg Endosc 29 (2):253–288. https://doi.org/10.1007/s00464-014-3916-9
Bahler CD, Sundaram CP (2014) Training in robotic surgery: simulators, surgery, and credentialing. Urol Clin N Am 41(4):581–589. https://doi.org/10.1016/j.ucl.2014.07.012
Herron DM, Marohn M (2008) A consensus document on robotic surgery. Surg Endosc 22(2):313–325. https://doi.org/10.1007/s00464-007-9727-5. (discussion 311–312)
Nickel F, Kowalewski KF, Muller-Stich BP (2015) Risk awareness and training for prevention of complications in minimally invasive surgery. Chirurg. https://doi.org/10.1007/s00104-015-0097-6
Brinkman WM, Luursema JM, Kengen B, Schout BM, Witjes JA, Bekkers RL (2013) da Vinci skills simulator for assessing learning curve and criterion-based training of robotic basic skills. Urology 81(3):562–566. https://doi.org/10.1016/j.urology.2012.10.020
Olthof E, Nio D, Bemelman WA (2008) The learning curve of robot-assisted laparoscopic surgery. In: Bozovic V (ed) Medical Robotics. I-Tech Education and Publishing, Vienna
Meier M, Horton K, John H (2016) Da Vinci(c) Skills Simulator: is an early selection of talented console surgeons possible? J Robot Surg 10(4):289–296. https://doi.org/10.1007/s11701-016-0616-6
Voelcker-Rehage C, Willimczik K (2006) Motor plasticity in a juggling task in older adults—a developmental study. Age Ageing 35(4):422–427
Harbin AC, Nadhan KS, Mooney JH, Yu D, Kaplan J, McGinley-Hence N, Kim A, Gu Y, Eun DD (2016) Prior video game utilization is associated with improved performance on a robotic skills simulator. J Robot Surg. https://doi.org/10.1007/s11701-016-0657-x
Paschold M, Schröder M, Kauff DW, Gorbauch T, Herzer M, Lang H, Kneist W (2011) Virtual reality laparoscopy: which potential trainee starts with a higher proficiency level? Int J Comput Assist Radiol Surg 6(5):653–662. https://doi.org/10.1007/s11548-010-0542-4
Fanning J, Fenton B, Johnson C, Johnson J, Rehman S (2011) Comparison of teenaged video gamers vs PGY-I residents in obstetrics and gynecology on a laparoscopic simulator. J Minim Invasive Gynecol 18(2):169–172. https://doi.org/10.1016/j.jmig.2010.11.002
Boyle E, Kennedy A-M, Traynor O, Hill AD (2011) Training surgical skills using nonsurgical tasks—can Nintendo Wii™ improve surgical performance? J Surg Educ 68(2):148–154
Giannotti D, Patrizi G, Di Rocco G, Vestri AR, Semproni CP, Fiengo L, Pontone S, Palazzini G, Redler A (2013) Play to become a surgeon: impact of Nintendo Wii training on laparoscopic skills. PLoS ONE 8(2):e57372. https://doi.org/10.1371/journal.pone.0057372
Moglia A, Ferrari V, Morelli L, Ferrari M, Mosca F, Cuschieri A (2016) A systematic review of virtual reality simulators for robot-assisted surgery. Eur Urol 69(6):1065–1080. https://doi.org/10.1016/j.eururo.2015.09.021
Nickel F, Hendrie JD, Bruckner T, Kowalewski KF, Kenngott HG, Muller-Stich BP, Fischer L (2016) Successful learning of surgical liver anatomy in a computer-based teaching module. Int J Comput Assist Radiol Surg. https://doi.org/10.1007/s11548-016-1354-y
Moorthy K, Munz Y, Sarker SK, Darzi A (2003) Objective assessment of technical skills in surgery. BMJ 327(7422):1032–1037. https://doi.org/10.1136/bmj.327.7422.1032
Ramos P, Montez J, Tripp A, Ng CK, Gill IS, Hung AJ (2014) Face, content, construct and concurrent validity of dry laboratory exercises for robotic training using a global assessment tool. BJU Int 113(5):836–842. https://doi.org/10.1111/bju.12559
Acknowledgements
The authors would like to thank Mr. Tilman Schlick from Intuitive Surgical Inc. for access to the dVSS which made the conduction of the study possible.
Funding
The current study was supported by the Heidelberg Surgery Foundation and by the Ministry of Science and Arts of the State Baden Wurttemberg.
Author information
Authors and Affiliations
Contributions
Study conception and design: Kowalewski, Nickel, Müller-Stich, Kenngott. Acquisition of data: Schmidt, Karadza, Romero, Kowalewski. Statistical analysis: Proctor, Pohl, Wennberg. Analysis and interpretation of data: Kowalewski, Schmidt, Wennberg, Proctor, Pohl. Drafting of manuscript: Schmidt, Wennberg, Kowalewski, Karadza, Nickel. Critical revision: Müller-Stich, Kenngott, Nickel, Romero.
Corresponding author
Ethics declarations
Disclosure
Felix Nickel reports receiving travel support for conference participation as well as equipment provided for laparoscopic surgery courses by KARL STORZ, Johnson & Johnson, and Medtronic. Karl-Friedrich Kowalewski, Mona W. Schmidt, Tanja Proctor, Philipp Romero, Erica Wennberg, Emir Karadza Hannes Kenngott, and Beat Müller-Stich have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Kowalewski, KF., Schmidt, M.W., Proctor, T. et al. Skills in minimally invasive and open surgery show limited transferability to robotic surgery: results from a prospective study. Surg Endosc 32, 1656–1667 (2018). https://doi.org/10.1007/s00464-018-6109-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6109-0