Abstract
Background
Although robotic pancreaticoduodenectomy (RPD) has been successfully performed since 2003, its advantages over open pancreaticoduodenectomy (OPD) are still uncertain. The aim of this systematic review and meta-analysis was to compare the clinical outcomes of RPD to those of OPD.
Methods
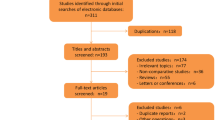
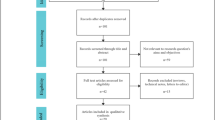
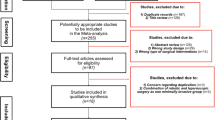
A systematic literature review was performed to identify RPD versus OPD comparative studies published between January 2003 and January 2016. Intraoperative outcomes, post-operative outcomes and oncologic safety were evaluated. Pooled odds ratios (ORs) and weighted mean differences (WMDs) with a 95% confidence interval (95% CI) were calculated using fixed-effect or random-effect models.
Results
Nine non-randomized observational clinical studies involving 680 patients met the inclusion criteria and involved 245 RPDs and 435 OPDs. The overall complication rate was significantly lower in RPD (OR 0.65, 95% CI 0.47–0.91, P = 0.012), as well as the margin positivity rate (OR 0.40, 95% CI 0.20–0.77, P = 0.006), the wound infection rate (OR 0.18, 95% CI 0.06–0.53, P = 0.002) and the length of hospital stay (WMD = −6.00, 95% CI −9.80 to −2.21, P = 0.002). There was no significant difference in the following: the number of lymph nodes harvested; the operation time; the reoperation rate; the incidence of delayed gastric emptying, bile leakage, pancreatic fistula and clinically significant pancreatic fistula; and mortality. The mean conversion rate was 7.3% (range 0–14%).
Conclusions
According to the results of this meta-analysis, RPD is as safe and efficient as OPD and is even favourable in terms of margin-negative resection, overall complication and wound infection rates and length of hospital stay. Given that there have not yet been any high-quality randomized controlled trials (RCTs), the evidence is still limited. Additional prospective, multi-centre RCTs are needed to further define the role of the robotic technique in PD.






Similar content being viewed by others
References
Cameron JL, He J (2015) Two thousand consecutive pancreaticoduodenectomies. J Am Coll Surg 220:530–536
Gagner M, Pomp A (1994) Laparoscopic pylorus-preserving pancreatoduodenectomy. Surg Endosc 8:408–410
Usoh AC, Ammori BJ (2012) Laparoscopic versus open distal pancreatectomy: a systematic review of comparative studies. Surg Endosc 26:904–913
Giulianotti PC, Coratti A, Angelini M, Sbrana F, Cecconi S, Balestracci T, Caravaglios G (2003) Robotics in general surgery: personal experience in a large community hospital. Arch Surg 8:777–784
Buchs NC, Addeo P, Bianco FM, Ayloo S, Benedetti E, Giulianotti PC (2011) Robotic versus open pancreaticoduodenectomy: a comparative study at a single institution. World J Surg 35:2739–2746
Baker EH, Ross SW, Seshadri R, Swan RZ, Iannitti DA, Vrochides D, Martinie JB (2016) Robotic pancreaticoduodenectomy: comparison of complications and cost to the open approach. Int J Med Robot 12:554–560
Bao PQ, Mazirka PO, Watkins KT (2014) Retrospective comparison of robot-assisted minimally invasive versus open pancreaticoduodenectomy for periampullary neoplasms. J Gastrointest Surg 18:682–689
Chalikonda S, Aguilar-Saavedra JR, Walsh RM (2012) Laparoscopic robotic-assisted pancreaticoduodenectomy: a case-matched comparison with open resection. Surg Endosc 26:2397–2402
Chen S, Chen JZ, Zhan Q, Deng XX, Shen BY, Peng CH, Li HW (2015) Robot-assisted laparoscopic versus open pancreaticoduodenectomy: a prospective, matched, mid-term follow-up study. Surg Endosc 29:3698–3711
Hammill C, Cassera M, Swanstrom L, Hansen P (2010) Robotic assistance may provide the technical capability to perform a safe, minimally invasive pancreaticoduodenectomy. HPB 12:198
Lai EC, Yang GP, Tang CN (2012) Robot-assisted laparoscopic pancreaticoduodenectomy versus open pancreaticoduodenectomy—a comparative study. Int J Surg 10:475–479
Walsh M, Chalikonda S, Saavedra JRA (2011) Laparoscopic robotic assisted Whipple: early results of a novel technique and comparison with the standard open procedure. Surg Endosc 25:S221
Zhou NX, Chen JZ, Liu Q, Zhang X, Wang Z, Ren S, Chen XF (2011) Outcomes of pancreatoduodenectomy with robotic surgery versus open surgery. Int J Med Robot 7:131–137
Zhang J, Wu WM, You L, Zhao YP (2013) Robotic versus open pancreatectomy: a systematic review and meta-analysis. Ann Surg Oncol 20:1774–1780
Correa-Gallego C, Dinkelspiel HE, Sulimanoff I, Fisher S, Viñuela EF, Kingham TP, Fong Y, DeMatteo RP, D’Angelica MI, Jarnagin WR, Allen PJ (2014) Minimally-invasive vs open pancreaticoduodenectomy: systematic review and meta-analysis. J Am Coll Surg 218:129–139
Howard TJ, Krug JE, Yu J, Zyromski NJ, Schmidt CM, Jacobson LE, Madura JA, Wiebke EA, Lillemoe KD (2006) A margin-negative R0 resection accomplished with minimal postoperative complications is the surgeon’s contribution to long-term survival in pancreatic cancer. J Gastrointest Surg 10:1338–1345
Rau BM, Moritz K, Schuschan S, Alsfasser G, Prall F, Klar E (2012) R1 resection in pancreatic cancer has significant impact on long-term outcome in standardized pathology modified for routine use. Surgery 152:S103–S111
Jamieson NB, Chan NI, Foulis AK, Dickson EJ, McKay CJ, Carter CR (2013) The prognostic influence of resection margin clearance following pancreaticoduodenectomy for pancreatic ductal adenocarcinoma. J Gastrointest Surg 17:511–521
Fatima J, Schnelldorfer T, Barton J, Wood CM, Wiste HJ, Smyrk TC, Zhang L, Sarr MG, Nagorney DM, Farnell MB (2010) Pancreatoduodenectomy for ductal adenocarcinoma: implications of positive margin on survival. Arch Surg 145:167–172
Chang DK, Johns AL, Merrett ND, Gill AJ, Colvin EK, Scarlett CJ, Scarlett CJ, Nguyen NQ, Leong RW, Cosman PH, Kelly MI, Sutherland RL, Henshall SM, Kench JG, Biankin AV (2009) Margin clearance and outcome in resected pancreatic cancer. J Clin Oncol 27:2855–2862
Pawlik TM, Abdalla EK, Barnett CC, Ahmad SA, Cleary KR, Vauthey JN, Lee JE, Evans DB, Pisters PW (2005) Feasibility of a randomized trial of extended lymphadenectomy for pancreatic cancer. Arch Surg 140:584–589
Slidell MB, Chang DC, Cameron JL, Wolfgang C, Herman JM, Schulick RD, Choti MA, Pawlik TM (2008) Impact of total lymph node count and lymph node ratio on staging and survival after pancreatectomy for pancreatic adenocarcinoma: a large, population-based analysis. Ann Surg Oncol 15:165–174
Lim JE, Chien MW, Earle CC (2003) Prognostic factors following curative resection for pancreatic adenocarcinoma: a population-based, linked database analysis of 396 patients. Ann Surg 237:74–85
Burke EE, Marmor S, Virnig BA, Tuttle TM, Jensen EH (2015) Lymph node evaluation for pancreatic adenocarcinoma and its value as a quality metric. J Gastrointest Surg 19:2162–2170
Nguyen KT, Zureikat AH, Chalikonda S, Bartlett DL, Moser AJ, Zeh HJ (2011) Technical aspects of robotic-assisted pancreaticoduodenectomy (RAPD). J Gastrointest Surg 15:870–875
Waters JA, Canal DF, Wiebke EA, Dumas RP, Beane JD, Aguilar-Saavedra JR, Ball CG, House MG, Zyromski NJ, Nakeeb A, Pitt HA, Lillemoe KD, Schmidt CM (2010) Robotic distal pancreatectomy: cost effective? Surgery 148:814–823
Napoli N, Kauffmann EF, Palmeri M, Miccoli M, Costa F, Vistoli F, Amorese G, Boggi U (2016) The learning curve in robotic pancreaticoduodenectomy. Dig Surg 33:299–307
Nguyen TK, Zenati MS, Boone BA, Steve J, Hogg ME, Bartlett DL, Zeh HJ 3rd, Zureikat AH (2015) Robotic pancreaticoduodenectomy in the presence of aberrant or anomalous hepatic arterial anatomy: safety and oncologic outcomes. HPB (Oxford) 17:594–599
Abdullah SS, Mabrut JY, Garbit V, De La Roche E, Olagne E, Rode A, Morin A, Berthezene Y, Baulieux J, Ducerf C (2006) Anatomical variations of the hepatic artery: study of 932 cases in liver transplantation. Surg Radiol Anat 28:468–473
Stauffer JA, Bridges MD, Turan N, Nguyen JH, Martin JK (2009) Aberrant right hepatic arterial anatomy and pancreaticoduodenectomy: recognition, prevalence and management. HPB 11:161–165
Pugalenthi A, Protic M, Gonen M, Kingham TP, Angelica MI, Dematteo RP, Fong Y, Jarnagin WR, Allen PJ (2016) Postoperative complications and overall survival after pancreaticoduodenectomy for pancreatic ductal adenocarcinoma. J Surg Oncol 113:188–193
Memon S, Heriot AG, Murphy DG, Bressel M, Lynch AC (2012) Robotic versus laparoscopic proctectomy for rectal cancer: a meta-analysis. Ann Surg Oncol 19:2095–2101
Büchler MW, Kleeff J, Friess H (2007) Surgical treatment of pancreatic cancer. J Am Coll Surg 205:S81–S86
Kawai M, Yamaue H (2010) Analysis of clinical trials evaluating complications after pancreaticoduodenectomy: a new era of pancreatic surgery. Surg Today 40:1011–1017
Braham NS, Byrne CJ, Young JM, Solomon MJ (2010) Meta-analysis of well-designed non-randomized comparative studies of surgical procedures is as good as randomized controlled trials. J Clin Epidemiol 63:238–245
Drymousis P, Raptis DA, Spalding D, Fernandez-Cruz L, Menon D, Breitenstein S, Davidson B, Frilling A (2014) Laparoscopic versus open pancreas resection for pancreatic neuroendocrine tumours: a systematic review and meta-analysis. HPB 16:397–406
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Long Peng, Shengrong Lin, Yong Li and Weidong Xiao have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Peng, L., Lin, S., Li, Y. et al. Systematic review and meta-analysis of robotic versus open pancreaticoduodenectomy. Surg Endosc 31, 3085–3097 (2017). https://doi.org/10.1007/s00464-016-5371-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5371-2