Abstract
Background
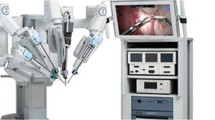
This study investigated the use of robotics to perform extended esophageal resection in a series of patients.
Methods
A total of 14 patients with a median age of 64 years underwent esophagectomy using the da Vinci robot. At presentation, there were 12 cases of cancer, staged at T2N1 (n = 2), T3N0 (n = 2), T3N1 (n = 6), T4N1 (n = 1), and M1a (n = 1); 2 cases of high-grade dysplasia; 8 cases of adenocarcinoma; and 4 cases of squamous cell cancer; as well as 2 middle third, 9 lower third, and one gastroesophageal junction tumor. Nine patients had undergone preoperative chemoradiotherapy, and six had undergone prior abdominal surgery. The patients were categorized into three chronological groups according to the procedure performed. Group 1 consisted of the first three patients in the series, whose surgery was thoracic only (robotically assisted esophagectomy). Group 2, the next three patients, had robotically assisted thoracic esophagectomy plus thoracic duct ligation using a laparoscopic gastric conduit. Group 3, the last eight patients, underwent completely robotic esophagectomy.
Results
For Group 3, the total operating room time was 11.1 ± 0.8 h (range, 11.3–13.2 h), with a console time of 5.0 ± 0.5 h (range, 4.8–5.8 h). The estimated blood loss was 400 ± 300 ml (range, 200–950 ml). One patient in group 1 had a thoracic duct leak. In groups 2 and 3, thoracic duct ligation resulted in no further leaks. Other postoperative complications included severe pneumonia (1 case), atrial fibrillation (5 cases), cervical anastomotic leak (2 cases), wound infection (1 case), and bilateral vocal cord paresis requiring tracheostomy (1 case). In seven of the cases, no intensive care unit time was required. There was one death from pneumonia 72 days after the procedure. The rate of disease-free survival was 87%.
Conclusion
The robotic approach facilitates an extended three-field esophagolymphadenectomy even after induction therapy and abdominal surgery. Larger scale trials are needed to define the role of this technique.
Similar content being viewed by others
Esophagectomy is a palliative and potentially curative treatment for esophageal cancer. As the sole means of therapy, the cure rate of esophagectomy is 10% to 50% [1–9]. A wider periesophageal resection may improve long-term survival [10–13]. Additional chemoradiation has failed to consistently demonstrate superior cure rates. Given the relatively poor long-term survival with surgery alone, chemoradiation without surgery is appealing to some [14].
Minimally invasive esophagectomy has been performed to lessen the biologic impact of surgery and potentially reduce pain and encumbrance. It appears to lower morbidity and mortality with a good outcome [15–18]. To date, few centers have embraced this technique.
As an alternative, robotic engineering may provide the minimally invasive option for a greater number of surgeons and patients. A potentially less oncologic approach, robotic transhiatal esophagectomy has been reported [19]. Mortality, length of hospital stay, morbidity, and outcome are yet to be reported.
In this report, we investigate the use of robotics to perform a two-stage, same-anesthesia esophageal resection with an en bloc three-field lymphadenectomy using a previously described technique: the three-field esophagolymphadenectomy [20]. The procedure consists of a thoracic esophagectomy with a cervical, wide thoracic, and adominal lymphadenectomy in addition to thoracic duct resection and ligation, creation of a 4-cm-wide gastric tube, and jejunostomy feeding tube placement with esophagogastric anastomosis in the left neck. We present our initial experience and the procedure modifications performed in a consecutive series of patients.
Materials and methods
Patients
From November 2002 to November 2003, 14 patients underwent a robotically assisted esophagectomy. In the first six cases, a robot was used to mobilize the thoracic esophagus. In the remaining cases, the procedure was completely robotic. Investigational review board approval was obtained.
All the patients underwent a preoperative computed tomogram (CT) of the chest and upper abdomen, bronchoscopy for middle third tumors, fluorodeoxyglucose positron emission tomography (PET), esophagogastroduodenoscopy, endoscopic ultrasound with fine-needle aspiration of suspicious adenopathy, and reexamination of any pathologic slides not previously examined by our pathologists.
Information concerning patient demographics is presented in Table 1. The T4N1 patient had pleural involvement, and the M1a patient had celiac axis disease.
Operative technique
The 14 patients underwent esophagectomy using the da Vinci computer-assisted surgical system (Intuitive Surgical, Inc., Sunnyvale, CA, USA). Refinements were made during the study period. Chronologically, there were three groups. Group 1 consisted of the first three patients, who underwent the robotic thoracic-only portion of the esophagectomy, which involved resection of the esophagus en bloc with the associated nodes in the thorax and the neck and a laparotomy for the abdominal portion of the procedure. Group 2, the next three patients, underwent esophagectomy as did group 1, with the addition of a thoracic duct ligation and a laparoscopic resection rather than a laparotomy. Group 3, the last eight patients, underwent a completely robotic esophagectomy.
The details and sequence of the “to-date” two-stage procedure used for group 3 are as follows [20]. Figures 1 to 7 illustrate the major steps. The goal of the procedure is wide en bloc resection of the esophagus and periesophageal tissue.
A, B, C Thoracic robotic setup. The chest phase is performed first. Patients are intubated with a double-lumen endotracheal tube, and the body is positioned in the left lateral decubitus position to slightly forward. The right arm is padded and draped over the right ear, and the patient is secured to the operating table. The table then is tilted 30° to 45° from the prone position. The ports are placed as described in the text. Note the position of the monitors, console, instrument table, and console.
Abdominal robotic setup. Six abdominal ports are placed. Before the robot is brought into position, the esophagus is exposed through the left neck incision and encircled with a Penrose drain. A feeding tube is placed just below the level of the umbilicus and the midclavicular line. The stomach is mobilized through the ports. Wide nodal resection is performed, and a gastric tube is created.
Completed procedure. The gastric tube is pulled into the posterior mediastinum using the esophageal specimen as a guide. At the left neck incision, the specimen is resected, and the remaining esophagus is anastomosed to the gastric tube in a triangular side-to-side functional end-to-end completely stapled fashion.
After double-lumen endotracheal intubation and placement of a measured length of nasogastric tube (the distance of the insertion is important later in the procedure so the tube can be pulled back out of the stomach before creation of the gastric conduit), the patients are positioned laterally to slightly face down and strapped securely to the operating table. The right arm is well padded and positioned over the ear with the elbow below the horizontal plane of the right shoulder. The operating table is tilted as far anteriorly as possible so that the patient is 30° to 45° from prone (Fig. 1).
Five puncture wounds are made in the right midanterolateral chest. (Figs. 1 and 4) A 12-mm trocar is placed in the fifth to the sixth intercostal space in the anterior axillary line. A second port, an 8-mm robotic and right arm port, is placed in the posterior axillary line just anterior to the border of the scapula in the third to the fourth intercostal space. A third port, the second 8-mm robotic and left arm port, is placed in the seventh to the eighth intercostal space in the posterior axillary line.
The robot then is brought into position. The robotic arms are placed through the 8-mm trocars, and the 0° videoscope is placed through the 12-mm trocar. Two accessory trocars are placed, both at the level of the anterior axillary line. The first, a 5-mm trocar, is placed at the level of the third intercostal space, and the second, a 12-mm trocar, is placed at the level of the sixth to the seventh intercostal space. The upper trocar is used for suctioning and grasping instruments, whereas the lower trocar is used for access to place a fan retractor for the lung, the suctioning and grasping instruments, and the sutures used for ligation of the thoracic duct. Carbon dioxide (CO2) is insufflated to 10 mmHg of pressure to evacuate cautery smoke and to compress the lung away from the surgical site.
Over the course of the series, new details in the approach were discovered to reduce bleeding and improve the efficiency of the procedure. The order and the details of the surgical resection follow. Initially, the hook cautery and Caudier grasper (Intuitive Surgical) are used to dissect along the anterior aspect of the esophagus just at the pericardial bulge cephalad to the inferior pulmonary vein. The dissection is continued inferiorly to the esophageal hiatus, with the inferior pulmonary ligament and adherent lung taken down as necessary for access to the periesophageal nodes, completely cleaning the pericardium, hiatus, and left pleura. Both hila are cleared of nodal tissue and taken contiguously with the specimen. The periaortic–spinal–azygous nodes and thoracic duct also are taken en bloc. The dissection is continued along the azygous vein, which is preserved when the vein is uninvolved, as determined by CT scan, endoscopic ultrasound, and direct visual assessment. Small lymphatic tributaries seen under high robotic magnification are endoclipped through the accessory port or robotically.
The supra-azygous esophagus and periesophageal tissue are resected into the thoracic apex, well into the neck. First, over the intended resection area, the pleura is scored with the hook cautery. Then the associated peritracheal nodes and the right vagus nerve are transected with the ultrasonic shears (SonoSurg; Olympus, Co., Melville, NY, USA), reducing the potential of electrical transmission to the recurrent laryngeal nerve. The posterior and rightward aspect of the trachea and the thoracic peritracheal and cervical spaces are completely cleaned of periesophageal tissue, and the dissection is continued into the thoracic inlet.
In groups 2 and 3, at the level of the diaphragm, the thoracic duct is triply ligated, encompassing all the tissue beneath the remaining intact pleura between the azygous vein and the aorta with 2-0 Ethibond (Ethicon, Inc., Cincinnati, OH, USA) on an SH needle. At the conclusion of the chest phase, two drains are placed: a 19-Fr round multiholed silastic drain through the lower accessory trocar along the diaphragm and a 15-Fr drain to the superior aspect of the thoracic cavity, through the upper accessory trocar (Fig. 4). The robotic arms then are removed, and the is robot moved away from the patient.
The patient next is positioned supinely and reintubated with a single-lumen endotracheal tube. The head is turned upward and to the patient’s right, exposing the left neck. The upper extremities are placed by the side, and the legs are placed together. After skin preparation and the placement of drapes, a 5-cm transverse incision is made in the left neck 3 cm above the medial left clavicle. The dissection is continued deeply and medially toward the spine, transecting the omohyoid muscle for exposure. The previously mobilized and dissected esophagus is encircled with a Penrose drain, and the incision later is packed with an antibiotic-soaked surgical sponge to prevent the later escape of CO2 from the peritoneal cavity. This initial dissection allows manipulation of the esophagus and unhindered withdrawal of the specimen later in the procedure.
The abdominal phase is performed next. Six puncture wounds in the abdomen are performed, for two 8-mm robotic arm trocars and the 12-mm robotic viewing trocar. A distance of 10 to 12 cm is maintained from either of the robotic arms. Two 5-mm trocars are placed beneath each costal margin in the anterior axillary line, and a 12-mm trocar is placed in the left midclavicular line at the umbilicus level (Fig. 5). The abdomen is inflated to 15 mmHg of CO2 pressure.
After these trocars have been positioned and before the gastric dissection, a transcutaneous small bowel feeding tube (Ross Flexiflow Lap J, 10-Fr; Ross Products Division, Abbott Laboratories, Columbus, OH, USA) is placed 20 cm from the ligament of Treitz with “T-fasteners.” A liver retractor exposing the esophageal hiatus is placed through the right 5-mm accessory port. The robot then is brought into position from the head of the operating table, and the two robotic arms are placed through the 8-mm trocars located 8 cm subcostally in the right and left midclavicular lines. The 0° videoscope is placed through the supraumbilical 12-mm trocar.
Using the SonoSurg, the lesser omentum is transected from the base of the liver up to the esophageal hiatus. The short gastric arteries are taken, with preservation of the right gastroepiploic arcade along its entirety, to the right gastroepiploic vein at the transverse mesentery. The pyloric attachments are transected to free the pylorus, allowing mobilization sufficient to reach toward the esophageal hiatus. No Kocher maneuver is performed. Additional nodes are resected from the splenic hilum along the splenic artery to the origin of the left gastric artery and along the common hepatic artery up to the dissection plane completed in the thoracic phase of the procedure.
Next, the gastric conduit is created. Approximately 4 to 5 cm cephalad from the origin of the right gastric artery along the lesser gastric curve, the gastric wall is cleared of perigastric tissue. A 4-cm-wide (from the greater curvature) gastric tube is created with the Ethicon 45 × 4.1-mm linear endostapler (Ethicon Endo-Surgery, Inc., Cincinnati, OH, a Johnson and Johnson Company, New Brunswick, NJ, USA), requiring approximately 8 to 10 firings. No pyloroplasty is performed. The most cephalad aspect of the gastric tube then is sutured to the most distal aspect of the specimen with two widely spaced figure-of-eight sutures to avoid later twisting of the conduit when it is pulled up in the posterior mediastinum. The suction of the ventilator and chest drains is briefly discontinued, and the Penrose drain is used as a handle to pull the specimen carefully up through the neck incision, with the conduit watched closely as it is pulled to the neck.
Once the conduit has been pulled to reach the neck, at the esophageal hiatus level, the anterior gastric conduit serosa is sutured to each esophageal hiatus crus with two figure-of-eight 3-0 Ethibond sutures to reduce the risk of later periconduit herniation. The abdominal phase is now complete, and the robot is moved away from the patient to allow access to the left neck incision site. The abdominal trocar sites are closed.
At the left neck incision, the specimen is transected, and a completely stapled esophagogastrostomy is performed, a triangular side-to-side functional end-to-end stapled anastomosis with a 45 × 4.1-mm linear endostapler and a 60 × 4.1-mm transverse stapler. Before completion of the 4 to 5 × 6-cm triangular anastomosis, a nasogastric tube is placed through the anastomosis [21] (Fig. 6). Before neck fascia and skin closure, a soft flat multiholed drain is placed in the neck beneath the platysma, avoiding the perimeter of the anastomosis, and the wound is closed with interrupted absorbable sutures.
The nasogastric tube is left in place for a minimum of 6 days, after which an esophagram is performed. For the patients without a suspicious defect or leak, the diet is advanced to five small feedings per day. If there is any concern, the tube is left in place, and the study repeated in 3 to 5 days. The next day, after reasonable certainty that no anastomotic leak exists, the neck and chest drains are removed. The patients are encouraged to use acetaminophen rather than narcotics by postoperative day 2.
Results
The results are presented in Table 2. There were no intraoperative or postoperative deaths over a 30-day period. One patient, an 82-year-old smoker with chronic obstructive pulmonary disease (COPD) in group 3, died of pneumonia. Intubated 5 days after surgery, she had remained on the ventilator until her death 72 days later. For one patient with a body mass index (BMI) of 42 and a large chest, the robotic procedure was aborted during the chest phase. The robotic arms were not sufficiently long for completion of the procedure. The esophagectomy was completed by a modified McKeown technique [22, 23]. Despite a negative preoperative CT and PET, one T3N1 82-year-old noninduction patient in group 2 was found during the robotic neck exploration to have a metastatic cervical lymph node.
An average of 18 ± 7 lymph nodes (range, 10–32 lymph nodes) were counted in each specimen, and the averages were 14 in group 1, 18 in group 2, and 25 in group 3. There were no statistical differences between the groups. Although not formally studied, there appeared to be less pain. Five of the eight group 3 patients were taking acetaminophen by postoperative day 3. The remaining three patients still were receiving narcotics.
The combined complications for groups 1, 2, and 3 are shown in Table 3. Major complications (defined as potentially life threatening or involving a significant change in the course of treatment) were experienced by 4 patients (29%), and 13 of the 14 patients (93%) experienced minor complications. One patient in group 1 had a thoracic duct leak. In groups 2 and 3, a thoracic duct ligation resulted in no further leaks. However, one patient had a high chest tube output, with low triglyceride effusion lasting longer than 7 days. Three patients had anastomotic problems, one with a leak and stricture and two with strictures requiring dilation. Three patients had temporary aspiration. There were two vocal cord paralyses. One case required a temporary protective tracheostomy for bilateral vocal cord paresis. The other case, a right recurrent laryngeal nerve paralysis in a patient previously described as having a malignancy, involved a node adjacent to the nerve. Although the nerve was preserved, Gelfoam and later Teflon vocal cord injections were required for medialization of the right vocal cord. The patient with bilateral vocal cord paresis required 3 days of ventilation and tracheostomy placement early in the series, and subsequently required 3 months to recover with residual left vocal cord paresis.
Five patients had atrial fibrillation, and one patient had preoperative heart failure requiring postoperative cardioversion. In one patient who had received preoperative chemoradiotherapy, the right main stem bronchus was injured with the metal post of the SonoSurg dissector. The injury was repaired robotically and healed without incident.
Five of the eight patients in group 3 (four of whom had received induction radiation therapy) experienced a chronic cough, which was associated initially with significant sputum production. The one patient who died had sputum so voluminous that she was unable to clear her airway, had to be reintubated, and later contracted pneumonia. For the other patients, the cough lingered without incident for several months. There were no cases of gastric outlet obstruction.
All the patients underwent a complete resection, with gross and microscopic examination showing no tumor at the surgical margins. In three of the nine patients who received induction therapy, no tumor was found in the specimen.
At 17 months, the survival for the series was 87% (12/14 alive). The median follow-up period was 9 months (range, 3–17 months). Two patients in this series died: the patient previously described as contracting postoperative pneumonia and another patient who experienced a fatal head injury 6 months after surgery. Three patients experienced recurrence. The patient found to have an involved cervical node at the time of surgery experienced recurrence in his liver and is still alive 16 months since surgery. He had refused pre- and postoperative chemotherapy. The patient who died of the head injury had recurrent esophageal cancer in the cerebellum, which was treated surgically. The remaining patient experienced recurrent cancer in the right perilaryngeal area. Preoperatively, his cancer had been diagnosed as stage T3N0, and he had received induction therapy without significant response to the preoperative treatment.
Discussion
Esophagectomy is a technically demanding procedure with relatively high morbidity and mortality rates. As a sole means of cancer treatment, it does not appear to be curative for the majority of patients. Minimally invasive esophageal surgery potentially offers patients less encumbrance than the more conventional open procedures. However, there is controversy over whether there is sufficiently wide periesophageal tissue resection via the minimally invasive techniques to provide an adequate cancer operation.
With the advent of robotics, the increased magnification and three-dimensional visual clarity facilitate a precise esophageal resection en bloc with the periesophageal tissue. In contrast to the open procedures, robotics can improve visibility in the thoracic cavity, improving the exposure to the hiatus and the thoracic apex through the relatively unyielding chest wall incision. Robotic dexterity and precision appear to be superior to those achieved by the minimally invasive technique.
During the first 2 to 5 days after surgery, given the extensive nodal resection, we initially noticed voluminous chest drain output, sometimes in excess of 0.4 to 0.8 l per day. With ligation of the thoracic duct, we have noticed a significant reduction in the drain output and elimination of the thoracic duct leaks. However, the drain output still seems excessive and prolonged. Neither careful intraoperative preventive cauterization nor ultrasonic ligation has been adequate to prevent high postoperative chest drainage. Additional multiple endoclip ligations of the visible lymphatic tributaries seem to reduce the drainage further. Fibrin sealant or topical fibrin glue has not been used for fear of the potential for postoperative bowel adhesions and obstruction should the material leak into the peritoneal cavity.
We did not perform a pyloroplasty or a pyloromyotomy. There is no evidence that either is necessary with a gastric tube [24]. Furthermore, the ideal width of the gastric tube has not been determined. The width we chose (4 cm) was a result of our prior minimally invasive experience, review of the literature, and discussions with other minimally invasive surgeons. The esophagogastric anastomotic leak rate, conduit clearance, and dysphagia were not worsened.
When creating the stapled gastric tube, we allow 20 to 30 s to elapse after the stapler is clamped down on the stomach before firing each staple cartridge along the line of resection. This time delay enhances uniform tissue compression and ensures a more precise staple line in the relatively thick-walled stomach (by recommendation of the Ethicon Surgical Corporation). Each stapler cartridge application to the tissue should precisely meet the prior stapler transection site, leaving no unstapled tissue along the gastric conduit staple line. With this accomplished, there should be no need to oversew the staple line. We believe that oversewing does not enhance healing, and may potentially reduce the ability of the gastric conduit to reach the anastomotic site in the neck, or may disrupt the submucosal blood supply. Unlike a larger tube, a 4-cm tube brings the cut edges of the stomach tube closer to the blood supply and may improve healing. To improve the blood supply to the cut edges, 4.1-mm staples rather than of 3.5-mm staples are used. We have not experienced any conduit leak to date.
We do not resect the azygous vein unless it is involved with the cancer. We do, however, remove all the surrounding tissue with the esophageal specimen. We believe that preservation of the azygous vein reduces the potential of gastric conduit twisting during the “pull up” of the gastric tube and helps to maintain its orientation in the mediastinum. To fix the conduit in the new location, the nasogastric tube is left in place until the esophagram is performed 5 to 6 days later.
Some surgeons advocate resecting the azygous vein with the specimen. First, there may be an oncologic purpose, reducing the likelihood of local recurrence. Second, with healing and the physiologic adjustment of the gastric tube to its new location, the azygous vein may become a restrictive band, reducing blood flow to the tip of the conduit, causing venous congestion, or potentially narrowing the conduit. We respect those concerns, but are not convinced because we have had patients whose azygous vein was transected during the esophagectomy, with the conduits migrating into the right chest over time. In particularly one patient, the migration and conduit dilation served to restrict pulmonary function.
In this initial series, the operating room time was excessive. The console time or surgical robotic time of 4.9 h was similar to the transhiatal operative time of 4.2 h [10] and less than the operating time of 7 h for the open three-field approach [25]. If we assume that the robot docking, neck exposure, feeding tube placement, and esophagogastric anastomosis requires 1.5 h, the resultant true surgical time is estimated to be 6.4 h (4.9 + 1.5 h), which leaves nearly 5 h of nonsurgical time. To minimize the operating room time and improve efficiency, we suggest the following:
-
1.
Development of a focused robotic operating team. An operating nurse and support nursing staff familiar with the procedure, robotics, and equipment are essential.
-
2.
Use of an experienced surgical assistant. The knowledge and manual dexterity necessary for precise and careful retraction as well as assistance in mobilization and suctioning helps to maintain the momentum of the procedure.
-
3.
Use of an experienced anesthesiologist who can efficiently intubate and manage single lung ventilation and hemodynamically support of the patient during the procedure.
-
4.
Precise initial port placement and minimization of the frequency of changing robotic instrumentation.
We believe that greater experience of the surgical team and the surgeon will significantly reduce the total operating time.
This operation is not intended to replicate “extended” esophageal resection for cancer, but rather to skeletonize the remaining uninvolved mediastinal structures [26]. With the robotically assisted surgical procedure, the pericardium, the azygous vein, and the opposing pleura are not resected with the specimen, nor is a hiatus diaphragmatic cuff, because we believe that there is no benefit (unless these structures are involved) and that the resection of these structures may increase morbidity. However, with the robotic three-dimensional visibility and dexterity, resection of these structures would not be difficult [27]. We do not perform a complete neck dissection, but rather remove the deep cervical nodes only. The en bloc removal is appealing because it may provide a potentially more oncologic resection, but it may potentially leave metastatic cervical nodes behind. We found one patient whose cancer recurred in the perilaryngeal area [7].
The cohort demographics are not dissimilar from the characteristics of other surgical series [23]. This two-stage approach has some limitations: Patients who may not be appropriate are those who cannot tolerate single lung ventilation, those who possess severe pleural adhesions or pleural symphysis, those who have a large or invasive esophageal cancer (with a transverse diameter exceeding 4 to 5 cm), and those who have severe mediastinal scarring from prior surgery, infection, or remote radiation therapy. We expect that greater surgical experience will define the role for this operation.
This is the first reported series of a two-stage, three-field robotic esophagectomy and en bloc three-field lymphadenectomy. Larger scale trials are needed to define the role of this technique. There have been a number of refinements over the course of this series, and we expect that there will be further improvements as other surgeons perform robotic esophagectomies. We are encouraged by the three-dimensional visibility, instrument dexterity, and our ability to perform a complex operation safely. It remains to be determined whether there is short- or long-term benefit. With further improvements in the robotic equipment and the development of a robotics team, we expect that this minimally invasive wide resection of the esophagus en bloc with the periesophageal tissue in three separate fields may provide a more oncologic operation, reducing the encumbrance to the patient.
References
Orringer MB, Sloan H (1978) Esophagectomy without thoracotomy. J Thorac Cardiovasc Surg 76: 643–654
Skinner DB (1983) En bloc resection for neoplasms of the esophagus and cardia. J Thorac Cardiovasc Surg 85: 59–71
Wang PY, Chien KY (1983) Surgical treatment of carcinoma of the esophagus and cardia among the Chinese. Ann Thorac Surg 35: 143–151
Blot WJ, Fraumeni JF Jr (1987) Trends in esophageal cancer mortality among U.S. blacks and whites. Am J Public Health 77: 296–298
Katlic MR, Wilkins EW Jr, Grillo HC (1990) Three decades of treatment of esophageal squamous carcinoma at the Massachusetts General Hospital. J Thorac Cardio Surg 99: 929–938
Collard JM, Otte JB, Fiasse R, Laterre PF, De Kock M, Longueville J, Glineur D, Romagnoli R, Reynaert M, Kestens PJ (2001) Skeletonizing en bloc esophagectomy for cancer. Ann Surg 234: 25–32
Tsurumaru M, Kajiyama Y, Udagawa H, Akiyama H (2001) Outcomes of extended lymph node dissection for squamous cell carcinoma of the thoracic esophagus. Ann Thorac Cardiovasc Surg 7: 325–329
Ando N, Iizuka T, Ide H, Ishida K, Shinoda M, Nishimaki T, Takiyama W, Watanabe H, Isono K, Aoyama N, Makuuchi H, Tanaka O, Yamana H, Ikeuchi S, Kabuto T, Nagai K, Shimada Y, Kinjo Y, Kukuda H, Japan Clinical Oncology Group (2003) Surgery plus chemotherapy compared with surgery alone for localized squamous cell carcinoma of the thoracic esophagus: a Japan Clinical Oncology Group Study–JCOG9204. J Clin Oncol 21: 4592–4596
Lerut T, Nafteux P, Moons J, Coosemans W, Decker G, De Leyn P, Van Raemdonck D, Ectors N (2004) Three-field lymphadenectomy for carcinoma of the esophagus and gastroesophageal junction in 174 R0 resections: impact on staging, disease-free survival, and outcome: a plea for adaptation of TNM classification in upper-half esophageal carcinoma. Ann Surg 240: 962–972
Hulscher JB, Tijssen JG, Obertop H, van Lanschot JJ (2001) Transthoracic versus transhiatal resection for carcinoma of the esophagus: a meta-analysis. Ann Thorac Surg 72: 306–313
Hulscher JB, Van Sandick JW, Offerhaus GJ, Tilanus HW, Obertop H, Van Lanschot JJ (2001) Prospective analysis of the diagnostic yield of extended en bloc resection for adenocarcinoma of the oesophagus or gastric cardia. Br J Surg 88: 715–719
Altorki N, Kent M, Ferrara C, Port J (2002) Three-field lymph node dissection for squamous cell and adenocarcinoma of the esophagus. Ann Surg 236: 177–183
Ando N, Ozawa S, Kitagawa Y, Shinozawa Y, Kitajima M (2000) Improvement in the results of surgical treatment of advanced squamous esophageal carcinoma during 15 consecutive years. Ann Surg 232: 225–232
Cooper JS, Guo MD, Herskovic A, Macdonald JS, Martenson JA Jr, Al-Sarraf M, Byhardt R, Russell AH, Beitler JJ, Spencer S, Asbell SO, Graham MV, Leichman LL (1999) Chemoradiotherapy of locally advanced esophageal cancer: long-term follow-up of a prospective randomized trial (RTOG 85-01). Radiation Therapy Oncology Group. JAMA 281: 1623–1627
Swanstrom LL, Hansen P (1997) Laparoscopic total esophagectomy. Arch Surg 132: 943–947
Nguyen NT, Schauer P, Luketich JD (2000) Minimally invasive esophagectomy for Barrett’s esophagus with high-grade dysplasia. Surgery 127: 284–290
Nguyen NT, Roberts P, Follette DM, Rivers R, Wolfe BM (2003) Thoracoscopic and laparoscopic esophagectomy for benign and malignant disease: lessons learned from 46 consecutive procedures. J Am Coll Surg 197: 902–913
Luketich JD, Alvelo-Rivera M, Buenaventura PO, Christie NA, McCaughan JS, Litle VR, Schauer PR, Close JM, Fernando HC (2003) Minimally invasive esophagectomy: outcomes in 222 patients. Ann Surg 238: 486–494
Horgan S, Berger RA, Elli EF, Espat NJ (2003) Robotic-assisted minimally invasive transhiatal esophagectomy. Am Surg 69: 624–626
Kernstine KH, DeArmond DT, Karimi M, VanNatta TL, Campos JC, Yoder MR, Everett JE (2004) The robotic, 2-stage, 3-field esophagolymphadenectomy. J Thorac Cardiovasc Surg 127: 1847–1849
Singh D, Maley RH, Santucci T, Macherey RS, Bartley S, Weyant RJ, Landreneau RJ (2001) Experience and technique of stapled mechanical cervical esophagogastric anastomosis. Ann Thorac Surg 71: 419–424
McKeown KC (1985) The surgical treatment of carcinoma of the esophagus: a review of the results of 478 cases. J R Coll Surg Edinb 30: 1–14
Swanson SJ, Batirel HF, Bueno R, Jaklitsch MT, Lukanich JM, Allred E, Mentzer SJ, Sugarbaker DJ (2001) Transthoracic esophagectomy with radical mediastinal and abdominal lymph node dissection and cervical esophagogastrostomy for esophageal carcinoma. Ann Thorac Surg 72: 1918–1924
Lerut TE, van Lanschot JJ (2004) Chronic symptoms after subtotal or partial oesophagectomy: diagnosis and treatment. Best Pract Res Clin Gastroenterol 18: 901–915
Altorki NK (2000) Three-field lymphadenectomy for esophageal cancer. Chest Surg Clin North Am 10: 553–560
Collard JM, Otte JB, Reynaert M, Kestens PJ (1991) Long gastroplasties with the GIA stapler in esophageal surgery. In: Ravich MM, Steichen FM, Welter R (eds) Current practice of surgical stapling. Lea & Febiger, Philadelphia, PA pp 183–187
Kernstine KH (2004) Robotics in thoracic surgery. Am J Surg 188(4A Suppl): 89S–97S
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kernstine, K.H., DeArmond, D.T., Shamoun, D.M. et al. The first series of completely robotic esophagectomies with three-field lymphadenectomy: initial experience. Surg Endosc 21, 2285–2292 (2007). https://doi.org/10.1007/s00464-007-9405-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-007-9405-7