Abstract
In adulthood, an induced nephron-specific deficiency of αENaC (Scnn1a) resulted in pseudohypoaldosteronism type 1 (PHA-1) with sodium loss, hyperkalemia, and metabolic acidosis that is rescued through high-sodium/low-potassium (HNa+/LK+) diet. In the present study, we addressed whether renal βENaC expression is required for sodium and potassium balance or can be compensated by remaining (α and γ) ENaC subunits using adult nephron-specific knockout (Scnn1bPax8/LC1) mice. Upon induction, these mice present a severe PHA-1 phenotype with weight loss, hyperkalemia, and dehydration, but unlike the Scnn1aPax8/LC1 mice without persistent salt wasting. This is followed by a marked downregulation of STE20/SPS1-related proline-alanine-rich protein kinase (SPAK) and Na+/Cl− co-transporter (NCC) protein expression and activity. Most of the experimental Scnn1bPax8/LC1 mice survived with a HNa+/LK+ diet that partly normalized NCC phosphorylation, but not total NCC expression. Since salt loss was minor, we applied a standard-sodium/LK+ diet that efficiently rescued these mice resulting in normokalemia and normalization of NCC phosphorylation, but not total NCC expression. A further switch to LNa+/standard-K+ diet induced again a severe PHA-1-like phenotype, but with only transient salt wasting indicating that low-K+ intake is critical to decrease hyperkalemia in a NCC-dependent manner. In conclusion, while the βENaC subunit plays only a minor role in sodium balance, severe hyperkalemia results in downregulation of NCC expression and activity. Our data demonstrate the importance to primarily correct the hyperkalemia with a low-potassium diet that normalizes NCC activity.








Similar content being viewed by others
References
Amin N, Alvi NS, Barth JH, Field HP, Finlay E, Tyerman K, Frazer S, Savill G, Wright NP, Makaya T, Mushtaq T (2013) Pseudohypoaldosteronism type 1: clinical features and management in infancy. Endocrinol Diabetes Metab Case Rep 2013:130010. doi:10.1530/EDM-13-0010
Arroyo JP, Lagnaz D, Ronzaud C, Vazquez N, Ko BS, Moddes L, Ruffieux-Daidie D, Hausel P, Koesters R, Yang B, Stokes JB, Hoover RS, Gamba G, Staub O (2011) Nedd4-2 modulates renal Na+-Cl- cotransporter via the aldosterone-SGK1-Nedd4-2 pathway. J Am Soc Nephrol 22:1707–1719. doi:10.1681/ASN.2011020132
Arroyo JP, Ronzaud C, Lagnaz D, Staub O, Gamba G (2011) Aldosterone paradox: differential regulation of ion transport in distal nephron. Physiology (Bethesda) 26:115–123. doi:10.1152/physiol.00049.2010
Barker PM, Nguyen MS, Gatzy JT, Grubb B, Norman H, Hummler E, Rossier B, Boucher RC, Koller B (1998) Role of gammaENaC subunit in lung liquid clearance and electrolyte balance in newborn mice. Insights into perinatal adaptation and pseudohypoaldosteronism. J Clin Invest 102:1634–1640. doi:10.1172/JCI3971
Bonny O, Chraibi A, Loffing J, Jaeger NF, Grunder S, Horisberger JD, Rossier BC (1999) Functional expression of a pseudohypoaldosteronism type I mutated epithelial Na+ channel lacking the pore-forming region of its alpha subunit. J Clin Invest 104:967–974. doi:10.1172/JCI6821
Canessa CM, Schild L, Buell G, Thorens B, Gautschi I, Horisberger JD, Rossier BC (1994) Amiloride-sensitive epithelial Na+ channel is made of three homologous subunits. Nature 367:463–467. doi:10.1038/367463a0
Cheek DB, Perry JW (1958) A salt wasting syndrome in infancy. Arch Dis Child 33:252–256
Chiga M, Rai T, Yang SS, Ohta A, Takizawa T, Sasaki S, Uchida S (2008) Dietary salt regulates the phosphorylation of OSR1/SPAK kinases and the sodium chloride cotransporter through aldosterone. Kidney Int 74:1403–1409. doi:10.1038/ki.2008.451
Christensen BM, Perrier R, Wang Q, Zuber AM, Maillard M, Mordasini D, Malsure S, Ronzaud C, Stehle JC, Rossier BC, Hummler E (2010) Sodium and potassium balance depends on alphaENaC expression in connecting tubule. J Am Soc Nephrol 21:1942–1951. doi:10.1681/ASN.2009101077
Cornelius RJ, Wen D, Hatcher LI, Sansom SC (2012) Bicarbonate promotes BK-alpha/beta4-mediated K excretion in the renal distal nephron. Am J Physiol Renal Physiol 303:F1563–F1571. doi:10.1152/ajprenal.00490.2012
Delpire E, Gagnon KB (2008) SPAK and OSR1: STE20 kinases involved in the regulation of ion homoeostasis and volume control in mammalian cells. Biochem J 409:321–331. doi:10.1042/BJ20071324
Espinel CH (1976) The FENa test. Use in the differential diagnosis of acute renal failure. JAMA 236:579–581
Evers S, Engelien A, Karsch V, Hund M (1998) Secondary hyperkalaemic paralysis. J Neurol Neurosurg Psychiatry 64:249–252
Frindt G, McNair T, Dahlmann A, Jacobs-Palmer E, Palmer LG (2002) Epithelial Na channels and short-term renal response to salt deprivation. Am J Physiol Renal Physiol 283:F717–F726. doi:10.1152/ajprenal.00379.2001
Frindt G, Palmer LG (2010) Effects of dietary K on cell-surface expression of renal ion channels and transporters. Am J Physiol Renal Physiol 299:F890–F897. doi:10.1152/ajprenal.00323.2010
Garg SK, Saxena S, Juneja D, Singh O, Kumar M, Mukherji JD (2014) Hyperkalemia: a rare cause of acute flaccid quadriparesis. Indian J Crit Care Med 18:46–48. doi:10.4103/0972-5229.125439
Geller DS, Rodriguez-Soriano J, Vallo Boado A, Schifter S, Bayer M, Chang SS, Lifton RP (1998) Mutations in the mineralocorticoid receptor gene cause autosomal dominant pseudohypoaldosteronism type I. Nat Genet 19:279–281. doi:10.1038/966
Hanukoglu A, Edelheit O, Shriki Y, Gizewska M, Dascal N, Hanukoglu I (2008) Renin-aldosterone response, urinary Na/K ratio and growth in pseudohypoaldosteronism patients with mutations in epithelial sodium channel (ENaC) subunit genes. J Steroid Biochem Mol Biol 111:268–274. doi:10.1016/j.jsbmb.2008.06.013
Hummler E, Barker P, Gatzy J, Beermann F, Verdumo C, Schmidt A, Boucher R, Rossier BC (1996) Early death due to defective neonatal lung liquid clearance in alpha-ENaC-deficient mice. Nat Genet 12:325–328. doi:10.1038/ng0396-325
Kellendonk C, Tronche F, Casanova E, Anlag K, Opherk C, Schutz G (1999) Inducible site-specific recombination in the brain. J Mol Biol 285:175–182. doi:10.1006/jmbi.1998.2307
Ko B, Mistry AC, Hanson L, Mallick R, Wynne BM, Thai TL, Bailey JL, Klein JD, Hoover RS (2013) Aldosterone acutely stimulates NCC activity via a SPAK-mediated pathway. Am J Physiol Renal Physiol 305:F645–F652. doi:10.1152/ajprenal.00053.2013
Kraut JA, Xing SX (2011) Approach to the evaluation of a patient with an increased serum osmolal gap and high-anion-gap metabolic acidosis. Am J Kidney Dis 58:480–484. doi:10.1053/j.ajkd.2011.05.018
McCormick JA, Mutig K, Nelson JH, Saritas T, Hoorn EJ, Yang CL, Rogers S, Curry J, Delpire E, Bachmann S, Ellison DH (2011) A SPAK isoform switch modulates renal salt transport and blood pressure. Cell Metab 14:352–364. doi:10.1016/j.cmet.2011.07.009
McDonald FJ, Yang B, Hrstka RF, Drummond HA, Tarr DE, McCray PB Jr, Stokes JB, Welsh MJ, Williamson RA (1999) Disruption of the beta subunit of the epithelial Na+ channel in mice: hyperkalemia and neonatal death associated with a pseudohypoaldosteronism phenotype. Proc Natl Acad Sci U S A 96:1727–1731
Merillat AM, Charles RP, Porret A, Maillard M, Rossier B, Beermann F, Hummler E (2009) Conditional gene targeting of the ENaC subunit genes Scnn1b and Scnn1g. Am J Physiol Renal Physiol 296:F249–F256. doi:10.1152/ajprenal.00612.2007
Nesterov V, Dahlmann A, Krueger B, Bertog M, Loffing J, Korbmacher C (2012) Aldosterone-dependent and -independent regulation of the epithelial sodium channel (ENaC) in mouse distal nephron. Am J Physiol Renal Physiol 303:F1289–F1299. doi:10.1152/ajprenal.00247.2012
Nobel YR, Lodish MB, Raygada M, Rivero JD, Faucz FR, Abraham SB, Lyssikatos C, Belyavskaya E, Stratakis CA, Zilbermint M (2016) Pseudohypoaldosteronism type 1 due to novel variants of SCNN1B gene. Endocrinol Diabetes Metab Case Rep 2016:150104. doi:10.1530/EDM-15-0104
Penton D, Czogalla J, Wengi A, Himmerkus N, Loffing-Cueni D, Carrel M, Rajaram RD, Staub O, Bleich M, Schweda F, Loffing J (2016) Extracellular K+ rapidly controls NaCl cotransporter phosphorylation in the native distal convoluted tubule by Cl--dependent and independent mechanisms. J Physiol 594:6319–6331. doi:10.1113/JP272504
Perrier R, Boscardin E, Malsure S, Sergi C, Maillard MP, Loffing J, Loffing DC, Sorensen MV, Koesters R, Rossier BC, Frateschi S, Hummler E (2015) Severe salt-losing syndrome and hyperkalemia induced by adult nephron-specific knockout of the epithelial sodium channel alpha-subunit. J Am Soc Nephrol. doi:10.1681/ASN.2015020154
Poulsen SB, Praetorius J, Damkier HH, Miller L, Nelson RD, Hummler E, Christensen BM (2015) Reducing alphaENaC expression in kidney connecting tubule induces pseudohypoaldosteronism type 1 symptoms during K+ loading. Am J Physiol Renal Physiol ajprenal. doi:10.1152/ajprenal.00258.2015
Pradervand S, Barker PM, Wang Q, Ernst SA, Beermann F, Grubb BR, Burnier M, Schmidt A, Bindels RJ, Gatzy JT, Rossier BC, Hummler E (1999) Salt restriction induces pseudohypoaldosteronism type 1 in mice expressing low levels of the beta-subunit of the amiloride-sensitive epithelial sodium channel. Proc Natl Acad Sci U S A 96:1732–1737
Rajpoot SK, Maggi C, Bhangoo A (2014) Pseudohypoaldosteronism in a neonate presenting as life-threatening arrhythmia. Endocrinol Diabetes Metab Case Rep 2014:130077. doi:10.1530/EDM-13-0077
Richardson C, Rafiqi FH, Karlsson HK, Moleleki N, Vandewalle A, Campbell DG, Morrice NA, Alessi DR (2008) Activation of the thiazide-sensitive Na+-Cl- cotransporter by the WNK-regulated kinases SPAK and OSR1. J Cell Sci 121:675–684. doi:10.1242/jcs.025312
Rossier BC, Staub O, Hummler E (2013) Genetic dissection of sodium and potassium transport along the aldosterone-sensitive distal nephron: importance in the control of blood pressure and hypertension. FEBS Lett 587:1929–1941. doi:10.1016/j.febslet.2013.05.013
Rubera I, Loffing J, Palmer LG, Frindt G, Fowler-Jaeger N, Sauter D, Carroll T, McMahon A, Hummler E, Rossier BC (2003) Collecting duct-specific gene inactivation of alphaENaC in the mouse kidney does not impair sodium and potassium balance. J Clin Invest 112:554–565. doi:10.1172/JCI16956
Sorensen MV, Grossmann S, Roesinger M, Gresko N, Todkar AP, Barmettler G, Ziegler U, Odermatt A, Loffing-Cueni D, Loffing J (2013) Rapid dephosphorylation of the renal sodium chloride cotransporter in response to oral potassium intake in mice. Kidney Int 83:811–824. doi:10.1038/ki.2013.14
Staub O, Gautschi I, Ishikawa T, Breitschopf K, Ciechanover A, Schild L, Rotin D (1997) Regulation of stability and function of the epithelial Na+ channel (ENaC) by ubiquitination. EMBO J 16:6325–6336. doi:10.1093/emboj/16.21.6325
Sterns RH, Grieff M, Bernstein PL (2016) Treatment of hyperkalemia: something old, something new. Kidney Int 89:546–554. doi:10.1016/j.kint.2015.11.018
Terker AS, Zhang C, Erspamer KJ, Gamba G, Yang CL, Ellison DH (2015) Unique chloride-sensing properties of WNK4 permit the distal nephron to modulate potassium homeostasis. Kidney Int. doi:10.1038/ki.2015.289
Traykova-Brauch M, Schonig K, Greiner O, Miloud T, Jauch A, Bode M, Felsher DW, Glick AB, Kwiatkowski DJ, Bujard H, Horst J, von Knebel DM, Niggli FK, Kriz W, Grone HJ, Koesters R (2008) An efficient and versatile system for acute and chronic modulation of renal tubular function in transgenic mice. Nat Med 14:979–984. doi:10.1038/nm.1865
Vallon V, Schroth J, Lang F, Kuhl D, Uchida S (2009) Expression and phosphorylation of the Na+-Cl- cotransporter NCC in vivo is regulated by dietary salt, potassium, and SGK1. Am J Physiol Renal Physiol 297:F704–F712. doi:10.1152/ajprenal.00030.2009
Vitari AC, Deak M, Morrice NA, Alessi DR (2005) The WNK1 and WNK4 protein kinases that are mutated in Gordon’s hypertension syndrome phosphorylate and activate SPAK and OSR1 protein kinases. Biochem J 391:17–24. doi:10.1042/BJ20051180
Vitzthum H, Seniuk A, Schulte LH, Muller ML, Hetz H, Ehmke H (2014) Functional coupling of renal K+ and Na+ handling causes high blood pressure in Na+ replete mice. J Physiol 592:1139–1157. doi:10.1113/jphysiol.2013.266924
Wade JB, Liu J, Coleman R, Grimm PR, Delpire E, Welling PA (2015) SPAK-mediated NCC regulation in response to low-K+ diet. Am J Physiol Renal Physiol 308:F923–F931. doi:10.1152/ajprenal.00388.2014
Wagner CA, Loffing-Cueni D, Yan Q, Schulz N, Fakitsas P, Carrel M, Wang T, Verrey F, Geibel JP, Giebisch G, Hebert SC, Loffing J (2008) Mouse model of type II Bartter’s syndrome. II. Altered expression of renal sodium- and water-transporting proteins. Am J Physiol Renal Physiol 294:F1373–F1380. doi:10.1152/ajprenal.00613.2007
Wen D, Cornelius RJ, Rivero-Hernandez D, Yuan Y, Li H, Weinstein AM, Sansom SC (2014) Relation between BK-alpha/beta4-mediated potassium secretion and ENaC-mediated sodium reabsorption. Kidney Int 86:139–145. doi:10.1038/ki.2014.14
Zennaro MC, Hubert EL, Fernandes-Rosa FL (2012) Aldosterone resistance: structural and functional considerations and new perspectives. Mol Cell Endocrinol 350:206–215. doi:10.1016/j.mce.2011.04.023
Acknowledgements
We thank Olivier Bonny for critically reading the manuscript and Anne-Marie Mérillat for the excellent photographic work. Kidney protein lysate from SPAK KO mice was kindly provided by Olivier Staub. This work was supported by the Swiss National Science Foundation Grants FNRS 31003A_144198/1 and 31003A_163347 (to E.H.), the Leducq Foundation (to E.H.), Swiss National Center of Competence in Research (NCCR kidney.CH) and the networking support by the COST Action ADMIRE BM1301 (to E.H.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the institution. Protocols followed the Swiss federal guidelines and were approved by the veterinarian local authorities (« Service de la consommation et des affaires vétérinaires ») of the Canton de Vaud, Switzerland.
Electronic supplementary material
.
Supplemental Figure 1
Schema of the experimental protocols. Representative setup used to determine physiological parameters in Scnn1bPax8/LC1 mice placed either in standard (thin line) or metabolic cages (bold line) and induced by doxycycline (Dox) under standard diet (A), a short term high Na+ and low K+ diet (B), a long-term high Na+ and low K+ diet (C), and a long-term low K+ diet (D), back to standard diet after one month under HNa+/LK+ diet (E), and back to LNa+ diet after 16 days under LK+ diet (F). Arrows indicate the end of the experiment, and the time point of serum and organ recovery. (PDF 1795 kb)
Supplemental Figure 2
Physiological parameters as measured following induction under standard diet. Measurement of daily 24 hours (A) food (g/24 h/gBW), (B) water intake (ml/24 h/g BW), (C) feces (g/24 h/gBW), (D) urine volume output (ml/24 h/gBW), and measurement of (E) Na+ and (F) K+ intake (mmol/24/gBW) in Scnn1b control (n = 20) and experimental mice (n = 8), protocol A. Values were normalized to the body weight * P < 0.05, ** P < 0.01, ***P < 0.001 (PDF 208 kb).
Supplemental Figure 3
Physiological parameters as measured following induction under acute High Na+ and low K+ diet. (A) Food intake (g/gBW), (B) water intake (ml//gBW), (C) feces output (g/gBW), (D) urine volume (ml/gBW), and measurement of daily urinary Na+ (E) and K+ (F) excretion (mmol/24 h/gBW), and (G) Na+ and K+ (H) intake (mmol/24 h/gBW), in Scnn1b control (n = 6) and experimental mice (n = 8) following doxycycline treatment upon standard diet (24-hour measurement) and high Na+/low K+ (6-hour measurement); protocol B. Values were normalized to the body weight. * P < 0.05, *** P < 0.001 (PDF 175 kb).
Supplemental Figure 4
Long term high Na+ and low K+ diet normalizes all physiological parameters in Scnn1bPax8/LC1 mice. Measurement of (A) body weight changes (Δ body weight, BW) in percentage of initial BW, and (B) plasma Na+ and K+ concentration (mmol/l), (C) 24 hours urinary Na+ and (D) K+ excretion (mmol/24 h/gBW), and (E) Na+ and (F) K+ intake (mmol/24 h/gBW) in control (n = 8) and Scnn1bPax8/LC1 mice (n = 6), (protocol C). ** P < 0.01 (PDF 229 kb).
Supplemental Figure 5
Long term high Na+ and low K+ diet normalizes food and water intake, feces weight and urinary volume excretion in Scnn1bPax8/LC1 mice. 24 hours (A) food (g/24 h/gBW) and (B) water intake (ml/24 h/gBW), (C) feces output (g/24 h/gBW), and (D) urine volume (ml/24 h/gBW) in control (n = 8) and Scnn1bPax8/LC1 mice (n = 6), (protocol C). Results are presented as mean ± SEM and data were analyzed by unpaired t test. P values <0.05 were considered statistically significant. (PDF 232 kb).
Supplemental Figure 6
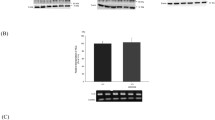
α- and γ-ENaC protein expression is unchanged in Scnn1bPax8/LC1 mice. Representative Western blot analyses of α-, γ-ENaC and actin on kidney from Scnn1b control and experimental mice upon standard diet (protocol A) (A); controls, n = 6 and experimental Scnn1b mice: n = 6; (B) Acute high Na+ and low K+ diet (protocol B); control and experimental mice, each group, n = 6; (C) Long - term high Na+ and low K+ diet (protocol C); control (n = 8) and experimental mice (n = 6). Left panel, quantification of proteins from corresponding Western blots analyses. Protein levels were normalized to actin and expressed in percentage of control. Results are presented as mean ± SEM and data were analyzed by unpaired t test. P values <0.05 were considered statistically significant. (PDF 6735 kb).
Supplemental Figure 7
High Na+ and low K+ diet normalizes pSPAK in Scnn1bPax8/LC1 mice. Representative Western blot analyses of phosphorylated SPAK and actin on kidney cortex extracts from Scnn1b control and experimental mice upon standard diet (protocol A) (A); controls, n = 6 and experimental Scnn1b mice: n = 5; (C) high Na+ and low K+ diet (protocol B); in control and experimental mice, each group, n = 5. (B and D) Quantification of proteins from corresponding Western blot analyses. Protein levels were normalized to actin and expressed in percentage of control. Results are presented as mean ± SEM and data were analyzed by unpaired t test. ** P < 0.01 (PDF 1032 kb).
Supplemental Figure 8
Long-term low K+ diet and standard Na+ restores food and water intake, feces weight and urinary volume excretion in Scnn1bPax8/LC1 mice. Daily (A) food (g/24 h/gBW) and (B) water intake (ml/24 h/gBW), (C) feces output (g/24 h/gBW) and (D), urine volume (ml/24 h/gBW), in control (n = 6) and experimental mice (n = 6; protocol D). Results are presented as mean ± SEM and data were analyzed by unpaired t test. P values <0.05 were considered statistically significant. (PDF 196 kb).
Supplemental Figure 9
Long-term low K+ diet normalizes pSPAK in Scnn1bPax8/LC1 mice. Representative Western blot analyses of phosphorylated SPAK and actin on kidney cortex extracts from Scnn1b control and experimental mice upon standard Na+ and low K+ diet (A); protocol D), each group, n = 5. (B) Quantification of proteins from corresponding Western blot analyses. Protein levels were normalized to actin and expressed in percentage of control. Results are presented as mean ± SEM and data were analyzed by unpaired t test. P values <0.05 were considered statistically significant. (PDF 569 kb).
Supplemental Figure 10
Physiological parameters as measured under both standard Na+/low K+ and standard K+/low Na+ diet in Scnn1bPax8/LC1 mice. (A) Food intake (g/24h/gBW), (B) water intake (ml/24h/gBW), (C) feces output (g/24h/gBW), (D) urine volume (ml/24h/gBW), and measurement of (E) Na+ and K+ (F) intake (mmol/24h/gBW), in control (n = 6) and experimental mice (n = 4) under low K+ diet and following LNa+ diet (24-hour measurement); protocol F. Values were normalized to the body weight. * P<0.05, ** P <0.01 (PDF 121 kb).
Rights and permissions
About this article
Cite this article
Boscardin, E., Perrier, R., Sergi, C. et al. Severe hyperkalemia is rescued by low-potassium diet in renal βENaC-deficient mice. Pflugers Arch - Eur J Physiol 469, 1387–1399 (2017). https://doi.org/10.1007/s00424-017-1990-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-017-1990-2