Abstract
Background
Benign esophageal pseudoachalasia is a rare condition.
Discussion
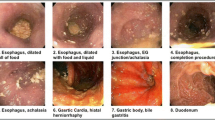
We report the case of a 70-year-old man who complained of severe dysphagia after laparoscopic Nissen fundoplication and crural mesh repair performed for long-standing gastroesophageal reflux disease. Severe dysphagia and nocturnal aspiration developed soon after the operation. A marked dilatation of the esophageal body and a manometric pattern resembling achalasia was documented.
Results
Endoscopic balloon dilatation was ineffective. Five months after the initial operation, the patient underwent revisional laparoscopic surgery that consisted of Nissen’s wrap takedown, enlargement of the hiatus with partial resection of the mesh, Heller myotomy, and Dor fundoplication. After a 2-year follow-up, the patient is doing well and is free of symptoms.


Similar content being viewed by others
References
Horwath W (1919) Dilatation of the oesophagus without anatomical stenosis. Proc R Soc Med 12(Laryngology section):64
Ogilvie H (1947) Early diagnosis of cancer of the oesophagus and stomach. Br Med J 2:405–407
Davis J, Kantrowitz P, Chandler H, Schatzki S (1975) Reversible achalasia due to reticulum-cell sarcoma. N Engl J Med 293:130–132
Kahrilas P, Kishk S, Helm J, Dodds W, Harig J, Hogan W (1987) Comparison of pseudoachalasia and achalasia. Am J Med 82:439–446
Bonavina L, Fociani P, Asnaghi D, Ferrero S (1998) Synovial sarcoma of the esophagus simulating achalasia. Dis Esophagus 11:268–271
Moonka R, Patti M, Feo C, Arcerito M, De Pinto M, Horgan S, Pellegrini C (1999) Clinical presentation and evaluation of malignant pseudoachalasia. J Gastrointest Surg 3:456–461
Liu W, Fackler W, Rice T, Richter J, Achkar E, Goldblum J (2002) The pathogenesis of pseudoachalasia. A clinicopathologic study of 13 cases of a rare entity. Am J Surg Pathol 26:784–788
Stlylopoulos N, Bunker C, Rattner D (2002) Development of achalasia secondary to laparoscopic Nissen fundoplication. J Gastrointest Surg 6:368–378
Smith C, McClusky D, Rajad M, Lederman A, Hunter J (2005) When fundoplication fails. Redo? Ann Surg 241:861–871
Byrne J, Smithers B, Nathanson L, Martin I, Ong H, Gotley D (2005) Symptomatic and functional outcome after laparoscopic reoperation for failed antireflux surgery. Br J Surg 92:996–1001
Little A, Correnti F, Calleja I, Montag A, Chow Y, Ferguson M, Skinner D (1986) Effect of incomplete obstruction on feline esophageal function with a clinical correlation. Surgery 100:430–436
Hunter J, Smith D, Branum G, Waring P, Trus T, Cornwell M, Galloway K (1999) Laparoscopic fundoplication failures. Patterns of failure and response to fundoplication revision. Ann Surg 230:595–606
Targarona E, Bendahan G, Balague C, Garriga J, Trias M (2004) Mesh in the hiatus. A controversial issue. Arch Surg 139:1286–1296
Mattox H, Albertson D, Castell D, Richter J (1990) Dysphagia following fundoplication: “slipped” fundoplication versus achalasia complicated by fundoplication. Am J Gastroenterol 85:1468–1472
Trus T, Bax T, Richardson W, Branum G, Mauren S, Swanstrom L, Hunter J (1997) Complication of laparoscopic paraesophageal hernia repair. J Gastrointest Surg 1:221–228
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bonavina, L., Bona, D., Saino, G. et al. Pseudoachalasia occurring after laparoscopic Nissen fundoplication and crural mesh repair. Langenbecks Arch Surg 392, 653–656 (2007). https://doi.org/10.1007/s00423-007-0191-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-007-0191-4