Abstract
Purpose
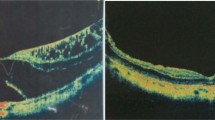
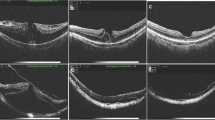
The purpose of this study was to investigate and present the results of a new vitrectomy technique to preserve the foveolar internal limiting membrane (ILM) during ILM peeling in early stage 2 macular holes (MH).
Methods
The medical records of 28 consecutive patients (28 eyes) with early stage 2 MH were retrospectively reviewed and randomly divided into two groups by the extent of ILM peeing. Group 1: foveolar ILM nonpeeling group (14 eyes), and group 2: total peeling of foveal ILM group (14 eyes). A donut-shaped ILM was peeled off, leaving a 400-μm-diameter ILM over foveola in group 1.
Results
Smooth and symmetric umbo foveolar contour was restored without inner retinal dimpling in all eyes in group 1, but not in group 2. The final vision was better in group 1 (P = 0.011). All eyes in group 1 (100 %) and seven of 14 eyes in group 2 (50 %)regained the inner segment/outer segment (IS/OS) line. Restoration of the umbo light reflex was found in 12 of 14 eyes in group 1 (86 %) but none in group 2 (0 %).
Conclusions
Nonpeeling of the foveolar ILM in early stage 2 idiopathic MH surgery prevented inner retinal damages, restored umbo light reflex, achieved better foveolar microstructures, and led to better final visual acuity.






Similar content being viewed by others
References
Mester V, Kuhn F (2000) Internal limiting membrane removal in the management of full-thickness macular holes. Am J Ophthalmol 129:769–777
Funata M, Wendel RT, de la Cruz Z et al (1992) Clinicopathologic study of bilateral macular holes treated with pars plana vitrectomy and gas tamponade. Retina 12:289–298
Nakamura T, Murata T, Hisatomi T et al (2003) Ultrastructure of the vitreoretinal interface following the removal of the internal limiting membrane using indocyanine green. Curr Eye Res 27:395–399
Terasaki H, Miyake Y, Nomura R et al (2001) Focal macular ERGs in eyes after removal of macular ILM during macular hole surgery. Invest Ophthalmol Vis Sci 42:229–234
Alkabes M, Salinas C, Vitale L et al (2011) En face optical coherence tomography of inner retinal defect after internal limiting membrane peeling for idiopathic macular hole. Invest Ophthalmol Vis Sci 52(11):8349–8355
Haritoglou C, Gandorfer A, Kampik A (2006) NFL appearance after peeling. Ophthalmology 113:1690
Christensen UC, Kroyer K, Sander B et al (2009) Value of internal limiting membrane peeling in surgery idiopathic macular hole stage 2 and 3: a randomized clinical trial. Br J Ophthalmol 93:1005–1012
Spaide RF (2012) “Dissociated optic nerve fiber layer appearance” after internal limiting membrane removal is inner retinal dimpling. Retina DOI:101097/IAE.0b013e3182671191 pg. 1719-1726
Kim JH, Kang SW, Park DY et al (2012) Asymmetric elongation of foveal tissue after macular hole surgery and its impact on metamorphopsia. Ophthalmology 119:2133–2140
Baba Y, Yamamoto S, Kimoto R et al (2012) Reduction of thickness of ganglion cell complex after internal limiting membrane peeling during vitrectomy for idiopathic macular hole. Eye advance online publication 17 August 2012;doi:10.1038/eye.2012.170
Chang S (2012) Controversies regarding internal limiting membrane peeling in idiopathic epiretinal membrane and macular hole. Retina DOI:10.1097/IAE.0b013e31825bc026pg. S200-S204
Pilli S, Zawadzki RJ, Werner JS et al (2012) Visual outcome correlates with inner macular volume in eyes with surgically closed macular hole. Retina 32(10):2085–2095
Gass JDM (1988) Idiopathic senile macular hole: its early stages and pathogenesis. Arch Ophthalmol 106:629–639
Sjaarda RN, Thompson J (2006) Macular hole. In: Retina 4th ed. Ryan SJ, ed.: Mosby-Elsevier pg. 2527
Tadayoni R, Gaudric A, Haouchine B et al (2006) Relationship between macular hole size and the potential benefit of internal limiting membrane peeling. Br J Ophthalmol 90:1239–1241
Ho TC, Chen MS, Hung JS et al (2012) Foveola nonpeeling technique in internal limiting membrane peeling of myopic foveoschisis surgery. Retina 32(3):631–634
Shimada N, Sugamoto Y, Ogawa M et al (2012) Fovea-sparing internal limiting membrane peeling for myopic traction maculopathy. Am J Ophthalmol 154:693–701
Wakabayashi T, Oshima Y, Fujimoto H et al (2009) Foveal microstructure and visual acuity after retinal detachment repair. Ophthalmology 116(3):519–528
Wakabayashi T, Fujiwara M, Sakaguchi H et al (2010) Foveal microstructure and visual acuity in surgically closed macular holes: spectral-domain optical coherence tomographic analysis. Ophthalmology 117(9):1815–1824
Lois N, Norrie J, Vale L et al (2011) Internal limiting membrane peeling versus no peeling for idiopathic full-thickness macular hole: a pragmatic randomized controlled trial. Invest Ophthalmol Vis Sci 52(3):1586–1592
Chan P, Hoang QV, Chang S (2012) Frequency and Significance of Vitreoretinal Interface Remodeling after Repair of Idiopathic Macular Holes ARVO abstract poster #: A248
Chang S, Gregory-Roberts E, Park S et al (2013) Double peeling during vitrectomy for macular pucker. The Charles L. Schepens Lecture. JAMA Ophthalmol 131(4):525–530
Yoshikawa M, Murakami T, Nishijima K et al (2013) Macular migration toward the optic disc after inner limiting membrane peeling for diabetic macular edema. Invest Ophthalmol Vis Sci 54:629–635
Gaudric A, Tadayoni R. (2013) Macular hole. In: Retina 5th ed. Ryan SJ. P.1962-1978
Franze K, Grosche J, Skatchkov SN et al (2007) Müller cells are living optical fibers in the vertebrate retina. Proc Natl Acad Sci U S A 104(20):8287–8292
Mitamura Y, Ohtsuka K (2005) Relationship of dissociated optic nerve fiber layer appearance to internal limiting membrane peeling. Ophthalmology 112:1766–1770
Ito Y, Terasaki H, Takahashi A et al (2005) Dissociated optic nerve fiber layer appearance after internal limiting membrane peeling for idiopathic macular holes. Ophthalmology 112:1415–1420
Nukada K, Hangai M, Ooto S et al (2013) Tomographic features of macula after successful macular hole surgery. Invest Ophthalmol Vis Sci Published online as manuscript iovs 12-10838
DeCroos FC, Toth CA, Folgar FA et al (2012) Characterisation of vitreoretinal interface disorders using OCT in the interventional phase 3 trials of Ocriplasmin. Invest Ophthalmol Vis Sci 53(10):6504–6511
Tsui I, Pan CK, Rahimy E, Schwartz SD. (2012) Ocriplasmin for Vitreoretinal Diseases. J Biomed Biotechnol Article ID 354979, 6 pages doi:10.1155/2012/354979
Folgar FA, Toth CA, DeCroos FC et al (2012) Assessment of retinal morphology with spectral and time domain OCT in the phase III trials of enzymatic vitreolysis. Invest Ophthalmol Vis Sci 53(11):7395–7401
Schneider EW, Johnson MW (2011) Emerging nonsurgical methods for the treatment of vitreomacular adhesion: a review. Clin Ophthalmol 5:1151–1165
Gandorfer A, Rohleder M, Sethi C et al (2004) Posterior vitreous detachment induced by microplasmin. Invest Ophthalmol Vis Sci 45(2):641–647
Sakuma T, Tanaka M, Mizota A et al (2005) Safety of in vivo pharmacologic vitreolysis with recombinant microplasmin in rabbit eyes. Invest Ophthalmol Vis Sci 46(9):3295–3299
De Smet MD, Valmaggia C, Zarranz-Ventura J et al (2009) Microplasmin: ex vivo characterization of its activity in porcine vitreous. Invest Ophthalmol Vis Sci 50(2):814–819
Stalmans P, Benz MS, Gandorfer A et al (2012) Enzymatic vitreolysis with Ocriplasmin for vitreomacular traction and macular holes. N Engl J Med 367(7):606–615
Tognetto D, Grandin R, Sanguinetti G et al (2006) Internal limiting membrane removal during macular hole surgery: results of a multicenter retrospective study. Ophthalmology 113:1401–1410
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Supplemental Digital Content Stage 2 Macular Hole
Below is the link to the electronic supplementary material.
(MPG 81047 kb)
Rights and permissions
About this article
Cite this article
Ho, TC., Yang, CM., Huang, JS. et al. Foveola nonpeeling internal limiting membrane surgery to prevent inner retinal damages in early stage 2 idiopathic macula hole. Graefes Arch Clin Exp Ophthalmol 252, 1553–1560 (2014). https://doi.org/10.1007/s00417-014-2613-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-014-2613-7