Abstract
Aim
For the treatment of complex pelvic organ prolapse, many different surgical procedures are described without any comparative studies available. Laparoscopic ventral mesh rectopexy after D’Hoore is one of the methods, which is publicized to treat patients with symptomatic rectocele, enterocele and rectal prolapse.
Method
All patients who received ventral mesh rectopexy since 07/10 for symptomatic rectocele, enterocele and possible rectal prolapse I ° or II ° in terms of a complex pelvic floor disorder were included in this follow-up study. The Wexner score for incontinence was recorded (range 0–20), the constipation score of Herold (r6-30) was evaluated as well as supplementary questions compiled by D’Hoore concerning outlet symptoms (r0-20). In addition, the quality of life (SF-12) was requested.
Results
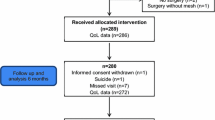
Thirty-one women were operated in the period, and 27 were eligible to be included in the present study. Median follow-up was 22 months (2–39). The preoperative Wexner score was in median 8 (0–20), going down to 6 (0–20) without significance (p = 0.735). The constipation score decreased significantly from median 14 (9–21) to 11 (6–25) (p = 0.007). The median score after D’Hoore was preoperatively 8 (4–16) and 4.5 (0–17) postoperatively (p = 0.004). The SF-12 values were preoperatively significantly reduced compared to the normal population; postoperatively, they equalized.
Conclusion
Two years after laparoscopic ventral mesh rectopexy, constipation and quality of life improve significantly in patients with complex pelvic organ prolapse. The grade of incontinence remains essentially the same, but was not the dominant clinical problem in the treated patients of our study.
Statement
The improvement in constipation and quality of life after laparoscopic ventral mesh rectopexy for obstructive defecation is encouraging. However, the impact on sexual life differs; some patients improve but a relevant number reports a change for the worse.

Similar content being viewed by others
References
DeLancey JO (1999) Structural anatomy of the posterior pelvic compartment as it relates to rectocele. Am J Obstet Gynecol 180(4):815–823
Schafer AO, Burk J, Baumann T, Langer M (2012) MR defaecography for the diagnosis of obstructive defaecation disorders. Zentralbl Chir 137(4):352–356. doi:10.1055/s-0032-1315103
Shorvon PJ, McHugh S, Diamant NE, Somers S, Stevenson GW (1989) Defecography in normal volunteers: results and implications. Gut 30(12):1737–1749
Zbar AP, Lienemann A, Fritsch H, Beer-Gabel M, Pescatori M (2003) Rectocele: pathogenesis and surgical management. Int J Colorectal Dis 18(5):369–384. doi:10.1007/s00384-003-0478-z
Gagliardi G, Pescatori M, Altomare DF, Binda GA, Bottini C, Dodi G, Filingeri V, Milito G, Rinaldi M, Romano G, Spazzafumo L, Trompetto M, Italian Society of Colo-Rectal S (2008) Results, outcome predictors, and complications after stapled transanal rectal resection for obstructed defecation. Dis Colon Rectum 51(2):186–195. doi:10.1007/s10350-007-9096-0, discussion 195
Thornton MJ, Lam A, King DW (2005) Laparoscopic or transanal repair of rectocele? A retrospective matched cohort study. Dis Colon Rectum 48(4):792–798. doi:10.1007/s10350-004-0843-1
Abet E, Lehur PA, Wong M, Rigaud J, Darnis E, Meurette G (2012) Sexual function and laparoscopic ventral rectopexy for complex rectocoele. Colorectal Dis 14(10):e721–e726. doi:10.1111/j.1463-1318.2012.03113.x
D’Hoore A, Cadoni R, Penninckx F (2004) Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg 91(11):1500–1505. doi:10.1002/bjs.4779
Braun M (2005) Evaluierung eines Scores zur Unterscheidung verschiedener Obstipationsformen (hier: Outlet-Obstruction und Slow-Transit-Obstipation). Karl-Ruprechts-Universität Heidelberg, Heidelberg
D’Hoore A, Vanbeckevoort D, Penninckx F (2008) Clinical, physiological and radiological assessment of rectovaginal septum reinforcement with mesh for complex rectocele. Br J Surg 95(10):1264–1272. doi:10.1002/bjs.6322
Lundby L, Laurberg S (2014) Laparoscopic ventral mesh rectopexy for ODS—time for a critical appraisal. Colorectal Dis. doi:10.1111/codi.12830
Collinson R, Wijffels N, Cunningham C, Lindsey I (2010) Laparoscopic ventral rectopexy for internal rectal prolapse: short-term functional results. Colorectal Dis 12(2):97–104. doi:10.1111/j.1463-1318.2009.02049.x, CDI2049 [pii]
Portier G, Kirzin S, Cabarrot P, Queralto M, Lazorthes F (2011) The effect of abdominal ventral rectopexy on faecal incontinence and constipation in patients with internal intra-anal rectal intussusception. Colorectal Dis 13(8):914–917. doi:10.1111/j.1463-1318.2010.02327.x, CDI2327 [pii]
Slawik S, Soulsby R, Carter H, Payne H, Dixon AR (2008) Laparoscopic ventral rectopexy, posterior colporrhaphy and vaginal sacrocolpopexy for the treatment of recto-genital prolapse and mechanical outlet obstruction. Colorectal Dis 10(2):138–143. doi:10.1111/j.1463-1318.2007.01259.x, CDI1259 [pii]
van den Esschert JW, Van Geloven AA, Vermulst N, Groenedijk AG, De Wit LT, Gerhards MF (2008) Laparoscopic ventral rectopexy for obstructed defecation syndrome. Surg Endosc 22(12):2728–2732. doi:10.1007/s00464-008-9771-9
Wong MT, Abet E, Rigaud J, Frampas E, Lehur PA, Meurette G (2011) Minimally invasive ventral mesh rectopexy for complex rectocoele: impact on anorectal and sexual function. Colorectal Dis 13(10):e320–e326. doi:10.1111/j.1463-1318.2011.02688.x
Oom DM, Gosselink MP, Van Wijk JJ, Van Dijl VR, Schouten WR (2008) Rectocele repair by anterolateral rectopexy: long-term functional outcome. Colorectal Dis 10(9):925–930. doi:10.1111/j.1463-1318.2008.01538.x, CDI1538 [pii]
Von Papen M, Ashari LH, Lumley JW, Stevenson AR, Stitz RW (2007) Functional results of laparoscopic resection rectopexy for symptomatic rectal intussusception. Dis Colon Rectum 50(1):50–55. doi:10.1007/s10350-006-0781-1
Laubert T, Kleemann M, Roblick UJ, Burk C, Schorcht A, Hildebrand P, Bruch HP (2012) Laparoscopic resection rectopexy as treatment for obstructive defecation syndrome. Zentralbl Chir 137(4):357–363. doi:10.1055/s-0032-1315125
Kellokumpu IH, Vironen J, Scheinin T (2000) Laparoscopic repair of rectal prolapse: a prospective study evaluating surgical outcome and changes in symptoms and bowel function. Surg Endosc 14(7):634–640. doi:10.1007/s004640000017 [pii]
Borie F, Bigourdan JM, Pissas MH, Guillon F (2014) Laparoscopic ventral rectopexy for the treatment of outlet obstruction associated with recto-anal intussusception and rectocele: a valid alternative to STARR procedure in patients with anal sphincter weakness. Clinics and research in hepatology and gastroenterology 38(4):528–534. doi:10.1016/j.clinre.2013.12.010
Festen S, Van Geloven AA, D’Hoore A, Lindsey I, Gerhards MF (2011) Controversy in the treatment of symptomatic internal rectal prolapse: suspension or resection? Surg Endosc 25(6):2000–2003. doi:10.1007/s00464-010-1501-4
Reibetanz J, Boenicke L, Kim M, Germer CT, Isbert C (2011) Enterocele is not a contraindication to stapled transanal surgery for outlet obstruction: an analysis of 170 patients. Colorectal Dis 13(6):e131–e136. doi:10.1111/j.1463-1318.2011.02554.x
Badrek-Al Amoudi AH, Greenslade GL, Dixon AR (2013) How to deal with complications after laparoscopic ventral mesh rectopexy: lessons learnt from a tertiary referral centre. Colorectal Dis 15(6):707–712. doi:10.1111/codi.12164
Van Geluwe B, Wolthuis A, Penninckx F, D’Hoore A (2013) Lessons learned after more than 400 laparoscopic ventral rectopexies. Acta Chir Belg 113(2):103–106
Senapati A, Gray RG, Middleton LJ, Harding J, Hills RK, Armitage NC, Buckley L, Northover JM, Group PC (2013) PROSPER: a randomised comparison of surgical treatments for rectal prolapse. Colorectal Dis 15(7):858–868. doi:10.1111/codi.12177
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Horisberger, K., Rickert, A., Templin, S. et al. Laparoscopic ventral mesh rectopexy in complex pelvic floor disorder. Int J Colorectal Dis 31, 991–996 (2016). https://doi.org/10.1007/s00384-016-2545-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-016-2545-2