Abstract
Purpose
The aim of this study was to determine the incidence of gastroschisis-related complications (GRCs) after closure of the abdominal wall defect, with a focus on frequency, type and timing of required surgical interventions, and to identify the impact of these on further outcome.
Methods
All gastroschisis patients treated from 1975 to 2008 in a tertiary-level center were retrospectively reviewed. Surgical procedures for GRCs following abdominal wall closure of simple gastroschisis [SG (intact continuous bowel)] and complex gastroschisis [CG (additional gastrointestinal malformations)] were compared, and outcomes were determined.
Results
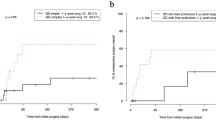
One hundred and eight patients were identified with a median follow-up of 15.0 years (range 4–37). Ninety-four (87 %) had SG, and 14 (13 %) CG. Surgical interventions for GRCs were performed in 28 (26 %) patients with 16 requiring multiple operations. Overall, 60 surgical procedures were performed. Bowel obstruction (n = 34) was the most common GRC, followed by anastomotic stricture (n = 8) and ischemic bowel (n = 3). The median interval between gastroschisis closure and secondary surgery for GRCs was 62.5 days (range 1 day–15 years). Surgical interventions were significantly more frequent in CG compared with SG [12/14 (86 %) vs. 16/94 (17 %); P < 0.0001]. The overall survival rate was 90 %. Significantly, more patients required parenteral nutrition for more than 28 days [9/28 (32 %) vs. 13/80 (16 %); P = 0.0468], longer median time to achieve full enteral feedings (87 vs. 33 days; P < 0.0001) and longer median hospital stay (117 vs. 54 days; P < 0.0001) compared with those not requiring additional surgery.
Conclusion
GRCs requiring surgical interventions were more common in patients with CG, which were associated with delay in achieving full enteral feedings and prolonged hospital stay.

Similar content being viewed by others
References
Holland AJ, Walker K, Badawi N (2010) Gastroschisis: an update. Pediatr Surg Int 26(9):871–878
Fillingham A, Rankin J (2008) Prevalence, prenatal diagnosis and survival of gastroschisis. Prenat Diagn 28(13):1232–1237
Nichol PF, Byrne JL, Dodgion C et al (2008) Clinical considerations in gastroschisis: incremental advances against a congenital anomaly with severe secondary effects. Am J Med Genet C Semin Med Genet 148C(3):231–240
Cusick E, Spicer RD, Beck JM (1997) Small-bowel continuity: a crucial factor in determining survival in gastroschisis. Pediatr Surg Int 12(1):34–37
Fleet MS, de la Hunt MN (2000) Intestinal atresia with gastroschisis: a selective approach to management. J Pediatr Surg 35(9):1323–1325
Hoehner JC, Ein SH, Kim PC (1998) Management of gastroschisis with concomitant jejuno-ileal atresia. J Pediatr Surg 33(6):885–888
Snyder CL, Miller KA, Sharp RJ et al (2001) Management of intestinal atresia in patients with gastroschisis. J Pediatr Surg 36(10):1542–1545
Abdullah F, Arnold MA, Nabaweesi R et al (2007) Gastroschisis in the United States 1988–2003: analysis and risk categorization of 4344 patients. J Perinatol 27(1):50–55
Marven S, Owen A (2008) Contemporary postnatal surgical management strategies for congenital abdominal wall defects. Semin Pediatr Surg 17(4):222–235
Aldrink JH, Caniano DA, Nwomeh BC (2012) Variability in gastroschisis management: a survey of North American pediatric surgery training programs. J Surg Res 176(1):159–163
Zani A, Ruttenstock E, Davenport M et al (2013) Is there Unity in Europe? First survey of EUPSA delegates on the management of gastroschisis. Eur J Pediatr Surg 23(1):19–24
Owen A, Marven S, Jackson L et al (2006) Experience of bedside preformed silo staged reduction and closure for gastroschisis. J Pediatr Surg 41(11):1830–1835
Pastor AC, Phillips JD, Fenton SJ et al (2008) Routine use of a SILASTIC spring-loaded silo for infants with gastroschisis: a multicenter randomized controlled trial. J Pediatr Surg 43(10):1807–1812
van Eijck FC, Wijnen RM, van Goor H (2008) The incidence and morbidity of adhesions after treatment of neonates with gastroschisis and omphalocele: a 30-year review. J Pediatr Surg 43(3):479–483
Arnold MA, Chang DC, Nabaweesi R et al (2007) Risk stratification of 4,344 patients with gastroschisis into simple and complex categories. J Pediatr Surg 42(9):1520–1525
Boutros J, Regier M, Skarsgard ED (2009) Is timing everything? The influence of gestational age, birth weight, route, and intent of delivery on outcome in gastroschisis. J Pediatr Surg 44(5):912–917
Baerg J, Kaban G, Tonita J et al (2003) Gastroschisis: a sixteen-year review. J Pediatr Surg 38(5):771–774
Eggink BH, Richardson CJ, Malloy MH et al (2006) Outcome of gastroschisis: a 20-year case review of infants with gastroschisis born in Galveston, Texas. J Pediatr Surg 41(6):1103–1108
Owen A, Marven S, Johnson P et al (2010) Gastroschisis: a national cohort study to describe contemporary surgical strategies and outcomes. J Pediatr Surg 45(9):1808–1816
Bradnock TJ, Marven S, Owen A et al (2011) Gastroschisis: one year outcomes from national cohort study. BMJ 343:d6749
Koivusalo A, Lindahl H, Rintala RJ (2002) Morbidity and quality of life in adult patients with a congenital abdominal wall defect: a questionnaire survey. J Pediatr Surg 37(11):1594–1601
Davies BW, Stringer MD (1997) The survivors of gastroschisis. Arch Dis Child 77(2):158–160
Wilkins BM, Spitz L (1986) Incidence of postoperative adhesion obstruction following neonatal laparotomy. Br J Surg 73(9):762–764
Grant HW, Parker MC, Wilson MS et al (2006) Population-based analysis of the risk of adhesion-related readmissions after abdominal surgery in children. J Pediatr Surg 41(8):1453–1456
Langer JC, Longaker MT, Crombleholme TM et al (1989) Etiology of intestinal damage in gastroschisis. I: effects of amniotic fluid exposure and bowel constriction in a fetal lamb model. J Pediatr Surg 24(10):992–997
Correia-Pinto J, Tavares ML, Baptista MJ et al (2002) Meconium dependence of bowel damage in gastroschisis. J Pediatr Surg 37(1):31–35
Bealer JF, Graf J, Bruch SW et al (1996) Gastroschisis increases small bowel nitric oxide synthase activity. J Pediatr Surg 31(8):1043–1045
Shah R, Woolley MM (1991) Gastroschisis and intestinal atresia. J Pediatr Surg 26(7):788–790
Tunell WP, Puffinbarger NK, Tuggle DW et al (1995) Abdominal-wall defects in infants: survival and implications for adult life. Ann Surg 221(5):525–530
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Friedmacher, F., Hock, A., Castellani, C. et al. Gastroschisis-related complications requiring further surgical interventions. Pediatr Surg Int 30, 615–620 (2014). https://doi.org/10.1007/s00383-014-3500-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-014-3500-3