Abstract
Objective
To determine all-cause mortality risk in patients with and without adrenal incidentaloma.
Methods
Retrospective cohort study of patients with CT abdomen performed within 24 h of emergency room presentation at an academic medical center from January 1, 2005, to December 31, 2009, without history of adrenal disease, adrenal lab testing, or cancer. Incidentaloma cohort identified by database query of imaging reports followed by manual review and matched to no-nodule controls at 3:1 on age ± 1 year and exam date ± 3 months. Mortality ascertained by in-hospital deaths and National Death Index query. Survival analysis performed with Kaplan-Meier curves and Cox proportional hazards models.
Results
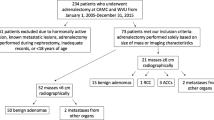
Among 42,575 adults with abdominal CT exams, 969 adrenal incidentaloma patients and 2907 no-nodule controls were identified. All 3876 individuals entered survival analysis with 31,182 person-years at risk (median follow-up 8.9 years [IQR, 6.9–10.7]). All-cause mortality was significantly higher among those with adrenal incidentalomas (353/969, 36.4%) compared with those without (919/2907, 31.6%; mortality difference 7.6 per 1000 person-years; multivariable-adjusted hazard ratio [aHR] 1.14; 95% CI, 1.003–1.29). Exploratory analyses, limited by missing covariates, found that adrenal incidentalomas were associated with significantly increased incidence of malignancy (aHR 1.61; 95% CI, 1.22–2.12), diabetes (aHR 1.43; 95% CI, 1.18–1.71), heart failure (aHR 1.32; 95% CI, 1.07–1.63), peripheral vascular disease (aHR 1.28; 95% CI, 1.95–1.56), renal disease (aHR 1.21; 95% CI, 1.01–1.44), and chronic pulmonary disease (aHR 1.22; 95% CI, 1.01–1.46) compared with controls.
Conclusions
Adrenal incidentalomas are associated with increased mortality and may represent a clinically valuable biomarker.
Key Points
• Adrenal incidentalomas are associated with increased mortality.
• Adrenal incidentaloma size is not predictive of mortality.
• On exploratory analyses, adrenal incidentalomas are associated with chronic illnesses.




Similar content being viewed by others
Abbreviations
- AACE:
-
American Association of Clinical Endocrinologists
- AAES:
-
American Association of Endocrine Surgeons
- ACR:
-
American College of Radiology
- aHR:
-
Adjusted hazard ratio
- CI:
-
Confidence interval
- ICD-9:
-
International Classification of Diseases Ninth Revision
- IQR:
-
Interquartile range
- NDI:
-
National Death Index
- SD:
-
Standard deviation
References
Grumbach MM, Biller BM, Braunstein GD et al (2003) Management of the clinically inapparent adrenal mass (“incidentaloma”). Ann Intern Med 138:424–429
Young WF Jr (2007) Clinical practice. The incidentally discovered adrenal mass. N Engl J Med 356:601–610
Song JH, Chaudhry FS, Mayo-Smith WW (2008) The incidental adrenal mass on CT: prevalence of adrenal disease in 1,049 consecutive adrenal masses in patients with no known malignancy. AJR Am J Roentgenol 190:1163–1168
Hu M, Yip R, Yankelevitz DY, Henschke CI (2016) CT screening for lung cancer: frequency of enlarged adrenal glands identified in baseline and annual repeat rounds. Eur Radiol 26:4475–4481
Mayo-Smith WW, Song JH, Boland GL et al (2017) Management of incidental adrenal masses: a white paper of the ACR incidental findings committee. J Am Coll Radiol 14:1038–1044
Berland LL, Silverman SG, Gore RM et al (2010) Managing incidental findings on abdominal CT: white paper of the ACR incidental findings committee. J Am Coll Radiol 7:754–773
Zeiger MA, Thompson GB, Duh QY et al (2009) American Association of Clinical Endocrinologists and American Association of Endocrine Surgeons Medical Guidelines for the management of adrenal incidentalomas: executive summary of recommendations. Endocr Pract 15:450–453
Fassnacht M, Arlt W, Bancos I et al (2016) Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the study of adrenal tumors. Eur J Endocrinol 175:G1–G34
Kastelan D, Kraljevic I, Dusek T et al (2015) The clinical course of patients with adrenal incidentaloma: is it time to reconsider the current recommendations? Eur J Endocrinol 173:275–282
Cawood TJ, Hunt PJ, O'Shea D, Cole D, Soule S (2009) Recommended evaluation of adrenal incidentalomas is costly, has high false-positive rates and confers a risk of fatal cancer that is similar to the risk of the adrenal lesion becoming malignant; time for a rethink? Eur J Endocrinol 161:513–527
Kaltsas G, Chrisoulidou A, Piaditis G, Kassi E, Chrousos G (2012) Current status and controversies in adrenal incidentalomas. Trends Endocrinol Metab 23:602–609
Di Dalmazi G, Vicennati V, Garelli S et al (2014) Cardiovascular events and mortality in patients with adrenal incidentalomas that are either non-secreting or associated with intermediate phenotype or subclinical Cushing's syndrome: a 15-year retrospective study. Lancet Diabetes Endocrinol 2:396–405
Morelli V, Reimondo G, Giordano R et al (2014) Long-term follow-up in adrenal incidentalomas: an Italian multicenter study. J Clin Endocrinol Metab 99:827–834
Debono M, Bradburn M, Bull M, Harrison B, Ross RJ, Newell-Price J (2014) Cortisol as a marker for increased mortality in patients with incidental adrenocortical adenomas. J Clin Endocrinol Metab 99:4462–4470
Patrova J, Kjellman M, Wahrenberg H, Falhammar H (2017) Increased mortality in patients with adrenal incidentalomas and autonomous cortisol secretion: a 13-year retrospective study from one center. Endocrine 58:267–275
Lopez D, Luque-Fernandez MA, Steele A, Adler GK, Turchin A, Vaidya A (2016) “Nonfunctional” adrenal tumors and the risk for incident diabetes and cardiovascular outcomes: a cohort study. Ann Intern Med 165:533–542
Becker J, Woloszyn J, Bold R, Campbell MJ (2018) The adrenal incidentaloma: an opportunity to improve patient care. J Gen Intern Med 33:256
Bellin E, Fletcher DD, Geberer N, Islam S, Srivastava N (2010) Democratizing information creation from health care data for quality improvement, research, and education-the Montefiore Medical Center Experience. Acad Med 85:1362–1368
Bellin E (2017) How to ask and answer questions using electronic medical record data. CreateSpace, North Charleston, South Carolina
Bellin E (2015) Riddles in accountable healthcare: a primer to develop analytic intuition for medical homes and population health. CreateSpace, North Charleston, South Carolina
Quan H, Li B, Couris CM et al (2011) Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol 173:676–682
Quan H, Sundararajan V, Halfon P et al (2005) Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care 43:1130–1139
Hong AR, Kim JH, Park KS et al (2017) Optimal follow-up strategies for adrenal incidentalomas: reappraisal of the 2016 ESE-ENSAT guidelines in real clinical practice. Eur J Endocrinol 177:475–483
Androulakis II, Kaltsas GA, Kollias GE et al (2014) Patients with apparently nonfunctioning adrenal incidentalomas may be at increased cardiovascular risk due to excessive cortisol secretion. J Clin Endocrinol Metab 99:2754–2762
Akkan T, Altay M, Unsal Y, Dagdeviren M, Beyan E (2017) Nonfunctioning adrenal incidentaloma affecting central blood pressure and arterial stiffness parameters. Endocrine 58:513–520
Muscogiuri G, Colao A, Orio F (2015) Insulin-mediated diseases: adrenal mass and polycystic ovary syndrome. Trends Endocrinol Metab 26:512–514
Peppa M, Boutati E, Koliaki C et al (2010) Insulin resistance and metabolic syndrome in patients with nonfunctioning adrenal incidentalomas: a cause-effect relationship? Metabolism 59:1435–1441
Kamio T, Shigematsu K, Kawai K, Tsuchiyama H (1991) Immunoreactivity and receptor expression of insulinlike growth factor I and insulin in human adrenal tumors. An immunohistochemical study of 94 cases. Am J Pathol 138:83–91
Ilvesmaki V, Kahri AI, Miettinen PJ, Voutilainen R (1993) Insulin-like growth factors (IGFs) and their receptors in adrenal tumors: high IGF-II expression in functional adrenocortical carcinomas. J Clin Endocrinol Metab 77:852–858
Corwin MT, Chalfant JS, Loehfelm TW, Fananapazir G, Lamba R, Mayo-Smith WW (2018) Incidentally detected bilateral adrenal nodules in patients without cancer: is further workup necessary? AJR Am J Roentgenol 210:780–784
Derwahl M, Studer H (2002) Hyperplasia versus adenoma in endocrine tissues: are they different? Trends Endocrinol Metab 13:23–28
Acknowledgements
The preliminary findings were presented as an oral presentation at the Radiological Society of North America Annual Meeting, November 26, 2018, Chicago, IL.
Funding
This study has received funding by the Einstein Montefiore Department of Radiology and a National Institutes of Health Clinical and Translational Science Awards grant number 1UL-1TR001073 from the National Center for Advancing Translational Sciences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Michio Taya, MD MS.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
The first author has significant statistical expertise.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 570 kb)
Rights and permissions
About this article
Cite this article
Taya, M., Paroder, V., Bellin, E. et al. The relationship between adrenal incidentalomas and mortality risk. Eur Radiol 29, 6245–6255 (2019). https://doi.org/10.1007/s00330-019-06202-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06202-y