Abstract
Purpose
The aim of this study was to systematically review and conduct a meta-analysis of published data about the diagnostic performance of 18F-dihydroxyphenylalanine (DOPA) positron emission tomography (PET) in patients with paraganglioma (PG).
Methods
A comprehensive computer literature search of studies published through 30 June 2011 regarding 18F-DOPA PET or PET/computed tomography (PET/CT) in patients with PG was performed in PubMed/MEDLINE, Embase and Scopus databases. Pooled sensitivity and specificity of 18F-DOPA PET or PET/CT in patients with PG on a per patient- and on a per lesion-based analysis were calculated. The area under the receiver-operating characteristic (ROC) curve was calculated to measure the accuracy of 18F-DOPA PET or PET/CT in patients with PG. Furthermore, a sub-analysis taking into account the different genetic mutations in PG patients was also performed.
Results
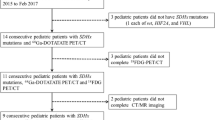
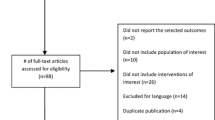
Eleven studies comprising 275 patients with suspected PG were included in this meta-analysis. The pooled sensitivity of 18F-DOPA PET and PET/CT in detecting PG was 91% [95% confidence interval (CI) 87–94%] on a per patient-based analysis and 79% (95% CI 76–81%) on a per lesion-based analysis. The pooled specificity of 18F-DOPA PET and PET/CT in detecting PG was 95% (95% CI 86–99%) on a per patient-based analysis and 95% (95% CI 84–99%) on a per lesion-based analysis. The area under the ROC curve was 0.95 on a per patient- and 0.94 on a per lesion-based analysis. Heterogeneity between the studies about sensitivity of 18F-DOPA PET or PET/CT was found. A significant increase in sensitivity of 18F-DOPA PET or PET/CT was observed when a sub-analysis excluding patients with succinate dehydrogenase subunit B (SDHB) gene mutations was performed.
Conclusion
In patients with suspected PG 18F-DOPA PET or PET/CT demonstrated high sensitivity and specificity. 18F-DOPA PET or PET/CT are accurate methods in this setting. Nevertheless, possible sources of false-negative results should be kept in mind. Furthermore, SDHB gene mutations could influence 18F-DOPA PET or PET/CT diagnostic performance.






Similar content being viewed by others
References
Solcia E, Kloppel G, Sobin L. Histological typing of the endocrine tumours. 2nd ed. Berlin: Springer; 2000.
Goldstein RE, O’Neill Jr JA, Holcomb III GW, Morgan III WM, Neblett III WW, Oates JA, et al. Clinical experience over 48 years with pheochromocytoma. Ann Surg 1999;229:755–64.
Havekes B, King K, Lai EW, Romijn JA, Corssmit EP, Pacak K. New imaging approaches to phaeochromocytomas and paragangliomas. Clin Endocrinol (Oxf) 2010;72:137–45.
Rufini V, Calcagni ML, Baum RP. Imaging of neuroendocrine tumors. Semin Nucl Med 2006;36:228–47.
Taïeb D, Rubello D, Al-Nahhas A, Calzada M, Marzola MC, Hindié E. Modern PET imaging for paragangliomas: relation to genetic mutations. Eur J Surg Oncol 2011;37:662–8.
Brink I, Hoegerle S, Klisch J, Bley TA. Imaging of pheochromocytoma and paraganglioma. Fam Cancer 2005;4:61–8.
Jager PL, Chirakal R, Marriott CJ, Brouwers AH, Koopmans KP, Gulenchyn KY. 6-L-18F-fluorodihydroxyphenylalanine PET in neuroendocrine tumors: basic aspects and emerging clinical applications. J Nucl Med 2008;49:573–86.
Eisenhofer G. The role of neuronal and extraneuronal plasma membrane transporters in the inactivation of peripheral catecholamines. Pharmacol Ther 2001;91:35–62.
Bergström M, Eriksson B, Oberg K, Sundin A, Ahlström H, Lindner KJ, et al. In vivo demonstration of enzyme activity in endocrine pancreatic tumors: decarboxylation of carbon-11-DOPA to carbon-11-dopamine. J Nucl Med 1996;37:32–7.
Whiting PF, Weswood ME, Rutjes AW, Reitsma JB, Bossuyt PN, Kleijnen J. Evaluation of QUADAS, a tool for the quality assessment of diagnostic accuracy studies. BMC Med Res Methodol 2006;6:9.
Van den Bruel A, Thompson MJ, Haj-Hassan T, Stevens R, Moll H, Lakhanpaul M, Mant D. Diagnostic value of laboratory tests in identifying serious infections in febrile children: systematic review. BMJ 2011;342:d3082.
Zamora J, Abraira V, Muriel A, Khan K, Coomarasamy A. Meta-DiSc: a software for meta-analysis of test accuracy data. BMC Med Res Methodol 2006;6:31.
Levine DS, Metzger DL, Nadel HR, Oviedo A, Adam MJ, Skarsgard E. Novel use of F-DOPA PET/CT imaging in a child with paraganglioma/pheochromocytoma syndrome. Pediatr Radiol 2011;41:1321–5. doi:10.1007/s00247-011-2109-0.
Grassi I, Nanni C, Vicennati V, Castellucci P, Allegri V, Montini GC, et al. I-123 MIBG scintigraphy and 68Ga-DOTANOC PET/CT negative but F-18 DOPA PET/CT positive pheochromocytoma: a case report. Clin Nucl Med 2011;36:124–6.
King KS, Whatley MA, Alexopoulos DK, Reynolds JC, Chen CC, Mattox DE, et al. The use of functional imaging in a patient with head and neck paragangliomas. J Clin Endocrinol Metab 2010;95:481–2.
Fiebrich HB, Brouwers AH, van Bergeijk L, van den Berg G. Image in endocrinology. Localization of an adrenocorticotropin-producing pheochromocytoma using 18F-dihydroxyphenylalanine positron emission tomography. J Clin Endocrinol Metab 2009;94:748–9.
Mackenzie IS, Gurnell M, Balan KK, Simpson H, Chatterjee K, Brown MJ. The use of 18-fluoro-dihydroxyphenylalanine and 18-fluorodeoxyglucose positron emission tomography scanning in the assessment of metaiodobenzylguanidine-negative phaeochromocytoma. Eur J Endocrinol 2007;157:533–7.
Brink I, Schaefer O, Walz M, Neumann HP. Fluorine-18 DOPA PET imaging of paraganglioma syndrome. Clin Nucl Med 2006;31:39–41.
Timmers HJ, Hadi M, Carrasquillo JA, Chen CC, Martiniova L, Whatley M, et al. The effects of carbidopa on uptake of 6-18F-fluoro-L-DOPA in PET of pheochromocytoma and extraadrenal abdominal paraganglioma. J Nucl Med 2007;48:1599–606.
Boedeker CC, Neumann HP, Maier W, Bausch B, Schipper J, Ridder GJ. Malignant head and neck paragangliomas in SDHB mutation carriers. Otolaryngol Head Neck Surg 2007;137:126–9.
Boedeker CC, Neumann HP, Ridder GJ, Maier W, Schipper J. Paragangliomas in patients with mutations of the SDHD gene. Otolaryngol Head Neck Surg 2005;132:467–70.
Bausch B, Boedeker CC, Berlis A, Brink I, Cybulla M, Walz MK, et al. Genetic and clinical investigation of pheochromocytoma: a 22-year experience, from Freiburg, Germany to international effort. Ann N Y Acad Sci 2006;1073:122–37.
Hoegerle S, Nitzsche E, Altehoefer C, Ghanem N, Manz T, Brink I, et al. Pheochromocytomas: detection with 18F DOPA whole body PET–initial results. Radiology 2002;222:507–12.
Hoegerle S, Ghanem N, Altehoefer C, Schipper J, Brink I, Moser E, Neumann HP. 18F-DOPA positron emission tomography for the detection of glomus tumours. Eur J Nucl Med Mol Imaging 2003;30:689–94.
Taïeb D, Tessonnier L, Sebag F, Niccoli-Sire P, Morange I, Colavolpe C, et al. The role of 18F-FDOPA and 18F-FDG-PET in the management of malignant and multifocal phaeochromocytomas. Clin Endocrinol (Oxf) 2008;69:580–6.
Kauhanen S, Seppänen M, Ovaska J, Minn H, Bergman J, Korsoff P, et al. The clinical value of [18F]fluoro-dihydroxyphenylalanine positron emission tomography in primary diagnosis, staging, and restaging of neuroendocrine tumors. Endocr Relat Cancer 2009;16:255–65.
Imani F, Agopian VG, Auerbach MS, Walter MA, Imani F, Benz MR, et al. 18F-FDOPA PET and PET/CT accurately localize pheochromocytomas. J Nucl Med 2009;50:513–9.
Fiebrich HB, Brouwers AH, Kerstens MN, Pijl ME, Kema IP, de Jong JR, et al. 6-[F-18]Fluoro-L-dihydroxyphenylalanine positron emission tomography is superior to conventional imaging with (123)I-metaiodobenzylguanidine scintigraphy, computer tomography, and magnetic resonance imaging in localizing tumors causing catecholamine excess. J Clin Endocrinol Metab 2009;94:3922–30.
Timmers HJ, Chen CC, Carrasquillo JA, Whatley M, Ling A, Havekes B, et al. Comparison of 18F-fluoro-L-DOPA, 18F-fluoro-deoxyglucose, and 18F-fluorodopamine PET and 123I-MIBG scintigraphy in the localization of pheochromocytoma and paraganglioma. J Clin Endocrinol Metab 2009;94:4757–67.
Luster M, Karges W, Zeich K, Pauls S, Verburg FA, Dralle H, et al. Clinical value of 18F-fluorodihydroxyphenylalanine positron emission tomography/computed tomography (18F-DOPA PET/CT) for detecting pheochromocytoma. Eur J Nucl Med Mol Imaging 2010;37:484–93.
Fottner C, Helisch A, Anlauf M, Rossmann H, Musholt TJ, Kreft A, et al. 6-18F-fluoro-L-dihydroxyphenylalanine positron emission tomography is superior to 123I-metaiodobenzyl-guanidine scintigraphy in the detection of extraadrenal and hereditary pheochromocytomas and paragangliomas: correlation with vesicular monoamine transporter expression. J Clin Endocrinol Metab 2010;95:2800–10.
Charrier N, Deveze A, Fakhry N, Sebag F, Morange I, Gaborit B, et al. Comparison of [111In]pentetreotide-SPECT and [18F]FDOPA-PET in the localization of extra-adrenal paragangliomas: the case for a patient-tailored use of nuclear imaging modalities. Clin Endocrinol (Oxf) 2011;74:21–9.
Rufini V, Treglia G, Castaldi P, Perotti G, Calcagni ML, Corsello SM, et al. Comparison of 123I-MIBG SPECT-CT and 18F-DOPA PET-CT in the evaluation of patients with known or suspected recurrent paraganglioma. Nucl Med Commun 2011;32:575–82.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Treglia, G., Cocciolillo, F., de Waure, C. et al. Diagnostic performance of 18F-dihydroxyphenylalanine positron emission tomography in patients with paraganglioma: a meta-analysis. Eur J Nucl Med Mol Imaging 39, 1144–1153 (2012). https://doi.org/10.1007/s00259-012-2087-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-012-2087-y