Abstract
Introduction
The therapeutic efficacy of systemic Janus kinase (JAK) inhibitors in moderate-to-severe atopic dermatitis (AD) is well established. However, the associated risk of incident acne, which is a prevalent adverse event in AD patients treated with systemic JAK inhibitors, has yet to be systematically analyzed.
Methodology
To evaluate the risk of incident acne in AD patients treated with systemic JAK inhibitors, an extensive database search (clinicaltrials.gov, PubMed) was performed to identify publications eligible for inclusion from January 2020 to October 2022. Five randomized clinical trials (RCTs) of abrocitinib, four RCTs of upadacitinib, and one RCT of baricitinib, encompassing a total of 7901 participants, were included in the analysis. The risk difference for incident acne between systemic JAK inhibitors and controls was assessed using Review Manager, version 5.3, adhering to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.
Results
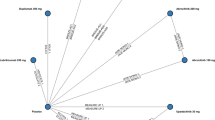
Meta-analysis elucidated a significant difference in the risk of incident acne between AD participants receiving 200 mg abrocitinib (Mantel–Haenszel risk difference, 3.69; 95% CI 1.60–8.48; P < 0.01), 15 mg upadacitinib (Mantel–Haenszel risk difference, 4.61; 95% CI 2.79–7.62; P < 0.00001), and 30 mg upadacitinib (Mantel–Haenszel risk difference, 6.82; 95% CI 4.59–10.13; P < 0.00001) compared with controls receiving placebo or dupilumab. In contrast, no significant difference was found in the risk of incident acne between participants receiving 100 mg abrocitinib, 2 mg baricitinib, and 4 mg baricitinib, as compared with controls.
Conclusions
Based on the current evidence, there is an increased risk of acne related to systemic JAK inhibitors, particularly with abrocitinib and upadacitinib. For patients predisposed to acne, the balance between the benefits of symptomatic relief from AD and the potential risk of acne may need to be carefully considered. This study contributes to a nuanced understanding of the risk profile of systemic JAK inhibitors and has the potential to guide personalized treatment decisions for AD patients.





Similar content being viewed by others
Availability of data and materials
All data generated or analyzed during this study are included in this published article and its supplementary information files.
Code availability
Not applicable.
References
Thomsen SF. Atopic dermatitis: natural history, diagnosis, and treatment. ISRN Allergy. 2014;2014: 354250. https://doi.org/10.1155/2014/354250.
Chen TL, Lee LL, Huang HK, Chen LY, Loh CH, Chi CC. Association of risk of incident venous thromboembolism with atopic dermatitis and treatment with janus kinase inhibitors: a systematic review and meta-analysis. JAMA Dermatol. 2022;158(11):1254–61. https://doi.org/10.1001/jamadermatol.2022.3516.
Kim J, Kim BE, Leung DYM. Pathophysiology of atopic dermatitis: clinical implications. Allergy Asthma Proc. 2019;40(2):84–92. https://doi.org/10.2500/aap.2019.40.4202.
Ferreira S, Guttman-Yassky E, Torres T. Selective JAK1 inhibitors for the treatment of atopic dermatitis: focus on upadacitinib and abrocitinib. Am J Clin Dermatol. 2020;21(6):783–98. https://doi.org/10.1007/s40257-020-00548-6.
Damsky W, Peterson D, Ramseier J, Al-Bawardy B, Chun H, Proctor D, et al. The emerging role of Janus kinase inhibitors in the treatment of autoimmune and inflammatory diseases. J Allergy Clin Immunol. 2021;147(3):814–26. https://doi.org/10.1016/j.jaci.2020.10.022.
Nezamololama N, Fieldhouse K, Metzger K, Gooderham M. Emerging systemic JAK inhibitors in the treatment of atopic dermatitis: a review of abrocitinib, baricitinib, and upadacitinib. Drugs Context. 2020;9:2020-8-5. https://doi.org/10.7573/dic.2020-8-5.
Chovatiya R, Paller AS. JAK inhibitors in the treatment of atopic dermatitis. J Allergy Clin Immunol. 2021;148(4):927–40. https://doi.org/10.1016/j.jaci.2021.08.009.
Deeks E, Duggan S. Correction to: Abrocitinib: first approval. Drugs. 2022;82(5):609. https://doi.org/10.1007/s40265-022-01694-3.
Silverberg JI, Simpson EL, Thyssen JP, Gooderham M, Chan G, Feeney C, et al. Efficacy and safety of abrocitinib in patients with moderate-to-severe atopic dermatitis: a randomized clinical trial. JAMA Dermatol. 2020;156(8):863–73. https://doi.org/10.1001/jamadermatol.2020.1406.
Thyssen JP, Yosipovitch G, Paul C, Kwatra SG, Chu CY, DiBonaventura M, et al. Patient-reported outcomes from the JADE COMPARE randomized phase 3 study of abrocitinib in adults with moderate-to-severe atopic dermatitis. J Eur Acad Dermatol Venereol. 2022;36(3):434–43. https://doi.org/10.1111/jdv.17813.
Wan H, Jia H, Xia T, Zhang D. Comparative efficacy and safety of abrocitinib, baricitinib, and upadacitinib for moderate-to-severe atopic dermatitis: a network meta-analysis. Dermatol Ther. 2022;35(9): e15636. https://doi.org/10.1111/dth.15636.
Drucker AM, Morra DE, Prieto-Merino D, Ellis AG, Yiu ZZN, Rochwerg B, et al. Systemic immunomodulatory treatments for atopic dermatitis: update of a living systematic review and network meta-analysis. JAMA Dermatol. 2022;158(5):523–32. https://doi.org/10.1001/jamadermatol.2022.0455.
Bieber T, Simpson EL, Silverberg JI, Thaci D, Paul C, Pink AE, et al. Comparing abrocitinib and dupilumab in the treatment of atopic dermatitis: a plain language summary. Immunotherapy. 2022;14(1):5–14. https://doi.org/10.2217/imt-2021-0224.
Wood H, Chandler A, Nezamololama N, Papp K, Gooderham MJ. Safety of Janus kinase (JAK) inhibitors in the short-term treatment of atopic dermatitis. Int J Dermatol. 2022;61(6):746–54. https://doi.org/10.1111/ijd.15853.
Han KH, Cho KH, Han C, Cui S, Lin L, Baek HY, Kim J. The effectiveness and safety of acupuncture treatment on sciatica: a systematic review and meta-analysis. Complement Ther Med. 2022;71: 102872. https://doi.org/10.1016/j.ctim.2022.102872.
Ryan C, Leonardi CL, Krueger JG, Kimball AB, Strober BE, Gordon KB, et al. Association between biologic therapies for chronic plaque psoriasis and cardiovascular events: a meta-analysis of randomized controlled trials. JAMA. 2011;306(8):864–71. https://doi.org/10.1001/jama.2011.1211.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557–60. https://doi.org/10.1136/bmj.327.7414.557.
Sterne JAC, Savovic J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366: l4898. https://doi.org/10.1136/bmj.l4898.
Tsai HR, Lu JW, Chen LY, Chen TL. Application of Janus kinase inhibitors in atopic dermatitis: an updated systematic review and meta-analysis of clinical trials. J Pers Med. 2021;11(4):279. https://doi.org/10.3390/jpm11040279.
Reich K, Teixeira HD, de Bruin-Weller M, Bieber T, Soong W, Kabashima K, et al. Safety and efficacy of upadacitinib in combination with topical corticosteroids in adolescents and adults with moderate-to-severe atopic dermatitis (AD Up): results from a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2021;397(10290):2169–81. https://doi.org/10.1016/S0140-6736(21)00589-4.
Saleiro D, Platanias LC. Intersection of mTOR and STAT signaling in immunity. Trends Immunol. 2015;36(1):21–9. https://doi.org/10.1016/j.it.2014.10.006.
Melnik BC. Diet in acne: further evidence for the role of nutrient signalling in acne pathogenesis. Acta Derm Venereol. 2012;92(3):228–31. https://doi.org/10.2340/00015555-1358.
Lee SD, Ahn HJ, Shin MK. A case series of acne following Janus kinase inhibitors in patients with atopic dermatitis. JAAD Case Rep. 2022;30:11–6. https://doi.org/10.1016/j.jdcr.2022.09.029.
Awad SM, Tawfik YM, El-Mokhtar MA, El-Gazzar AF, Abdel Motaleb AA. Activation of Janus kinase signaling pathway in acne lesions. Dermatol Ther. 2021;34(1): e14563. https://doi.org/10.1111/dth.14563.
Thyssen JP, Nymand LK, Maul JT, Schmid-Grendelmeier P, Wu JJ, Thomsen SF, Egeberg A. Incidence, prevalence and risk of acne in adolescent and adult patients with atopic dermatitis: a matched cohort study. J Eur Acad Dermatol Venereol. 2022;36(6):890–6. https://doi.org/10.1111/jdv.18027.
Ballanger F, Auffret N, Leccia MT, Claudel JP, Dréno B. Acneiform lesions but not acne after treatment with Janus kinase inhibitors: diagnosis and management of Janus kinase-acne. Acta Derm Venereol. 2023;103: adv11657. https://doi.org/10.2340/actadv.v103.11657.
Mendes-Bastos P, Ladizinski B, Guttman-Yassky E, Jiang P, Liu J, Prajapati VH, et al. Characterization of acne associated with upadacitinib treatment in patients with moderate-to-severe atopic dermatitis: a post hoc integrated analysis of 3 phase 3 randomized, double-blind, placebo-controlled trials. J Am Acad Dermatol. 2022;87(4):784–91. https://doi.org/10.1016/j.jaad.2022.06.012.
Reich K, Thyssen JP, Blauvelt A, Eyerich K, Soong W, Rice ZP, et al. Efficacy and safety of abrocitinib versus dupilumab in adults with moderate-to-severe atopic dermatitis: a randomised, double-blind, multicentre phase 3 trial. Lancet. 2022;400(10348):273–82. https://doi.org/10.1016/s0140-6736(22)01199-0.
Blauvelt A, Silverberg JI, Lynde CW, Bieber T, Eisman S, Zdybski J, et al. Abrocitinib induction, randomized withdrawal, and retreatment in patients with moderate-to-severe atopic dermatitis: results from the JAK1 Atopic dermatitis efficacy and safety (JADE) REGIMEN phase 3 trial. J Am Acad Dermatol. 2022;86(1):104–12. https://doi.org/10.1016/j.jaad.2021.05.075.
Eichenfield LF, Flohr C, Sidbury R, Siegfried E, Szalai Z, Galus R, et al. Efficacy and safety of abrocitinib in combination with topical therapy in adolescents with moderate-to-severe atopic dermatitis: the JADE TEEN randomized clinical trial. JAMA Dermatol. 2021;157(10):1165–73. https://doi.org/10.1001/jamadermatol.2021.2830.
Guttman-Yassky E, Teixeira HD, Simpson EL, Papp KA, Pangan AL, Blauvelt A, et al. Once-daily upadacitinib versus placebo in adolescents and adults with moderate-to-severe atopic dermatitis (measure Up 1 and measure Up 2): results from two replicate double-blind, randomised controlled phase 3 trials. Lancet. 2021;397(10290):2151–68. https://doi.org/10.1016/S0140-6736(21)00588-2.
Blauvelt A, Teixeira HD, Simpson EL, Costanzo A, De Bruin-Weller M, Barbarot S, et al. Efficacy and safety of upadacitinib vs dupilumab in adults with moderate-to-severe atopic dermatitis: a randomized clinical trial. JAMA Dermatol. 2021;157(9):1047–55. https://doi.org/10.1001/jamadermatol.2021.3023.
Reich K, Kabashima K, Peris K, Silverberg JI, Eichenfield LF, Bieber T, et al. Efficacy and safety of baricitinib combined with topical corticosteroids for treatment of moderate to severe atopic dermatitis: a randomized clinical trial. JAMA Dermatol. 2020;156(12):1333–43. https://doi.org/10.1001/jamadermatol.2020.3260.
Funding
This study was supported by National High Level Hospital Clinical Research Funding (2022-PUMCH-B-092).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. CS, ZS, and Y-PZ were responsible for material preparation, data collection and analysis. The first draft of the manuscript was written by CS and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no conflict of interest.
Ethical approval
Not applicable.
Consent to participate/publish
All authors have read and approved of the final version of the manuscript.
Additional information
Responsible Editor: John Di Battista.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sun, C., Su, Z. & Zeng, YP. Association of risk of incident acne and treatment with systemic Janus kinase inhibitors in atopic dermatitis: a systematic review and meta-analysis. Inflamm. Res. 72, 1861–1871 (2023). https://doi.org/10.1007/s00011-023-01789-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-023-01789-x