Abstract
Background
Although the increasing use of drugs in elderly persons has raised many concerns in recent years, the process leading to polypharmacy (PP) and excessive polypharmacy (EPP) remains largely unknown.
Objective
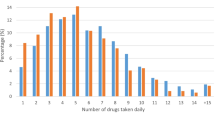
To describe the number and type of drugs used and to evaluate the role of different factors associated with PP (i.e. 6–9 drugs) and EPP (i.e. ≥10 drugs), with special reference to the number and type of medical diagnoses and symptoms, in a population of home-dwelling elderly persons aged ≥75 years.
Methods
The study was a cross-sectional analysis of a population-based cohort in 1998. The population consisted of home-dwelling elderly persons aged ≥75 years in the city of Kuopio, Finland. The data for the analysis were obtained from the Kuopio 75+ Study, which drew a random sample of 700 elderly residents aged ≥75 years living in the city of Kuopio from the population register. Of these, 601 attended a structured clinical examination and an interview carried out by a geriatrician and a trained nurse in 1998. For this analysis, all home-dwelling elderly participants (n = 523) were included. Study data were expressed as proportions and means with standard deviations. The factors associated with PP and EPP were examined by multinomial logistic regression.
Results
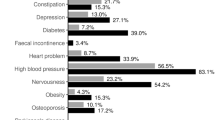
The most commonly used drugs were cardiovascular drugs (97% in EPP, 94% in PP and 59% in non-PP group) and analgesics (89%, 76% and 54%), respectively. Use of psychotropics was markedly higher in the EPP group (77%) than in the PP (42%) and non-PP groups (20%). The mean number of drugs per diagnosis was 3.6 in the EPP group, 2.6 in the PP group and 1.6 in the non-PP group. Factors associated only with EPP were moderate self-reported health (odds ratio [OR] 2.05; 95% CI 1.08, 3.89), female gender (OR 2.43; 95% CI 1.27, 4.65) and age ≥85 years (OR 2.84; 95% CI 1.41, 5.72). Factors that were associated with both PP and EPP included poor self-reported health (PP: OR 2.15; 95% CI 1.01, 4.59 and EPP: OR 6.02; 95% CI 2.55, 14.20), diabetes mellitus (PP: OR 2.28; 95% CI 1.26, 4.15 and EPP: OR 2.07; 95% CI 1.03, 4.18), depression (PP: OR 2.13; 95% CI 1.16, 3.90 and EPP: OR 2.93; 95% CI 1.51, 5.66), pain (PP: OR 2.69; 95% CI 1.68, 4.30 and EPP: OR 2.74; 95% CI 1.56, 4.82), heart disease (PP: OR 2.51; 95% CI 1.54, 4.08 and EPP: OR 4.63; 95% CI 2.45, 8.74) and obstructive pulmonary disease (including asthma or chronic obstructive pulmonary disease) [PP: OR 2.79; 95% CI 1.24, 6.25 and EPP: OR 6.82; 95% CI 2.87, 16.20].
Conclusions
The study indicates that the factors associated with PP and EPP are not uniform. Age ≥85 years, female gender and moderate self-reported health were factors associated only with EPP, while poor self-reported health and several specific disease states were associated with both PP and EPP. The high number of drugs per diagnosis observed in this study calls for a thorough assessment of the need for and outcomes associated with use of these drugs.




Similar content being viewed by others
References
Fulton MM, Allen ER. Polypharmacy in the elderly: a literature review. J Am Acad Nurse Pract 2005; 17: 123–32
Frazier SC. Health outcomes and polypharmacy in elderly individuals: an integrated literature review. J Gerontol Nurs 2005; 31: 4–11
Hajjar ER, Cafiero AC, Hanlon JT. Polypharmacy in elderly patients. Am J Geriatr Pharmacother 2007; 5: 345–51
Klaukka T, Mäkelä M, Sipilä J, et al. Multiuse of medicines in Finland. Med Care 1993; 31: 445–50
Linjakumpu T, Hartikainen S, Klaukka T, et al. Use of medications and polypharmacy are increasing among the elderly. J Clin Epidemiol 2002; 55: 809–17
Jyrkkä J, Vartiainen L, Hartikainen S, et al. Increasing use of medicines in elderly persons: a five-year follow-up of the Kuopio 75+ Study. Eur J Clin Pharmacol 2006; 62: 151–8
Thomas HF, Sweetnam PM, Janchawee B, et al. Polypharmacy among older men in South Wales. Eur J Clin Pharmacol 1999; 55: 411–5
Kennerfalk A, Ruigomez A, Wallander MA, et al. Geriatric drug therapy and healthcare utilization in the United Kingdom. Ann Pharmacother 2002; 36: 797–803
Chen YF, Dewey ME, Avery AJ, et al. Self-reported medication use for older people in England and Wales. J Clin Pharm Ther 2001; 26: 129–40
Veehof L, Stewart R, Haaijer-Ruskamp F, et al. The development of polypharmacy: a longitudinal study. Fam Pract 2000; 17: 261–7
Gurwitz JH, Field TS, Harrold LR, et al. Incidence and preventability of adverse drug events among older persons in the ambulatory setting. JAMA 2003; 289: 1107–16
Green JL, Hawley JN, Rask KJ. Is the number of prescribing physicians an independent risk factor for adverse drug events in an elderly outpatient population? Am J Geriatr Pharmacother 2007; 5: 31–9
Jörgensen T, Johansson S, Kennerfalk A, et al. Prescription drug use, diagnoses, and healthcare utilization among the elderly. Ann Pharmacother 2001; 35: 1004–9
Kuijpers MA, van Marum RJ, Egberts AC, et al. Relationship between polypharmacy and underprescribing. Br J Clin Pharmacol 2008; 65: 130–3
Linton A, Garber M, Fagan NK, et al. Examination of multiple medication use among TRICARE beneficiaries aged 65 years and older. J Manag Care Pharm 2007; 13: 155–62
Nordic Medico-Statistical Committee (NOMESCO). Medicines consumption in the Nordic countries 1999–2003. Copenhagen: NOMESCO, 2004
Hajjar ER, Hanlon JT, Sloane RJ, et al. Unnecessary drug use in frail older people at hospital discharge. J Am Geriatr Soc 2005; 53: 1518–23
Cannon KT, Choi MM, Zuniga MA. Potentially inappropriate medication use in elderly patients receiving home health care: a retrospective data analysis. Am J Geriatr Pharmacother 2006; 4: 134–43
Åstrand B, Åstrand E, Antonov K, et al. Detection of potential drug interactions: a model for a national pharmacy register. Eur J Clin Pharmacol 2006; 62: 749–56
Rosholm JU, Christensen K. Relationship between drug use and self-reported health in elderly Danes. Eur J Clin Pharmacol 1997; 53: 179–83
Barat I, Andreasen F, Damsgaard EM. The consumption of drugs by 75-year-old individuals living in their own homes. Eur J Clin Pharmacol 2000; 56: 501–9
Aparasu RR, Mort JR, Brandt H. Polypharmacy trends in office visits by the elderly in the United States, 1990 and 2000. Res Soc Adm Pharm 2005; 1: 446–59
Haider SI, Johnell K, Thorslund M, et al. Analysis of the association between polypharmacy and socioeconomic position among elderly aged ≥77 years in Sweden. Clin Ther 2008; 30: 419–27
Bjerrum L, Sogaard J, Hallas J, et al. Polypharmacy: correlations with sex, age and drug regimen: a prescription database study. Eur J Clin Pharmacol 1998; 54: 197–202
Barat I, Andreasen F, Damsgaard EM. Drug therapy in the elderly: what doctors believe and patients actually do. Br J Clin Pharmacol 2001; 51: 615–22
Sorensen L, Stokes JA, Purdie DM, et al. Medication management at home: medication-related risk factors associated with poor health outcomes. Age Ageing 2005; 34: 626–32
Alarcon T, Barcena A, Gonzalez-Montalvo JI, et al. Factors predictive of outcome on admission to an acute geriatric ward. Age Ageing 1999; 28: 429–32
Ziere G, Dieleman JP, Hofman A, et al. Polypharmacy and falls in the middle age and elderly population. Br J Clin Pharmacol 2006; 61: 218–23
Field TS, Gurwitz JH, Harrold LR, et al. Risk factors for adverse drug events among older adults in the ambulatory setting. J Am Geriatr Soc 2004; 52: 1349–54
Fialová D, Topinková E, Gambassi G, et al. Potentially inappropriate medication use among elderly home care patients in Europe. JAMA 2005; 293: 1348–58
Haider SI, Johnell K, Thorslund M, et al. Trends in polypharmacy and potential drug-drug interactions across educational groups in elderly patients in Sweden for the period 1992–2002. Int J Clin Pharmacol Ther 2007; 45: 643–53
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Washington, DC: American Psychiatric Association, 1994
Junius-Walker U, Theile G, Hummers-Pradier E. Prevalence and predictors of polypharmacy among older primary care patients in Germany. Fam Pract 2007; 24: 14–9
Jensen E, Schroll M. A 30-year survey of drug use in the 1914 birth cohort in Glostrup County, Denmark: 1964–1994. Aging Clin Exp Res 2008; 20: 145–52
Kuzuya M, Masuda Y, Hirakawa Y, et al. Underuse of medications for chronic diseases in the oldest of community-dwelling older frail Japanese. J Am Geriatr Soc 2006; 54: 598–605
Linjakumpu T, Hartikainen S, Klaukka T, et al. Psychotropics among the home-dwelling elderly: increasing trends. Int J Geriatr Psychiatry 2002; 17: 874–83
Steinman MA, Landefeld CS, Rosenthal GE, et al. Polypharmacy and prescribing quality in older people. J Am Geriatr Soc 2006; 54: 1516–23
Ruiz B, Garcia M, Aguirre U, et al. Factors predicting hospital readmissions related to adverse drug reactions. Eur J Clin Pharmacol 2008; 64: 715–22
Fillit HM, Futterman R, Orland BI, et al. Polypharmacy management in Medicare managed care: changes in prescribing by primary care physicians resulting from a program promoting medication reviews. Am J Manag Care 1999; 5: 587–94
Saltvedt I, Spigset O, Ruths S, et al. Patterns of drug prescription in a geriatric evaluation and management unit as compared with the general medical wards: a randomised study. Eur J Clin Pharmacol 2005; 61: 921–8
Denneboom W, Dautzenberg MG, Grol R, et al. Analysis of polypharmacy in older patients in primary care using a multidisciplinary expert panel. Br J Gen Pract 2006; 56: 504–10
Zarowitz BJ, Stebelsky LA, Muma BK, et al. Reduction of high-risk polypharmacy drug combinations in patients in a managed care setting. Pharmacotherapy 2005; 25: 1636–45
Rajska-Neumann A, Wieczorowska-Tobis K. Polypharmacy and potential inappropriateness of pharmacological treatment among community-dwelling elderly patients. Arch Gerontol Geriatr 2007; 44Suppl. 1: 303–9
Lernfelt B, Samuelsson O, Skoog I, et al. Changes in drug treatment in the elderly between 1971 and 2000. Eur J Clin Pharmacol 2003; 59: 637–44
Klaukka T, Martikainen J, Kalimo E. Drug utilization in Finland 1964–1987. Publications of the social Insurance Institution M:71. Helsinki: Social Insurance Institution, 1990
Jylhä M. Ten-year change in the use of medical drugs among the elderly — a longitudinal study and cohort comparison. J Clin Epidemiol 1994; 47: 69–79
Acknowledgements
The Kuopio 75+ Study was funded by the Nordic Red Feather of the Lions. Subsequent financial support for data analysis was obtained from the Kuopio University Pharmacy Fund and the Social Insurance of Finland. In addition, the study was supported by grants from the Jenny and Antti Wihuri Foundation, and the Orion-Farmos Research Foundation. The funders had no role in the design of the Kuopio 75+ Study or the preparation of this article.
The authors would like to thank the dedicated research staff who collected and saved the data. The authors are also grateful to Ms Päivi Heikura for her role in maintaining and updating the Kuopio 75+ database. In addition, the authors would like to thank statistician Piia Lavikainen for her advice regarding the statistical analysis.
The authors have no conflicts of interest that are directly relevant to the content of this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jyrkkä, J., Enlund, H., Korhonen, M.J. et al. Patterns of Drug Use and Factors Associated with Polypharmacy and Excessive Polypharmacy in Elderly Persons. Drugs Aging 26, 493–503 (2009). https://doi.org/10.2165/00002512-200926060-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00002512-200926060-00006