Abstract
Purpose
The aim of this experimental study is to investigate cardiovascular tolerance of blockade of beta-adrenergic receptors in an endotoxin model.
Design
Prospective, randomized, controlled study.
Setting
Animal laboratory in a university medical center.
Methods
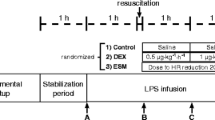
Ten anesthetized, mechanically ventilated pigs were challenged with intravenous lipopolysaccharide (LPS) to achieve a status of profound hypodynamic shock. Systemic and pulmonary hemodynamics and cardiac output were continuously monitored throughout the 5-h study period, and blood samples were taken at baseline (T − 30 min), 1 h from the beginning of LPS infusion (T + 60 min), and every 2 h (T + 180 min and T + 300 min). Animals were randomly assigned to continuous intravenous esmolol infusion titrated to decrease heart rate by 20% or isotonic saline.
Results
Esmolol decreased heart rate by 20%, while in the saline group, heart rate increased by 7% and 22% at T + 180 min and T + 300 min, respectively (p < 0.001). In esmolol-treated animals, cardiac index decreased by 9% at T + 180 min and by 2% at T + 300 min, and in controls by 14% at T + 180 min and by 27% at T + 300 min (p = 0.870). In esmolol-treated animals, median (interquartile range, IQR) stroke index was 31 (6) and 47 (11) ml/min/m2 at T + 180 min and T + 300 min, respectively, and decreased steadily from 45 (20) to 18 (13) ml/min/m2 in controls (p = 0.030). There were no significant differences between groups for any other hemodynamics variables, except for systemic vascular resistance (SVR) (p = 0.017).
Conclusions
In large animals with endotoxemic shock, continuous infusion of esmolol, a selective beta-1 adrenergic blocker, titrated to decrease heart rate by 20%, was well tolerated and may offset LPS-induced cardiac dysfunction by a preload positive effect.


Similar content being viewed by others
References
Annane D, Bellissant E, Cavaillon JM (2005) Septic shock. Lancet 365:63–78
Parrillo JE, Parker MM, Natanson C, Suffredini AF, Danner RL, Cunnion RE, Ognibene FP (1990) Septic shock in humans. Advances in the understanding of pathogenesis, cardiovascular dysfunction, and therapy. Ann Intern Med 113:227–242
Gulick T, Chung MK, Pieper SJ (1989) Interleukin 1 and tumor necrosis factor inhibit cardiac myocyte beta-adrenergic responsiveness. Proc Natl Acad Sci USA 86:6753–6757
Kumar A, Thota V, Dee L, Olson J, Uretz E, Parrillo JE (1996) Tumor necrosis factor alpha and interleukin 1 beta are responsible for in vitro myocardial cell depression induced by human septic shock serum. J Exp Med 183:949–958
Benedict CR, Grahame-Smith DG (1978) Plasma noradrenaline and adrenaline concentrations and dopamine beta hydroxylase activity in patients with shock due to septicemia, trauma, and heamorrhage. Q J Med 185:1–20
Goldstein B, Kempski MH, Stair D, Tipton RB, De King D, De Long DJ, De Asla R, Cox C, Lund N, Woolf PD (1995) Autonomic modulation of heart rate variability during endotoxin shock in rabbits. Crit Care Med 23:1694–1702
Annane D, Trabold F, Sharshar T, Jarrin I, Blanc AS, Raphael JC, Gajdos P (1999) Inappropriate sympathetic activation at onset of septic shock: a spectral analysis approach. Am J Respir Crit Care Med 160:458–465
Mann DL, Bristow MR (2005) Mechanisms and models in heart failure: the biomechanical model and beyond. Circulation 11:2837–2849
Sharshar T, Gray F, Lorin de la Grandmaison G, Hopkinson NS, Ross E, Dorandeu A, Orlikowski D, Raphael JC, Gajdos P, Annane D (2003) Apoptosis of neurons in cardiovascular autonomic centres triggered by inducible nitric oxide synthase after death from septic shock. Lancet 362:1799–1805
Bristow MR, Feldman AM, Adams KF Jr, Goldstein S (2003) Selective versus nonselective beta-blockade for heart failure therapy: are there lessons to be learned from the COMET trial? J Card Fail 9:444–453
de Montmollin E, Aboab J, Mansart A, Annane D (2009) Bench-to-bedside review: beta-adrenergic modulation in sepsis. Crit Care 13:230
Werdan K, Schmidt H, Ebelt H, Zorn-Pauly K, Koidl B, Hoke RS, Heinroth K, Müller-Werdan U (2009) Impaired regulation of cardiac function in sepsis, SIRS, MODS. Can J Physiol Pharmacol 87:266–274
Zaugg M, Schaub MC, Pasch T (2002) Modulation of beta-adrenergic receptor subtype activities in perioperative medicine: mechanisms and sites of action. Br J Anaesth 88:101–123
Mangano DT, Layug EL, Wallace A, Tateo I (1996) Effect of atenolol on mortality and cardiovascular morbidity after non cardiac surgery. N Engl J Med 335:1713–1720
Poldermans D, Boersma E, Bax JJ (1999) The effect of bisoprolol on perioperative mortality and myocardial infarction in high-risk patients undergoing vascular surgery. N Engl J Med 341:1789–1794
Herndon DN, Hart DW, Wolf SE, Chinkes DL, Wolfe RR (2001) Reversal of catabolism by beta-blockade after severe burns. N Engl J Med 345:1223–1229
Gore DC, Wolfe RR (2006) Hemodynamic and metabolic effects of selective beta1 adrenergic blockade during sepsis. Surgery 139:686–694
Suzuki T, Morisaki H, Serita R, Yamamoto M, Kotate Y, Ishizaka A, Takeda J (2005) Infusion of the beta-adrenergic blocker esmolol attenuates myocardial dysfunction in septic rats. Crit Care Med 33:2294–2301
Ackland GL, Yao ST, Rudiger A, Dyson A, Stidwill R, Poputnikov D, Singer M, Gourine AV (2010) Cardioprotection, attenuated systemic inflammation, and survival benefit of beta1-adrenoceptor blockade in severe sepsis in rats. Crit Care Med 38:388–394
Jourdain M, Carrette O, Tournoys A, Fourrier F, Mizon C, Mangalaboyi J, Goudemand J, Mizon J, Chopin C (1997) Effects of inter-alpha-inhibitor in experimental endotoxic shock and disseminated intravascular coagulation. Am J Respir Crit Care Med 156:1825–1833
Fincke R, Hochman JS, Lowe AM, Menon V, Slater JN, Webb JG, Le Jemtel TH, Cotter G, Shock Investigators (2004) Cardiac power is the strongest hemodynamic correlate of mortality in cardiogenic shock: a report from the shock trial registry. J Am Coll Cardiol 44:340–348
Kelley KW, Curtis SE, Marzan GT, Karara HM, Anderson CR (1973) Body surface area of female swine. J Anim Sci 36:927–930
Verbeke G, Molenberghs G (2000) Linear mixed models for longitudinal data. Springer, New York
Kenward MG, Roger JH (1997) Small sample inference for fixed effects from restricted maximum likelihood. Biometrics 53:983–997
Akaike H (1974) A new look at the statistical model identification. IEEE Trans Automat Control AC-19:716–723
Schwarz G (1978) Estimating the dimension of a model. Ann Stat 6:461–464
Schmidt DA, Tumbleson ME (1986) Swine hematology. In: Tumbleson ME (ed) Swine in biomedical research. Plenum, New York, pp 767–782
Volz-Zang C, Eckrich B, Jahn P, Schneidrowski B, Schulte B, Palm D (1994) Esmolol, an ultrashort acting selective beta 1-adrenoreceptor antagonist: pharmacodynamic and pharmacokinetic properties. Eur J Clin Pharmacol 46:399–404
Berk JL, Hagen JF, Beyer WH, Gerber MJ, Dochat GR (1969) The treatment of endotoxin shock by beta adrenergic blockade. Ann Surg 169:74–81
POISE Study Group, Devereaux PJ, Yang H, Yusuf S, Guyatt G, Leslie K, Villar JC, Xavier D, Chrolavicius S, Greenspan L, Pogue J, Pais P, Liu L, Xu S, Málaga G, Avezum A, Chan M, Montori VM, Jacka M, Choi P (2008) Effects of extended-release metoprolol succinate in patients undergoing non-cardiac surgery (POISE trial): a randomised controlled trial. Lancet 371:1839–1847
Acknowledgments
This study was funded by a grant from the Société de Réanimation de Langue Française.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Aboab, J., Sebille, V., Jourdain, M. et al. Effects of esmolol on systemic and pulmonary hemodynamics and on oxygenation in pigs with hypodynamic endotoxin shock. Intensive Care Med 37, 1344–1351 (2011). https://doi.org/10.1007/s00134-011-2236-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-011-2236-y