Abstract
Background
Coronaviruses mainly affect the respiratory system; however, there are reports of SARS-CoV and MERS-CoV causing neurological manifestations. We aimed at discussing the various neurological manifestations of SARS-CoV-2 infection and to estimate the prevalence of each of them.
Methods
We searched the following electronic databases; PubMed, MEDLINE, Scopus, EMBASE, Google Scholar, EBSCO, Web of Science, Cochrane Library, WHO database, and ClinicalTrials.gov. Relevant MeSH terms for COVID-19 and neurological manifestations were used. Randomized controlled trials, non-randomized controlled trials, case-control studies, cohort studies, cross-sectional studies, case series, and case reports were included in the study. To estimate the overall proportion of each neurological manifestations, the study employed meta-analysis of proportions using a random-effects model.
Results
Pooled prevalence of each neurological manifestations are, smell disturbances (35.8%; 95% CI 21.4–50.2), taste disturbances (38.5%; 95%CI 24.0–53.0), myalgia (19.3%; 95% CI 15.1–23.6), headache (14.7%; 95% CI 10.4–18.9), dizziness (6.1%; 95% CI 3.1–9.2), and syncope (1.8%; 95% CI 0.9–4.6). Pooled prevalence of acute cerebrovascular disease was (2.3%; 95%CI 1.0–3.6), of which majority were ischaemic stroke (2.1%; 95% CI 0.9–3.3), followed by haemorrhagic stroke (0.4%; 95% CI 0.2–0.6), and cerebral venous thrombosis (0.3%; 95% CI 0.1–0.6).
Conclusions
Neurological symptoms are common in SARS-CoV-2 infection, and from the large number of cases reported from all over the world daily, the prevalence of neurological features might increase again. Identifying some neurological manifestations like smell and taste disturbances can be used to screen patients with COVID-19 so that early identification and isolation is possible.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Coronaviruses are enveloped, positive-stranded RNA viruses that mainly cause respiratory and gastrointestinal tract infections [1]. They are divided into four genera: alpha, beta, delta, and gamma. Alphacoronavirus and betacoronavirus cause human infections [1]. Betacoronaviruses are further divided into 4 clades, a–d [2]. SARS-CoV and MERS-CoV are betacoronaviruses which caused outbreaks in 2002 and 2012 respectively [3]. The likely reservoirs of SARS-CoV and MERS-CoV viruses were identified as bats [2]. SARS-CoV-2 is a coronavirus and is classified into the betacoronavirus 2b lineage; however, a distinct clade from the SARS-CoV and MERS-CoV [4, 5]. It has been postulated that reservoir of SARS-CoV-2 is also bats; however, more evidence is needed for proving the assumption [6]. The disease caused by SARS-CoV-2 is termed as COVID-19. COVID-19 outbreak started as a cluster of respiratory illnesses and the first case was reported from Wuhan, Hubei Province, China on 8th December [7, 8]. It was declared as a pandemic by WHO on March 11, 2020 [9].
The most common symptoms of COVID-19 are similar to other coronaviruses which include fever, fatigue, dry cough, anorexia, shortness of breath, myalgia, and headache [10,11,12]. Old age and co-morbidities are associated with higher mortality and morbidity as compared with younger patients and those without any co-morbidities [10, 12, 13].
The neuroinvasive and neurotropic potential of coronaviruses like SARS-CoV and MERS-CoV has been demonstrated in many previous studies [14, 15]. A similar mechanism is suggested for the SARS-CoV-2 also [16]. Neurological manifestations reported of SARS-CoV, MERS-CoV, and other coronaviruses include peripheral neuropathy [17], myopathies with elevated creatinine kinase [17], large vessel stroke [18], olfactory neuropathy/anosmia [19], meningoencephalitis [20, 21], post-infectious acute disseminated encephalomyelitis [22, 23], Bickerstaff’s encephalitis overlapping with Guillain-Barré syndrome [24], and Guillain-Barré syndrome [24]. This review is aimed at discussing various neurological manifestations in COVID-19, including the frequency of neurological symptoms, morbidity, mortality, laboratory parameters, and imaging findings associated with patients with neurological symptoms. In the meta-analysis, we estimated the proportion of COVID-19 patients developing neurological manifestations.
Methods
Selection criteria and search strategy
We searched the following electronic databases for articles published between 1st December 2019 to 25th June 2020; PubMed, MEDLINE, Scopus, EMBASE, Google Scholar, EBSCO, Web of Science, Cochrane Library, WHO database, and ClinicalTrials.gov. The MeSH terms and keywords used include: “COVID-19” OR “COVID 19” OR “SARS-CoV-2” OR “2019 novel coronavirus” OR “2019 nCoV” AND “Neurological” OR “Brain” OR “CNS features” OR “central nervous system features” OR “peripheral nervous system features” OR “neuropathy” OR “skeletal muscle” OR “myositis” OR “neuromuscular junction” OR “headache” OR “anosmia” OR “olfactory” OR “ageusia” OR “cranial neuropathy” OR “seizures” OR “encephalitis” OR “meningitis” OR “stroke” OR “cerebrovascular disease” OR “cerebral hemorrhage” OR “intracerebral hemorrhage” OR “cerebral infarct” OR “cortical venous thrombosis” OR “deep cerebral venous thrombosis” OR “impaired consciousness” OR “confusion” OR “weakness” OR “Guillain-Barre’ syndrome” OR “Miller Fisher syndrome” OR “ataxia” OR “myopathy” OR “myelitis” OR “myelopathy” with an additional filter of “studies in human subjects”. The search was done between 31st March 2020 and 25th June 2020. To ensure literature saturation, we inspected the references of all studies included in this review. The protocol of this review was registered at PROSPERO (ID-CRD42020185593) prospectively in May 2020.
Inclusion and exclusion criteria
All published randomized controlled trials, non-randomized controlled trials, case-control studies, cohort studies, cross-sectional studies, case series, and case reports, if they had sufficient data on neurological features, laboratory parameters, imaging findings were included in this review. Only those studies were included in which subjects were diagnosed with SARS-CoV-2 infection by real-time RT-PCR or high throughput sequencing analysis of swab specimens or serology or culture. We also included pre-prints and letters if they included data on neurological manifestations in COVID-19. Editorials, systematic reviews, meta-analysis, narrative reviews, conference abstracts, commentaries, animal studies, post-mortem studies, and where translation into English was not possible were excluded. The authors were contacted twice by email if any missing data in the articles.
Data extraction and study quality assessment
Databases selected were searched independently by two members (TF and AP) in the team, and, following duplicate removal, reviewed all the articles and selected articles based on inclusion and exclusion criteria. Reporting was done according to the recommendations of the PRISMA statement [25]. Quality of the non-randomized studies was evaluated using the Newcastle-Ottawa Scale [26, 27] and the quality of one randomized controlled trial was assessed using the CONSORT criteria [28]. Any disagreements between two main reviewers were discussed with a third evaluator. Data about the author’s name, publication date, study setting and design, time and duration of the study, follow-up, the total number of patients evaluated, study population, age, gender, co-morbidities, neurological features, laboratory parameters, imaging findings, morbidity, and mortality were extracted.
Outcome measures
Primary outcomes assessed were neurological manifestations in COVID-19 patients and its prevalence. For the categorical variables, simple and relative frequency and proportions were used. For continuous variables, central tendency (mean or median) and dispersion measures (standard error, standard deviation) were used. To measure association, risk ratios, odds ratios, and hazard ratios were used and 95% confidence intervals calculated. We also assessed secondary outcomes like the association of neurological manifestations with age, co-morbidities, lab parameters including CSF study, imaging features, length of hospital stay, ICU admission, time from onset of typical COVID-19 symptoms to neurological manifestations, and morbidity/mortality.
Strategy for data synthesis, statistical analysis for meta-analysis
Data synthesis and illustration were done in tables and figures. For the categorical variables, simple and relative frequency and proportions were used. For continuous variables, measures of central tendency (mean or median) and dispersion (standard error, standard deviation) were calculated. The primary aim of our study was to synthesize the findings from multiple studies that investigated the issues related to neurological manifestations in COVID-19 and thus provide a quantitative summary, to better direct future work. The data are available in the form of proportions, defined as the number of cases of interest in a sample with a particular characteristic divided by the size of the sample. To achieve the objective of obtaining a more precise estimate of the overall proportion for a certain event (neurological manifestations) related to COVID-19, the study employed meta-analysis of proportions using a random-effects model and by the DerSimonian-Laird method [29, 30]. We performed data analysis using meta-packages in R (version 3.5.0). Heterogeneity was assessed using the I2 value. I2 can take values from 0% to 100% and it is assumed that an I2 of 25%, 50%, and 75% indicate low, medium, and large heterogeneity respectively [31]. Forest plot was used to visualize the point estimates of study effects and their confidence intervals. Publication bias was evaluated using the funnel plot.
Results
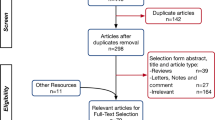
Among the 6789 articles identified, 212 studies were included in the systematic review and 74 studies in the meta-analysis (PRISMA flow diagram (Fig. 1)). Out of them, most were retrospective studies, 18 were cohort studies, 11 were prospective studies, nine were cross-sectional studies, one was a randomized controlled trial, one was a case-control study and the rest were all case series and case reports. Among these studies, we found only 19 studies, which investigated specifically neurological features in COVID-19 patients. Other studies, evaluated parameters in general. Table 1 shows a summary of all the observational studies included.
Neurological manifestations
Neurological manifestations have been reported in patients with COVID-19 from all over the world. A multicentre, retrospective study by Mao et al. [32] was the first study to evaluate the neurological manifestations in COVID-19 and found that neurological manifestations were present in 36.4% of total 214 patients, out of which most common was CNS manifestations(24.8%) followed by peripheral nervous system manifestations(8.9%). Other large retrospective observational studies reported the incidence of neurological manifestations as 4.3% [45], 15% [47], and 57.4% [49]. The most common neurological manifestations reported in COVID-19 were smell disturbances, taste disturbances, headache, myalgia, and disturbances in consciousness/altered mental status. The prevalence of all the neurological manifestations assessed is given in Table 2. A summary estimate of pooled prevalence and heterogeneity of each neurological manifestation are given in Table 3. Forest plot and funnel plot is given in Figs. 2 and 3 respectively.
Smell and taste disturbances
The overall incidence of smell disturbances in the studies ranged from 4.9–85.6% [49, 54] and the most common type of smell disturbance was anosmia. Other smell disturbances noticed were hyposmia, phantosmia, and parosmia [54]. Similarly, the incidence of taste disturbances reported was 0.3–88.8% [47, 54] and the most commonly reported were dysgeusia and ageusia. In the meta-analysis, we found 17 and 14 studies, which assessed the prevalence of smell and taste disturbances respectively and disturbances of smell (35.8%; 95%CI 21.4–50.2) and taste (38.5%; 95%CI 24.0–53.0) sensation were the most common neurological manifestation followed by non-specific neurological manifestations.
A case-control study of 79 COVID-19 patients and 40 historical controls of influenza patients from Spain [52] revealed that new-onset smell and taste disorders were significantly higher in the COVID-19 group. Patients in COVID-19 were significantly younger. Another study reported olfactory and taste disturbances occur more frequently in females than males [53]. Lechien et al. [54], Gilani S et al. [140], and Rachel Kaye et al. [141] reported that anosmia can be the initial and early manifestations of COVID-19. Population surveys on new-onset olfactory dysfunction from Iran [142] and UK [143] have reported an increase in olfactory dysfunction during the COVID-19 pandemic.
Non-specific symptoms
The most common non-specific neurological symptoms reported in SARS-CoV-2 infection were myalgia, headache syncope, and dizziness. The overall pooled prevalence estimate of the proportion of cases are given in Table 3. Incidence of myalgia reported in various studies ranged from 1.8–62.5% [47, 111], headache from 0.6–70.3% [90, 111], and dizziness from 0.6–21% [47, 113]. In children, myalgia and dizziness were less common and rarely reported. In health care workers, the incidence of myalgia, headache, and dizziness was higher compared with the general population. Syncope was reported in three studies with incidence of 0.3% [45], 0.6% [49], and 4.8% [86]. Few studies showed an increase in creatine kinase, LDH, and myoglobin in COVID-19 patients [12, 62, 66].
Acute cerebrovascular disease
Acute cerebrovascular disease (CVD) was reported in 0.5–5.9% [33, 48] of COVID-19 patients. Out of them, the most common type was acute ischaemic stroke and severe COVID-19 patients were more at risk of developing the acute CVD [33]. From these studies, the incidence of acute CVD in severe/ICU patients reported were 0.8–9.8% [33, 41]. The incidence of ischaemic stroke, hemorrhagic stroke, and cerebral venous thrombosis reported from various studies ranged from 0.4–4.9% [33, 48], 0.2–0.9% [38, 48], and 0.3–0.5% [33, 47] respectively. A study by Mao et al. [32] reported that two patients presented with hemiplegia without any typical COVID-19 symptoms. The median time to onset of cerebrovascular disease was 9 days. Another study by Li Y et.al [33] showed that acute CVD was more likely to be present with severe COVID-19; however, they were older, and had cardiovascular risk factors. These findings were similar to the above study by Mao et al. [32]. In both these studies, the laboratory parameters in patients with CNS symptoms were different from the other COVID-19 patients, with a higher white cell and neutrophil counts, reduced lymphocyte and platelet counts, elevated CRP and D-dimer levels [32, 33].
We found two studies that specifically studied the thrombotic complications in COVID-19 patients and found acute ischaemic stroke in COVID-19 patients receiving thromboprophylaxis [35, 36]. A retrospective observational case series in COVID-19 patients from Italy [144] reported six cases of stroke, four were ischaemic and two were hemorrhagic. Five of them had pre-existing vascular risk factors. Three patients with ischaemic stroke and one patient with hemorrhagic stroke showed hypercoagulable blood parameters [144]. Two studies reported six cases of stroke in young(< 50 years) COVID-19 patients, out of which three patients did not have any risk factors [145, 146]. Also there are multiple case reports and case series of ischaemic stroke including large artery [147], aneurysmal [148, 149] and non-aneurysmal SAH [51], deep cerebral venous thrombosis [150,151,152,153,154,155,156,157], hemorrhagic stroke [38, 158, 159] and CNS vasculitis [160] from all over the world in COVID-19 patients [38, 51, 147,148,149,150,151,152,153,154,155,156,157,158,159,160,161,162,163,164,165,166,167,168,169,170,171,172,173].
Meningoencephalitis, encephalopathy, disturbances in consciousness
Several cases of meningoencephalitis and encephalopathy were reported in COVID-19 patients [39, 43, 49, 174,175,176,177,178,179,180,181,182,183]. The incidence of encephalitis reported in two retrospective studies was 0.03% [43] and 0.1% [49]. Only in four of the 15 reported cases of encephalitis, CSF RT-PCR test was positive for SARS-CoV-2 RNA, and surprisingly two cases among them had negative nasopharyngeal swab [50, 174,175,176]. Two reports showed elevated levels of cytokines like IL-6, IL-8, TNF-α, β2-microglobulin, IP-10, MCP-1 in CSF [177, 181]. Interestingly, fluid from the surgical evacuation of subdural hematoma was positive for SARS-CoV-2 RT-PCR in a COVID-19 patient [184]. Isolated meningoencephalitis without any respiratory involvement has also been reported [175, 185]. Another case of rhombencephalitis as a rare complication of COVID-19 patient has been reported [186]. Few retrospective studies [32, 47, 49] reported seizures with the incidence ranging from 0.5–1.4% [32, 47]. Cases of all types of seizures like febrile seizures [42], focal seizures [180, 187,188,189], generalized tonic-clonic seizures [183, 190,191,192], myoclonic status epilepticus [193], status epilepticus [188, 194] and non-convulsive status epilepticus [46] were reported in COVID-19 patients.
Generally, the SARS-CoV-2 virus causes mild disease in children. However, a study from Italy showed a total five patients with seizures, and out of them, two had febrile seizures (three children had a known history of epilepsy, one child had a history of febrile seizures, one child had a first episode of febrile seizures) [42]. Also, a case of a 6-week-old infant with SARS-CoV-2 in addition to rhinovirus, presenting with brief 10–15-s episodes of upward gaze and bilateral leg stiffening was reported with normal EEG and MRI brain [195]. Another case of an 11-year-old child with COVID-19 viral encephalitis has been reported, with CSF showing viral encephalitis picture [194].
PRES syndrome has also been reported in studies [47, 51]. Transient cortical blindness like presentation of PRES syndrome with MRI brain at admission revealing bilateral T2/FLAIR hyperintensities, especially left occipital, frontal cortical white matter and splenium of the corpus callosum and diffusion restriction in DWI revealing vasogenic edema has been reported [196]. Repeat MRI after 2 weeks showed a complete resolution of findings. Cases of acute necrotizing hemorrhagic encephalopathy [191, 197], hypoxic brain injury with encephalopathy [43, 47, 51, 65], delayed post-hypoxic leukoencephalopathy [198], mild encephalitis/encephalopathy with a reversible splenial lesion(MERS) [199], ADEM in elderly females [200, 201], MS plaque exacerbation [47] and CIS [176] were reported in SARS-CoV-2 infected patients.
Incidence of disturbances of consciousness/delirium ranged from 3.3–19.6% [49, 100] in retrospective studies. S.R. Beach, et al. [202] reported four cases of elderly COVID-19 patients, who presented to the hospital with altered mental status without any respiratory complaints, and only one among them developed respiratory complaints during the hospital stay. Similar cases have been reported in elderly patients from Saudi Arabia [203], Norway [204] and China [205]. An observational case series from France [39] in 58 COVID-19 patients with ARDS admitted in ICU reported agitation in 40(69%) patients, confusion in 26 of 40 patients, diffuse corticospinal tract signs in 39 patients (67%) and out of the 45 patients discharged, 15(33%) had a dysexecutive syndrome. MRI Brain showed enhancement of leptomeningeal spaces in eight patients, bilateral frontotemporal hypoperfusion in 11 patients who underwent perfusion imaging, two asymptomatic patients with small acute ischaemic stroke and one patient with subacute ischaemic stroke.
Guillain-Barré syndrome
There are multiple reports of GBS in patients with confirmed COVID-19. GBS has also been reported to be a presenting feature in one case report by Zhao H et al. [206] where the patient, later on, developed fever and other symptoms of COVID-19. All the variants of GBS like AIDP, AMAN, AMSAN has been reported in COVID-19 patients [47, 206,207,208,209,210,211,212,213,214,215,216,217,218,219] including both para [206,207,208,209,210,211,212, 220,221,222,223] and post-infectious pattern [210, 211, 214,215,216,217,218,219, 224,225,226]. Toscano et al. [227] reported a series of five patients of COVID-19 with GBS, with the interval between the onset of fever, cough and symptoms of GBS ranging from 5 to 10 days. Cases of MFS were also reported [47, 226, 228, 229]. One case of MFS was associated with a positive serum GD1b-IgG antibody [228]. Other rare variants reported were GBS/MF overlap syndrome [219], AMSAN variants with severe autonomic neuropathy [219], facial diplegia [222, 227] and post-infectious pattern of the demyelinating type of GBS with brainstem and cervical leptomeningeal enhancement [225]. Cranial neuropathies with abnormal perineural or cranial nerve findings [230], multiple cranial neuropathies [211, 219], peripheral motor neuropathy [231] and ataxia [32, 43, 51] are all reported as presentations of COVID-19.
Other neurological manifestations
The incidence of rhabdomyolysis has been reported between 0.2–2.6% in different studies [11, 49, 139]. A report illustrates a 38 year-old COVID-19 patient presenting with fever, dyspnea, and severe myalgia, with high creatine kinase (>42,670 U/L) and LDH (4301 U/La) and was diagnosed as viral myositis [232]. Another two cases of adult COVID-19 patients with lower extremity pain and weakness with rhabdomyolysis with high creatine kinase and LDH were reported [233, 234]. First case developed rhabdomyolysis on the 9th day of admission [233] and 2nd case presented to the hospital with rhabdomyolysis [234]. An isolated case of post-infectious myelitis has been reported from Germany in a COVID-19 patient [235].
Three cases of generalized brainstem type of myoclonus were reported from Spain, with normal CSF study in one patient (others not done) and normal imaging findings. However, nasopharyngeal RT-PCR for SARS-CoV-2 was positive in only one patient. In all these patients, EEG was showing mild diffuse slowing without any epileptic activity [236]. Paresthesias [51] and cutaneous hyperaesthesia [237] were reported as a presentation in COVID-19 patients. A case of COVID-19 patient with oropharyngeal dysphagia followed by aspiration pneumonia, taste impairment, impaired pharyngolaryngeal sensation, and nasopharyngeal contractile dysfunction with absent gag reflex was reported from Japan [238]. Visual symptoms were also reported in a few studies. Mao L et al. [32] reported visual impairment in 1.4% of the COVID-19 patients. Cases of optic neuritis [49], isolated central retinal artery occlusion [239], non-arteritic type of posterior ischaemic optic neuropathy (PION) [240] as a COVID-19 manifestation were also reported. The summary of all the neurological manifestations reported in COVID-19 is given in Table 4.
Heterogeneity
The heterogeneity was high in most of the neurological manifestations studied except for hemorrhagic stroke (medium), cerebral venous thrombosis (low), seizure (low), and ataxia (low). The funnel plots were symmetric in hemorrhagic stroke, ataxia, seizures, cerebral venous thrombosis and myalgia, which is pointing towards no bias in the selection of publications that are included in the study. However, the funnel plots were asymmetric in other neurological manifestations studied, which pointed towards the heterogeneity in the studies undertaken or bias in the selection of publications included in the study.
Discussion
In this systematic review and meta-analysis, we assessed the neurological manifestations, risk factors, mortality, laboratory parameters, and imaging findings in those patients with neurological features. Involving 30,159 patients, our meta-analysis is the first and most comprehensive study about the neurological manifestations of COVID-19.
The most common neurological manifestations reported were smell and taste disturbances. Another interesting finding is the geographical variations in the frequency of smell and taste disturbances. High incidence of smell and taste disturbances were noted in studies from most of the European countries [54] while studies from Asian countries showed a lower incidence [32]. However, most of the studies which reported a higher incidence of smell and taste disturbances evaluated mainly olfactory and taste symptoms only and studied mild to moderate cases and excluded severe/ICU patients compared with studies with lower incidence. This bias might have caused under-reporting of smell and taste disturbances in severe/ICU patients or could also be because of decreased awareness of investigator about these symptoms at the beginning of the pandemic. Supporting our assumption, a study from Spain which evaluated 841 COVID-19 patients with neurological manifestations reported only 4.9% of cases of smell disturbances and 6.2% cases of taste disturbances [49]. Other possibilities for these variations are, the difference in affinity of SARS-CoV-2 to tissues between populations, a different strain of mutated virus circulating in Europe compared with Asian countries. However, more studies are required to confirm these assumptions. Interestingly a study by Wan Y et al. [241] predicted that binding affinity between 2019-nCoV and human ACE2 may be enhanced by a single N501T mutation. Also, ACE2 receptors are highly expressed by sustentacular cells of the olfactory epithelium. Olfactory and taste disorders were more common in younger patients [52, 140] most occurs in the early stages as initial manifestations of the disease and even as the only manifestation of COVID-19. Hence, olfactory and gustatory disorders can be the initial and early manifestations of COVID-19 and early identification of these symptoms might lead to early diagnosis and disease containment.
Non-specific neurological manifestations could be just systemic features of a viral infection. Similar to olfactory disturbances, the incidence of myalgia, headache, and dizziness also shows geographical variations with the highest incidence reported from Europe, the USA, and Chile. The incidence of non-specific symptoms was lower in children. We noticed that non-specific symptoms were higher among the studies conducted in health care workers. This may be due to increased knowledge and awareness of the symptoms and disease.
The most common type of acute CVD reported was an ischaemic stroke. Hemorrhagic stroke, deep cerebral venous thrombosis, SAH (both non-aneurysmal and aneurysmal), and TIA were also reported; however, with much lesser prevalence. Severe infection or ICU requirement, older age, cardiovascular risk factors, prior co-morbidities, and hypercoagulable lab parameters were found to be a risk factor for developing acute CVD [32, 33]. The apparent association of COVID-19 and stroke is likely due to the sharing of similar risk factors. The severity of COVID-19 has been proved to be directly related to the presence of co-morbidities like hypertension and DM. An earlier meta-analysis by Yang J et al. [242] comprising [46, 243] COVID-19 patients reported the prevalence of risk factors, hypertension in 21.1%, DM in 9.7%, and cardiovascular diseases in 8.4%. Also, hypercoagulable blood parameters as shown by Li Y et.al [33], can lead to ischaemic stroke and cerebral venous thrombosis. Nervous system involvement in SARS-CoV-2 infection can be due to direct invasion of neural tissues, inflammatory response, or immune dysregulation. The SARS-CoV-2 virus uses the ACE2 and TMPRSS2 for entry to the host cell and it is one of the main determinants of infectivity [241, 244]. Susceptibility to infection correlated with ACE2 expression in previous studies [245].
Very few retrospective studies showed meningoencephalitis as a presentation of COVID-19; however, there are multiple case reports from all over the world. The probable mechanism can again be direct invasion via the hematogenous route or retrograde pathway via peripheral nerve terminals. Two studies even showed higher levels of inflammatory cytokines in the CSF analysis of these patients [177, 181]. SARS-CoV-2 could trigger a seizure in predisposing patients through neurotropic mechanisms as explained earlier [188]. However, more evaluation is required in this field to find a temporal factor. All types of seizures were reported like febrile seizures, focal seizures, generalized tonic-clonic seizures, status epilepticus and myoclonic status epilepticus, NCSE and also brainstem type of myoclonus. Demyelinating disorders like ADEM, exacerbation of MS plaque, and the clinically isolated syndrome were all reported in COVID-19 patients.
Cases of GBS and its variants were also reported in COVID-19. Both post-infectious and pre-infectious pattern of GBS were reported. The most common type of GBS reported was AIDP. Other variants like AMAN, AMSAN, Miller Fisher syndrome, and facial diplegic variant were also reported. Patients presenting as GBS without any other typical symptoms of COVID-19 were also reported. Possible pathogenesis of GBS in COVID-19 includes immune dysregulation secondary to systemic hyper inflammation and cytokines produced as described by McGonagle et al. [246] and Quin et al. [247]. Hence, it is important to suspect and test for COVID-19 in those patients presenting with GBS and MFS. However, more studies are required to conclude that these cases were not just coincidental and COVID-19 itself is a trigger for GBS and MFS. GBS was also reported in other recent important viral infections like MERS-CoV [248] and Zika virus [243].
Change in laboratory parameters was also reported in COVID-19 patients with neurological manifestations like higher white cell and neutrophil counts, reduced lymphocyte and platelet counts, elevated CRP and D-dimer levels, and higher levels of creatine kinase, LDH, and myoglobin [12, 32, 33, 62].
High heterogeneity in our study could be because of differences in the selection of patients and ethnicity, the severity of the disease, co-morbidities, only a few studies evaluated neurological symptoms specifically, variation in the number of patients in different studies, or due to publication bias and differences in the methodology among the studies.
Comparison with previous systematic reviews
Earlier meta-analyses addressing general clinical features in COVID-19 were published. One such study showed myalgia in (28.5%; 95%CI 21.2–36.2), headache (14.0%; 95%CI 9.9–18.6), and dizziness (7.6%; 95%CI 0.0–23.5) [249]. Our results also found similar results for myalgia, headache, and dizziness, i.e. (19.3%; 95%CI 15.1–23.6), (14.7%; 95%CI 10.4–18.9), and (6.1%; 95%CI 3.1–9.2) respectively. Another similar meta-analysis also showed myalgia in (21.9%; 95%CI 17.7–26.4) and headache in (11.3%; 95%CI 8.9–14.0) [250]. One more study reported the prevalence of headache as (8.0%; 95%CI 5.7–10.2) [251]. However, no meta-analyses are published on the specific neurological manifestations till now.
Strengths and limitations
The strength of our study is that we did a comprehensive search in all the electronic databases. Study limitations include high heterogeneity in the estimation of the prevalence of some neurological manifestations, the inclusion of studies with very small sample size, and lack of meta-regression analysis. We excluded studies in languages other than English where translation was not possible. Most of the included studies were of moderate quality. More good- quality prospective cohort studies are required to establish that the neurological manifestations reported in the studies were not just coincidental.
Conclusions
In conclusion, our study showed neurological manifestations are common in COVID-19 and are even present as the only symptom without any other manifestation of the respiratory system involvement. Hence it is important to suspect every COVID-19 patient with neurological manifestations. In this pandemic, a neurologist needs to take necessary precautions while examining the patients presenting to them. Also, some symptoms like smell and taste disturbance can be used as a screening tool for SARS-CoV-2 infection and can help isolate suspected patients earlier to avoid the spread of the disease.
Data availability
All data available on request.
References
de Wilde AH, Snijder EJ, Kikkert M, van Hemert MJ (2018) Host factors in coronavirus replication. Curr Top Microbiol Immunol 419:1–42. https://doi.org/10.1007/82_2017_25
Drexler JF, Corman VM, Drosten C (2014) Ecology, evolution and classification of bat coronaviruses in the aftermath of SARS. Antivir Res 101:45–56. https://doi.org/10.1016/j.antiviral.2013.10.013
de Wit E, van Doremalen N, Falzarano D, Munster VJ (2016) SARS and MERS: recent insights into emerging coronaviruses. Nat Rev Microbiol 14(8):523–534. https://doi.org/10.1038/nrmicro.2016.81
Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, Zhao X, Huang B, Shi W, Lu R, Niu P, Zhan F, Ma X, Wang D, Xu W, Wu G, Gao GF, Tan W, China Novel Coronavirus Investigating and Research Team (2020) A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med 382(8):727–733. https://doi.org/10.1056/NEJMoa2001017
Letko M, Marzi A, Munster V (2020) Functional assessment of cell entry and receptor usage for SARS-CoV-2 and other lineage B betacoronaviruses. Nat Microbiol 5(4):562–569. https://doi.org/10.1038/s41564-020-0688-y
Zhou P, Yang X-L, Wang X-G, Hu B, Zhang L, Zhang W, Si HR, Zhu Y, Li B, Huang CL, Chen HD, Chen J, Luo Y, Guo H, Jiang RD, Liu MQ, Chen Y, Shen XR, Wang X, Zheng XS, Zhao K, Chen QJ, Deng F, Liu LL, Yan B, Zhan FX, Wang YY, Xiao GF, Shi ZL (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 579(7798):270–273. https://doi.org/10.1038/s41586-020-2012-7
Novel Coronavirus – China. World Health Organization. https://www.who.int/csr/don/12-january-2020-novel-coronavirus-china/en/. Published January 12, 2020. Accessed June 19, 2020
Chen X, Yu B (2020) First two months of the 2019 coronavirus disease (COVID-19) epidemic in China: real-time surveillance and evaluation with a second derivative model. Glob Health Res Policy 5(1):7. https://doi.org/10.1186/s41256-020-00137-4
Coronavirus Disease (COVID-19) - events as they happen. World Health Organization. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen. Published January 12, 2020. Accessed June 19, 2020
Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, Wang B, Xiang H, Cheng Z, Xiong Y, Zhao Y, Li Y, Wang X, Peng Z (2020) Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus–infected pneumonia in Wuhan, China. JAMA 323(11):1061–1069. https://doi.org/10.1001/jama.2020.1585
Guan W, Ni Z, Hu Y, Liang WH, Ou CQ, He JX, Liu L, Shan H, Lei CL, Hui DSC, du B, Li LJ, Zeng G, Yuen KY, Chen RC, Tang CL, Wang T, Chen PY, Xiang J, Li SY, Wang JL, Liang ZJ, Peng YX, Wei L, Liu Y, Hu YH, Peng P, Wang JM, Liu JY, Chen Z, Li G, Zheng ZJ, Qiu SQ, Luo J, Ye CJ, Zhu SY, Zhong NS, China Medical Treatment Expert Group for Covid-19 (2020) Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 382(18):1708–1720. https://doi.org/10.1056/NEJMoa2002032
Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, Qiu Y, Wang J, Liu Y, Wei Y, Xia J’, Yu T, Zhang X, Zhang L (2020) Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet 395(10223):507–513. https://doi.org/10.1016/S0140-6736(20)30211-7
Wu C, Chen X, Cai Y, Xia J’, Zhou X, Xu S, Huang H, Zhang L, Zhou X, du C, Zhang Y, Song J, Wang S, Chao Y, Yang Z, Xu J, Zhou X, Chen D, Xiong W, Xu L, Zhou F, Jiang J, Bai C, Zheng J, Song Y (2020) Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med 180(7):934–943. https://doi.org/10.1001/jamainternmed.2020.0994
Netland J, Meyerholz DK, Moore S, Cassell M, Perlman S (2008) Severe acute respiratory syndrome coronavirus infection causes neuronal death in the absence of encephalitis in mice transgenic for human ACE2. J Virol 82(15):7264–7275. https://doi.org/10.1128/JVI.00737-08
Li K, Wohlford-Lenane C, Perlman S, Zhao J, Jewell AK, Reznikov LR, Gibson-Corley KN, Meyerholz DK, McCray PB Jr (2016) Middle East respiratory syndrome coronavirus causes multiple organ damage and lethal disease in mice transgenic for human dipeptidyl peptidase 4. J Infect Dis 213(5):712–722. https://doi.org/10.1093/infdis/jiv499
Baig AM, Khaleeq A, Ali U, Syeda H (2020) Evidence of the COVID-19 virus targeting the CNS: tissue distribution, host–virus interaction, and proposed neurotropic mechanisms. ACS Chem Neurosci 11(7):995–998. https://doi.org/10.1021/acschemneuro.0c00122
Tsai L, Hsieh S, Chao C et al (2004) Neuromuscular disorders in severe acute respiratory syndrome. Arch Neurol 61(11):1669–1673. https://doi.org/10.1001/archneur.61.11.1669
Umapathi T, Kor AC, Venketasubramanian N, Lim CCT, Pang BC, Yeo TT, Lee CC, Lim PL, Ponnudurai K, Chuah KL, Tan PH, Tai DYH, Ang SPB (2004) Large artery ischaemic stroke in severe acute respiratory syndrome (SARS). J Neurol 251(10):1227–1231. https://doi.org/10.1007/s00415-004-0519-8
Hwang CS (2006) Olfactory neuropathy in severe acute respiratory syndrome: report of a case. Acta Neurol Taiwanica 15(1):26–28
Li Y, Li H, Fan R, Wen B, Zhang J, Cao X, Wang C, Song Z, Li S, Li X, Lv X, Qu X, Huang R, Liu W (2016) Coronavirus infections in the central nervous system and respiratory tract show distinct features in hospitalized children. Intervirology. 59(3):163–169. https://doi.org/10.1159/000453066
Morfopoulou S, Brown JR, Davies EG, Anderson G, Virasami A, Qasim W, Chong WK, Hubank M, Plagnol V, Desforges M, Jacques TS, Talbot PJ, Breuer J (2016) Human coronavirus OC43 associated with fatal encephalitis. N Engl J Med 375(5):497–498. https://doi.org/10.1056/NEJMc1509458
Arabi YM, Harthi A, Hussein J, Bouchama A, Johani S, Hajeer AH, Saeed BT, Wahbi A, Saedy A, AlDabbagh T, Okaili R, Sadat M, Balkhy H (2015) Severe neurologic syndrome associated with Middle East respiratory syndrome corona virus (MERS-CoV). Infection. 43(4):495–501. https://doi.org/10.1007/s15010-015-0720-y
Ann Yeh E, Collins A, Cohen ME, Duffner PK, Faden H (2004) Detection of coronavirus in the central nervous system of a child with acute disseminated encephalomyelitis. PEDIATRICS. 113(1):e73–e76. https://doi.org/10.1542/peds.113.1.e73
Kim J-E, Heo J-H, Kim H, Song SH, Park SS, Park TH, Ahn JY, Kim MK, Choi JP (2017) Neurological complications during treatment of Middle East Respiratory Syndrome. J Clin Neurol 13(3):227–233. https://doi.org/10.3988/jcn.2017.13.3.227
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605. https://doi.org/10.1007/s10654-010-9491-z
Wells GA, Shea B, O'Connell D, et al. The Ottawa Hospital Research Institute. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Published October 19, 2009. Accessed June 19, 2020
Schulz KF, Altman DG, Moher D, for the CONSORT Group (2010) CONSORT 2010 Statement: updated guidelines for reporting parallel group randomised trials. BMJ 340(mar23 1):c332–c332. https://doi.org/10.1136/bmj.c332
Viechtbauer W. Conducting meta-analyses in R with the metafor Package. J Stat Softw. 2010;36(3). https://doi.org/10.18637/jss.v036.i03
Kontopantelis E, Reeves D (2012) Performance of statistical methods for meta-analysis when true study effects are non-normally distributed: a comparison between DerSimonian–Laird and restricted maximum likelihood. Stat Methods Med Res 21(6):657–659. https://doi.org/10.1177/0962280211413451
Higgins JPT (2003) Measuring inconsistency in meta-analyses. BMJ. 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Mao L, Jin H, Wang M, Hu Y, Chen S, He Q, Chang J, Hong C, Zhou Y, Wang D, Miao X, Li Y, Hu B (2020) Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol 77(6):683–690. https://doi.org/10.1001/jamaneurol.2020.1127
Li Y, Li M, Wang M, et al. Acute cerebrovascular disease following COVID-19: a single center, retrospective, observational study. Stroke Vasc Neurol. Published online July 2, 2020:svn-2020-000431. https://doi.org/10.1136/svn-2020-000431
Lu L, Xiong W, Liu D, Liu J, Yang D, Li N, Mu J, Guo J, Li W, Wang G, Gao H, Zhang Y, Lin M, Chen L, Shen S, Zhang H, Sander JW, Luo J, Chen S, Zhou D (2020) New onset acute symptomatic seizure and risk factors in coronavirus disease 2019: a retrospective multicenter study. Epilepsia. 61(6):e49–e53. https://doi.org/10.1111/epi.16524
Klok FA, Kruip MJHA, van der Meer NJM, Arbous MS, Gommers D, Kant KM, Kaptein FHJ, van Paassen J, Stals MAM, Huisman MV, Endeman H (2020) Confirmation of the high cumulative incidence of thrombotic complications in critically ill ICU patients with COVID-19: An updated analysis. Thromb Res 191:148–150. https://doi.org/10.1016/j.thromres.2020.04.041
Lodigiani C, Iapichino G, Carenzo L, Cecconi M, Ferrazzi P, Sebastian T, Kucher N, Studt JD, Sacco C, Alexia B, Sandri MT, Barco S, Humanitas COVID-19 Task Force (2020) Venous and arterial thromboembolic complications in COVID-19 patients admitted to an academic hospital in Milan, Italy. Thromb Res 191:9–14. https://doi.org/10.1016/j.thromres.2020.04.024
Fraissé M, Logre E, Pajot O, Mentec H, Plantefève G, Contou D (2020) Thrombotic and hemorrhagic events in critically ill COVID-19 patients: a French monocenter retrospective study. Crit Care 24(1):275. https://doi.org/10.1186/s13054-020-03025-y
Dogra S, Jain R, Cao M, Bilaloglu S, Zagzag D, Hochman S, Lewis A, Melmed K, Hochman K, Horwitz L, Galetta S, Berger J (2020) Hemorrhagic stroke and anticoagulation in COVID-19. J Stroke Cerebrovasc Dis 29(8):104984. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104984
Helms J, Kremer S, Merdji H, Clere-Jehl R, Schenck M, Kummerlen C, Collange O, Boulay C, Fafi-Kremer S, Ohana M, Anheim M, Meziani F (2020) Neurologic features in severe SARS-CoV-2 infection. N Engl J Med 382(23):2268–2270. https://doi.org/10.1056/NEJMc2008597
Helms J, Tacquard C, Severac F et al (2020) High risk of thrombosis in patients with severe SARS-CoV-2 infection: a multicenter prospective cohort study. Intensive Care Med 46(6):1089–1098. https://doi.org/10.1007/s00134-020-06062-x
Kandemirli SG, Dogan L, Sarikaya ZT, et al. (2020) Brain MRI findings in patients in the intensive care unit with COVID-19 infection [published online ahead of print, 2020 May 8]. Radiology. 201697. https://doi.org/10.1148/radiol.2020201697
Garazzino S, Montagnani C, Donà D, Meini A, Felici E, Vergine G, Bernardi S, Giacchero R, Lo Vecchio A, Marchisio P, Nicolini G, Pierantoni L, Rabbone I, Banderali G, Denina M, Venturini E, Krzysztofiak A, Badolato R, Bianchini S, Galli L, Villani A, Castelli-Gattinara G, Italian SITIP-SIP Pediatric Infection Study Group, Italian SITIP-SIP SARS-CoV-2 paediatric infection study group* (2020) Multicentre Italian study of SARS-CoV-2 infection in children and adolescents, preliminary data as at 10 April 2020. Euro Surveill 25(18):2000600. https://doi.org/10.2807/1560-7917.ES.2020.25.18.2000600
Jain R, Young M, Dogra S, Kennedy H, Nguyen V, Jones S, Bilaloglu S, Hochman K, Raz E, Galetta S, Horwtiz L (2020) COVID-19 related neuroimaging findings: a signal of thromboembolic complications and a strong prognostic marker of poor patient outcome. J Neurol Sci 414:116923. https://doi.org/10.1016/j.jns.2020.116923
Benussi A, Pilotto A, Premi E, et al. Clinical characteristics and outcomes of inpatients with neurologic disease and COVID-19 in Brescia, Lombardy, Italy [published online ahead of print, 2020 May 22]. Neurology. 2020;https://doi.org/10.1212/WNL.0000000000009848
Xiong W, Mu J, Guo J, et al. New onset neurologic events in people with COVID-19 infection in three regions in China [published online ahead of print, 2020 Jun 17]. Neurology. 2020;https://doi.org/10.1212/WNL.0000000000010034
Scullen T, Keen J, Mathkour M, Dumont AS, Kahn L (2020) Coronavirus 2019 (COVID-19)-associated encephalopathies and cerebrovascular disease: the New Orleans experience [published online ahead of print, 2020 May 28]. World Neurosurg. S1878–8750(20)31163–3. https://doi.org/10.1016/j.wneu.2020.05.192
Mahammedi A, Saba L, Vagal A, et al. (2020) Imaging in neurological disease of hospitalized COVID-19 patients: an Italian multicenter retrospective observational study [published online ahead of print, 2020 May 21]. Radiology. 201933. https://doi.org/10.1148/radiol.2020201933
Radmanesh A, Raz E, Zan E, Derman A, Kaminetzky M (2020) Brain imaging use and findings in COVID-19: a single academic center experience in the epicenter of disease in the United States. AJNR Am J Neuroradiol 41(7):1179–1183. https://doi.org/10.3174/ajnr.A6610
Romero-Sánchez CM, Díaz-Maroto I, Fernández-Díaz E, et al. (2020) Neurologic manifestations in hospitalized patients with COVID-19: The ALBACOVID registry [published online ahead of print, 2020 Jun 1]. Neurology. https://doi.org/10.1212/WNL.0000000000009937
Kremer S, Lersy F, de Sèze J, et al. (2020) Brain MRI findings in severe COVID-19: a retrospective observational study [published online ahead of print, 2020 Jun 16]. Radiology ;202222. https://doi.org/10.1148/radiol.2020202222
Pinna P, Grewal P, Hall JP, Tavarez T, Dafer RM, Garg R, Osteraas ND, Pellack DR, Asthana A, Fegan K, Patel V, Conners JJ, John S, Silva ID (2020) Neurological manifestations and COVID-19: experiences from a tertiary care center at the frontline. J Neurol Sci 415:116969. https://doi.org/10.1016/j.jns.2020.116969
Beltrán-Corbellini Á, Chico-García JL, Martínez-Poles J, et al. (2020) Acute-onset smell and taste disorders in the context of COVID-19: a pilot multicentre polymerase chain reaction based case-control study [published online ahead of print, 2020 Apr 22]. Eur J Neurol. https://doi.org/10.1111/ene.14273
Giacomelli A, Pezzati L, Conti F, et al. (2020) Self-reported olfactory and taste disorders in SARS-CoV-2 patients: a cross-sectional study [published online ahead of print, 2020 Mar 26]. Clin Infect Dis. ciaa330. https://doi.org/10.1093/cid/ciaa330
Lechien JR, Chiesa-Estomba CM, De Siati DR et al (2020) Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study. Eur Arch Otorhinolaryngol 277(8):2251–2261. https://doi.org/10.1007/s00405-020-05965-1
Spinato G, Fabbris C, Polesel J, Cazzador D, Borsetto D, Hopkins C, Boscolo-Rizzo P (2020) Alterations in smell or taste in mildly symptomatic outpatients with SARS-CoV-2 infection. JAMA 323(20):2089–2090. https://doi.org/10.1001/jama.2020.6771
Vaira LA, Deiana G, Fois AG, Pirina P, Madeddu G, de Vito A, Babudieri S, Petrocelli M, Serra A, Bussu F, Ligas E, Salzano G, de Riu G (2020) Objective evaluation of anosmia and ageusia in COVID-19 patients: single-center experience on 72 cases. Head Neck 42(6):1252–1258. https://doi.org/10.1002/hed.26204
Vaira LA, Salzano G, Petrocelli M, Deiana G, Salzano FA, De Riu G (2020) Validation of a self-administered olfactory and gustatory test for the remotely evaluation of COVID-19 patients in home quarantine. Head Neck 42(7):1570–1576. https://doi.org/10.1002/hed.26228
Vaira LA, Hopkins C, Salzano G, Petrocelli M, Melis A, Cucurullo M, Ferrari M, Gagliardini L, Pipolo C, Deiana G, Fiore V, de Vito A, Turra N, Canu S, Maglio A, Serra A, Bussu F, Madeddu G, Babudieri S, Giuseppe Fois A, Pirina P, Salzano FA, de Riu P, Biglioli F, de Riu G (2020) Olfactory and gustatory function impairment in COVID-19 patients: Italian objective multicenter-study. Head Neck 42(7):1560–1569. https://doi.org/10.1002/hed.26269
Lee Y, Min P, Lee S, Kim S-W (2020) Prevalence and duration of acute loss of smell or taste in COVID-19 patients. J Korean Med Sci 35(18):e174. https://doi.org/10.3346/jkms.2020.35.e174
Speth MM, Singer-Cornelius T, Oberle M, Gengler I, Brockmeier SJ, Sedaghat AR (2020) Olfactory dysfunction and sinonasal symptomatology in COVID-19: prevalence, severity, timing, and associated characteristics. Otolaryngol Head Neck Surg 163(1):114–120. https://doi.org/10.1177/0194599820929185
Klopfenstein T, Kadiane-Oussou NJ, Toko L, et al. (2020) Features of anosmia in COVID-19 [published online ahead of print, 2020 Apr 17]. Med Mal Infect. S0399-077X(20)30110–4. https://doi.org/10.1016/j.medmal.2020.04.006
Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, Zhang L, Fan G, Xu J, Gu X, Cheng Z, Yu T, Xia J, Wei Y, Wu W, Xie X, Yin W, Li H, Liu M, Xiao Y, Gao H, Guo L, Xie J, Wang G, Jiang R, Gao Z, Jin Q, Wang J, Cao B (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395(10223):497–506. https://doi.org/10.1016/S0140-6736(20)30183-5
Wu C, Chen X, Cai Y, Xia J’, Zhou X, Xu S, Huang H, Zhang L, Zhou X, du C, Zhang Y, Song J, Wang S, Chao Y, Yang Z, Xu J, Zhou X, Chen D, Xiong W, Xu L, Zhou F, Jiang J, Bai C, Zheng J, Song Y (2020) Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med 180(7):934–943. https://doi.org/10.1001/jamainternmed.2020.0994
Yang X, Yu Y, Xu J, Shu H, Xia J', Liu H, Wu Y, Zhang L, Yu Z, Fang M, Yu T, Wang Y, Pan S, Zou X, Yuan S, Shang Y (2020) Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med 8(5):475–481. https://doi.org/10.1016/S2213-2600(20)30079-5
Chen T, Wu D, Chen H, Yan W, Yang D, Chen G, Ma K, Xu D, Yu H, Wang H, Wang T, Guo W, Chen J, Ding C, Zhang X, Huang J, Han M, Li S, Luo X, Zhao J, Ning Q (2020) Clinical characteristics of 113 deceased patients with coronavirus disease 2019: retrospective study [published correction appears in BMJ. 2020 Mar 31;368:m1295]. BMJ 368:m1091 Published 2020 Mar 26. https://doi.org/10.1136/bmj.m1091
Du Y, Tu L, Zhu P et al (2020) Clinical features of 85 fatal cases of COVID-19 from Wuhan. A retrospective observational study. Am J Respir Crit Care Med 201(11):1372–1379. https://doi.org/10.1164/rccm.202003-0543OC
Zheng Y, Xu H, Yang M, Zeng Y, Chen H, Liu R, Li Q, Zhang N, Wang D (2020) Epidemiological characteristics and clinical features of 32 critical and 67 noncritical cases of COVID-19 in Chengdu. J Clin Virol 127:104366. https://doi.org/10.1016/j.jcv.2020.104366
Rodriguez-Morales AJ, Rodriguez-Morales AG, Méndez CA, Hernández-Botero S. Tracing new clinical manifestations in patients with COVID-19 in Chile and its potential relationship with the SARS-CoV-2 divergence [published online ahead of print, 2020 Apr 18]. Curr Trop Med Rep 2020;1–4. https://doi.org/10.1007/s40475-020-00205-2
Wang F, Yang Y, Dong K, Yan Y, Zhang S, Ren H, Yu X, Shi X (2020) Clinical characteristics of 28 patients with diabetes and COVID-19 in Wuhan, China. Endocr Pract 26(6):668–674. https://doi.org/10.4158/EP-2020-0108
Wan S, Xiang Y, Fang W, Zheng Y, Li B, Hu Y, Lang C, Huang D, Sun Q, Xiong Y, Huang X, Lv J, Luo Y, Shen L, Yang H, Huang G, Yang R (2020) Clinical features and treatment of COVID-19 patients in northeast Chongqing. J Med Virol 92(7):797–806. https://doi.org/10.1002/jmv.25783
Wang Z, Yang B, Li Q, Wen L, Zhang R (2020) Clinical features of 69 cases with coronavirus disease 2019 in Wuhan, China [published online ahead of print, 2020 Mar 16]. Clin Infect Dis. ciaa272. https://doi.org/10.1093/cid/ciaa272
Sun D, Li H, Lu X-X, Xiao H, Ren J, Zhang FR, Liu ZS (2020) Clinical features of severe pediatric patients with coronavirus disease 2019 in Wuhan: a single center’s observational study. World J Pediatr 16(3):251–259. https://doi.org/10.1007/s12519-020-00354-4
Tian S, Hu N, Lou J, Chen K, Kang X, Xiang Z, Chen H, Wang D, Liu N, Liu D, Chen G, Zhang Y, Li D, Li J, Lian H, Niu S, Zhang L, Zhang J (2020) Characteristics of COVID-19 infection in Beijing. J Inf Secur 80(4):401–406. https://doi.org/10.1016/j.jinf.2020.02.018
Zhou F, Yu T, Du R et al (2020) Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 395(10229):1054–1062. https://doi.org/10.1016/S0140-6736(20)30566-3
Du N, Chen H, Zhang Q et al (2020) A case series describing the epidemiology and clinical characteristics of COVID-19 infection in Jilin Province. Virulence 11(1):482–485. https://doi.org/10.1080/21505594.2020.1767357
Liu K, Fang Y-Y, Deng Y et al (2020) Clinical characteristics of novel coronavirus cases in tertiary hospitals in Hubei Province. Chin Med J 133(9):1025–1031. https://doi.org/10.1097/CM9.0000000000000744
Tostmann A, Bradley J, Bousema T, et al. (2020) Strong associations and moderate predictive value of early symptoms for SARS-CoV-2 test positivity among healthcare workers, the Netherlands, March 2020. Eurosurveillance. 25(16). https://doi.org/10.2807/1560-7917.ES.2020.25.16.2000508
Yan Y, Yang Y, Wang F, Ren H, Zhang S, Shi X, Yu X, Dong K (2020) Clinical characteristics and outcomes of patients with severe covid-19 with diabetes. BMJ Open Diabetes Res Care 8(1):e001343. https://doi.org/10.1136/bmjdrc-2020-001343
Xu XW, Wu XX, Jiang XG, Xu KJ, Ying LJ, Ma CL, Li SB, Wang HY, Zhang S, Gao HN, Sheng JF, Cai HL, Qiu YQ, Li LJ (2020) Clinical findings in a group of patients infected with the 2019 novel coronavirus (SARS-Cov-2) outside of Wuhan, China: retrospective case series [published correction appears in BMJ. 2020 Feb 27;368:m792]. BMJ 368:m606 Published 2020 Feb 19. https://doi.org/10.1136/bmj.m606
Lian J, Cai H, Hao S, Jin X, Zhang XL, Zheng L, Jia HY, Hu JH, Zhang SY, Yu GD, Gu JQ, Ye CY, Jin CL, Lu YF, Sheng JF, Yang YD (2020) Comparison of epidemiological and clinical characteristics of COVID-19 patients with and without Wuhan exposure. J Zhejiang Univ-Sci B 21(5):369–377. https://doi.org/10.1631/jzus.B2000112
Gupta N, Agrawal S, Ish P, et al. (2020) Clinical and epidemiologic profile of the initial COVID-19 patients at a tertiary care centre in India. Monaldi Arch Chest Dis. 90(1). https://doi.org/10.4081/monaldi.2020.1294
Zhang X, Cai H, Hu J, Lian J, Gu J, Zhang S, Ye C, Lu Y, Jin C, Yu G, Jia H, Zhang Y, Sheng J, Li L, Yang Y (2020) Epidemiological, clinical characteristics of cases of SARS-CoV-2 infection with abnormal imaging findings. Int J Infect Dis 94:81–87. https://doi.org/10.1016/j.ijid.2020.03.040
Li J, Li S, Cai Y et al (2020) Epidemiological and clinical characteristics of 17 hospitalized patients with 2019 novel coronavirus infections outside Wuhan, China. Epidemiology. https://doi.org/10.1101/2020.02.11.20022053
Hung IF-N, Lung K-C, Tso EY-K, Liu R, Chung TWH, Chu MY, Ng YY, Lo J, Chan J, Tam AR, Shum HP, Chan V, Wu AKL, Sin KM, Leung WS, Law WL, Lung DC, Sin S, Yeung P, Yip CCY, Zhang RR, Fung AYF, Yan EYW, Leung KH, Ip JD, Chu AWH, Chan WM, Ng ACK, Lee R, Fung K, Yeung A, Wu TC, Chan JWM, Yan WW, Chan WM, Chan JFW, Lie AKW, Tsang OTY, Cheng VCC, Que TL, Lau CS, Chan KH, To KKW, Yuen KY (2020) Triple combination of interferon beta-1b, lopinavir–ritonavir, and ribavirin in the treatment of patients admitted to hospital with COVID-19: an open-label, randomised, phase 2 trial. Lancet 395(10238):1695–1704. https://doi.org/10.1016/S0140-6736(20)31042-4
Wu H, Zhu H, Yuan C, Yao C, Luo W, Shen X, Wang J, Shao J, Xiang Y (2020) Clinical and immune features of hospitalized pediatric patients with coronavirus disease 2019 (COVID-19) in Wuhan, China. JAMA Netw Open 3(6):e2010895. https://doi.org/10.1001/jamanetworkopen.2020.10895
Argenziano MG, Bruce SL, Slater CL et al (2020) Characterization and clinical course of 1000 patients with coronavirus disease 2019 in New York: retrospective case series. BMJ 369:m1996. Published 2020 May 29. https://doi.org/10.1136/bmj.m1996
Israelsen SB, Kristiansen KT, Hindsberger B et al (2020) Characteristics of patients with COVID-19 pneumonia at Hvidovre Hospital, March–April 2020. Dan Med J 67(6):A05200313 Published 2020 May 15
Cummings MJ, Baldwin MR, Abrams D, Jacobson SD, Meyer BJ, Balough EM, Aaron JG, Claassen J, Rabbani LRE, Hastie J, Hochman BR, Salazar-Schicchi J, Yip NH, Brodie D, O’Donnell MR (2020) Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: a prospective cohort study. Lancet 395(10239):1763–1770. https://doi.org/10.1016/S0140-6736(20)31189-2
Kluytmans-van den Bergh MFQ, AGM B, Pas SD et al (2020) Prevalence and clinical presentation of health care workers with symptoms of coronavirus disease 2019 in 2 Dutch hospitals during an early phase of the pandemic. JAMA Netw Open 3(5):e209673. https://doi.org/10.1001/jamanetworkopen.2020.9673
Nowak B, Szymański P, Pańkowski I, et al. Clinical characteristics and short-term outcomes of coronavirus disease 2019: retrospective, single-center experience of designated hospital in Poland. Pol Arch Intern Med. Published online May 18, 2020. https://doi.org/10.20452/pamw.15361
Lai X, Wang M, Qin C, Tan L, Ran L, Chen D, Zhang H, Shang K, Xia C, Wang S, Xu S, Wang W (2020) Coronavirus disease 2019 (COVID-2019) infection among health care workers and implications for prevention measures in a tertiary Hospital in Wuhan,China. JAMA Netw Open 3(5):e209666. https://doi.org/10.1001/jamanetworkopen.2020.9666
Wang X, Fang J, Zhu Y, et al. Clinical characteristics of non-critically ill patients with novel coronavirus infection (COVID-19) in a Fangcang Hospital. Clin Microbiol Infect. Published online April 2020:S1198743X20301774. https://doi.org/10.1016/j.cmi.2020.03.032
Liu Z, Jin C, Wu CC, Liang T, Zhao H, Wang Y, Wang Z, Li F, Zhou J, Cai S, Zeng L, Yang J (2020) Association between initial chest CT or clinical features and clinical course in patients with coronavirus disease 2019 pneumonia. Korean J Radiol 21(6):736–745. https://doi.org/10.3348/kjr.2020.0171
Huang Q, Deng X, Li Y, Sun X, Chen Q, Xie M, Liu S, Qu H, Liu S, Wang L, He G, Gong Z (2020) Clinical characteristics and drug therapies in patients with the common-type coronavirus disease 2019 in Hunan, China. Int J Clin Pharm 42(3):837–845. https://doi.org/10.1007/s11096-020-01031-2
Hong KS, Lee KH, Chung JH, Shin KC, Choi EY, Jin HJ, Jang JG, Lee W, Ahn JH (2020) Clinical features and outcomes of 98 patients hospitalized with SARS-CoV-2 infection in Daegu, South Korea: a brief descriptive study. Yonsei Med J 61(5):431–437. https://doi.org/10.3349/ymj.2020.61.5.431
Huang R, Zhu L, Xue L et al (2020) Clinical findings of patients with coronavirus disease 2019 in Jiangsu province, China: a retrospective, multi-center study. Santiago H da C, ed. PLoS Negl Trop Dis 14(5):e0008280. https://doi.org/10.1371/journal.pntd.0008280
Ji M, Yuan L, Shen W et al (2020) Characteristics of disease progress in patients with coronavirus disease 2019 in Wuhan, China. Epidemiol Infect 148:e94. Published 2020 May 6. https://doi.org/10.1017/S0950268820000977
Wang D, Yin Y, Hu C, Liu X, Zhang X, Zhou S, Jian M, Xu H, Prowle J, Hu B, Li Y, Peng Z (2020) Clinical course and outcome of 107 patients infected with the novel coronavirus, SARS-CoV-2, discharged from two hospitals in Wuhan, China. Crit Care 24(1):188. https://doi.org/10.1186/s13054-020-02895-6
Aggarwal S, Garcia-Telles N, Aggarwal G, Lavie C, Lippi G, Henry BM (2020) Clinical features, laboratory characteristics, and outcomes of patients hospitalized with coronavirus disease 2019 (COVID-19): early report from the United States. Diagnosis 7(2):91–96. https://doi.org/10.1515/dx-2020-0046
Zhao X-Y, Xu X-X, Yin H-S, Hu QM, Xiong T, Tang YY, Yang AY, Yu BP, Huang ZP (2020) Clinical characteristics of patients with 2019 coronavirus disease in a non-Wuhan area of Hubei Province, China: a retrospective study. BMC Infect Dis 20(1):311. https://doi.org/10.1186/s12879-020-05010-w
Meng Y, Wu P, Lu W et al (2020) Sex-specific clinical characteristics and prognosis of coronavirus disease-19 infection in Wuhan, China: A retrospective study of 168 severe patients. Perlman S, ed. PLoS Pathog 16(4):e1008520. https://doi.org/10.1371/journal.ppat.1008520
Yao Q, Wang P, Wang X, et al. Retrospective study of risk factors for severe SARS-Cov-2 infections in hospitalized adult patients. Pol Arch Intern Med. Published online April 24, 2020. https://doi.org/10.20452/pamw.15312
Zhu L, Wang J, Huang R, Liu L, Zhao H, Wu C, Zhu C (2020) Clinical characteristics of a case series of children with coronavirus disease 2019. Pediatr Pulmonol 55(6):1430–1432. https://doi.org/10.1002/ppul.24767
Kim ES, Chin BS, Kang CK, Kim NJ, Kang YM, Choi JP, Oh DH, Kim JH, Koh B, Kim SE, Yun NR, Lee JH, Kim JY, Kim Y, Bang JH, Song KH, Kim HB, Chung KH, Oh MD, on behalf of the Korea National Committee for Clinical Management of COVID-19 (2020) Clinical course and outcomes of patients with severe acute respiratory syndrome coronavirus 2 infection: a preliminary report of the first 28 patients from the Korean cohort study on COVID-19. J Korean Med Sci 35(13):e142. https://doi.org/10.3346/jkms.2020.35.e142
Bhatraju PK, Ghassemieh BJ, Nichols M, Kim R, Jerome KR, Nalla AK, Greninger AL, Pipavath S, Wurfel MM, Evans L, Kritek PA, West TE, Luks A, Gerbino A, Dale CR, Goldman JD, O’Mahony S, Mikacenic C (2020) Covid-19 in critically ill patients in the Seattle region — case series. N Engl J Med 382(21):2012–2022. https://doi.org/10.1056/NEJMoa2004500
Qiu H, Wu J, Hong L, Luo Y, Song Q, Chen D (2020) Clinical and epidemiological features of 36 children with coronavirus disease 2019 (COVID-19) in Zhejiang, China: an observational cohort study. Lancet Infect Dis 20(6):689–696. https://doi.org/10.1016/S1473-3099(20)30198-5
Chen G, Wu D, Guo W, Cao Y, Huang D, Wang H, Wang T, Zhang X, Chen H, Yu H, Zhang X, Zhang M, Wu S, Song J, Chen T, Han M, Li S, Luo X, Zhao J, Ning Q (2020) Clinical and immunological features of severe and moderate coronavirus disease 2019. J Clin Invest 130(5):2620–2629. https://doi.org/10.1172/JCI137244
Yang W, Cao Q, Qin L, Wang X, Cheng Z, Pan A, Dai J, Sun Q, Zhao F, Qu J, Yan F (2020) Clinical characteristics and imaging manifestations of the 2019 novel coronavirus disease (COVID-19):a multi-center study in Wenzhou city, Zhejiang, China. J Inf Secur 80(4):388–393. https://doi.org/10.1016/j.jinf.2020.02.016
Xu Y-H, Dong J-H, An W-M, Lv XY, Yin XP, Zhang JZ, Dong L, Ma X, Zhang HJ, Gao BL (2020) Clinical and computed tomographic imaging features of novel coronavirus pneumonia caused by SARS-CoV-2. J Inf Secur 80(4):394–400. https://doi.org/10.1016/j.jinf.2020.02.017
Xu X, Yu C, Qu J, Zhang L, Jiang S, Huang D, Chen B, Zhang Z, Guan W, Ling Z, Jiang R, Hu T, Ding Y, Lin L, Gan Q, Luo L, Tang X, Liu J (2020) Imaging and clinical features of patients with 2019 novel coronavirus SARS-CoV-2. Eur J Nucl Med Mol Imaging 47(5):1275–1280. https://doi.org/10.1007/s00259-020-04735-9
Lechien JR, Chiesa-Estomba CM, Place S, et al. Clinical and epidemiological characteristics of 1420 European patients with mild-to-moderate coronavirus disease 2019. J Intern Med. Published online June 17, 2020:joim.13089. https://doi.org/10.1111/joim.13089
CDC COVID-19 response team. Characteristics of health care personnel with COVID-19 - United States, February 12-April 9, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(15):477–481. Published 2020 Apr 17. https://doi.org/10.15585/mmwr.mm6915e6
Levinson R, Elbaz M, Ben-Ami R, Shasha D, Levinson T, Choshen G, Petrov K, Gadoth A, Paran Y (2020) Time course of anosmia and dysgeusia in patients with mild SARS-CoV-2 infection. Infect Dis (Lond) 52(8):600–602. https://doi.org/10.1080/23744235.2020.1772992
Zhu X, Yuan W, Huang K, et al. Clinical features and short-term outcomes of 114 elderly patients with COVID-19 in Wuhan, China: a single-center, retrospective, observational study. SSRN Electron J. Published online 2020. https://doi.org/10.2139/ssrn.3548774
Wang D, Li R, Wang J, et al. Correlation analysis between disease severity and clinical and biochemical characteristics of 143 cases of COVID-19 in Wuhan, China: a descriptive study. BMC Infect Dis. 2020;20(1):519. Published 2020 Jul 16. https://doi.org/10.1186/s12879-020-05242-w
Chen C, Cao M, Peng L, et al. Coronavirus disease-19 among children outside Wuhan, China. SSRN Electron J. Published online 2020. https://doi.org/10.2139/ssrn.3546071
Mo P, Xing Y, Xiao Y, et al. Clinical characteristics of refractory COVID-19 pneumonia in Wuhan, China. Clin Infect Dis. Published online March 16, 2020:ciaa270. https://doi.org/10.1093/cid/ciaa270
Zhang G, Hu C, Luo L, Fang F, Chen Y, Li J, Peng Z, Pan H (2020) Clinical features and short-term outcomes of 221 patients with COVID-19 in Wuhan, China. J Clin Virol 127:104364. https://doi.org/10.1016/j.jcv.2020.104364
Tomlins J, Hamilton F, Gunning S, Sheehy C, Moran E, MacGowan A (2020) Clinical features of 95 sequential hospitalised patients with novel coronavirus 2019 disease (COVID-19), the first UK cohort. J Infect Published online April S0163445320302322:e59–e61. https://doi.org/10.1016/j.jinf.2020.04.020
Zhao Z, Xie J, Yin M, et al. Clinical and laboratory profiles of 75 hospitalized patients with novel coronavirus disease 2019 in Hefei, China. Infectious Diseases (except HIV/AIDS); 2020. https://doi.org/10.1101/2020.03.01.20029785
Huang Y, Yang R, Xu Y, Gong P. Clinical characteristics of 36 non-survivors with COVID-19 in Wuhan, China. Infectious Diseases (except HIV/AIDS); 2020. https://doi.org/10.1101/2020.02.27.20029009
Yan CH, Faraji F, Prajapati DP, Boone CE, DeConde AS (2020) Association of chemosensory dysfunction and COVID-19 in patients presenting with influenza-like symptoms. Int Forum Allergy Rhinol 10(7):806–813. https://doi.org/10.1002/alr.22579
Deng Y, Liu W, Liu K, Fang YY, Shang J, Zhou L, Wang K, Leng F, Wei S, Chen L, Liu HG (2020) Clinical characteristics of fatal and recovered cases of coronavirus disease 2019 in Wuhan, China: a retrospective study. Chin Med J 133(11):1261–1267. https://doi.org/10.1097/CM9.0000000000000824
Chu J, Yang N, Wei Y, Yue H, Zhang F, Zhao J, He L, Sheng G, Chen P, Li G, Wu S, Zhang B, Zhang S, Wang C, Miao X, Li J, Liu W, Zhang H (2020) Clinical characteristics of 54 medical staff with COVID-19: a retrospective study in a single center in Wuhan, China. J Med Virol 92(7):807–813. https://doi.org/10.1002/jmv.25793
Ihle-Hansen H, Berge T, Tveita A, et al. (2020) COVID-19: Symptoms, course of illness and use of clinical scoring systems for the first 42 patients admitted to a Norwegian local hospital. Covid-19: Symptomer, forløp og bruk av kliniske skåringsverktøy hos de 42 første pasientene innlagt på et norsk lokalsykehus. Tidsskr Nor Laegeforen. 140(7):https://doi.org/10.4045/tidsskr.20.0301. Published 2020 Apr 10. https://doi.org/10.4045/tidsskr.20.0301
Goyal P, Choi JJ, Pinheiro LC, Schenck EJ, Chen R, Jabri A, Satlin MJ, Campion TR Jr, Nahid M, Ringel JB, Hoffman KL, Alshak MN, Li HA, Wehmeyer GT, Rajan M, Reshetnyak E, Hupert N, Horn EM, Martinez FJ, Gulick RM, Safford MM (2020) Clinical characteristics of Covid-19 in New York City. N Engl J Med 382(24):2372–2374. https://doi.org/10.1056/NEJMc2010419
Cao J, Tu W-J, Cheng W, et al. Clinical features and short-term outcomes of 102 patients with coronavirus disease 2019 in Wuhan, China. Clin Infect Dis. Published online March 13, 2020:ciaa243. https://doi.org/10.1093/cid/ciaa243
Chang D, Lin M, Wei L, Xie L, Zhu G, dela Cruz CS, Sharma L (2020) Epidemiologic and clinical characteristics of novel coronavirus infections involving 13 patients outside Wuhan, China. JAMA 323(11):1092–1093. https://doi.org/10.1001/jama.2020.1623
Chen H, Guo J, Wang C, Luo F, Yu X, Zhang W, Li J, Zhao D, Xu D, Gong Q, Liao J, Yang H, Hou W, Zhang Y (2020) Clinical characteristics and intrauterine vertical transmission potential of COVID-19 infection in nine pregnant women: a retrospective review of medical records. Lancet 395(10226):809–815. https://doi.org/10.1016/S0140-6736(20)30360-3
Wang L, He W, Yu X, Hu D, Bao M, Liu H, Zhou J, Jiang H (2020) Coronavirus disease 2019 in elderly patients: characteristics and prognostic factors based on 4-week follow-up. J Inf Secur 80(6):639–645. https://doi.org/10.1016/j.jinf.2020.03.019
Spiteri G, Fielding J, Diercke M, et al. (2020) First cases of coronavirus disease 2019 (COVID-19) in the WHO European Region, 24 January to 21 February 2020. Eurosurveillance. 25(9). https://doi.org/10.2807/1560-7917.ES.2020.25.9.2000178
Liu Y, Yang Y, Zhang C, Huang F, Wang F, Yuan J, Wang Z, Li J, Li J, Feng C, Zhang Z, Wang L, Peng L, Chen L, Qin Y, Zhao D, Tan S, Yin L, Xu J, Zhou C, Jiang C, Liu L (2020) Clinical and biochemical indexes from 2019-nCoV infected patients linked to viral loads and lung injury. Sci China Life Sci 63(3):364–374. https://doi.org/10.1007/s11427-020-1643-8
Xu T, Chen C, Zhu Z, Cui M, Chen C, Dai H, Xue Y (2020) Clinical features and dynamics of viral load in imported and non-imported patients with COVID-19. Int J Infect Dis 94:68–71. https://doi.org/10.1016/j.ijid.2020.03.022
Chung M, Bernheim A, Mei X, Zhang N, Huang M, Zeng X, Cui J, Xu W, Yang Y, Fayad ZA, Jacobi A, Li K, Li S, Shan H (2020) CT imaging features of 2019 novel coronavirus (2019-nCoV). Radiology 295(1):202–207. https://doi.org/10.1148/radiol.2020200230
Shi H, Han X, Jiang N, Cao Y, Alwalid O, Gu J, Fan Y, Zheng C (2020) Radiological findings from 81 patients with COVID-19 pneumonia in Wuhan, China: a descriptive study. Lancet Infect Dis 20(4):425–434. https://doi.org/10.1016/S1473-3099(20)30086-4
Yang L, Liu J, Zhang R, Li M, Li Z, Zhou X, Hu C, Tian F, Zhou F, Lei Y (2020) Epidemiological and clinical features of 200 hospitalized patients with corona virus disease 2019 outside Wuhan, China: a descriptive study. J Clin Virol 129:104475. https://doi.org/10.1016/j.jcv.2020.104475
Zhao W, Zhong Z, Xie X, Yu Q, Liu J (2020) Relation between chest CT findings and clinical conditions of coronavirus disease (COVID-19) pneumonia: a multicenter study. Am J Roentgenol 214(5):1072–1077. https://doi.org/10.2214/AJR.20.22976
Han Y, Feng Z, Sun L, et al. A comparative-descriptive analysis of clinical characteristics in 2019-coronavirus-infected children and adults. J Med Virol. Published online April 17, 2020:jmv.25835. https://doi.org/10.1002/jmv.25835
Wang Y, Lu X, Li Y, Chen H, Chen T, Su N, Huang F, Zhou J, Zhang B, Yan F, Wang J (2020) Clinical course and outcomes of 344 intensive care patients with COVID-19. Am J Respir Crit Care Med 201(11):1430–1434. https://doi.org/10.1164/rccm.202003-0736LE
Gilani S, Roditi R, Naraghi M (2020) COVID-19 and anosmia in Tehran, Iran. Med Hypotheses 141:109757. https://doi.org/10.1016/j.mehy.2020.109757
Kaye R, Chang CWD, Kazahaya K, Brereton J, Denneny JC (2020) COVID-19 anosmia reporting tool: initial findings. Otolaryngol Neck Surg 163(1):132–134. https://doi.org/10.1177/0194599820922992
Bagheri SHR, Asghari AM, Farhadi M et al (2020) Coincidence of COVID-19 epidemic and olfactory dysfunction outbreak. Otolaryngology. https://doi.org/10.1101/2020.03.23.20041889
Hopkins C, Surda P, Kumar N (2020) Presentation of new onset anosmia during the COVID-19 pandemic. Rhinol J 58(3):295–298. https://doi.org/10.4193/Rhin20.116
Morassi M, Bagatto D, Cobelli M, D’Agostini S, Gigli GL, Bnà C, Vogrig A (2020) Stroke in patients with SARS-CoV-2 infection: case series. J Neurol 267(8):2185–2192. https://doi.org/10.1007/s00415-020-09885-2
Oxley TJ, Mocco J, Majidi S, Kellner CP, Shoirah H, Singh IP, de Leacy RA, Shigematsu T, Ladner TR, Yaeger KA, Skliut M, Weinberger J, Dangayach NS, Bederson JB, Tuhrim S, Fifi JT (2020) Large-vessel stroke as a presenting feature of Covid-19 in the young. N Engl J Med 382(20):e60. https://doi.org/10.1056/NEJMc2009787
Deliwala S, Abdulhamid S, Abusalih MF, Al-Qasmi MM, Bachuwa G. Encephalopathy as the sentinel sign of a cortical stroke in a patient infected with coronavirus disease-19 (COVID-19). Cureus. Published online May 14, 2020. https://doi.org/10.7759/cureus.8121
Moshayedi P, Ryan TE, Mejia LLP, Nour M, Liebeskind DS (2020) Triage of acute ischemic stroke in confirmed COVID-19: large vessel occlusion associated with coronavirus infection. Front Neurol 11:353. https://doi.org/10.3389/fneur.2020.00353
Muhammad S, Petridis A, Cornelius JF, Hänggi D (2020) Letter to editor: severe brain haemorrhage and concomitant COVID-19 infection: a neurovascular complication of COVID-19. Brain Behav Immun 87:150–151. https://doi.org/10.1016/j.bbi.2020.05.015
Al Saiegh F, Ghosh R, Leibold A, et al. (2020) Status of SARS-CoV-2 in cerebrospinal fluid of patients with COVID-19 and stroke [published online ahead of print, 2020 Apr 30]. J Neurol Neurosurg Psychiatry. jnnp-2020-323522. https://doi.org/10.1136/jnnp-2020-323522
Klein DE, Libman R, Kirsch C, Arora R (2020) Cerebral venous thrombosis: a typical presentation of COVID-19 in the young. J Stroke Cerebrovasc Dis 29(8):104989. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104989
Garaci F, Di Giuliano F, Picchi E, Da Ros V, Floris R (2020) Venous cerebral thrombosis in COVID-19 patient. J Neurol Sci 414:116871. https://doi.org/10.1016/j.jns.2020.116871
Chougar L, Mathon B, Weiss N, Degos V, Shor N. Atypical deep cerebral vein thrombosis with hemorrhagic venous infarction in a patient positive for COVID-19. Am J Neuroradiol. Published online June 18, 2020:ajnr;ajnr.A6642v1. https://doi.org/10.3174/ajnr.A6642
Cavalcanti DD, Raz E, Shapiro M, et al. Cerebral venous thrombosis associated with COVID-19. Am J Neuroradiol. Published online June 18, 2020:ajnr;ajnr.A6644v1. https://doi.org/10.3174/ajnr.A6644
Hemasian H, Ansari B (2020) First case of Covid-19 presented with cerebral venous thrombosis: a rare and dreaded case. Rev Neurol (Paris) 176(6):521–523. https://doi.org/10.1016/j.neurol.2020.04.013
Sweid A, Hammoud B, Weinberg JH, et al. Letter: thrombotic neurovascular disease in COVID-19 patients. Neurosurgery. Published online June 4, 2020:nyaa254. https://doi.org/10.1093/neuros/nyaa254
Hughes C, Nichols T, Pike M, Subbe C, Elghenzai S. Cerebral venous sinus thrombosis as a presentation of COVID-19. Eur J Case Rep Intern Med. Published online 2020:1–4. https://doi.org/10.12890/2020_001691
Zhou B, She J, Wang Y, Ma X (2020) A case of coronavirus disease 2019 with concomitant acute cerebral infarction and deep vein thrombosis. Front Neurol 11:296. https://doi.org/10.3389/fneur.2020.00296
Muhammad S, Petridis A, Cornelius JF, Hänggi D (2020) Letter to editor: severe brain haemorrhage and concomitant COVID-19 infection: a neurovascular complication of COVID-19. Brain Behav Immun 87:150–151. https://doi.org/10.1016/j.bbi.2020.05.015
Sharifi-Razavi A, Karimi N, Rouhani N (2020) COVID-19 and intracerebral haemorrhage: causative or coincidental? New Microbes New Infect 35:100669. https://doi.org/10.1016/j.nmni.2020.100669
Hanafi R, Roger PA, Perin B, et al. (2020) COVID-19 neurologic complication with CNS vasculitis-like pattern [published online ahead of print, 2020 Jun 18]. AJNR Am J Neuroradiol. https://doi.org/10.3174/ajnr.A6651. https://doi.org/10.3174/ajnr.A6651
Fara MG, Stein LK, Skliut M, Morgello S, Fifi JT, Dhamoon MS. Macrothrombosis and stroke in patients with mild Covid-19 infection. J Thromb Haemost. Published online June 25, 2020:jth.14938. https://doi.org/10.1111/jth.14938
Brüggemann R, Gietema H, Jallah B, ten Cate H, Stehouwer C, Spaetgens B (2020) Arterial and venous thromboembolic disease in a patient with COVID-19: a case report. Thromb Res 191:153–155. https://doi.org/10.1016/j.thromres.2020.04.046
Guillan M, Villacieros-Alvarez J, Bellido S, Perez-Jorge Peremarch C, Suarez-Vega VM, Aragones-Garcia M, Cabrera-Rojo C, Fernandez-Ferro J (2020) Unusual simultaneous cerebral infarcts in multiple arterial territories in a COVID-19 patient. Thromb Res 193:107–109. https://doi.org/10.1016/j.thromres.2020.06.015
Escalard S, Maïer B, Redjem H, Delvoye F, Hébert S, Smajda S, Ciccio G, Desilles JP, Mazighi M, Blanc R, Piotin M Treatment of acute ischemic stroke due to large vessel occlusion with COVID-19: experience from Paris. Stroke Published online May 29, 2020. https://doi.org/10.1161/STROKEAHA.120.030574, 2540, 2543
Griffin DO, Jensen A, Khan M, et al. (2020) Arterial thromboembolic complications in COVID-19 in low-risk patients despite prophylaxis. Br J Haematol. 190(1). https://doi.org/10.1111/bjh.16792
Beyrouti R, Adams ME, Benjamin L, et al. Characteristics of ischaemic stroke associated with COVID-19. J Neurol Neurosurg Psychiatry. Published online April 30, 2020:jnnp-2020-323586. https://doi.org/10.1136/jnnp-2020-323586
Nepal P, Batchala PP, Songmen S, Parashar K, Sapire J. An unresponsive COVID-19 patient. Emerg Radiol Published online May 28, 2020. https://doi.org/10.1007/s10140-020-01799-w
Rudilosso S, Esteller D, Urra X, Chamorro Á (2020) Thalamic perforating artery stroke on computed tomography perfusion in a patient with coronavirus disease 2019. J Stroke Cerebrovasc Dis 29(8):104974. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104974
Viguier A, Delamarre L, Duplantier J, Olivot J-M, Bonneville F. Acute ischemic stroke complicating common carotid artery thrombosis during a severe COVID-19 infection. J Neuroradiol Published online May 2020:S0150986120301590. https://doi.org/10.1016/j.neurad.2020.04.003
Zhang Y, Xiao M, Zhang S, Xia P, Cao W, Jiang W, Chen H, Ding X, Zhao H, Zhang H, Wang C, Zhao J, Sun X, Tian R, Wu W, Wu D, Ma J, Chen Y, Zhang D, Xie J, Yan X, Zhou X, Liu Z, Wang J, du B, Qin Y, Gao P, Qin X, Xu Y, Zhang W, Li T, Zhang F, Zhao Y, Li Y, Zhang S (2020) Coagulopathy and antiphospholipid antibodies in patients with Covid-19. N Engl J Med 382(17):e38. https://doi.org/10.1056/NEJMc2007575
Valderrama EV, Humbert K, Lord A, Frontera J, Yaghi S (2020) Severe acute respiratory syndrome coronavirus 2 infection and ischemic stroke. Stroke. 51(7). https://doi.org/10.1161/STROKEAHA.120.030153
Goldberg MF, Goldberg MF, Cerejo R, Tayal AH (2020) Cerebrovascular disease in COVID-19. Am J Neuroradiol 41(7):1170–1172. https://doi.org/10.3174/ajnr.A6588
Sharifi-Razavi A, Karimi N, Zarvani A, Cheraghmakani H, Baghbanian SM. Ischemic stroke associated with novel coronavirus 2019: a report of three cases. Int J Neurosci Published online June 17, 2020:1–5. https://doi.org/10.1080/00207454.2020.1782902
Moriguchi T, Harii N, Goto J, Harada D, Sugawara H, Takamino J, Ueno M, Sakata H, Kondo K, Myose N, Nakao A, Takeda M, Haro H, Inoue O, Suzuki-Inoue K, Kubokawa K, Ogihara S, Sasaki T, Kinouchi H, Kojin H, Ito M, Onishi H, Shimizu T, Sasaki Y, Enomoto N, Ishihara H, Furuya S, Yamamoto T, Shimada S (2020) A first case of meningitis/encephalitis associated with SARS-Coronavirus-2. Int J Infect Dis 94:55–58. https://doi.org/10.1016/j.ijid.2020.03.062
Huang YH, Jiang D, Huang JT (2020) SARS-CoV-2 detected in cerebrospinal fluid by PCR in a case of COVID-19 encephalitis. Brain Behav Immun 87:149. https://doi.org/10.1016/j.bbi.2020.05.012
Domingues RB, Mendes-Correa MC, de Moura Leite FBV, Sabino EC, Salarini DZ, Claro I, Santos DW, de Jesus JG, Ferreira NE, Romano CM, Soares CAS First case of SARS-COV-2 sequencing in cerebrospinal fluid of a patient with suspected demyelinating disease. J Neurol Published online June 20, 2020. https://doi.org/10.1007/s00415-020-09996-w
Farhadian S, Glick LR, Vogels CBF, Thomas J, Chiarella J, Casanovas-Massana A, Zhou J, Odio C, Vijayakumar P, Geng B, Fournier J, Bermejo S, Fauver JR, Alpert T, Wyllie AL, Turcotte C, Steinle M, Paczkowski P, dela Cruz C, Wilen C, Ko AI, MacKay S, Grubaugh ND, Spudich S, Barakat LA (2020) Acute encephalopathy with elevated CSF inflammatory markers as the initial presentation of COVID-19. BMC Neurol 20(1):248. https://doi.org/10.1186/s12883-020-01812-2
Filatov A, Sharma P, Hindi F, Espinosa PS. Neurological complications of coronavirus disease (COVID-19): encephalopathy. Cureus Published online March 21, 2020. https://doi.org/10.7759/cureus.7352
Espinosa PS, Rizvi Z, Sharma P, Hindi F, Filatov A. Neurological complications of coronavirus disease (COVID-19): encephalopathy, MRI brain and cerebrospinal fluid findings: case 2. Cureus. Published online May 2, 2020. https://doi.org/10.7759/cureus.7930
Hepburn M, Mullaguri N, George P, Hantus S, Punia V, Bhimraj A, Newey CR Acute symptomatic seizures in critically ill patients with COVID-19: is there an association? Neurocrit Care Published online May 28, 2020. https://doi.org/10.1007/s12028-020-01006-1
Pilotto A, Odolini S, Masciocchi S, et al. Steroid-responsive encephalitis in coronavirus disease 2019. Ann Neurol. Published online June 9, 2020:ana.25783. https://doi.org/10.1002/ana.25783
Yin R, Feng W, Wang T, et al. Concomitant neurological symptoms observed in a patient diagnosed with coronavirus disease 2019. J Med Virol. Published online June 29, 2020:jmv.25888. https://doi.org/10.1002/jmv.25888
Afshar H, Yassin Z, Kalantari S, Aloosh O, Lotfi T, Moghaddasi M, Sadeghipour A, Emamikhah M Evolution and resolution of brain involvement associated with SARS- CoV2 infection: a close clinical – paraclinical follow up study of a case. Mult Scler Relat Disord 2020;43:102216. https://doi.org/10.1016/j.msard.2020.102216
Al-olama M, Rashid A, Garozzo D (2020) COVID-19-associated meningoencephalitis complicated with intracranial hemorrhage: a case report. Acta Neurochir 162(7):1495–1499. https://doi.org/10.1007/s00701-020-04402-w
Duong L, Xu P, Liu A (2020) Meningoencephalitis without respiratory failure in a young female patient with COVID-19 infection in Downtown Los Angeles, early April 2020. Brain Behav Immun 87:33. https://doi.org/10.1016/j.bbi.2020.04.024
Wong PF, Craik S, Newman P, Makan A, Srinivasan K, Crawford E, Dev D, Moudgil H, Ahmad N (2020) Lessons of the month 1: a case of rhombencephalitis as a rare complication of acute COVID-19 infection. Clin Med 20(3):293–294. https://doi.org/10.7861/clinmed.2020-0182
Zanin L, Saraceno G, Panciani PP, Renisi G, Signorini L, Migliorati K, Fontanella MM (2020) SARS-CoV-2 can induce brain and spine demyelinating lesions. Acta Neurochir 162(7):1491–1494. https://doi.org/10.1007/s00701-020-04374-x
Vollono C, Rollo E, Romozzi M, Frisullo G, Servidei S, Borghetti A, Calabresi P (2020) Focal status epilepticus as unique clinical feature of COVID-19: a case report. Seizure 78:109–112. https://doi.org/10.1016/j.seizure.2020.04.009
Kadono Y, Nakamura Y, Ogawa Y, Yamamoto S, Kajikawa R, Nakajima Y, Matsumoto M, Kishima H (2020) A case of COVID-19 infection presenting with a seizure following severe brain edema. Seizure 80:53–55. https://doi.org/10.1016/j.seizure.2020.06.015
Sohal S, Mansur M (2020) COVID-19 presenting with seizures. IDCases 20:e00782. https://doi.org/10.1016/j.idcr.2020.e00782
Dixon L, Varley J, Gontsarova A, Mallon D, Tona F, Muir D, Luqmani A, Jenkins IH, Nicholas R, Jones B, Everitt A (2020) COVID-19-related acute necrotizing encephalopathy with brain stem involvement in a patient with aplastic anemia. Neurol - Neuroimmunol Neuroinflammation 7(5):e789. https://doi.org/10.1212/NXI.0000000000000789
Karimi N, Sharifi Razavi A, Rouhani N (2020) Frequent convulsive seizures in an adult patient with COVID-19: a case report. Iran Red Crescent Med J 22(3). https://doi.org/10.5812/ircmj.102828
Somani S, Pati S, Gaston T, Chitlangia A, Agnihotri S (2020) De novo status epilepticus in patients with COVID-19. Ann Clin Transl Neurol 7(7):1240–1244. https://doi.org/10.1002/acn3.51071
McAbee GN, Brosgol Y, Pavlakis S, Agha R, Gaffoor M. Encephalitis associated with COVID-19 infection in an 11-year-old child. Pediatr Neurol. Published online April 2020:S0887899420301430. https://doi.org/10.1016/j.pediatrneurol.2020.04.013
Dugue R, Cay-Martínez KC, Thakur KT, Garcia JA, Chauhan LV, Williams SH, Briese T, Jain K, Foca M, McBrian DK, Bain JM, Lipkin WI, Mishra N (2020) Neurologic manifestations in an infant with COVID-19. Neurology 94(24):1100–1102. https://doi.org/10.1212/WNL.0000000000009653
Kaya Y, Kara S, Akinci C, Kocaman AS (2020) Transient cortical blindness in COVID-19 pneumonia; a PRES-like syndrome: case report. J Neurol Sci 413:116858. https://doi.org/10.1016/j.jns.2020.116858
Poyiadji N, Shahin G, Noujaim D, Stone M, Patel S, Griffith B. COVID-19–associated acute hemorrhagic necrotizing encephalopathy: CT and MRI features. Radiology. Published online March 31, 2020:201187. https://doi.org/10.1148/radiol.2020201187
Radmanesh A, Derman A, Ishida K (2020) COVID-19-associated delayed posthypoxic necrotizing leukoencephalopathy. J Neurol Sci 415:116945. https://doi.org/10.1016/j.jns.2020.116945
Hayashi M, Sahashi Y, Baba Y, Okura H, Shimohata T (2020) COVID-19-associated mild encephalitis/encephalopathy with a reversible splenial lesion. J Neurol Sci 415:116941. https://doi.org/10.1016/j.jns.2020.116941
Parsons T, Banks S, Bae C, Gelber J, Alahmadi H, Tichauer M. COVID-19-associated acute disseminated encephalomyelitis (ADEM). J Neurol Published online May 30, 2020. https://doi.org/10.1007/s00415-020-09951-9
Novi G, Rossi T, Pedemonte E, Saitta L, Rolla C, Roccatagliata L, Inglese M, Farinini D (2020) Acute disseminated encephalomyelitis after SARS-CoV-2 infection. Neurol - Neuroimmunol Neuroinflammation 7(5):e797. https://doi.org/10.1212/NXI.0000000000000797
Beach SR, Praschan NC, Hogan C, Dotson S, Merideth F, Kontos N, Fricchione GL, Smith FA (2020) Delirium in COVID-19: a case series and exploration of potential mechanisms for central nervous system involvement. Gen Hosp Psychiatry 65:47–53. https://doi.org/10.1016/j.genhosppsych.2020.05.008
Alkeridy WA, Almaghlouth I, Alrashed R, Alayed K, Binkhamis K, Alsharidi A, Liu-Ambrose T (2020) A unique presentation of delirium in a patient with otherwise asymptomatic COVID -19. J Am Geriatr Soc 68(7):1382–1384. https://doi.org/10.1111/jgs.16536
Neerland BE, Dobloug A, Nore KG, Mikaelsen EE, Halsen A, Ahmed MV. COVID-19 in an elderly woman with acute functional decline. Covid-19 påvist hos eldre kvinne med akutt funksjonssvikt. Tidsskr Nor Laegeforen. 2020;140(7):https://doi.org/10.4045/tidsskr.20.0307. Published 2020 Apr 9.
Yin R, Feng W, Wang T, et al. Concomitant neurological symptoms observed in a patient diagnosed with coronavirus disease 2019. J Med Virol. Published online June 29, 2020:jmv.25888. https://doi.org/10.1002/jmv.25888
Zhao H, Shen D, Zhou H, Liu J, Chen S (2020) Guillain-Barré syndrome associated with SARS-CoV-2 infection: causality or coincidence? Lancet Neurol 19(5):383–384. https://doi.org/10.1016/S1474-4422(20)30109-5
Camdessanche J-P, Morel J, Pozzetto B, Paul S, Tholance Y, Botelho-Nevers E (2020) COVID-19 may induce Guillain–Barré syndrome. Rev Neurol (Paris) 176(6):516–518. https://doi.org/10.1016/j.neurol.2020.04.003
Coen M, Jeanson G, Culebras Almeida LA, Hübers A, Stierlin F, Najjar I, Ongaro M, Moulin K, Makrygianni M, Leemann B, Kronig I, Bertrand J, Reny JL, Schibler M, Serratrice J (2020) Guillain-Barré syndrome as a complication of SARS-CoV-2 infection. Brain Behav Immun 87:111–112. https://doi.org/10.1016/j.bbi.2020.04.074
El Otmani H, El Moutawakil B, Rafai M-A et al (2020) Covid-19 and Guillain-Barré syndrome: more than a coincidence! Rev Neurol (Paris) 176(6):518–519. https://doi.org/10.1016/j.neurol.2020.04.007
Lascano AM, Epiney J, Coen M, et al. SARS-CoV-2 and Guillain-Barré syndrome: AIDP variant with favorable outcome. Eur J Neurol. Published online June 2020:ene.14368. https://doi.org/10.1111/ene.14368
Bigaut K, Mallaret M, Baloglu S, Nemoz B, Morand P, Baicry F, Godon A, Voulleminot P, Kremer L, Chanson JB, de Seze J (2020) Guillain-Barré syndrome related to SARS-CoV-2 infection. Neurol - Neuroimmunol Neuroinflammation 7(5):e785. https://doi.org/10.1212/NXI.0000000000000785
Alberti P, Beretta S, Piatti M, Karantzoulis A, Piatti ML, Santoro P, Viganò M, Giovannelli G, Pirro F, Montisano DA, Appollonio I, Ferrarese C (2020) Guillain-Barré syndrome related to COVID-19 infection. Neurol - Neuroimmunol Neuroinflammation 7(4):e741. https://doi.org/10.1212/NXI.0000000000000741
Padroni M, Mastrangelo V, Asioli GM, Pavolucci L, Abu-Rumeileh S, Piscaglia MG, Querzani P, Callegarini C, Foschi M (2020) Guillain-Barré syndrome following COVID-19: new infection, old complication? J Neurol 267(7):1877–1879. https://doi.org/10.1007/s00415-020-09849-6
Helbok R, Beer R, Löscher W, et al. Guillain-Barré syndrome in a patient with antibodies against SARS-COV-2. Eur J Neurol. Published online June 12, 2020:ene.14388. https://doi.org/10.1111/ene.14388
Scheidl E, Canseco DD, Hadji-Naumov A, Bereznai B (2020) Guillain-Barr é syndrome during SARS-CoV-2 pandemic: a case report and review of recent literature. J Peripher Nerv Syst 25(2):204–207. https://doi.org/10.1111/jns.12382
Kilinc D, van de Pasch S, Doets AY, Jacobs BC, van Vliet J, Garssen MPJ. Guillain-Barré syndrome after SARS-CoV-2 infection. Eur J Neurol. Published online June 13, 2020:ene.14398. https://doi.org/10.1111/ene.14398
Sedaghat Z, Karimi N (2020) Guillain Barre syndrome associated with COVID-19 infection: a case report. J Clin Neurosci 76:233–235. https://doi.org/10.1016/j.jocn.2020.04.062
Rana S, Lima AA, Chandra R, Valeriano J, Desai T, Freiberg W, Small G (2020) Novel coronavirus (COVID-19)-associated Guillain-Barré syndrome: case report. J Clin Neuromuscul Dis 21(4):240–242. https://doi.org/10.1097/CND.0000000000000309
Assini A, Benedetti L, Di Maio S, Schirinzi E, Del Sette M (2020) New clinical manifestation of COVID-19 related Guillain-Barrè syndrome highly responsive to intravenous immunoglobulins: two Italian cases. Neurol Sci 41(7):1657–1658. https://doi.org/10.1007/s10072-020-04484-5
Virani A, Rabold E, Hanson T, Haag A, Elrufay R, Cheema T, Balaan M, Bhanot N (2020) Guillain-Barré syndrome associated with SARS-CoV-2 infection. IDCases 20:e00771. https://doi.org/10.1016/j.idcr.2020.e00771
Ottaviani D, Boso F, Tranquillini E, Gapeni I, Pedrotti G, Cozzio S, Guarrera GM, Giometto B (2020) Early Guillain-Barré syndrome in coronavirus disease 2019 (COVID-19): a case report from an Italian COVID-hospital. Neurol Sci 41(6):1351–1354. https://doi.org/10.1007/s10072-020-04449-8
Juliao Caamaño DS, Alonso BR (2020) Facial diplegia, a possible atypical variant of Guillain-Barré syndrome as a rare neurological complication of SARS-CoV-2. J Clin Neurosci 77:230–232. https://doi.org/10.1016/j.jocn.2020.05.016
Webb S, Wallace VC, Martin-Lopez D, Yogarajah M (2020) Guillain-Barré syndrome following COVID-19: a newly emerging post-infectious complication. BMJ Case Rep 13(6):e236182. https://doi.org/10.1136/bcr-2020-236182
Arnaud S, Budowski C, Wing N, Tin S, Degos B (2020) Post SARS-CoV-2 Guillain-Barré syndrome. Clin Neurophysiol 131(7):1652–1654. https://doi.org/10.1016/j.clinph.2020.05.003
Sancho-Saldaña A, Lambea-Gil Á, Liesa JLC, Caballo MRB, Garay MH, Celada DR, Serrano-Ponz M (2020) Guillain–Barré syndrome associated with leptomeningeal enhancement following SARS-CoV-2 infection. Clin Med 20(4):e93–e94. https://doi.org/10.7861/clinmed.2020-0213
Reyes-Bueno JA, García-Trujillo L, Urbaneja P, et al. Miller-Fisher syndrome after SARS-CoV-2 infection. Eur J Neurol. Published online June 5, 2020:ene.14383. https://doi.org/10.1111/ene.14383
Toscano G, Palmerini F, Ravaglia S, Ruiz L, Invernizzi P, Cuzzoni MG, Franciotta D, Baldanti F, Daturi R, Postorino P, Cavallini A, Micieli G (2020) Guillain–Barré syndrome associated with SARS-CoV-2. N Engl J Med 382(26):2574–2576. https://doi.org/10.1056/NEJMc2009191
Gutiérrez-Ortiz C, Méndez A, Rodrigo-Rey S, et al. Miller Fisher syndrome and polyneuritis cranialis in COVID-19. Neurology. Published online April 17, 2020:https://doi.org/10.1212/WNL.0000000000009619.
Manganotti P, Pesavento V, Buoite Stella A, Bonzi L, Campagnolo E, Bellavita G, Fabris B, Luzzati R Miller Fisher syndrome diagnosis and treatment in a patient with SARS-CoV-2. J Neurovirol Published online June 11, 2020. https://doi.org/10.1007/s13365-020-00858-9
Dinkin M, Gao V, Kahan J, et al. COVID-19 presenting with ophthalmoparesis from cranial nerve palsy. Neurology. Published online May 1, 2020:https://doi.org/10.1212/WNL.0000000000009700. https://doi.org/10.1212/WNL.0000000000009700
Abdelnour L, Eltahir Abdalla M, Babiker S (2020) COVID 19 infection presenting as motor peripheral neuropathy. J Formos Med Assoc 119(6):1119–1120. https://doi.org/10.1016/j.jfma.2020.04.024
Zhang Q, Shan KS, Minalyan A, O’Sullivan C, Nace T. A rare presentation of coronavirus disease 2019 (COVID-19) induced viral myositis with subsequent rhabdomyolysis. Cureus Published online May 12, 2020. https://doi.org/10.7759/cureus.8074
Jin M, Tong Q (2020) Rhabdomyolysis as potential late complication associated with COVID-19. Emerg Infect Dis 26(7):1618–1620. https://doi.org/10.3201/eid2607.200445
Suwanwongse K, Shabarek N. Rhabdomyolysis as a presentation of 2019 novel coronavirus disease. Cureus Published online April 6, 2020. https://doi.org/10.7759/cureus.7561
Munz M, Wessendorf S, Koretsis G, Tewald F, Baegi R, Krämer S, Geissler M, Reinhard M (2020) Acute transverse myelitis after COVID-19 pneumonia. J Neurol 267(8):2196–2197. https://doi.org/10.1007/s00415-020-09934-w
Rábano-Suárez P, Bermejo-Guerrero L, Méndez-Guerrero A, et al. Generalized myoclonus in COVID-19. Neurology. Published online May 21, 2020:https://doi.org/10.1212/WNL.0000000000009829.
Krajewski PK, Szepietowski JC, Maj J (2020) Cutaneous hyperesthesia: a novel manifestation of COVID-19. Brain Behav Immun 87:188. https://doi.org/10.1016/j.bbi.2020.05.064
Aoyagi Y, Ohashi M, Funahashi R, Otaka Y, Saitoh E (2020) Oropharyngeal dysphagia and aspiration pneumonia following coronavirus disease 2019: a case report. Dysphagia 35(4):545–548. https://doi.org/10.1007/s00455-020-10140-z
Acharya S, Diamond M, Anwar S, Glaser A, Tyagi P (2020) Unique case of central retinal artery occlusion secondary to COVID-19 disease. IDCases 21:e00867. https://doi.org/10.1016/j.idcr.2020.e00867
Selvaraj V, Sacchetti D, Finn A, Dapaah-Afriyie K (2020) Acute vision loss in a patient with COVID-19. R I Med J (2013) 103(6):37–38 Published 2020 Jun 10
Wan Y, Shang J, Graham R, Baric RS, Li F (2020) Receptor recognition by the novel coronavirus from Wuhan: an analysis based on decade-long structural studies of SARS coronavirus. Gallagher T, ed. J Virol 94(7):e00127–e00120, /jvi/94/7/JVI.00127–20.atom. https://doi.org/10.1128/JVI.00127-20
Yang J, Zheng Y, Gou X, Pu K, Chen Z, Guo Q, Ji R, Wang H, Wang Y, Zhou Y (2020) Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis 94:91–95. https://doi.org/10.1016/j.ijid.2020.03.017
Krauer F, Riesen M, Reveiz L et al (2017) Zika virus infection as a cause of congenital brain abnormalities and Guillain–Barré syndrome: systematic review. von Seidlein L, ed. PLoS Med 14(1):e1002203. https://doi.org/10.1371/journal.pmed.1002203
Hoffmann M, Kleine-Weber H, Schroeder S et al (2020) SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 181(2):271–280.e8. https://doi.org/10.1016/j.cell.2020.02.052
Hofmann H, Geier M, Marzi A, Krumbiegel M, Peipp M, Fey GH, Gramberg T, Pöhlmann S (2004) Susceptibility to SARS coronavirus S protein-driven infection correlates with expression of angiotensin converting enzyme 2 and infection can be blocked by soluble receptor. Biochem Biophys Res Commun 319(4):1216–1221. https://doi.org/10.1016/j.bbrc.2004.05.114
McGonagle D, Sharif K, O’Regan A, Bridgewood C (2020) The role of cytokines including interleukin-6 in COVID-19 induced pneumonia and macrophage activation syndrome-like disease. Autoimmun Rev 19(6):102537. https://doi.org/10.1016/j.autrev.2020.102537
Qin C, Zhou L, Hu Z, Zhang S, Yang S, Tao Y, Xie C, Ma K, Shang K, Wang W, Tian DS (2020) Dysregulation of immune response in patients with coronavirus 2019 (COVID-19) in Wuhan, China. Clin Infect Dis 71(15):762–768. https://doi.org/10.1093/cid/ciaa248
Kim J-E, Heo J-H, Kim H, Song SH, Park SS, Park TH, Ahn JY, Kim MK, Choi JP (2017) Neurological complications during treatment of Middle East respiratory syndrome. J Clin Neurol 13(3):227. https://doi.org/10.3988/jcn.2017.13.3.227
Fu L, Wang B, Yuan T, Chen X, Ao Y, Fitzpatrick T, Li P, Zhou Y, Lin YF, Duan Q, Luo G, Fan S, Lu Y, Feng A, Zhan Y, Liang B, Cai W, Zhang L, du X, Li L, Shu Y, Zou H (2020) Clinical characteristics of coronavirus disease 2019 (COVID-19) in China: a systematic review and meta-analysis. J Inf Secur 80(6):656–665. https://doi.org/10.1016/j.jinf.2020.03.041
Zhu J, Zhong Z, Ji P et al (2020) Clinicopathological characteristics of 8697 patients with COVID-19 in China: a meta-analysis [published correction appears in Fam Med Community Health. 2020 May;8(2)]. Fam Med Community Health 8(2):e000406. https://doi.org/10.1136/fmch-2020-000406
Rodriguez-Morales AJ, Cardona-Ospina JA, Gutiérrez-Ocampo E, Villamizar-Peña R, Holguin-Rivera Y, Escalera-Antezana JP, Alvarado-Arnez LE, Bonilla-Aldana DK, Franco-Paredes C, Henao-Martinez AF, Paniz-Mondolfi A, Lagos-Grisales GJ, Ramírez-Vallejo E, Suárez JA, Zambrano LI, Villamil-Gómez WE, Balbin-Ramon GJ, Rabaan AA, Harapan H, Dhama K, Nishiura H, Kataoka H, Ahmad T, Sah R, Latin American Network of Coronavirus Disease 2019-COVID-19 Research (LANCOVID-19). Electronic address: https://www.lancovid.org (2020) Clinical, laboratory and imaging features of COVID-19: a systematic review and meta-analysis. Travel Med Infect Dis 34:101623. https://doi.org/10.1016/j.tmaid.2020.101623
Author information
Authors and Affiliations
Contributions
TF and AP conceptualized the study and searched and screened the literature. PD and RNC extracted and analysed the data. RNC contributed to figures, tables, and interpretation of images. KC was involved in extraction of data. DJ, VNM, TF, and AP were involved in study design, data interpretation, and data analysis. RM and MP did the statistical analysis. AK drafted the manuscript, data collection, figures. VKS did literature search, drafted the manuscript, and contributed to study design. TF wrote the first draft of the manuscript with input from AP.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Favas, T.T., Dev, P., Chaurasia, R.N. et al. Neurological manifestations of COVID-19: a systematic review and meta-analysis of proportions. Neurol Sci 41, 3437–3470 (2020). https://doi.org/10.1007/s10072-020-04801-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-020-04801-y