Abstract
Background
Reflux frequently occurs after a gastric conduit has replaced the resected esophagus. In this Swedish population-based cohort study, the potential antireflux effects of using cervical anastomosis, intrathoracic antireflux anastomosis, or pyloric drainage, and a risk of dysphagia due to cervical anastomosis and intrathoracic antireflux anastomosis were studied.
Methods
Patients undergoing esophagectomy with gastric conduit reconstruction in 2001–2005 were included. Reflux symptoms and dysphagia were assessed 6 months and 3 years postoperatively using a validated questionnaire (EORTC QLQ-OES18). The study exposures were cervical anastomosis, antireflux anastomosis, and pyloric drainage procedure. Multivariable logistic regression and propensity-adjusted analyses based on multinomial logistic regression estimated odds ratios (OR) with 95 % confidence intervals (CI), adjusted for potential confounding.
Results
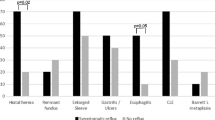
A total of 304 patients were included in the study. Adjusted ORs for reflux symptoms were 0.9 (95 % CI 0.3–2.2) for patients with a cervical anastomosis compared to patients with an intrathoracic anastomosis, 0.9 (95 % CI 0.4–2.0) for patients with an antireflux anastomosis versus patients with a conventional anastomosis, and 1.5 (95 % CI 0.9–2.6) for patients after pyloric drainage versus patients without such a pyloric drainage procedure. Dysphagia was not statistically significantly increased after cervical anastomosis or antireflux anastomosis. ORs were virtually similar 3 years after surgery. No interactions were identified. The propensity analyses rendered similar results as the logistic regression models, except for a possibly increased dysphagia with a cervical anastomosis.
Conclusions
Cervical anastomosis, antireflux anastomosis, and pyloric drainage do not seem to prevent reflux symptoms 6 months or 3 years after esophagectomy for cancer with a gastric conduit.
Similar content being viewed by others
References
Djarv T, Lagergren J, Blazeby JM, Lagergren P. Long-term health-related quality of life following surgery for oesophageal cancer. Br J Surg. 2008;95:1121–6.
Blazeby JM, Metcalfe C, Nicklin J, et al. Association between quality of life scores and short-term outcome after surgery for cancer of the oesophagus or gastric cardia. Br J Surg. 2005;92:1502–7.
Shibuya S, Fukudo S, Shineha R, et al. High incidence of reflux esophagitis observed by routine endoscopic examination after gastric pull-up esophagectomy. World J Surg. 2003;27:580–3.
Bemelman WA, Verburg J, Brummelkamp WH, Klopper PJ. A physical model of the intrathoracic stomach. Am J Physiol. 1988;254:G168–75.
Aly A, Jamieson GG, Pyragius M, Devitt PG. Antireflux anastomosis following oesophagectomy. ANZ J Surg. 2004;74:434–8.
Aly A, Jamieson GG. Reflux after oesophagectomy. Br J Surg. 2004;91:137–41.
Aly A, Jamieson GG, Watson DI, et al. An antireflux anastomosis following esophagectomy: a randomized controlled trial. J Gastrointest Surg. 2010;14:470–5.
Velanovich V, Mohlberg N. The split-stomach fundoplication after esophagogastrectomy. J Gastrointest Surg. 2006;10:178–83.
De Leyn P, Coosemans W, Lerut T. Early and late functional results in patients with intrathoracic gastric replacement after oesophagectomy for carcinoma. Eur J Cardiothorac Surg. 1992;6:79–84.
D’Journo XB, Martin J, Ferraro P, Duranceau A. The esophageal remnant after gastric interposition. Dis Esophagus. 2008;21:377–88.
van Heijl M, Gooszen JA, Fockens P, et al. Risk factors for development of benign cervical strictures after esophagectomy. Ann Surg. 2010;251:1064–9.
Sutcliffe RP, Forshaw MJ, Tandon R, et al. Anastomotic strictures and delayed gastric emptying after esophagectomy: incidence, risk factors and management. Dis Esophagus. 2008;21:712–7.
Palmes D, Weilinghoff M, Colombo-Benkmann M, et al. Effect of pyloric drainage procedures on gastric passage and bile reflux after esophagectomy with gastric conduit reconstruction. Langenbecks Arch Surg. 2007;392:135–41.
Urschel JD, Blewett CJ, Young JE, et al. Pyloric drainage (pyloroplasty) or no drainage in gastric reconstruction after esophagectomy: a meta-analysis of randomized controlled trials. Dig Surg. 2002;19:160–4.
Chattopadhyay TK, Shad SK, Kumar A. Intragastric bile acid and symptoms in patients with an intrathoracic stomach after oesophagectomy. Br J Surg. 1993;80:371–3.
Poghosyan T, Gaujoux S, Chirica M, et al. Functional disorders and quality of life after esophagectomy and gastric tube reconstruction for cancer. J Visc Surg. 2011;148:e327–35.
Borst HG, Dragojevic D, Stegmann T, Hetzer R. Anastomotic leakage, stenosis, and reflux after esophageal replacement. World J Surg. 1978;2:861–4.
Bais JE, Wijnhoven BP, Masclee AA, et al. Analysis and surgical treatment of persistent dysphagia after Nissen fundoplication. Br J Surg. 2001;88:569–76.
Stein HJ, Feussner H, Siewert JR. Failure of antireflux surgery: causes and management strategies. Am J Surg. 1996;171:36–9.
Viklund P, Lindblad M, Lu M, et al. Risk factors for complications after esophageal cancer resection: a prospective population-based study in Sweden. Ann Surg. 2006;243:204–11.
Lagergren J, Bergstrom R, Lindgren A, Nyren O. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med. 1999;340:825–31.
Blazeby JM, Conroy T, Hammerlid E, et al. Clinical and psychometric validation of an EORTC questionnaire module, the EORTC QLQ-OES18, to assess quality of life in patients with oesophageal cancer. Eur J Cancer. 2003;39:1384–94.
Lagergren P, Johar AM, Lagergren J. Validation of the reflux scale in the European Organisation for Research and Treatment of Cancer QLQ-OES18. Eur J Cancer. 2013;49(5):1097–103.
Djarv T, Lagergren P. Six-month postoperative quality of life predicts long-term survival after oesophageal cancer surgery. Eur J Cancer. 2011;47:530–5.
Djarv T, Blazeby JM, Lagergren P. Predictors of postoperative quality of life after esophagectomy for cancer. J Clin Oncol. 2009;27:1963–8.
D’Agostino RB Jr. Propensity score methods for bias reduction in the comparison of a treatment to a non-randomized control group. Stat Med. 1998;17:2265–81.
Imbens GW. The role of the propensity score in estimating dose-response functions. Biometrika. 2000;87:5.
Reeve BB, Smith AW, Arora NK, Hays RD. Reducing bias in cancer research: application of propensity score matching. Health Care Financ Rev. 2008;29:69–80.
Vakil N, van Zanten SV, Kahrilas P, et al. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101:1900–20.
D’Journo XB, Martin J, Rakovich G, et al. Mucosal damage in the esophageal remnant after esophagectomy and gastric transposition. Ann Surg. 2009;249:262–8.
Johansson J, Johnsson F, Groshen S, Walther B. Pharyngeal reflux after gastric pull-up esophagectomy with neck and chest anastomoses. J Thorac Cardiovasc Surg. 1999;118:1078–83.
Okuyama M, Motoyama S, Maruyama K, et al. Proton pump inhibitors relieve and prevent symptoms related to gastric acidity after esophagectomy. World J Surg. 2008;32:246–54.
Storr M, Meining A, Allescher HD. Pathophysiology and pharmacological treatment of gastroesophageal reflux disease. Dig Dis. 2000;18:93–102.
Khan OA, Manners J, Rengarajan A, Dunning J. Does pyloroplasty following esophagectomy improve early clinical outcomes? Interact Cardiovasc Thorac Surg. 2007;6:247–50.
Fok M, Cheng SW, Wong J. Pyloroplasty versus no drainage in gastric replacement of the esophagus. Am J Surg. 1991;162:447–52.
FUNDING
Funding was provided by the Swedish Cancer Society and the Swedish Research Council.
CONFLICT OF INTEREST
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van der Schaaf, M., Johar, A., Lagergren, P. et al. Surgical Prevention of Reflux after Esophagectomy for Cancer. Ann Surg Oncol 20, 3655–3661 (2013). https://doi.org/10.1245/s10434-013-3041-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-013-3041-3