Key Summary Points
To review the published literature on the cost of delirium.
AbstractSection FindingsEvery study has found that delirium increases the cost of care in every setting, in hospital, after discharge at home and in long-term care.
AbstractSection MessageDelirium results in increased financial and social costs which, when considered with the impacts on morbidity and mortality, support the call to urgently improve prevention, screening, diagnosis and treatment of delirium.
Abstract
Purpose
Delirium is common with serious short- and long-term sequelae. However, there are no licensed treatments internationally and relatively little biomedical discovery with the target of finding a cure, with the invisibility or underestimation of the economic implications as a potential driver for this inertia.
Methods
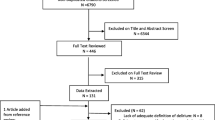
We conducted a narrative review of published literature in English quantitatively evaluating the financial and social costs of delirium to the health and care systems, patients and their carers.
Results
Delirium increases the cost of the index hospitalisation as well as increasing the need for post-acute care and the demands on unpaid, often older, carers. Delirium may cause as much as 10% of all cases of dementia and the ongoing need for care of these people with dementia doubles the cost of delirium. Prevention of delirium not only reduces the cost of delirium but also may decrease subsequent rate of dementia.
Conclusion
The high cost of delirium itself as well as the resultant dementia warrants greater efforts to prevent delirium and discover effective treatment.
Similar content being viewed by others
References
Caplan G (2011) Managing delirium in older patients. Aust Prescr 34(1):16–18
Witlox J, Eurelings LSM, de Jonghe JFM et al (2010) Delirium in elderly patients and the risk of postdischarge mortality, institutionalization, and dementia: a meta-analysis. JAMA 304(4):443–451
Crocker E, Beggs T, Hassan A et al (2016) Long-term effects of postoperative delirium in patients undergoing cardiac operation: a systematic review. Ann Thorac Surg 102:1391–1399
Gleason LJ, Schmitt EM, Kosar CM et al (2015) Effect of delirium and other major complications on outcomes after elective surgery in older adults. JAMA Surg 150(12):1134–1140
Caplan GA, Brown A (1997) Post acute care: can hospitals do better with less? Aust Hlth Rev 20:43–54
Collinsworth AW, Priest EL, Campbell CR et al (2016) A review of multifaceted care approaches for the prevention and mitigation of delirium in intensive care units. J Intensive Care Med 31(2):127–141. https://doi.org/10.1177/0885066614553925
Inouye SK, Bogardus ST Jr, Charpentier PA et al (1999) A multicomponent intervention to prevent delirium in hospitalized older patients. N Engl J Med 340(9):669–676
Rubin FH, Williams JT, Lecisin DA et al (2006) Replicating the hospital elder life program in a community hospital and demonstrating effectiveness using quality improvement methodology. J Amer Geriatr Soc 54:969–974
Caplan GA, Harper E (2007) Recruitment of volunteers to improve vitality in the elderly (The REVIVE Study). Int Med J 37:95–100
Rubin FH, Neal K, Fenlon K, Hassan S, Inouye SK (2011) Sustainability and scalability of the hospital elder life program at a community hospital. J Amer Geriatr Soc 59:359–365
Awissi D-K, Begin C, Moisan J, Lachaine J, Skrobik Y (2012) I-SAVE study: impact of sedation, analgesia, and delirium protocols evaluated in the intensive care unit: an economic evaluation. Ann Pharmacother 46:21–28. https://doi.org/10.1345/aph.1Q284
Zaubler TS, Murphy K, Rizzuto L et al (2013) Quality improvement and cost savings with multicomponent delirium interventions: replication of the hospital elder life program in a community hospital. Psychosomatics 54(3):219–226
Tanajewski L, Franklin M, Gkountouras G et al (2015) Economic evaluation of a general hospital unit for older people with delirium and dementia (TEAM randomised controlled trial). PLoS One 10(12):e0140662. https://doi.org/10.1371/journal.pone.0140662
Fick DM, Kolanowski AM, Walker JL, Inouye SK (2005) Delirium superimposed on dementia in a community-dwelling managed care population: a 3-year retrospective study of occurrence, costs, and utilization. J Gerontol: Med Sci 60A(6):748–753
Markar SR, Smith IA, Karthikesalingam A, Low DE (2013) The clinical and economic costs of delirium after surgical resection for esophageal malignancy. Ann Surg 258:77–81
Zywiel MG, Hurley RT, Perruccio AV et al (2015) Health economic implications of perioperative delirium in older patients after surgery for a fragility hip fracture. J Bone Jt Surg 97(10):829–836. https://doi.org/10.2106/JBJS.N.00724
Brown CH, Laflam A, Max L et al (2016) The impact of delirium after cardiac surgery on postoperative resource utilization. Ann Thorac Surg 101(5):1663–1669. https://doi.org/10.1016/j.athoracsur.2015.12.074
Weinrebe W, Johannsdottir E, Karaman M, Füsgen I (2016) What does delirium cost? An economic evaluation of hyperactive delirium. Z Gerontol Geriat 49:52–58. https://doi.org/10.1007/s00391-015-0871-6
Traube C, Mauer EA, Gerber LM et al (2016) Cost associated with pediatric delirium in the ICU. CCM 44(12):e1175–e1179. https://doi.org/10.1097/CCM.0000000000002004
Tropea J, LoGiudice D, Liew D, Gorelik A, Brand C (2017) Poorer outcomes and greater healthcare costs for hospitalised older people with dementia and delirium: a retrospective cohort study. Int J Geriatr Psychiatry 32:539–547. https://doi.org/10.1002/gps.4491
Ha A, Krasnow RE, Mossanen M et al (2018) A contemporary population-based analysis of the incidence, cost, and outcomes of postoperative delirium following major urologic cancer surgeries. Urol Oncol 36:341e.15–341e.22. https://doi.org/10.1016/j.urolonc.2018.04.012
Vasilevskis EE, Chandrashekhar R, Holtze CH et al (2018) The cost of ICU delirium and coma in the intensive care unit patient. Med Care 56:890–897
Rizzo JA, Bogardus ST, Leo-Summers L et al (2001) Multicomponent targeted intervention to prevent delirium in hospitalized older patients: what is the economic value? Med Care 39(7):740–752
Leslie DL, Zhang Y, Bogardus ST et al (2005) Consequences of preventing delirium in hospitalized older adults on nursing home costs. J Am Geriatri Soc 53:405–409
Leslie DL, Marcantonio ER, Zhang Y, Leo-Summers L, Inouye SK (2008) One-year health care costs associated with delirium in the elderly population. Arch Int Med 168(1):27–32
Hsieh TT, Yang T, Gartaganis SL, Yue J, Inouye SK (2018) Hospital elder life program: systematic review and meta-analysis of effectiveness. Am J Geriatr Psychiatry 26(10):1015–1033
Pezzullo L, Streatfeild J, Hickson J, Teodorczuk A, Agar MR, Caplan GA (2019) The economic impact of delirium in Australia: a cost of illness study. BMJ Open 9:e027514. https://doi.org/10.1136/bmjopen-2018-027514
Lundström M, Edlund A, Bucht G et al (2003) Dementia after delirium in patients with femoral neck fractures. J Am Geriatr Soc 51:1002–1006
Davis DHJ, Muniz Terrera G, Keage H et al (2012) Delirium is a strong risk factor for dementia in the oldest-old: a population-based cohort study. Brain 135:2809–2816
Rockwood K et al (1999) The risk of dementia and death after delirium. Age Ageing 28:551–556
Hsieh TT, Yang T, Gartaganis SL, Yue J, Inouye SK (2018) Hospital elder life program: systematic review and meta-analysis of effectiveness. Am J Ger Psychiatry 26(10):1015–1033
https://www.ato.gov.au/Tax-professionals/TP/Financial-year-ending-30-June-2017/. Accessed 11 Jun 2019
https://data.worldbank.org/indicator/SH.XPD.CHEX.GD.ZS. Accessed 11 Jun 2019
https://www.oecd.org/health/health-systems/International-Comparisons-of-Health-Prices-and-Volumes-New-Findings.pdf. Accessed 27 Jul 2019
Acknowledgements
We acknowledge the support of the Australasian Delirium Association.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Caplan, G.A., Teodorczuk, A., Streatfeild, J. et al. The financial and social costs of delirium. Eur Geriatr Med 11, 105–112 (2020). https://doi.org/10.1007/s41999-019-00257-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-019-00257-2