Abstract
Background
There is little consensus regarding the prevalence and distribution of underlying systemic diseases among patients with pyoderma gangrenosum.
Objective
The objective of this study was to synthesize existing data on the prevalence of associated systemic diseases in patients with pyoderma gangrenosum.
Methods
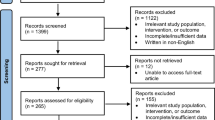
We performed a systematic review and meta-analysis of observational studies in MEDLINE, EMBASE, and Scopus (1823–2017). The quality of evidence was assessed using a modified Newcastle–Ottawa Scale. A meta-analysis was performed using random-effects models to estimate pooled prevalence rates with 95% confidence intervals.
Results
Twenty-one eligible studies comprising 2611 patients with pyoderma gangrenosum were included in the quantitative synthesis. The overall random-effects pooled prevalence of associated systemic diseases was 56.8% (95% confidence interval 45.5–67.4). The leading underlying disease was inflammatory bowel disease (17.6%; 95% confidence interval 13.0–22.7), followed by arthritis (12.8%; 95% confidence interval 9.2–16.9), hematological malignancies (8.9%; 95% confidence interval 6.5–11.6), and solid malignancies (7.4%; 95% confidence interval 5.8–9.1). In 16.3% (95% confidence interval 7.7–27.1) of cases, the onset of pyoderma gangrenosum was attributed to the pathergy phenomenon.
Conclusions
More than half of patients with pyoderma gangrenosum present with a relevant underlying disease. Inflammatory bowel disease and arthritis are the most frequently associated diseases. Relative to the reported literature, the pooled prevalence of arthritis and hematological malignancies is lower, while the pooled prevalence of solid malignancies is higher. Owing to the high level of heterogeneity among most of the comparisons, results should be interpreted with caution.


Similar content being viewed by others
References
Marzano AV, Ishak RS, Saibeni S, Crosti C, Meroni PL, Cugno M. Autoinflammatory skin disorders in inflammatory bowel diseases, pyoderma gangrenosum and Sweet’s syndrome: a comprehensive review and disease classification criteria. Clin Rev Allergy Immunol. 2013;45:202–10.
Marzano AV, Damiani G, Ceccherini I, Berti E, Gattorno M, Cugno M. Autoinflammation in pyoderma gangrenosum and its syndromic form (pyoderma gangrenosum, acne and suppurative hidradenitis). Br J Dermatol. 2017;176:1588–98.
Marzano AV, Fanoni D, Antiga E, Quaglino P, Caproni M, Crosti C, et al. Expression of cytokines, chemokines and other effector molecules in two prototypic autoinflammatory skin diseases, pyoderma gangrenosum and Sweet’s syndrome. Clin Exp Immunol. 2014;178:48–56.
Marzano AV, Cugno M, Trevisan V, Fanoni D, Venegoni L, Berti E, et al. Role of inflammatory cells, cytokines and matrix metalloproteinases in neutrophil-mediated skin diseases. Clin Exp Immunol. 2010;162:100–7.
Braswell SF, Kostopoulos TC, Ortega-Loayza AG. Pathophysiology of pyoderma gangrenosum (PG): an updated review. J Am Acad Dermatol. 2015;73:691–8.
Marzano AV, Borghi A, Meroni PL, Cugno M. Pyoderma gangrenosum and its syndromic forms: evidence for a link with autoinflammation. Br J Dermatol. 2016;175(5):882–91.
Wollina U. Clinical management of pyoderma gangrenosum. Am J Clin Dermatol. 2002;3:149–58.
Maverakis E, Ma C, Shinkai K, Fiorentino D, Callen JP, Wollina U, et al. Diagnostic criteria of ulcerative pyoderma gangrenosum: a Delphi Consensus of International Experts. JAMA Dermatol. 2018. https://doi.org/10.1001/jamadermatol.2017.5980 (epub ahead of print).
Reichrath J, Bens G, Bonowitz A, Tilgen W. Treatment recommendations for pyoderma gangrenosum: an evidence-based review of the literature based on more than 350 patients. J Am Acad Dermatol. 2005;53:273–83.
Hasselmann DO, Bens G, Tilgen W, Reichrath J. Pyoderma gangrenosum: clinical presentation and outcome in 18 cases and review of the literature. J Dtsch Dermatol Ges. 2007;5:560–4.
Al Ghazal P, Körber A, Klode J, Dissemond J. Investigation of new co-factors in 49 patients with pyoderma gangrenosum. Dtsch Dermatol Ges. 2012;10:251–7.
Al Ghazal P, Herberger K, Schaller J, Strölin A, Hoff N-P, Goerge T, et al. Associated factors and comorbidities in patients with pyoderma gangrenosum in Germany: a retrospective multicentric analysis in 259 patients. Orphanet J Rare Dis. 2013;8:136.
Newcombe RG. Two-sided confidence intervals for the single proportion: comparison of seven methods. Stat Med. 1998;17:857–72.
Stang A. Critical evaluation of the Newcastle–Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25:603–5.
Barbosa KGN, de Macedo Bernardino Í, d’Avila S, Ferreira EFE, Ferreira RC. Systematic review and meta-analysis to determine the proportion of maxillofacial trauma resulting from different etiologies among children and adolescents. Oral Maxillofac Surg. 2017;21:131–45.
Hermont AP, Oliveira PA, Martins CC, Paiva SM, Pordeus IA, Auad SM. Tooth erosion and eating disorders: a systematic review and meta-analysis. PLoS One. 2014;9:e111123.
Mlika RB, Riahi I, Fenniche S, Mokni M, Raouf Dhaoui M, Dess N, et al. Pyoderma gangrenosum: a report of 21 cases. Int J Dermatol. 2002;41:65–8.
Cabalag MS, Wasiak J, Lim SW, Raiola FB. Inpatient management of pyoderma gangrenosum: treatments, outcomes, and clinical implications. Ann Plast Surg. 2015;74:354–60.
Powell FC, Schroeter AL, Su WP, Perry HO. Pyoderma gangrenosum: a review of 86 patients. Q J Med. 1985;55:173–86.
Suárez-Pérez JA, Herrera-Acosta E, López-Navarro N, Vilchez-Márquez F, Prieto JD, Bosch RJ, et al. Pyoderma gangrenosum: a report of 15 cases and review of the literature. Actas Dermosifiliogr. 2012;103:120–6.
Marzano AV, Trevisan V, Lazzari R, Crosti C. Pyoderma gangrenosum: study of 21 patients and proposal of a “clinicotherapeutic” classification. J Dermatolog Treat. 2011;22:254–60.
Pereira N, Brites MM, Goncalo M, Tellechea O, Figueiredo A. Pyoderma gangrenosum: a review of 24 cases observed over 10 years. Int J Dermatol. 2013;52:938–45.
Bennett ML, Jackson JM, Jorizzo JL, Fleischer AB Jr, White WL, Callen JP. Pyoderma gangrenosum: a comparison of typical and atypical forms with an emphasis on time to remission. Case review of 86 patients from 2 institutions. Medicine (Baltimore). 2000;79:37–46.
Inoue S, Furuta JI, Fujisawa Y, Onizawa S, Ito S, Sakiyama M, et al. Pyoderma gangrenosum and underlying diseases in Japanese patients: a regional long-term study. J Dermatol. 2017;44:1281–4.
Binus AM, Qureshi AA, Li VW, Winterfield LS. Pyoderma gangrenosum: a retrospective review of patient characteristics, comorbidities and therapy in 103 patients. Br J Dermatol. 2011;165:1244–50.
Jockenhöfer F, Herberger K, Schaller J, Hohaus KC, Stoffels-Weindorf M, Ghazal PA, et al. Tricenter analysis of cofactors and comorbidity in patients with pyoderma gangrenosum. J Dtsch Dermatol Ges. 2016;14:1023–30.
Langan SM, Groves RW, Card TR, Gulliford MC. Incidence, mortality, and disease associations of pyoderma gangrenosum in the United Kingdom: a retrospective cohort study. J Invest Dermatol. 2012;132:2166–70.
Jockenhofer F, Klode J, Kroger K, Roesch A, Al Ghazal P, Dissemond J. Patients with pyoderma gangrenosum: analyses of the German DRG data from 2012. Int Wound J. 2016;13:951–6.
Vidal D, Puig L, Gilaberte M, Alomar A. Review of 26 cases of classical pyoderma gangrenosum: clinical and therapeutic features. J Dermatolog Treat. 2004;15:146–52.
Von Den Driesch P. Pyoderma gangrenosum: a report of 44 cases with follow-up. Br J Dermatol. 1997;137:1000–5.
Ye MJ, Ye JM. Pyoderma gangrenosum: a review of clinical features and outcomes of 23 cases requiring inpatient management. Dermatol Res Pract. 2014;2014:461467.
Saracino A, Kelly R, Liew D, Chong A. Pyoderma gangrenosum requiring inpatient management: a report of 26 cases with follow up. Australas J Dermatol. 2011;52:218–21.
Vacas AS, Torre AC, Bollea-Garlatti ML, Warley F, Galimberti RL. Pyoderma gangrenosum: clinical characteristics, associated diseases, and responses to treatment in a retrospective cohort study of 31 patients. Int J Dermatol. 2017;56:386–91.
Callen JP, Jackson JM. Pyoderma gangrenosum: an update. Rheum Dis Clin North Am. 2007;33:787–802.
Jackson JM, Callen JP. Pyoderma gangrenosum: an expert commentary. Expert Rev. Dermatol. 2006;1:391–400.
Davis MDP, Moschella SL. Neutrophilic dermatoses. In: Bolognia J, Schaffer J, Cerroni L, editors. Dermatology. 4th ed. Philadelphia; Elsevier; 2017. p. 453–71.
Wolff K, Stingl G. Pyoderma gangrenosum. In: Freedberg I, Eisen A, Wolff K, editors. Fitzpatrick’s dermatology in general medicine. 5th ed. New York (NY): McGraw-Hill; 1999. p. 2207–13.
Jackson JM, Callen JP. Pyoderma gangrenosum: background, epidemiology, prognosis. 2017. Available from: https://emedicine.medscape.com/article/1123821-overview. Accessed 20 Dec 2017.
Adisen E, Erduran F, Gurer MA. Pyoderma gangrenosum: a report of 27 patients. Int J Low Extrem Wounds. 2016;15:148–54.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for the conduct of this study or the preparation of this article.
Conflict of interest
Khalaf Kridin, Arnon D. Cohen, and Kyle T. Amber have no conflicts of interest directly relevant to the content of this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kridin, K., Cohen, A.D. & Amber, K.T. Underlying Systemic Diseases in Pyoderma Gangrenosum: A Systematic Review and Meta-Analysis. Am J Clin Dermatol 19, 479–487 (2018). https://doi.org/10.1007/s40257-018-0356-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40257-018-0356-7