Abstract
Introduction
Azithromycin, a broad-spectrum antibiotic with potent anti-inflammatory activities, has the potential to effectively treat blepharitis, an inflammatory disease of the eyelid with abnormal eyelid flora as an etiologic determinant. The present study compared the efficacy of topical azithromycin ophthalmic solution 1% (AzaSite®; Inspire Pharmaceuticals, Inc, NC, USA) combined with warm compresses (azithromycin group) to warm compresses alone (compress group) in patients with posterior blepharitis.
Methods
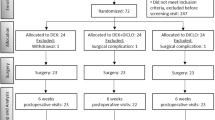
Twenty-one patients diagnosed with posterior blepharitis were randomized in an open-label study to receive either azithromycin plus warm compresses (10 patients), or compresses alone (11 patients). All patients were instructed to apply compresses to each eye for 5–10 minutes twice daily for 14 days. Each eye in the azithromycin group also received azithromycin solution (1 drop) twice daily for the first 2 days followed by once daily for the next 12 days. Patients were evaluated at study initiation (visit 1) and at end of treatment (visit 2) for the severity of five clinical signs: eyelid debris, eyelid redness, eyelid swelling, meibomian gland (MG) plugging, and the quality of MG secretion. At visit 2, patients also rated their degree of overall symptomatic relief.
Results
Twenty patients completed the study. At visit 2, patients in the azithromycin group demonstrated significant improvements in MG plugging, MG secretions, and eyelid redness as compared with the compress group. In the azithromycin group, MG plugging resolved completely in three patients and MG secretion returned to normal in two patients; no such results were seen in the compress group. Furthermore, a higher percentage of patients in the azithromycin group rated overall symptomatic relief as excellent or good. Visual acuity measurements and biomicroscopic evaluation revealed no ocular safety issues.
Conclusion
Azithromycin ophthalmic solution in combination with warm compresses provided a significantly greater clinical benefit than warm compresses alone in treating the signs and symptoms of posterior blepharitis.
Similar content being viewed by others
References
Jackson WB. Blepharitis: current strategies for diagnosis and management. Can J Ophthalmol. 2008;43:170–179.
Smith RE, Flowers CW Jr. Chronic blepharitis: a review. CLAO J. 1995;21:200–207.
Foulks GN, Bron AJ. Meibomian gland dysfunction: a clinical scheme for description, diagnosis, classification, and grading. Ocul Surf. 2003;1:107–126.
McCulley JP, Dougherty JM. Bacterial aspects of chronic blepharitis. Trans Ophthalmol Soc U K. 1986;105:314–318.
Dougherty JM, McCulley JP. Comparative bacteriology of chronic blepharitis. Br J Ophthalmol. 1984;68:524–528.
Dougherty JM, McCulley JP. Bacterial lipases and chronic blepharitis. Invest Ophthalmol Vis Sci. 1986;27:486–491.
Seal D, Ficker L, Ramakrishnan M, Wright P. Role of staphylococcal toxin production in blepharitis. Ophthalmology. 1990;97:1684–1688.
Mondino BJ, Caster AI, Dethlefs B. A rabbit model of staphylococcal blepharitis. Arch Ophthalmol. 1987;105:409–412.
Ficker L, Ramakrishnan M, Seal D, Wright P. Role of cell-mediated immunity to staphylococci in blepharitis. Am J Ophthalmol. 1991;111:473–479.
Yanoff M, Fine B. Ocular Pathology. Philadelphia, PA: J. B. Lippincott; 1989.
Friedlaender MH, Protzko E. Clinical development of 1% azithromycin in DuraSite, a topical azalide anti-infective for ocular surface therapy. Clin Ophthalmol. 2007;1:3–10.
Amsden GW. Anti-inflammatory effects of macrolides—an underappreciated benefit in the treatment of community-acquired respiratory tract infections and chronic inflammatory pulmonary conditions? J Antimicrob Chemother. 2005;55:10–21.
Giamarellos-Bourboulis EJ. Macrolides beyond the conventional antimicrobials: a class of potent immunomodulators. Int J Antimicrob Agents. 2008;31:12–20.
Culic O, Erakovic V, Cepelak I, et al. Azithromycin modulates neutrophil function and circulating inflammatory mediators in healthy human subjects. Eur J Pharmacol. 2002;450:277–289.
Ferris FL 3rd, Kassoff A, Bresnick GH, Bailey I. New visual acuity charts for clinical research. Am J Ophthalmol. 1982;94:91–96.
Early Treatment Diabetic Retinopathy Study Research Group. Early treatment diabetic retinopathy study design and baseline patient characteristics. ETDRS report number 7. Ophthalmology. 1991;98:741–756.
Smith K, Leyden JJ. Safety of doxycycline and minocycline: a systematic review. Clin Ther. 2005;27:1329–1342.
Groden LR, Murphy B, Rodnite J, Genvert GI. Lid flora in blepharitis. Cornea. 1991;10:50–53.
Seal DV, McGill JI, Jacobs P, Liakos GM, Goulding NJ. Microbial and immunological investigations of chronic non-ulcerative blepharitis and meibomianitis. Br J Ophthalmol. 1985;69:604–611.
Bron AJ, Tiffany JM. The contribution of meibomian disease to dry eye. Ocul Surf. 2004;2:149–165.
McCulley JP, Shine WE. The lipid layer of tears: dependent on meibomian gland function. Exp Eye Res. 2004;78:361–365.
Song PI, Abraham TA, Park Y, et al. The expression of functional LPS receptor proteins CD14 and toll-like receptor 4 in human corneal cells. Invest Ophthalmol Vis Sci. 2001;42:2867–2877.
Dougherty JM, McCulley JP, Silvany RE, Meyer DR. The role of tetracycline in chronic blepharitis. Inhibition of lipase production in staphylococci. Invest Ophthalmol Vis Sci. 1991;32:2970–2975.
Yoon KC, Jeong IY, Park YG, Yang SY. Interleukin-6 and tumor necrosis factoralpha levels in tears of patients with dry eye syndrome. Cornea. 2007;26:431–437.
Barton K, Monroy DC, Nava A, Pflugfelder SC. Inflammatory cytokines in the tears of patients with ocular rosacea. Ophthalmology. 1997;104:1868–1874.
Solomon A, Dursun D, Liu Z, Xie Y, Macri A, Pflugfelder SC. Pro-and anti-inflammatory forms of interleukin-1 in the tear fluid and conjunctiva of patients with dry-eye disease. Invest Ophthalmol Vis Sci. 2001;42:2283–2292.
Afonso AA, Sobrin L, Monroy DC, Selzer M, Lokeshwar B, Pflugfelder SC. Tear fluid gelatinase B activity correlates with IL-1alpha concentration and fluorescein clearance in ocular rosacea. Invest Ophthalmol Vis Sci. 1999;40:2506–2512.
Perry HD, Doshi-Carnevale S, Donnenfeld ED, Solomon R, Biser SA, Bloom AH. Efficacy of commercially available topical cyclosporine A 0.05% in the treatment of meibomian gland dysfunction. Cornea. 2006;25:171–175.
Rubin M, Rao SN. Efficacy of topical cyclosporin 0.05% in the treatment of posterior blepharitis. J Ocul Pharmacol Ther. 2006;22:47–53.
Kunert KS, Tisdale AS, Stern ME, Smith JA, Gipson IK. Analysis of topical cyclosporine treatment of patients with dry eye syndrome: effect on conjunctival lymphocytes. Arch Ophthalmol. 2000;118:1489–1496.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Luchs, J. Efficacy of topical azithromycin ophthalmic solution 1% in the treatment of posterior blepharitis. Adv Therapy 25, 858–870 (2008). https://doi.org/10.1007/s12325-008-0096-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-008-0096-9