Abstract
Background
Elongation in patients with achondroplasia provides better overall skeletal proportionality and significantly improves such individuals’ access to their perineal region to self-manage personal hygiene. This paper describes our surgical technique and outcomes for bilateral humeral lengthening in achondroplasia patients over 26 years.
Methods
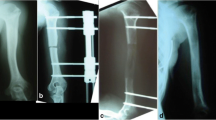
Ours was a retrospective study of 55 patients with achondroplasia-related short stature, in whom bilateral humeral lengthening was performed from 1990 to 2016. We describe the surgical technique and analyze mean gain in humeral length, days using an external fixator, mean percentage of lengthening, external fixation index, type of callus, and complications. Pre- and postoperative radiographic measurements were obtained. Patients also were contacted by telephone and asked about their ability to perform peri-anal self-hygiene and about their overall satisfaction.
Results
In total, 110 humeri were lengthened (28 males and 27 females) with medium elongation of 9.5 cm on the right and 9.6 cm on the left, while averaging 220 days in an external fixator. We observed 14 minor complications. There was no significant association between pin position and type of callus, and elongation most often external and in the presence of a straight callus. Before elongation, 77.1% of patients reported difficulties with perineal hygiene and 85.4% could not put their hands in their pockets. Upon completion of lengthening, 100% could perform both tasks and 94.5% were very satisfied.
Conclusions
Bilateral humeral elongation yields significant improvements in patient autonomy, with a relatively low complication rate and very high patient satisfaction.


Similar content being viewed by others
References
Horton WA, Hall JG, Hecht JT (2007) Achondroplasia. Lancet Lond Engl 370(9582):162–172
Kitoh H, Kitakoji T, Kurita K, Katoh M, Takamine Y (2002) Deformities of the elbow in achondroplasia. J Bone Joint Surg Br 84(5):680–683
Damsin JP, Ghanem I (2000) Upper limb lengthening. Hand Clin 16(4):685–701
Kashiwagi N, Suzuki S, Seto Y, Futami T (2001) Bilateral humeral lengthening in achondroplasia. Clin Orthop 391:251–257
Vilarrubias JM, Ginebreda I, Fernandez-Fairen M (1988) 500 cases of lower limb lengthening using a personal technic in achondroplasia. Acta Orthop Belg 54(4):384–390
Cai G, Yang L, Saleh M, Coulton L (2007) The effect of tibial diaphyseal lengthening on the longitudinal growth of the tibia. J Pediatr Orthop Part B 16(6):403–407
Paley D (1988) Current techniques of limb lengthening. J Pediatr Orthop 8(1):73–92
Cattaneo R, Villa A, Catagni M, Tentori L (1988) Strategies for limb lengthening in achondroplasia using the Ilizarov method–the experience of the hospital of Lecco, Italy. Basic Life Sci 48:381–388
Shadi M, Musielak B, Koczewski P, Janusz P (2018) Humeral lengthening in patients with achondroplasia and in patients with post-septic shortening: comparison of procedure efficiency and safety. Int Orthop 42(2):419–426
Hamanishi C, Yasuwaki Y, Kikuchi H, Tanaka S, Tamura K (1992) Classification of the callus in limb lengthening. Radiographic study of 35 limbs. Acta Orthop Scand 63(4):430–433
Paley D (1990) Problems, obstacles, and complications of limb lengthening by the Ilizarov technique. Clin Orthop 250:81–104
Yasui N, Kawabata H, Kojimoto H, Ohno H, Matsuda S, Araki N et al (1997) Lengthening of the lower limbs in patients with achondroplasia and hypochondroplasia. Clin Orthop 344:298–306
Malot R, Park K-W, Song S-H, Kwon H-N, Song H-R (2013) Role of hybrid monolateral fixators in managing humeral length and deformity correction. Acta Orthop 84(3):280–285
McLawhorn AS, Sherman SL, Blyakher A, Widmann RF (2011) Humeral lengthening and deformity correction with the multiaxial correction system. J Pediatr Orthop Part B 20(2):111–116
Hosny GA (2016) Humeral lengthening and deformity correction. J Child Orthop 10(6):585–592
Kim S-J, Agashe MV, Song S-H, Choi H-J, Lee H, Song H-R (2012) Comparison between upper and lower limb lengthening in patients with achondroplasia: a retrospective study. J Bone Joint Surg Br 94(1):128–133
Nakano-Matsuoka N, Fukiage K, Harada Y, Kashiwagi N, Futami T (2017) The prevalence of the complications and their associated factors in humeral lengthening for achondroplasia: retrospective study of 54 cases. J Pediatr Orthop B 26(6):519–525
Kiss S, Pap K, Vízkelety T, Terebessy T, Balla M, Szőke G (2008) The humerus is the best place for bone lengthening. Int Orthop 32(3):385–388
Kitoh H, Mishima K, Matsushita M, Nishida Y, Ishiguro N (2014) Early and late fracture following extensive limb lengthening in patients with achondroplasia and hypochondroplasia. Bone Jt J 96–B(9):1269–1273
Lee FY-I, Schoeb JS, Yu J, Christiansen BD, Dick HM (2005) Operative lengthening of the humerus: indications, benefits, and complications. J Pediatr Orthop 25(5):613–616
Funding
This research received no specific grants from any funding agency in the public, commercial, or not-for-profit sectors. Neither of the authors, their immediate family, nor any research foundation with which they are affiliated have received any financial payments or other benefits from any commercial entity related to the subject of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Hospital ethics committee approval was obtained by the ‘Comité de Etica Asistencial Hospital Quiron Salud.’
Informed consent
Informed consent was obtained from parents/LAR of all participants included in the study.
Rights and permissions
About this article
Cite this article
Ginebreda, I., Campillo-Recio, D., Cárdenas, C. et al. Surgical technique and outcomes for bilateral humeral lengthening for achondroplasia: 26-year experience. Musculoskelet Surg 103, 257–262 (2019). https://doi.org/10.1007/s12306-018-0583-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-018-0583-3