Abstract
Purpose
Breast cancer patients (BCP) are at risk of female sexual dysfunction (FSD). Our aim was to clarify the effects of treatment strategies, and steroid hormones levels on FSD.
Methods
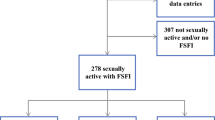
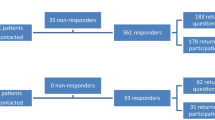
We enrolled 136 BCP (46.9 ± 0.8 years), and 122 completed questionnaires. BCP were divided into four groups: 22 women with advanced breast cancer on neoadjuvant therapy (NAT), 48 on adjuvant therapy (AT), 30 taking hormonal therapy (HT) and 22 with metastatic cancer on first line chemotherapy (FLT). Fifty-eight healthy women (43 ± 2.8 years) were enrolled as controls. FSD was evaluated by FSFI, and sexual distress was assessed with FSDS-R. We have collected demographic data, laboratory values, and LH, FSH, total testosterone (T), and estradiol (E2) levels.
Results
BCP showed a prevalence of FSD of 69%, total FSFI score was 17. FSDS-R was 8.3. FSD had a prevalence of 72 % in NAT, 65% in AT, 77% in metastatic BCP under FLT, 67% in HT, compared with a prevalence of 20% in controls. BCP showed lower E2 than normal values, as well as T. LH and FSH were significantly elevated than normal values. Total FSFI score was positively correlated with T in 122 BCP, no significant correlation was found between E2 and FSFI. Significant differences were found between NAT and HT in lubrication, pain domains and total FSDS-R score, AT and HT in pain domain, AT and NAT in lubrication domain.
Conclusions
BCP are at high risk of developing FSD both for treatment choice and hormonal status, but they have not sexually related personal distress.



Similar content being viewed by others
References
D.M. Conde, A.M. Pinto-Neto, C. Cabello, D. Santos-Sá, L. Costa-Paiva, E.Z. Martinez, Quality of life in Brazilian breast cancer survivors age 45-65 years: associated factors. Breast J. 11(6), 425–432 (2005)
American Cancer Society. Cancer Facts & Figures 2015. (Atlanta: American Cancer Society 2015)
S.L. Bober, J. Carter, S. Falk, Addressing female sexual function after cancer by internists and primary care providers. J. Sex. Med 10(Suppl 1), 112–119 (2013)
E. Gilbert, J.M. Ussher, J. Perz, Sexuality after breast cancer: a review. Maturitas 66(4), 397–407 (2010)
M.I. Maiorino, P. Chiodini, G. Bellastella, D. Giugliano, K. Esposito, Sexual dysfunction in women with cancer: a systematic review with meta-analysis of studies using the Female Sexual Function Index. Endocrine 54(2), 329–341 (2016)
J. Knapp, Sexual function as a quality of life issue: the impact of breast cancer treatment. J. Gynecol. Oncol. Nurs. 7, 37–40 (1997)
P. Fobair, D. Spiegel, Concerns about sexuality after breast cancer. Cancer J. 15(1), 19–26 (2009)
K. Abbott-Anderson, K.L. Kwekkeboom, A systematic review of sexual concerns reported by gynecological cancer survivors. Gynecol. Oncol. 124, 477–489 (2011)
S. Rajan, J. Foreman, M.G. Wallis, C. Caldas, P. Britton, Multidisciplinary decisions in breast cancer: does the patient receive what the team has recommended? Br. J. Cancer 108(12), 2442–2447 (2013)
I. Harirchi, A. Montazeri, F. Zamani Bidokhti, N. Mamishi, K. Zendehdel, Sexual function in breast cancer patients: a prospective study from Iran. J. Exp. Clin. Cancer Res. 31, 20–26 (2012)
J.A. Cavalheiro, A. Bittelbrunn, C.H. Menke, J.V. Biazús, N.L. Xavier, R. Cericatto, F. Schuh, C.V. Pinheiro, E.P. Passos, Sexual function and chemotherapy in postmenopausal women with breast cancer. BMC Women’s. Health 12, 28 (2012)
R. Rosen, C. Brown, J. Heiman, S. Leiblum, C. Meston, R. Shabsigh, D. Ferguson, R. D’Agostino, The Female Sexual Function Index (FSFI): A multidimensional self-report instrument for the assessment of female sexual function. J. Sex Marital Ther. 26, 191–208 (2000)
L. Derogatis, A. Clayton, D. Lewis-D’Agostino, G. Wunderlich, Y. Fu, Validation of the female sexual distress scale-revised for assessing distress in women with hypoactive sexual desire disorder. J. Sex. Med. 5, 357–364 (2008)
G. Accardo, G. Vallone, D. Esposito, F. Barbato, A. Renzullo, G. Conzo, G. Docimo, K. Esposito, D. Pasquali, Testicular parenchymal abnormalities in Klinefelter syndrome: a question of cancer? Examination of 40 consecutive patients. Asian J. Androl. 17(1), 154–158 (2015)
J.M. Ussher, J. Perz, E. Gilbert, Information needs associated with changes to sexual well-being after breast cancer. J. Adv. Nurs. 69(2), 327–337 (2013)
I. Bartula, K.A. Sherman, The Female Sexual Functioning Index (FSFI): evaluation of acceptability, reliability, and validity in women with breast cancer. Support. Care Cancer 23(9), 2633–2641 (2015)
M. Krychman, L.S. Millheiser, Sexual health issues in women with cancer. J. Sex. Med. Suppl 1, 5–15 (2013)
S. Keesing, L. Rosenwax, B. McNamara, A dyadic approach to understanding the impact of breast cancer on relationships between partners during early survivorship. BMC Women’s Health 16, 57 (2016)
A.J. Carroll, S.R. Baron, R.A. Carroll, Couple-based treatment for sexual problems following breast cancer: A review and synthesis of the literature. Support. Care Cancer 24(8), 3651–3659 (2016)
V. Pumo, G. Milone, M. Iacono, S.R. Giuliano, A. Di Mari, C. Lopiano, S. Bordonaro, P. Tralongo, Psychological and sexual disorders in long-term breast cancer survivors. Cancer Manag. Res. 4, 61–65 (2012)
J. Farthmann, A. Hanjalic-Beck, J. Veit, B. Rautenberg, E. Stickeler, T. Erbes, M. Földi, A. Hasenburg, The impact of chemotherapy for breast cancer on sexual function and health-related quality of life. Support. Care Cancer 24(6), 2603–2609 (2016)
M.F. Tiezzi, J.M. de Andrade, A.P. Romão, D.G. Tiezzi, M.R. Lerri, H.A. Carrara, L.A. Lara, Quality of life in women with breast cancer treated with or without chemotherapy. Cancer Nurs. 48, 37 (2016)
J.J. Speer, B. Hillenberg, D.P. Sugrue, C. Blacker, C.L. Kresge, V.B. Decker, D. Zakalik, D.A. Decker, Study of sexual functioning determinants in breast cancer survivors. Breast J. 11(6), 440–447 (2005)
M. Moegele, S. Buchholz, S. Seitz, O. Ortmann, Vaginal estrogen therapy in postmenopausal breast cancer patients treated with aromatase inhibitors. Arch. Gynecol. Obstet. 285(5), 1397–1402 (2012)
M. Dahir, D. Travers-Gustafson, Breast cancer, aromatase inhibitor therapy, and sexual functioning: a pilot study of the effects of vaginal testosterone therapy. Sex. Med. 2(1), 8–15 (2014)
S. Witherby, J. Johnson, L. Demers, S. Mount, B. Littenberg, C.D. Maclean, M. Wood, H. Muss, Topical testosterone for breast cancer patients with vaginal atrophy related to aromatase inhibitors: a phase I/II study. Oncologist 16(4), 424–431 (2011)
D. Barton, J.A. Sloan, L.T. Shuster, P. Gill, J.D. Bearden, D.B. Johnson, P.J. Stella, S.A. Terstriep, F.N. Rana, D.M. Anderson, C.L. Loprinz, Impact of vaginal dehydroepiandosterone (DHEA) on vaginal symptoms in female breast cancer survivors: Trial N10C1 (Alliance). J. Clin. Oncol. 32, 5s (2014)
S. Pruthi, J.A. Simon, A.P. Early, Current overview of the management of urogenital atrophy in women with breast cancer. Breast J. 17(4), 403–408 (2011)
M.L. Krychman, A. Katz, Breast cancer and sexuality: multi-modal treatment options. J. Sex. Med. 9(1), 5–13 (2012)
B. Candy, L. Jones, V. Vickerstaff, A. Tookman, M. King, Interventions for sexual dysfunction following treatments for cancer in women. Cochrane Database Syst. Rev. (2016) https://doi.org/10.1002/14651858.CD005540
S.R. Davis, S. Wahlin-Jacobsen, Testosterone in women-the clinical significance. Lancet Diabetes Endocrinol. 3(12), 980–992 (2015)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Gambardella, A., Esposito, D., Accardo, G. et al. Sexual function and sex hormones in breast cancer patients. Endocrine 60, 510–515 (2018). https://doi.org/10.1007/s12020-017-1470-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1470-7