Abstract
Background
Treatment decisions about menopause are predicated on a transient duration of vasomotor symptoms. However, evidence supporting a specific duration is weak.
Objective
To estimate the natural progression of vasomotor symptoms during the menopause transition by systematically compiling available evidence using meta-analytic techniques.
Data Sources
We searched MEDLINE, hand searched secondary references in relevant studies, book chapters, and review papers, and contacted investigators about relevant published research.
Review Methods
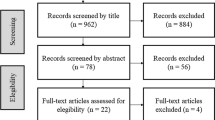
English language, population-based studies reporting vasomotor symptom prevalence among women in menopausal transition in time intervals based on years to or from final menstrual period were included. Two reviewers independently assessed eligibility and quality of studies and extracted data for vasomotor symptom prevalence.
Results
The analyses included 10 studies (2 longitudinal, 8 cross sectional) with 35,445 participants. The percentage of women experiencing symptoms increased sharply in the 2 years before final menstrual period, peaked 1 year after final menstrual period, and did not return to premenopausal levels until about 8 years after final menstrual period. Nearly 50% of all women reported vasomotor symptoms 4 years after final menstrual period, and 10% of all women reported symptoms as far as 12 years after final menstrual period. When data were examined according to symptom severity (‘any’ vs. ‘bothersome’), bothersome symptoms peaked about 1 year earlier and declined more rapidly than symptoms of any severity level.
Conclusions
Our findings suggest a median symptom duration of about 4 years among symptomatic women. A longer symptom duration may affect treatment decisions and clinical guidelines. Further prospective, longitudinal studies of menopausal symptoms should be conducted to confirm these results.




Similar content being viewed by others
References
McKinlay SM, Brambilla DJ, Posner JG. The normal menopause transition. Maturitas. 1992;14(2):103–15.
Guthrie J, Dennerstein L, Taffe J, Donnelly V. Health care-seeking for menopausal problems. Climacteric. 2003;6(2):112–7.
Lobo R (ed). Treatment of the postmenopausal woman: Basic and clinical aspects.: Academic Press; 2007.
Medical Knowledge Self Assessment Program 14. 2007.
North American Menopause Society. Treatment of menopause-associated vasomotor symptoms: Position statement of The North American Menopause Society. Menopause. 2004;11:11–33.
Kronenberg F. Hot flashes: epidemiology and physiology. Ann N Y Acad Sci. 1990;592:52–86. discussion 123–33.
Col NF. The impact of risk status, preexisting morbidity, and polypharmacy on treatment decisions concerning menopausal symptoms. Am J Med. 2005;118(12 Suppl 2):155–62.
Rossouw JE, Prentice RL, Manson JE, et al. Postmenopausal hormone therapy and risk of cardiovascular disease by age and years since menopause. JAMA. 2007;297(13):1465–77.
Women’s Health Initiative. Scientific Resources Website. Vol. 2006.
Grodstein F, Clarkson TB, Manson JE. Understanding the divergent data on postmenopausal hormone therapy. The New England Journal of Medicine. 2003;348(7):645–50.
American College of Obstetricians and Gynecologists. Executive Summary. Hormone Therapy. Obstetrics & Gynecology. 2004;104:1S.
Mosca L, Collins P, Herrington DM, et al. Hormone Replacement Therapy and cardiovascular disease: A statement for healthcare professionals from the American Heart Association. Circulation. 2001;104:499–503.
Grady D. Management of menopausal symptoms. The New England Journal of Medicine. 2006;355(22):2338–47.
National Institute of Health. NIH State-of-the-Science conference on management of menopause-related symptoms. Vol. 2005; 2005.
Woods NF, Mitchell ES. Symptoms during the perimenopause: Prevalence, severity, trajectory, and significance in women’s lives. Am J Med. 2005;118(12B):14S–24S.
Medical Women’s Federation. An investigation of the menopause in one thousand women. The Lancet. 1933:106–108.
Feldman BM, Voda A, Gronseth E. The prevalence of hot flash and associated variables among perimenopausal women. Res Nurs Health. 1985;8(3):261–8.
Kronenberg F. Hot Flashes. New York: Raven Press, Ltd.; 1994:97.
Association for Healthcare Research and Quality. Evidence report/Technology assessment: Management of menopause-related symptoms. Vol. 2005; 2005.
Wells GA, Shea B, O’Connell D, et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2000.
McKinlay SM, Jefferys M. The menopausal syndrome. Br J Prev Soc Med. 1974;28(2):108–15.
Oldenhave A, Jaszmann LJ, Haspels AA, Everaerd WT. Impact of climacteric on well-being. A survey based on 5213 women 39 to 60 years old. Am J Obstet Gynecol. 1993;168(3 Pt 1):772–80.
Thompson B, Hart SA, Durno D. Menopausal age and symptomatology in a general practice. J Biosoc Sci. 1973;5(1):71–82.
Berg G, Gottwall T, Hammar M, Lindgren R. Climacteric symptoms among women aged 60–62 in Linkoping, Sweden, in 1986. Maturitas. 1988;10(3):193–9.
Nedstrand E, Pertl J, Hammar M. Climacteric symptoms in a postmenopausal Czech population. Maturitas. 1996;23(1):85–9.
Avis NE, Brockwell S, Colvin A. A universal menopausal syndrome? Am J Med. 2005;118(12 Suppl 2):37–46.
Brown WJ, Mishra GD, Dobson A. Changes in physical symptoms during the menopause transition. Int J Behav Med. 2002;9(1):53–67.
Groenveld FPMJ, Bareman FP, Barentsen , Dokter HJ, Drogendijk AC, Hoes AW. Vasomotor symptoms and the well–being in the climacteric years. Maturitas. 1996;23:293–9.
Melby MK. Vasomotor symptom prevalence and language of menopause in Japan. Menopause: The Journal of the North American Menopause Society. 2005;12(3):250–7.
Soules M, Sherman S, Parrott E, et al. Executive summary: Stages of Reproductive Aging Workshop (STRAW). Climacteric. 2001;4(4):267–72.
Genazzani A, Nicolucci A, Campagnoli C, et al. Validation of Italian version of the Women’s Health Questionnaire: Assessment of quality of life of women from the general population and those attending menopause centers. Climacteric. 2002;5:70–7.
Binfa L, Castelo-Branco C, Blumel JE, et al. Influence of psychosocial factors on climacteric symptoms. Maturitas. 2004;48:425–31.
Travers C, O’Neill SM, King , Battistutta D, Khoo SK. Greene Climacteric Scale: Norms in an Australian population in relation to age and menopausal status. Climacteric. 2005;8:56–62.
Ford K, Sowers MF, Crutchfield M, Wilson A, Jannausch M. A longitudinal study of the predictors of prevalence and severity of symptoms commonly associated with menopause. Menopause: The Journal of the North American Menopause Society. 2005;12(3):308–17.
Stroup DF, Berlin JA, Morton SC, et al. Meta analysis of observational studies in epidemiology: A proposal for reporting. JAMA. 2000;283(15):2008–20012.
Lau J. Metaanalyst. Boston, MA, US.
DerSimonian , Laird N. Meta-analysis in Clinical Trials. Control Clin Trials. 1986;7:177–88.
Kaufert P, Syrotuik J. Symptom reporting at the menopause. Soc Sci Med. 1981;15(3):173–84.
Hunter M. The south-east England longitudinal study of the climacteric and postmenopause. Maturitas. 1992;14(2):117–26.
Bardel A, Wallander M-A, Svardsudd K. Hormone replacement therapy and symptom reporting in menopausal women. A population-based study of 35–65 year old women in mid-Sweden. Maturitas. 2002;41:7–15.
Overlie I, Finset A, Holte A. Gendered personality dispositions, hormone values, and hot flushes during and after menopause. J Psychosom Obstet Gynaecol. 2002;23:219–27.
Keenan NL, Mark S, Fugh-Berman A, Browne D, Kaczmarczyk J, Hunter C. Severity of menopausal symptoms and use of both conventional and complementary/alternative therapies. Menopause: The Journal of the North American Menopause Society. 2003;10(6):507–15.
Juang KD, Wang SJ, Lu S, Lee SJ, Fuh JL. Hot flashes are associated with psychological symptoms of anxiety and depression in peri- and post- but not premenopausal women. Maturitas. 2005;52(2):119–26.
Kumari M, Stafford M, Marmot M. The menopausal transition was associated in a prospective study with decreased health functioning in women who report menopausal symptoms. J Clin Epidemiol. 2005;58(7):719–27.
Miller S, Gallicchio LM, Lewis LM, et al. Association between race and hot flashes in midlife women. Maturitas. 2006;54:260–9.
Sievert LL, Obermeyer CM, Price K. Determinants of hot flashes and night sweats. Ann Hum Biol. 2006;33(1):4–16.
Huang AJ, Grady DG, Blackwell TL, Bauer DC, Sawaya GF. Persistent hot flashes in older postmenopausal women (abstract). J Gen Intern Med. 2007;22(suppl 1):168.
Guthrie J, Dennerstein L, Taffe J, Lehert P, Burger HG. Hot flushes during the menopause transition: a longitudinal study in Australian-born women. Menopause. 2005;12(4):460–7.
Warren MP. Historical perspectives in postmenopausal hormone therapy: Defining the right dose and duration. Mayo Clinic Proceedings. 2007;82(2):219–26.
Gold EB, Sternfeld B, Kelsey JL, et al. Relation of demographic and lifestyle factors to symptoms in a multi-racial/ethnic population of women 40–55 years of age. Am J Epidemiol. 2000;152(5):463–73.
Avis NE, Crawford SL, McKinlay SM. Psychosocial, behavioral, and health factors related to menopause symptomatology. Womens Health. 1997;3(2):103–20.
Avis NE, Stellato , Crawford S, et al. Is there a menopausal syndrome? Menopausal status and symptoms across racial/ethnic groups. Soc Sci Med. 2001;52(3):345–56.
Avis NE, Zhao X, Johannes CB, Ory M, Brockwell S, Greendale GA. Correlates of sexual function among multi-ethnic middle-aged women: results from the Study of Women’s Health Across the Nation (SWAN). Menopause. 2005;12(4):385–98.
Acknowledgements
This work was supported by the Agency for Healthcare, Research, and Quality (AHRQ) 2R01 HS013329-04A1. An earlier version was presented at the Society for Medical Decision Making Annual Meeting, October 2007. We would like to thank Nancy Avis, Ph.D. (Department of Public Health Sciences, Wake Forest University School of Medicine, Winston-Salem, NC), Janet Guthrie, M.Sc., Dip. Ed, Ph.D. (Center for Women’s Health, University of Melbourne, Australia), and Martha Hickey, M.D. (School of Women’s and Infants’ Health, University of Western Australia, Australia) for their thoughtful reviews of this manuscript.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix A
Quality assessment based on the Newcastle-Ottawa Quality Assessment Scale
Appendix B
Characteristics of studies with vague menopausal staging criteria
Rights and permissions
About this article
Cite this article
Politi, M.C., Schleinitz, M.D. & Col, N.F. Revisiting the Duration of Vasomotor Symptoms of Menopause: A Meta-Analysis. J GEN INTERN MED 23, 1507–1513 (2008). https://doi.org/10.1007/s11606-008-0655-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-008-0655-4