Abstract
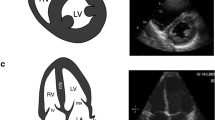
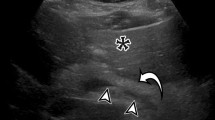
Interest in transthoracic ultrasound (US) procedures increased after the availability of portable US equipment suitable for use at the patient’s bedside. It is possible to detect space-occupying lesions of the pleura, pleural effusion, focal or diffuse pleural thickening and subpleural lesions of the lung, even in emergency settings. Transthoracic US is useful as a guidance system for thoracentesis and peripheral lesion biopsy, where it minimises the occurrence of pneumothorax and haemorrhage. Transthoracic US imaging is strongly influenced by physical interaction of the ultrasonic beam at the tissue/air interface, which gives rise to reverberations classified as simple (A-line), “comet tail” and “ring down”(B-line) artifacts. Although these artifacts can be suggestive of a disease condition, they are essentially imaging errors present even in normal subjects and in empty-pleura post-pneumonectomy patients. In order to clarify some confusion and to report on the state of the art, we present a review of the literature on transthoracic US in diseases of the pleura and peripheral lung regions and our own clinical experience over 3 decades. The review focuses on quality assurance procedures and their value in diagnostic imaging and patient monitoring and warns against possible inappropriate indications and misleading information. Thoracic US is much more than “fishing for the moon in the well”.









Similar content being viewed by others
References
Dunn F, Fry WJ (1961) Ultrasonic absorption and reflection by lung tissue. Phys Med Biol 5:401–410
Dunn F (1974) Attenuation and speed of ultrasound in lung. J Acoust Soc Am 56:1638–1639
Ziskin MC (1993) Fundamental physics of ultrasound and its propagation in tissue. Radiographics 13:705–709
Ziskin MC, Thickman DI, Goldenberg NJ et al (1982) The comet tail artifact. J Ultrasound Med 1:1–7
Lee RK (2005) Grayscale ultrasound artifacts. In: Dogra V, Rubens DJ (eds) Ultrasound secrets. Elseiver, Philadelphia, pp 8–13
Bamber JC (1986) Attenuation, and absorption. In: Hill CR (ed) Physical principles of medical ultrasonic. Ellis Horwood Ltd., Chichester, pp 135–138
Beckh S, Bolcskei PL, Lessnau KD (2002) Real time chest ultrasonography: a comprehensive review for the pneumologist. Chest 122:1759–1773
Mathis G (1997) Thorax sonography—part I: chest wall and pleura. Ultrasound Med Biol 23:1131–1139
Dietrich CF, Hirche TO, Schreiber D, Wagner TO (2003) Sonographie von pleura and lunge. Ultraschall Med 24:303–311
Herthj FJ, Becker HD (2003) Transthoracic ultrasound. Respiration 70:87–94
Reissig A, Görg C, Mathis G (2009) Transthoracic sonography in the diagnosis of pulmonary diseases: a systematic approach. Ultraschall Med 30:438–454
Sagar KB, Rhyne TL, Myers GS, Lees RS (1978) Characterization of normal and abnormal pulmonary surface by reflected ultrasound. Chest 74:29–33
Reuter KL, Bogdan A (2009) Physics of diagnostic ultrasound creating the image. In: Bolliger CT, Herth FJF, Mayo PH, Miyazawa T, Beamis JF (eds) Clinical chest ultrasound: from the ICU to the bronchoscopy suite. Prog Respir Res. Basel, Karger, vol 37, pp 2–10
Sperandeo M, Varriale A, Sperandeo G et al (2011) Characterization of the normal pulmonary surface and pneumonectomy space by reflected ultrasound. J Ultrasound 14:22–27
Scanlan K (1991) Sonographic artifacts and their origin. Am J Roentgenol 156:1267–1272
Gustavson S, Olin JW (2006) Image in vascular medicine mirror image artifact. Vasc Med 11:175–176
Avruch L, Cooperberg PL (1985) The ring-down artifact. J Ultrasound Med 4:21–28
Targhetta R, Chavagneux R, Bourgeois JM et al (1992) Sonographic approach to diagnosing pulmonary consolidation. J Ultrasound Med 11:667–672
Wilson S, Burns PN, Wilkinson LM et al (1999) Gas at abdominal US: appearance, relevance, and analysis of artifacts. Radiology 210:113–123
Pedersen PC, Ozcan HS (1986) Ultrasound properties of lung tissue and their measurements. Ultrasound Med Biol 12:483–499
Kremkau FW (2006) Diagnostic ultrasound. Principles and instruments, 7th edn. Saunders/Elsevier, Missouri, pp 263–265
Lim JH, Lee KS, Kim TS, Chung MP (1999) Ring-down artifacts posterior to the right hemidiaphragm on abdominal sonography: sign of pulmonary parenchymal abnormalities. J Ultrasound Med 18:403–410
Shapiro RS, Winsberg F (1990) Comet-tail artifact from cholesterol crystals: observations in the postlithotripsy gallbladder and an in vitro model. Radiology 177:153–156
Sperandeo M, Carnevale V, Varriale A (2010) Response to pleuropulmonary US examination artifacts: “errors in images”. Ultrasound Med Biol 36:357
Yang PC, Luh KT, Chang DB et al (1992) Value of sonography in determining the nature of pleura effusion: analysis of 320 cases. Am J Roentgenol 159:29–33
Eibemberger KI, Wolfgang ID, Anman ME et al (1994) Quantification of pleural effusion: sonography versus radiography. Radiology 191:681–684
Cardinale L, Ardissone F, Asteggiano F et al (2013) Diffuse neoplasms of the pleural serosa. Radiol Med 118:366–378
Yu CJ, Yang PC, Chang DB et al (1992) Diagnostic and therapeutic use of chest sonography; value in critically ill patients. Am J Roentgenol 159:695–701
Kirkpatric AW, Ng AK, Dulchavsky SA et al (2001) Sonographic diagnosis of a pneumothorax inapparent on plain radiography: confirmation by computed tomography. J Trauma 50:750–752
Targhetta R, Bourgeois JM, Chavagneux R, Balmes P (1992) Diagnosis of pneumothorax by ultrasound immediately after ultrasonically guided aspiration biopsy. Chest 101:855–856
Muller NL (1993) Imaging of the pleura. Radiology 186:297–309
Doust B, Baum JK, Doust VL (1975) Ultrasonic evaluation of pleural opacities. Radiology 114:135–140
Palazzetti V, Gasparri E, Gambini C et al (2013) Chest radiography in intensive care: an irreplaceable survey? Radiol Med 118:744–751
Mathis G (1997) Thorax sonography—part II: peripheral pulmonary consolidation. Ultrasound Med Biol 23:1141–1153
Yang PC, Luh KT, Wu HD (1990) Lung tumors associated with obstructive pneumonitis: US studies. Radiology 174:717–720
Sperandeo M, Varriale A, Sperandeo G et al (2009) Transthoracic ultrasound in the evaluation of pulmonary fibrosis: our experience. Ultrasound Med Biol 35:723–729
Bolliger CT, Herth FJF, Mayo PH et al (2009) Clinical chest ultrasound: from the ICU to the bronchoscopy suite. Karger, Basel
Sperandeo M, Carnevale V, Muscarella S et al (2011) Clinical application of transthoracic ultrasonography in inpatients with pneumonia. Eur J Clin Invest 41:1–7
Sconfienza LM, Mauri G, Grossi F et al (2013) Pleural and peripheral lung lesions: comparison of US- and CT-guided biopsy. Radiology 266:930–935
Fraioli F, Serra Liberali S et al (2011) Clinical application of dual-source CT in the evaluation of patients with lung cancer: correlation with perfusion scintigraphy and pulmonary function tests. Radiol Med 116:842–857
Wang HC, Yu CJ, Chang DB et al (1995) Transthoracic needle biopsy of thoracic tumours by a colour Doppler ultrasound puncture guiding device. Thorax 50:1258–1263
Sperandeo M, Sperandeo G, Varriale A et al (2006) Contrast-enhanced ultrasound (CEUS) for the study of peripheral lung lesions: a preliminary study. Ultrasound Med Biol 32(10):1467–1472
Trovato GM, Sperandeo M, Catalano D (2013) Computed tomography screening for lung cancer. Ann Intern Med 159:155
Sperandeo M, Varriale A, Sperandeo G et al (2012) Assessment of ultrasound acoustic artifacts in patients with acute dyspnea: a multicenter study. Acta Radiol 53:885–892
Trovato GM, Rollo VC, Martines GF et al (2013) Thoracic ultrasound in the differential diagnosis of severe dyspnea: a reappraisal. Int J Cardiol 167:1081–1083
Trovato GM, Sperandeo M (2013) Sounds, ultrasounds, and artifacts: which clinical role for lung imaging? Am J Respir Crit Care Med 187:780–781
Trovato GM, Catalano D, Martines GF, Sperandeo M (2013) Is it time to measure lung water by ultrasound? Intensive Care Med 39:1662
Di Marco V, Ginardi V, Mazzone O, Trovato GM (1980) Acute pericarditis treatment during maintenance hemodialysis. G Ital Cardiol 10:79–83
Sperandeo M, Filabozzi P, Varriale A et al (2008) Role of thoracic ultrasound in the assessment of pleural and pulmonary diseases. J Ultrasound 11:39–46
Cervi PM, Trevisani L, Zucchi F (1990) Echo-guided biopsy in peripheral pulmonary lesions. Our experience. Radiol Med 80:445–450
Liao WY, Chen MZ, Chang YL et al (2000) US guided transthoracic cutting biopsy for peripheral thoracic lesions less than 3 cm in diameter. Radiology 217:685–691
Sheth S, Hamper UM, Stanley DB et al (1999) US guidance for thoracic biopsy: a valuable alternative to CT. Radiology 210:721–726
Yang PC (2000) Ultrasound-guided transthoracic biopsy of the chest. Radiol Clin North Am 38:323–343
Conflict of interest
Marco Sperandeo, Antonio Rotondo, Giuseppe Guglielmi, Daniela Catalano, Beatrice Feragalli, and Guglielmo M. Trovato declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Appendix 1
Appendix 1
Key points of transthoracic ultrasound (TUS)
Context
-
Wider dissemination of competence in noninvasive diagnostic procedures for outpatient clinic, elective, emergency and intensive medicine
-
Benefits of imaging assistance for safer invasive procedures.
Contribution
-
US is primarily and almost exclusively an imaging technology: the quality requisites are the greatest possible correspondence and, hopefully, a good overlap with the real anatomy, reproducibility of methods and reliable predictivity.
-
In echocardiography, vascular US (both involving Doppler techniques), elastography and CEUS imaging is linked with physical measurements which, by association and relationship, rely on actual morphology and function.
-
TUS is a significant part of US knowledge skills and expertise and requires adequate comprehensive training and professional qualified certification.
-
The invasive US-guided procedures are diagnostic FNAB, useful also for lung and mediastinal nodes, therapeutic procedures, such as US-assisted puncture of liquid cavities (pleural, pericardial, cystic, others) or intervention therapy, such as ablations, scarcely used for lungs.
-
Reliable and affordable noninvasive procedures, such as TUS, must be appropriately used concurrently.
Caution
-
Noninvasive TUS has a good safety level.
-
TUS does not allow for time-wasting procedures or uncomfortable patient positioning: both can be even harmful and distress the patients.
-
Invasive US-guided procedures are safer when provided by expert and appropriately trained specialists with adequate equipment within well-articulated facilities.
Implications
-
Studies claiming advantages from any TUS procedure are meaningless and should not be considered within any evidence-based medicine report if the methodology is unreliable and there is no robust analysis of predictivity.
-
The cost-benefit ratio depends mostly on the actual expertise of the operators.
-
Clinical expertise in the specific field of medicine and knowledge and skills acquired by adequate preliminary and ongoing training are the conditions for achieving satisfactory information and beneficial outcomes.
Rights and permissions
About this article
Cite this article
Sperandeo, M., Rotondo, A., Guglielmi, G. et al. Transthoracic ultrasound in the assessment of pleural and pulmonary diseases: use and limitations. Radiol med 119, 729–740 (2014). https://doi.org/10.1007/s11547-014-0385-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-014-0385-0