Abstract
Purpose
This study was undertaken to compare semen quality, hormonal status, and social factors in transgender women seeking fertility preservation with those of fertile cisgender men. Long-range goals are to establish standard practice measures ensuring optimum semen quality for cryopreservation and fertility preservation in transgender women.
Methods
This is a case-control study carried out at an academic medical center. Cases are transgender women seeking fertility preservation prior to initiation of hormone therapy. Controls are cisgender men recently fathering a child. All participants completed the Depression Anxiety Stress Scales 21 survey and additional survey questions related to personal behaviors. Complete semen analysis was carried out in a clinical andrology laboratory according to WHO guidelines, 5th edition. Serum follicle stimulating hormone, estradiol, and testosterone were measured at the time of semen analysis.
Results
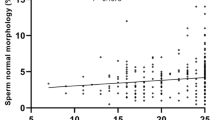
Sperm concentration, total sperm per ejaculate, total motile sperm, volume, and normal sperm morphology were significantly lower in transgender females compared with fertile cisgender men. Other measures of semen parameters and hormone concentrations were not different between groups. Survey results indicated transgender women were more likely to have symptoms of depression, anxiety, and stress and utilize tucking and tight undergarments, compared with controls; however, both groups reported similar numbers of ejaculations per week.
Conclusions
Although semen parameters were low, cryopreservation of sperm prior to hormone therapy is a viable fertility preservation option for most transgender women. The etiology of the differences in semen parameters is not known. Enhanced education related to personal behaviors or treatment to reduce effects of stressors prior to cryopreservation may improve future fertility potential.




Similar content being viewed by others
References
Institute of Medicine Committee on Lesbian GB, Transgender Health I, Research, Gaps Opportunities,. The National Academies Collection: Reports funded by National Institutes of Health. National Academies Press (US) National Academy of Sciences. 2011.
Fisk NM. Editorial: Gender dysphoria syndrome--the conceptualization that liberalizes indications for total gender reorientation and implies a broadly based multi-dimensional rehabilitative regimen. West J Med. 1974;120:386–91.
Coleman E, Bockting M, Botzer P. Standards of care for the health of transsexual, transgender, and gender-nonconforming people, version 7. Int J Transgender. 2012;13:165–232.
Medicine ECotASfR. Access to fertility services by transgender persons: an Ethics Committee opinion. Fertil Steril. 2015;104:1111–5.
Cooper TG, Noonan E, von Eckardstein S, Auger J, Baker HW, Behre HM, et al. World Health Organization reference values for human semen characteristics. Hum Reprod Update. 2010;16:231–45.
Redmon JB, Thomas W, Ma W, Drobnis EZ, Sparks A, Wang C, et al. Semen parameters in fertile US men: the Study for Future Families. Andrology. 2013;1:806–14.
Lovibond PF, Lovibond SH. The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav Res Ther. 1995;33:335–43.
Sinclair SJ, Siefert CJ, Slavin-Mulford JM, Stein MB, Renna M, Blais MA. Psychometric evaluation and normative data for the depression, anxiety, and stress scales-21 (DASS-21) in a nonclinical sample of U.S. adults. Eval Health Prof. 2012;35:259–79.
Antony MM, Bieling PJ, Cox BJ, Enns MW, Swinson RP. Psychometric properties of the 42- item and 21-item versions of the Depression Anxiety Stress Scales in clinical groups and a community sample. Psychol Assess. 1998;10:176–81.
Henry JD, Crawford JR. The short-form version of the Depression Anxiety Stress Scales (DASS-21): construct validity and normative data in a large non-clinical sample. Br J Clin Psychol. 2005;44:227–39.
Organization WH. WHO laboratory manual for the examination and processing of human semen. 5th ed: WHO Press; 2010.
Bjorndahl L, Barratt CL, Mortimer D, Jouannet P‘. How to count sperm properly’: checklist for acceptability of studies based on human semen analysis. Hum Reprod. 2016;31:227–32.
de Neergaard R, Nielsen JE, Jorgensen A, Toft BG, Goetze JP, Jorgensen N. Positive association between cholesterol in human seminal plasma and sperm counts: results from a cross-sectional cohort study and immunohistochemical investigations. Andrology. 2018;6:817–28.
Erenpreiss J, Punab M, Zilaitiene B, Hlevicka S, Zayakin P, Matulevicius V, et al. Semen quality of young men from the general population in Baltic countries. Hum Reprod. 2017;32:1334–40.
Priskorn L, Bang AK, Nordkap L, Krause M, Mendiola J, Jensen TK, et al. Anogenital distance is associated with semen quality but not reproductive hormones in 1106 young men from the general population. Hum Reprod. 2019;34:12–24.
Hart RJ, Doherty DA, McLachlan RI, Walls ML, Keelan JA, Dickinson JE, et al. Testicular function in a birth cohort of young men. Hum Reprod. 2015;30:2713–24.
Jensen TK, Swan S, Jorgensen N, Toppari J, Redmon B, Punab M, et al. Alcohol and male reproductive health: a cross-sectional study of 8344 healthy men from Europe and the USA. Hum Reprod. 2014;29:1801–9.
Huang C, Li B, Xu K, Liu D, Hu J, Yang Y, et al. Decline in semen quality among 30,636 young Chinese men from 2001 to 2015. Fertil Steril. 2017;107:83–88.e2.
Hammoud AO, Meikle AW, Peterson CM, Stanford J, Gibson M, Carrell DT. Association of 25-hydroxy-vitamin D levels with semen and hormonal parameters. Asian J Androl. 2012;14:855–9.
Levine H, Jorgensen N, Martino-Andrade A, Mendiola J, Weksler-Derri D, Mindlis I, et al. Temporal trends in sperm count: a systematic review and meta-regression analysis. Hum Reprod Update. 2017;23:646–59.
Fernandez MF, Duran I, Olea N, Avivar C, Vierula M, Toppari J, et al. Semen quality and reproductive hormone levels in men from Southern Spain. Int J Androl. 2012;35:1–10.
Jorgensen N, Joensen UN, Jensen TK, Jensen MB, Almstrup K, Olesen IA, et al. Human semen quality in the new millennium: a prospective cross-sectional population-based study of 4867 men. BMJ Open. 2012;2:e000990.
Jorgensen N, Vierula M, Jacobsen R, Pukkala E, Perheentupa A, Virtanen HE, et al. Recent adverse trends in semen quality and testis cancer incidence among Finnish men. Int J Androl. 2011;34:e37–48.
Virtanen HE, Jorgensen N, Toppari J. Semen quality in the 21(st) century. Nat Rev Urol. 2017;14:120–30.
Richthoff J, Rylander L, Hagmar L, Malm J, Giwercman A. Higher sperm counts in Southern Sweden compared with Denmark. Hum Reprod. 2002;17:2468–73.
Axelsson J, Rylander L, Rignell-Hydbom A, Giwercman A. No secular trend over the last decade in sperm counts among Swedish men from the general population. Hum Reprod. 2011;26:1012–6.
Hamada A, Kingsberg S, Wierckx K, T’Sjoen G, De Sutter P, Knudson G, et al. Semen characteristics of transwomen referred for sperm banking before sex transition: a case series. Andrologia. 2015;47:832–8.
Li K, Rodriguez D, Gabrielsen JS, Centola GM, Tanrikut C. Sperm cryopreservation of transgender individuals: trends and findings in the past decade. Andrology. 2018;6:860–4.
Jarow JP, Espeland MA, Lipshultz LI. Evaluation of the azoospermic patient. J Urol. 1989;142:62–5.
Glazer CH, Li S, Zhang CA, Giwercman A, Bonde JP, Eisenberg ML. Racial and sociodemographic differences of semen parameters among US men undergoing a semen analysis. Urology. 2019;123:126–32.
Swan SH, Brazil C, Drobnis EZ, Liu F, Kruse RL, Hatch M, et al. Geographic differences in semen quality of fertile U.S. males. Environ Health Perspect. 2003;111:414–20.
Fisch H, Goluboff ET, Olson JH, Feldshuh J, Broder SJ, Barad DH. Semen analyses in 1,283 men from the United States over a 25-year period: no decline in quality. Fertil Steril. 1996;65:1009–14.
Nordkap L, Joensen UN, Blomberg Jensen M, Jorgensen N. Regional differences and temporal trends in male reproductive health disorders: semen quality may be a sensitive marker of environmental exposures. Mol Cell Endocrinol. 2012;355:221–30.
Agarwal A, Gupta S, Du Plessis S, Sharma R, Esteves SC, Cirenza C, et al. Abstinence time and its impact on basic and advanced semen parameters. Urology. 2016;94:102–10.
Ayad BM, Horst GV, Plessis SSD. Revisiting the relationship between the ejaculatory abstinence period and semen characteristics. Int J Fertil Steril. 2018;11:238–46.
Rao M, Xia W, Yang J, Hu LX, Hu SF, Lei H, et al. Transient scrotal hyperthermia affects human sperm DNA integrity, sperm apoptosis, and sperm protein expression. Andrology. 2016;4:1054–63.
Rao M, Zhao XL, Yang J, Hu SF, Lei H, Xia W, et al. Effect of transient scrotal hyperthermia on sperm parameters, seminal plasma biochemical markers, and oxidative stress in men. Asian J Androl. 2015;17:668–75.
Garolla A, Torino M, Miola P, Caretta N, Pizzol D, Menegazzo M, et al. Twenty-four-hour monitoring of scrotal temperature in obese men and men with a varicocele as a mirror of spermatogenic function. Hum Reprod. 2015;30:1006–13.
Jurewicz J, Radwan M, Sobala W, Radwan P, Jakubowski L, Hawula W, et al. Lifestyle factors and sperm aneuploidy. Reprod Biol. 2014;14:190–9.
Sanger WG, Friman PC. Fit of underwear and male spermatogenesis: a pilot investigation. Reprod Toxicol. 1990;4:229–32.
Jung A, Schuppe HC. Influence of genital heat stress on semen quality in humans. Andrologia. 2007;39:203–15.
Munkelwitz R, Gilbert BR. Are boxer shorts really better? A critical analysis of the role of underwear type in male subfertility. J Urol. 1998;160:1329–33.
Shiraishi K, Matsuyama H. Gonadotoropin actions on spermatogenesis and hormonal therapies for spermatogenic disorders [Review]. Endocr J. 2017;64:123–31.
Mieusset R, Bujan L, Plantavid M, Grandjean H. Increased levels of serum follicle-stimulating hormone and luteinizing hormone associated with intrinsic testicular hyperthermia in oligospermic infertile men. J Clin Endocrinol Metab. 1989;68:419–25.
Cardona Maya W, Berdugo J, Cadavid Jaramillo A. The effects of male age on semen parameters: analysis of 1364 men attending an andrology center. Aging Male. 2009;12:100–3.
Levitas E, Lunenfeld E, Weisz N, Friger M, Potashnik G. Relationship between age and semen parameters in men with normal sperm concentration: analysis of 6022 semen samples. Andrologia. 2007;39:45–50.
Stone BA, Alex A, Werlin LB, Marrs RP. Age thresholds for changes in semen parameters in men. Fertil Steril. 2013;100:952–8.
Veron GL, Tissera AD, Bello R, Beltramone F, Estofan G, Molina RI, et al. Impact of age, clinical conditions, and lifestyle on routine semen parameters and sperm kinematics. Fertil Steril. 2018;110:68–75 e4.
Li Y, Lin H, Li Y, Cao J. Association between socio-psycho-behavioral factors and male semen quality: systematic review and meta-analyses. Fertil Steril. 2011;95:116–23.
Durairajanayagam D. Lifestyle causes of male infertility. Arab J Urol. 2018;16:10–20.
Nordkap L, Jensen TK, Hansen AM, Lassen TH, Bang AK, Joensen UN, et al. Psychological stress and testicular function: a cross-sectional study of 1,215 Danish men. Fertil Steril. 2016;105:174–87.e1-2.
Gollenberg AL, Liu F, Brazil C, Drobnis EZ, Guzick D, Overstreet JW, et al. Semen quality in fertile men in relation to psychosocial stress. Fertil Steril. 2010;93:1104–11.
Zou P, Wang X, Sun L, Chen Q, Yang H, Zhou N, et al. Semen quality in Chinese college students: associations with depression and physical activity in a cross-sectional study. Psychosom Med. 2018;80:564–72.
Bartolo A, Reis S, Monteiro S, Leite R, Montenegro N. Psychological adjustment of infertile men undergoing fertility treatments: an association with sperm parameters. Arch Psychiatr Nurs. 2016;30:521–6.
Eskiocak S, Gozen AS, Taskiran A, Kilic AS, Eskiocak M, Gulen S. Effect of psychological stress on the L-arginine-nitric oxide pathway and semen quality. Braz J Med Biol Res. 2006;39:581–8.
Vellani E, Colasante A, Mamazza L, Minasi MG, Greco E, Bevilacqua A. Association of state and trait anxiety to semen quality of in vitro fertilization patients: a controlled study. Fertil Steril. 2013;99:1565–72.
Volgsten H, Ekselius L, Poromaa IS, Svanberg AS. Personality traits associated with depressive and anxiety disorders in infertile women and men undergoing in vitro fertilization treatment. Acta Obstet Gynecol Scand. 2010;89:27–34.
Wdowiak A, Bien A, Iwanowicz-Palus G, Makara-Studzinska M, Bojar I. Impact of emotional disorders on semen quality in men treated for infertility. Neuro Endocrinol Lett. 2017;38:50–8.
Bhongade MB, Prasad S, Jiloha RC, Ray PC, Mohapatra S, Koner BC. Effect of psychological stress on fertility hormones and seminal quality in male partners of infertile couples. Andrologia. 2015;47:336–42.
Clarke RN, Klock SC, Geoghegan A, Travassos DE. Relationship between psychological stress and semen quality among in-vitro fertilization patients. Hum Reprod. 1999;14:753–8.
Eskiocak S, Gozen AS, Kilic AS, Molla S. Association between mental stress & some antioxidant enzymes of seminal plasma. Indian J Med Res. 2005;122:491–6.
Lampiao F. Variation of semen parameters in healthy medical students due to exam stress. Malawi Med J. 2009;21:166–7.
Drobnis EZ, Nangia AK. Psychotropics and male reproduction. Adv Exp Med Biol. 2017;1034:63–101.
Norr L, Bennedsen B, Fedder J, Larsen ER. Use of selective serotonin reuptake inhibitors reduces fertility in men. Andrology. 2016;4:389–94.
Acknowledgments
The authors thank the participants for contributing to this study.
Funding
This study was funded in part by a clinical and multidisciplinary pilot grant from the University of Kansas Medical Center Research Institute.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Marsh, C., McCracken, M., Gray, M. et al. Low total motile sperm in transgender women seeking hormone therapy. J Assist Reprod Genet 36, 1639–1648 (2019). https://doi.org/10.1007/s10815-019-01504-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-019-01504-y