Abstract
Purpose
Mosaicism is a prevalent characteristic of human preimplantation embryos. This retrospective cohort study aimed to investigate pregnancy outcomes after transfer of mosaic or euploid embryos.
Methods
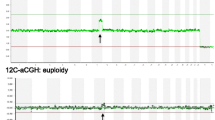
The embryos, which had been transferred as “euploidy,” were processed using array-based comparative genomic hybridization (aCGH). The original aCGH charts of the transferred embryos were reanalyzed. Mosaic and control euploid embryos were defined according to log2 ratio calls.
Results
Overall, 102 embryos were determined to be mosaic, of which 101 were estimated to harbor no more than 50% aneuploid mosaicism. Additionally, 268 euploid embryos were matched as controls. The rates of live birth (46.6% vs. 59.1%, odds ratio (OR) 0.60, 95% confidence interval (CI) 0.38–0.95), and biochemical pregnancy (65.7% vs. 76.1%, OR 0.60, 95% CI 0.37–0.99) per transfer cycle were significantly lower after mosaic embryo transfer than after euploid embryo transfer. The rates of clinical pregnancy and pregnancy loss and the risks of obstetric outcomes did not differ significantly between the two groups.
Conclusions
Compared with euploid embryo transfer, mosaic embryo transfer is associated with a lower rate of live birth, which is mainly attributed to a decreased rate of conception. However, as mosaic embryo transfer yielded a live birth rate of 46.6%, patients without euploid embryos could be counseled regarding this alternative option.

Similar content being viewed by others
References
Taylor TH, Gitlin SA, Patrick JL, Crain JL, Wilson JM, Griffin DK. The origin, mechanisms, incidence and clinical consequences of chromosomal mosaicism in humans. Hum Reprod Update. 2014;20(4):571–81. https://doi.org/10.1093/humupd/dmu016.
Delhanty JD, Griffin DK, Handyside AH, Harper J, Atkinson GH, Pieters MH, et al. Detection of aneuploidy and chromosomal mosaicism in human embryos during preimplantation sex determination by fluorescent in situ hybridisation (FISH). Hum Mol Genet. 1993;2(8):1183–5.
Munne S, Weier HU, Grifo J, Cohen J. Chromosome mosaicism in human embryos. Biol Reprod. 1994;51(3):373–9.
McCoy RC. Mosaicism in preimplantation human embryos: when chromosomal abnormalities are the norm. Trends Genet. 2017;33(7):448–63. https://doi.org/10.1016/j.tig.2017.04.001.
Delhanty JD, Harper JC, Ao A, Handyside AH, Winston RM. Multicolour FISH detects frequent chromosomal mosaicism and chaotic division in normal preimplantation embryos from fertile patients. Hum Genet. 1997;99(6):755–60.
Evsikov S, Verlinsky Y. Mosaicism in the inner cell mass of human blastocysts. Hum Reprod. 1998;13(11):3151–5.
Magli MC, Jones GM, Gras L, Gianaroli L, Korman I, Trounson AO. Chromosome mosaicism in day 3 aneuploid embryos that develop to morphologically normal blastocysts in vitro. Hum Reprod. 2000;15(8):1781–6.
Capalbo A, Wright G, Elliott T, Ubaldi FM, Rienzi L, Nagy ZP. FISH reanalysis of inner cell mass and trophectoderm samples of previously array-CGH screened blastocysts shows high accuracy of diagnosis and no major diagnostic impact of mosaicism at the blastocyst stage. Hum Reprod. 2013;28(8):2298–307. https://doi.org/10.1093/humrep/det245.
Bielanska M, Tan SL, Ao A. High rate of mixoploidy among human blastocysts cultured in vitro. Fertil Steril. 2002;78(6):1248–53.
Vorsanova SG, Kolotii AD, Iourov IY, Monakhov VV, Kirillova EA, Soloviev IV, et al. Evidence for high frequency of chromosomal mosaicism in spontaneous abortions revealed by interphase FISH analysis. J Histochem Cytochem. 2005;53(3):375–80. https://doi.org/10.1369/jhc.4A6424.2005.
Forsberg LA, Gisselsson D, Dumanski JP. Mosaicism in health and disease—clones picking up speed. Nat Rev Genet. 2017;18(2):128–42. https://doi.org/10.1038/nrg.2016.145.
Simon C. Introduction: to transfer or not transfera mosaic embryo, that is the question. Fertil Steril. 2017;107(5):1083–4. https://doi.org/10.1016/j.fertnstert.2017.03.025.
Maxwell SM, Colls P, Hodes-Wertz B, DH MC, McCaffrey C, Wells D, et al. Why do euploid embryos miscarry? A case-control study comparing the rate of aneuploidy within presumed euploid embryos that resulted in miscarriage or live birth using next-generation sequencing. Fertil Steril. 2016;106(6):1414–9. https://doi.org/10.1016/j.fertnstert.2016.08.017.
Gutierrez-Mateo C, Colls P, Sanchez-Garcia J, Escudero T, Prates R, Ketterson K, et al. Validation of microarray comparative genomic hybridization for comprehensive chromosome analysis of embryos. Fertil Steril. 2011;95(3):953–8. https://doi.org/10.1016/j.fertnstert.2010.09.010.
Yang Z, Liu J, Collins GS, Salem SA, Liu X, Lyle SS, et al. Selection of single blastocysts for fresh transfer via standard morphology assessment alone and with array CGH for good prognosis IVF patients: results from a randomized pilot study. Mol Cytogenet. 2012;5(1):24. https://doi.org/10.1186/1755-8166-5-24.
Sermon K, Capalbo A, Cohen J, Coonen E, De Rycke M, De Vos A, et al. The why, the how and the when of PGS 2.0: current practices and expert opinions of fertility specialists, molecular biologists, and embryologists. Mol Hum Reprod. 2016;22(8):845–57. https://doi.org/10.1093/molehr/gaw034.
Fiorentino F, Spizzichino L, Bono S, Biricik A, Kokkali G, Rienzi L, et al. PGD for reciprocal and Robertsonian translocations using array comparative genomic hybridization. Hum Reprod. 2011;26(7):1925–35. https://doi.org/10.1093/humrep/der082.
Alfarawati S, Fragouli E, Colls P, Wells D. First births after preimplantation genetic diagnosis of structural chromosome abnormalities using comparative genomic hybridization and microarray analysis. Hum Reprod. 2011;26(6):1560–74. https://doi.org/10.1093/humrep/der068.
Franasiak JM, Scott RT Jr. Embryonic aneuploidy: overcoming molecular genetics challenges improves outcomes and changes practice patterns. Trends Mol Med. 2014;20(9):499–508. https://doi.org/10.1016/j.molmed.2014.06.006.
Colls P, Escudero T, Fischer J, Cekleniak NA, Ben-Ozer S, Meyer B, et al. Validation of array comparative genome hybridization for diagnosis of translocations in preimplantation human embryos. Reprod BioMed Online. 2012;24(6):621–9. https://doi.org/10.1016/j.rbmo.2012.02.006.
Greco E, Minasi MG, Fiorentino F. Healthy babies after intrauterine transfer of mosaic aneuploid blastocysts. N Engl J Med. 2015;373(21):2089–90. https://doi.org/10.1056/NEJMc1500421.
Fragouli E, Alfarawati S, Spath K, Babariya D, Tarozzi N, Borini A, et al. Analysis of implantation and ongoing pregnancy rates following the transfer of mosaic diploid-aneuploid blastocysts. Hum Genet. 2017;136(7):805–19. https://doi.org/10.1007/s00439-017-1797-4.
Munne S, Blazek J, Large M, Martinez-Ortiz PA, Nisson H, Liu E, et al. Detailed investigation into the cytogenetic constitution and pregnancy outcome of replacing mosaic blastocysts detected with the use of high-resolution next-generation sequencing. Fertil Steril. 2017;108(1):62–71.e8. https://doi.org/10.1016/j.fertnstert.2017.05.002.
Spinella F, Fiorentino F, Biricik A, Bono S, Ruberti A, Cotroneo E, et al. Extent of chromosomal mosaicism influences the clinical outcome of in vitro fertilization treatments. Fertil Steril. 2018;109(1):77–83. https://doi.org/10.1016/j.fertnstert.2017.09.025.
Zhang Q, Li G, Zhang L, Sun X, Zhang D, Lu J et al. Maternal common variant rs2305957 spanning PLK4 is associated with blastocyst formation and early recurrent miscarriage. Fertil Steril 2017;107(4):1034–40 e5. doi:https://doi.org/10.1016/j.fertnstert.2017.01.006, 1040.e5.
Gardner DK, Lane M, Stevens J, Schlenker T, Schoolcraft WB. Blastocyst score affects implantation and pregnancy outcome: towards a single blastocyst transfer. Fertil Steril. 2000;73(6):1155–8. https://doi.org/10.1016/s0015-0282(00)00518-5.
Lledo B, Morales R, Ortiz JA, Blanca H, Ten J, Llacer J, et al. Implantation potential of mosaic embryos. Syst Biol Reprod Med. 2017;63(3):206–8. https://doi.org/10.1080/19396368.2017.1296045.
Garrisi G, Walmsley RH, Bauckman K, Mendola RJ, Colls P, Munne S. Discordance among serial biopsies of mosaic embryos. Fertil Steril. 2016;106((3):e151. https://doi.org/10.1016/j.fertnstert.2016.07.447.
Durrbaum M, Kuznetsova AY, Passerini V, Stingele S, Stoehr G, Storchova Z. Unique features of the transcriptional response to model aneuploidy in human cells. BMC Genomics. 2014;15:139. https://doi.org/10.1186/1471-2164-15-139.
Williams BR, Prabhu VR, Hunter KE, Glazier CM, Whittaker CA, Housman DE, et al. Aneuploidy affects proliferation and spontaneous immortalization in mammalian cells. Science. 2008;322(5902):703–9. https://doi.org/10.1126/science.1160058.
Lavon N, Narwani K, Golan-Lev T, Buehler N, Hill D, Benvenisty N. Derivation of euploid human embryonic stem cells from aneuploid embryos. Stem Cells. 2008;26(7):1874–82. https://doi.org/10.1634/stemcells.2008-0156.
Bolton H, Graham SJ, Van der Aa N, Kumar P, Theunis K, Fernandez Gallardo E, et al. Mouse model of chromosome mosaicism reveals lineage-specific depletion of aneuploid cells and normal developmental potential. Nat Commun. 2016;7:11165. https://doi.org/10.1038/ncomms11165.
Capalbo A, Rienzi L. Mosaicism between trophectoderm and inner cell mass. Fertil Steril. 2017;107(5):1098–106. https://doi.org/10.1016/j.fertnstert.2017.03.023.
Marin D, Scott RT Jr, Treff NR. Preimplantation embryonic mosaicism: origin, consequences and the reliability of comprehensive chromosome screening. Curr Opin Obstet Gynecol. 2017;29(3):168–74. https://doi.org/10.1097/GCO.0000000000000358.
Popovic M, Dheedene A, Christodoulou C, Taelman J, Dhaenens L, Van Nieuwerburgh F, et al. Chromosomal mosaicism in human blastocysts: the ultimate challenge of preimplantation genetic testing? Hum Reprod. 2018;33(7):1342–54. https://doi.org/10.1093/humrep/dey106.
Gleicher N, Metzger J, Croft G, Kushnir VA, Albertini DF, Barad DH. A single trophectoderm biopsy at blastocyst stage is mathematically unable to determine embryo ploidy accurately enough for clinical use. Reprod Biol Endocrinol. 2017;15(1):33. https://doi.org/10.1186/s12958-017-0251-8.
Capalbo A, Ubaldi FM, Rienzi L, Scott R, Treff N. Detecting mosaicism in trophectoderm biopsies: current challenges and future possibilities. Hum Reprod. 2017;32(3):492–8. https://doi.org/10.1093/humrep/dew250.
Segawa T, Kuroda T, Kato K, Kuroda M, Omi K, Miyauchi O, et al. Cytogenetic analysis of the retained products of conception after missed abortion following blastocyst transfer: a retrospective, large-scale, single-centre study. Reprod BioMed Online. 2017;34(2):203–10. https://doi.org/10.1016/j.rbmo.2016.11.005.
Malvestiti F, Agrati C, Grimi B, Pompilii E, Izzi C, Martinoni L, et al. Interpreting mosaicism in chorionic villi: results of a monocentric series of 1001 mosaics in chorionic villi with follow-up amniocentesis. Prenat Diagn. 2015;35(11):1117–27. https://doi.org/10.1002/pd.4656.
Munne S, Grifo J, Wells D. Mosaicism: “survival of the fittest” versus “no embryo left behind”. Fertil Steril. 2016;105(5):1146–9. https://doi.org/10.1016/j.fertnstert.2016.01.016.
Fiorentino F, Biricik A, Bono S, Spizzichino L, Cotroneo E, Cottone G, et al. Development and validation of a next-generation sequencing-based protocol for 24-chromosome aneuploidy screening of embryos. Fertil Steril. 2014;101(5):1375–82. https://doi.org/10.1016/j.fertnstert.2014.01.051.
Yang Z, Lin J, Zhang J, Fong WI, Li P, Zhao R, et al. Randomized comparison of next-generation sequencing and array comparative genomic hybridization for preimplantation genetic screening: a pilot study. BMC Med Genet. 2015;8:30. https://doi.org/10.1186/s12920-015-0110-4.
Acknowledgements
The authors expressed thanks to Wenjie Jiang, Hongqiang Xie, Hongchang Li, and Ping Li from Reproductive Hospital Affiliated to Shandong University for performing PGT procedures and following up.
Funding
This study was funded by the National Key Research and Development Program of China (grant number 2016YFC1000202), National Natural Science Foundation of China (grant number 81671522), and Innovative Foundation of Reproductive Hospital Affiliated to Shandong University (grant number 20171114).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhang, L., Wei, D., Zhu, Y. et al. Rates of live birth after mosaic embryo transfer compared with euploid embryo transfer. J Assist Reprod Genet 36, 165–172 (2019). https://doi.org/10.1007/s10815-018-1322-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-018-1322-2