Abstract
Purpose
To compare the time-course change in the postoperative anorectal function between laparoscopic intersphincteric resection (ISR) and low anterior resection (LAR).
Methods
This is a single-institution observational study. We evaluated the time-course change in the anorectal function using functional questionnaires before and at 6, 12, and 24 months after laparoscopic ISR or LAR.
Results
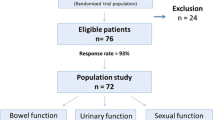
Sixty-two patients answered the functional questionnaires (28 in the ISR group and 34 in the LAR group). In the ISR group, the Wexner scores at 6, 12, and 24 months postoperatively were significantly higher than preoperatively. Importantly, the Wexner score at 24 months postoperatively was significantly lower than that at 6 months postoperatively. The low GIFO scores at 6 and 12 months postoperatively tended to be recovered to some extent at 24 months postoperatively. In the LAR group, Wexner score at 6 months postoperatively was significantly higher than that preoperatively. Notably, the Wexner score at 12 months postoperatively was recovered to almost the same as that preoperatively. The GIFO scores at 12 months postoperatively were mostly recovered to the same levels as those preoperatively.
Conclusions
Laparoscopic ISR exhibits different time-course changes in the anorectal function from laparoscopic LAR.



Similar content being viewed by others
References
Emmertsen KJ, Laurberg S, Rectal Cancer Function Study Group. Impact of bowel dysfunction on quality of life after sphincter-preserving resection for rectal cancer. Br J Surg. 2013;100:1377–87.
Schiessel R, Karner-Hanusch J, Herbst F, Teleky B, Wunderlich M. Intersphincteric resection for low rectal tumours. Br J Surg. 1994;81:1376–8.
Park JS, Choi GS, Jun SH, Hasegawa S, Sakai Y. Laparoscopic versus open intersphincteric resection and coloanal anastomosis for low rectal cancer: intermediate-term oncologic outcomes. Ann Surg. 2011;254:941–6.
Fujii S, Yamamoto S, Ito M, Yamaguchi S, Sakamoto K, Kinugasa Y, et al. Short-term outcomes of laparoscopic intersphincteric resection from a phase II trial to evaluate laparoscopic surgery for stage 0/I rectal cancer: Japan Society of Laparoscopic Colorectal Surgery Lap RC. Surg Endosc. 2012;6:3067–76.
Yamamoto S, Ito M, Okuda J, Fujii S, Yamaguchi S, Yoshimura K, et al. Laparoscopic surgery for stage 0/I rectal carcinoma: short-term outcomes of a single-arm phase II trial. Ann Surg. 2013;258:283–238.
Yamada K, Ogata S, Saiki Y, Fukunaga M, Tsuji Y, Takano M. Long-term results of intersphincteric resection for low rectal cancer. Dis Colon Rectum. 2009;52:1065–71.
Koyama M, Murata A, Sakamoto Y, Morohashi H, Takahashi S, Yoshida E, et al. Long-term clinical and functional results of intersphincteric resection for lower rectal cancer. Ann Surg Oncol. 2014;21:S422–S428.
Saito N, Ito M, Kobayashi A, Nishizawa Y, Kojima M, Nishizawa Y, et al. Long-term outcomes after intersphincteric resection for low-lying rectal cancer. Ann Surg Oncol. 2014;21:3608–3015.
Sakai Y, Kitano S. Practice guidelines on endoscopic surgery for qualified surgeons by the endoscopic surgical skill qualification system. Asian J Endosc Surg. 2015;8:103–13.
Hasegawa S, Nagayama S, Nomura A, Kawamura J, Sakai Y. Multimedia article. Autonomic nerve-preserving total mesorectal excision in the laparoscopic era. Dis Colon Rectum. 2008;51:1279–82.
Akagi Y, Kinugasa T, Shirouzu K. Intersphincteric resection for very low rectal cancer: a systematic review. Surg Today. 2013;43:838–47.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187–96.
van Duijvendijk P, Slors JF, Taat CW, Oosterveld P, Vasen HF. Functional outcome after colectomy and ileorectal anastomosis compared with proctocolectomy and ileal pouch-anal anastomosis in familial adenomatous polyposis. Ann Surg. 1999;230:648–54.
Jorge JM, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum. 1993;36:77–97.
Ito M, Saito N, Sugito M, Kobayashi A, Nishizawa Y, Tsunoda Y. Analysis of clinical factors associated with anal function after intersphincteric resection for very low rectal cancer. Dis Colon Rectum. 2009;52:64–70.
Floodeen H, Lindgren R, Hallböök O, Matthiessen P. Evaluation of long-term anorectal function after low anterior resection: a 5-year follow-up of a randomized multicenter trial. Dis Colon Rectum. 2014;57:1162–8.
Denost Q, Laurent C, Capdepont M, Zerbib F, Rullier E. Risk factors for fecal incontinence after intersphincteric resection for rectal cancer. Dis Colon Rectum. 2011;54:963–8.
Martin ST, Heneghan HM, Winter DC. Systematic review of outcomes after intersphincteric resection for low rectal cancer. Br J Surg. 2012;99:603–12.
Chamlou R, Parc Y, Simon T, Bennis M, Dehni N, Parc R, et al. Long-term results of intersphincteric resection for low rectal cancer. Ann Surg. 2007;246:916–21.
Honda M, Akiyoshi T, Noma H, Ogura A, Nagasaki T, Konishi T, et al. Patient-centered outcomes to decide treatment strategy for patients with low rectal cancer. J Surg Oncol. 2016;114:630–6.
Nishizawa Y, Fujii S, Saito N, Ito M, Ochiai S, Sugito M, et al. The association between anal function and neural degeneration after preoperative chemoradiotherapy followed by intersphincteric resection. Dis Colon Rectum. 2011;54:1423–9.
Acknowledgements
The authors thank the medical staff and residents of Kyoto University Hospital gastrointestinal surgery for their participation in this study. We could not have completed the study without their diligence and support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Kawada, K., Hida, K., Hasegawa, S. et al. A comparison of the long-term anorectal function between laparoscopic intersphincteric resection and low anterior resection for low rectal cancer. Surg Today 48, 921–927 (2018). https://doi.org/10.1007/s00595-018-1669-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-018-1669-0