Abstract
Purpose
Palliative care (PC) and palliative radiotherapy (RT) consultation are integral to the care of patients with advanced cancer. These services are not universally available in rural areas, and travel to urban centers to access them can be burdensome for patients and families. The objectives of our study were to assess the feasibility of using videoconferencing to provide specialist multidisciplinary PC and palliative RT consultation to cancer patients in rural areas and to explore symptom, cost, and satisfaction outcomes.
Methods
The Virtual Pain and Symptom Control and Palliative Radiotherapy Clinic was piloted from January 2008 to March 2011. Cancer patients in rural northern Alberta attended local telehealth facilities, accompanied by nurses trained in symptom assessment. The multidisciplinary team at the Cross Cancer Institute in Edmonton was linked by videoconference. Team recommendations were sent to the patients’ family physicians. Data were collected on referral, clinical, and consultation characteristics and symptom, cost, and satisfaction outcomes.
Results
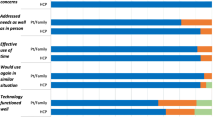
Forty-four initial consultation and 28 follow-up visits took place. Mean Edmonton Symptom Assessment Scale scores for anxiety and appetite were statistically significantly improved at the first follow-up visit (p < 0.01 and p = 0.03, respectively). Average per visit savings for patients seen by telehealth versus attending the CCI were 471.13 km, 7.96 hours, and Cdn $192.71, respectively. Patients and referring physicians indicated a high degree of satisfaction with the clinic.
Conclusion
Delivery of specialist multidisciplinary PC consultation by videoconferencing is feasible, may improve symptoms, results in cost savings to patients and families, and is satisfactory to users.


Similar content being viewed by others
References
Smith TJ, Temin S, Alesi ER et al (2012) American Society of Clinical Oncology Provisional Clinical Opinion: the integration of palliative care into standard oncology care. J Clin Oncol 30(8):880–887
Van Oorschot V, Schuler M, Simon A, Schleicher U, Geinitz H (2011) Patterns of care and course of symptoms in palliative radiotherapy: a multicenter pilot study analysis. Strahlenther Onkol 187:461–466
Robinson CA, Pesut B, Bottorff JL, Mowry A, Broughton S, Fyles G (2009) Rural palliative care: a comprehensive review. J Palliat Med 12:253–258
Pesut B, Robinson CA, Bottorff JL, Fyles G, Broughton S (2010) On the road again: patient perspectives on commuting for palliative care. Palliat Support Care 8:187–195
Lockie SJ, Borttorff JL, Robinson CA, Pesut B (2010) Experiences of rural family caregivers who assist with commuting for palliative care. CJNR 42:74–91
Lavergne ML, Johnston GM, Gao J, Dummer TJB, Rheaume DE (2010) Variation in the use of palliative radiotherapy at end of life: examining demographic, clinical, health service, and geographic factors in a population-based study. Palliat Med 25:101–110
Roine R, Ohinmaa A, Hailey D (2001) Assessing telemedicine: a systematic review of the literature. CMAJ 165:765–771
Kitamura C, Zurawel-Balaura L, Wong RKS (2010) How effective is video consultation in clinical oncology? A systematic review. Curr Oncol 17:17–27
Palkhivala A (2011) Canada develops models of teleoncology. J Natl Cancer Inst 103:1566–1568
Aoki N, Ohta S, Yamamoto H, Kikuchi N, Dunn K (2006) Triangulation analysis of tele-palliative care implementation in a rural community area in Japan. Telemed J E Health 12:655–662
Bensink M, Armfield N, Pinkerton R, Irving H, Hallahan A, Theodoros D, Russell T, Barnett AG, Scuffham PA, Wootton R (2009) Using videotelephony to support paediatric oncology-related palliative care in the home: from abandoned RCT to acceptability study. Palliat Med 23:228–237
Bowles K, Baugh A (2007) Applying research evidence to optimize telehomecare. J Cardiovasc Nurs 22:5–15
Coyle N, Khojainova N, Francavilla J, Gonzales G (2002) Audio-visual communication and its use in palliative care. J Pain Symptom Manage 23:171–175
Gagnon M, Lamothe L, Hebert M, Chanliau J, Fortin J (2006) Telehomecare for vulnerable populations: the evaluation of new models of care. Telemed J E Health 12:324–331
Field M, Grigsby J (2002) Telemedicine and remote patient monitoring. JAMA 288:423–425
Lynch J, Weaver L, Hall P, Langlois S, Stunt M, Schroder C, Bouvette M (2004) Using telehealth technology to support CME in end-of-life care for community physicians in Ontario. Telemed J E Health 10:103–107
Maudlin J, Keene J, Kobb R (2006) A road map for the last journey: home telehealth for holistic end-of-life care. Am J Hosp Palliat Care 23:399–403
Morgan G, Craig B, Grant B, Sands A, Doherty N, Casey F (2008) Home videoconferencing for patients with severe congenital heart disease following discharge. Congenit Heart Dis 3:317–324
Statistics Canada: Canada at a glance 2011. Available at http://www.statcan.gc.ca/pub/12-581-x/2011000/pop-eng.htm#t01. Accessed 21 Feb 2012
Bruera E, Michaud M, Vigano A, Neumann CM, Watanabe S, Hanson J (2001) Multidisciplinary symptom control clinic in a cancer center: a retrospective study. Support Care Cancer 9:162–168
Fairchild A, Pituskin E, Rose B et al (2009) The rapid access palliative radiotherapy program: blueprint for initiation of a one-stop multidisciplinary bone metastases clinic. Support Care Cancer 17:163–170
Danielson B, Fairchild A (2012) Beyond palliative radiotherapy: a pilot multidisciplinary brain metastases clinic. Support Care Cancer 20:773–781
Bruera E, Kuehn N, Miller MJ, Selmser P, Macmillan K (1991) The Edmonton Symptom Assessment System (ESAS): a simple method for the assessment of palliative care patients. J Palliat Care 7:6–9
Folstein MF, Folstein S, McHugh PR (1975) ‘Mini-mental state’: a practical method for grading the cognitive state of patients for the clinician. J Psychol Res 12:189–198
Scahg CC, Heinrich RL, Ganz PA (1984) Karnofsky performance status revisited: reliability, validity, and guidelines. J Clin Oncol 2:187–193
Anderson F, Downing GM, Hill J, Casorso L, Lerch N (1996) Palliative Performance Scale (PPS): a new tool. J Palliat Care 12:5–11
Fainsinger RL, Nekolaichuk CL (2008) A “TNM” classification system for cancer pain: the Edmonton Classification System for Cancer Pain (ECS-CP). Support Care Cancer 16:547–555
Treasury Board of Canada Secretariat: Travel. Available at http://www.tbs-sct.gc.ca/pubs_pol/hrpubs/tbm_113/menu-travel-voyage-eng.asp. Accessed 21 Feb 2012
Kidd L, Cayless S, Johnston B, Wengstrom Y (2010) Telehealth in palliative care in the UK: a review of the evidence. J Telemed Telecare 16:394–402
Pronovost A, Peng P, Kern R (2009) Telemedicine in the management of chronic pain: a cost analysis study. Can J Anesth 56:590–596
Acknowledgments
The authors would like to acknowledge the invaluable contributions of members of the Virtual Clinic Pilot Project Team, drawn from Alberta Health Services Cancer Care (Cross Cancer Institute and Community Oncology), Seniors Health (North Zone), and Telehealth. This study was funded by Alberta Health and Wellness.
Conflict of interest
There are no conflicts of interest to declare. The authors have full control of all primary data which may be reviewed by the journal if requested.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Watanabe, S.M., Fairchild, A., Pituskin, E. et al. Improving access to specialist multidisciplinary palliative care consultation for rural cancer patients by videoconferencing: report of a pilot project. Support Care Cancer 21, 1201–1207 (2013). https://doi.org/10.1007/s00520-012-1649-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-012-1649-7