Abstract
Background
The intraperitoneal application of surgical mesh remains a controversial issue because of possible complications, especially adhesion and fistula formation. This study aimed to assess the potential of a knitted polytetrafluoroethylene (PTFE) mesh for intraabdominal implantation.
Methods
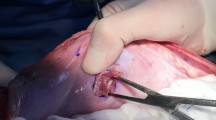
Twenty-eight 5 × 5 cm samples of knitted macroporous PTFE mesh and light-weight polypropylene mesh (LW-PP) were implanted intraperitoneally in 14 New Zealand white rabbits in a randomized manner and fixed using eight polypropylene stitches. After 90 days, the adhesion formation, adhesion score, shrinkage, strength of fixation to the abdominal wall, and histologic biocompatibility were assessed.
Results
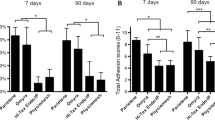
No intraoperative or anesthesia-related complications or mesh infection were recorded. The average area covered by adhesions was 4.7 ± 7.2% for the PTFE and 36.4 ± 36.1% for the LW-PP. The median adhesion score was 0 for the PTFE and 8 for the LW-PP. Shrinkage was 36.9 ± 12.9% for the PTFE mesh and 12.6 ± 8.72% for the LW-PP. The mesh-to-abdominal wall fixation strength was almost the same for both materials (PTFE 3.6 ± 1.9 vs. LW-PP 3.6 ± 2.9). The inflammatory cell count was almost the same for the two groups, with no statistically significant difference. The width of the inner granuloma was equal (PTFE 10.5 ± 0.9 vs. LW-PP 11.1 ± 0.9). The outer granuloma was reduced significantly in the PTFE group (PTFE 23.0 ± 2.1 vs. LW-PP 33.6 ± 7.9). One of the animals in the PTFE group died on postoperative day 12 because of ileus. The reason was an adhesion of the small intestine to the polypropylene fixation stitch, which caused small intestine strangulation.
Conclusions
The knitted PTFE mesh induces fewer intraperitoneal adhesions of lower density than the light-weight polypropylene mesh. The strength of the knitted PTFE mesh fixation to the abdominal wall is comparable with that of the light-weight polypropylene mesh, but the shrinkage is greater. The biocompatibility of the knitted PTFE mesh is comparable with that of the light-weight polypropylene implant.










Similar content being viewed by others
References
Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, de Lange D, Fortelny R, Heikkinen T, Kingsnorth A, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Miserez M (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13:343–403
Korenkov M, Paul A, Sauerland S, Neugebauer E, Arndt M, Chevrel JP, Corcione F, Fingerhut A, Flament JB, Kux M, Matzinger A, Myrvold HE, Rath AM, Simmermacher RK (2001) Classification and surgical treatment of incisional hernia: results of an experts’ meeting. Langenbecks Arch Surg 386:65–73
Leber GE, Garb JL, Alexander AI, Reed WP (1998) Long-term complications associated with prosthetic repair of incisional hernias. Arch Surg 133:378–382
Amid PK (1997) Classification of biomaterials and their related complications in abdominal wall hernia surgery. Hernia 1:15–21
Conze J, Rosch R, Klinge U, Weiss C, Anurov M, Titkowa S, Oettinger A, Schumpelick V (2004) Polypropylene in the intraabdominal position: influence of pore size and surface area. Hernia 8:365–372
Klosterhalfen B, Junge K, Klinge U (2005) The lightweight and large porous mesh concept for hernia repair. Expert Rev Med Devices 2:103–117
Bellón JM, Rodríguez M, García-Honduvilla N, Gómez-Gil V, Pascual G, Buján J (2009) Comparing the behavior of different polypropylene meshes (heavy and lightweight) in an experimental model of ventral hernia repair. J Biomed Mater Res B Appl Biomater 89B:448–455
Cobb WS, Kercher KW, Heniford BT (2005) The argument for lightweight polypropylene mesh in hernia repair. Surg Innov 12:63–69
Cobb WS, Burns JM, Peindl RD, Carbonell AM, Matthews BD, Kercher KW, Heniford BT (2006) Textile analysis of heavy weight, midweight, and lightweight polypropylene mesh in a porcine ventral hernia model. J Surg Res 136:1–7
Harrell AG, Novitsky YW, Cristiano JA, Gersin KS, Norton HJ, Kercher KW, Heniford BT (2007) Prospective histologic evaluation of intraabdominal prosthetics four months after implantation in a rabbit model. Surg Endosc 21:1170–1174
Wassenaar EB, Schoenmaeckers EJ, Raymakers JT, Rakic S (2010) Subsequent abdominal surgery after laparoscopic ventral and incisional hernia repair with an expanded polytetrafluoroethylene mesh: a single-institution experience with 72 reoperations. Hernia 14:137–142
Novitsky YW, Harrell AG, Cristiano JA, Paton BL, Norton HJ, Peindl RD, Kercher KW, Heniford BT (2007) Comparative evaluation of adhesion formation, strength of ingrowth, and textile properties of prosthetic meshes after long-term intraabdominal implantation in a rabbit. J Surg Res 140:6–11
Matthews BD, Mostafa G, Carbonell AM, Joels CS, Kercher KW, Austin C, Norton HJ, Heniford BT (2005) Evaluation of adhesion formation and host tissue response to intraabdominal polytetrafluoroethylene mesh and composite prosthetic mesh. J Surg Res 123:227–234
Foda M, Carlson MA (2009) Enterocutaneous fistula associated with ePTFE mesh: case report and review of the literature. Hernia 13:323–326
Robinson TN, Clarke JH, Schoen J, Walsh MD (2005) Major mesh-related complications following hernia repair: events reported to the Food and Drug Administration. Surg Endosc 19:1556–1560
Iannitti DA, Hope WW, Tsikitis V (2007) Strength of tissue attachment to composite and ePTFE grafts after ventral hernia repair. JSLS 11:415–421
Bellón JM, Jurado F, García-Honduvilla N, López R, Carrera-San Martín A, Buján J (2002) The structure of a biomaterial rather than its chemical composition modulates the repair process at the peritoneal level. Am J Surg 184:154–159
Bellón JM, García-Honduvilla N, Serrano N, Rodríguez M, Pascual G, Buján J (2005) Composite prostheses for the repair of abdominal wall defects: effect of the structure of the adhesion barrier component. Hernia 9:338–343
Bellón JM, Contreras LA, Pascual G, Buján J (2000) Evaluation of the acute scarring response to the implant of different types of biomaterial in the abdominal wall. J Mater Sci Mater Med 11:25–29
Bellón JM, Contreras LA, Pascual G, Bujan J (1999) Neoperitoneal formation after implantation of various biomaterials for the repair of abdominal wall defects in rabbits. Eur J Surg 165:145–150
The Surgical Membrane Study Group (1992) Prophylaxis of pelvic sidewall adhesions with Gore-Tex surgical membrane: a multicenter clinical investigation. Fertil Steril 57:921–923
Binnebösel M, Klink CD, Otto J, Conze J, Jansen PL, Anurov M, Schumpelick V, Junge K (2010) Impact of mesh positioning on foreign body reaction and collagenous ingrowth in a rabbit model of open incisional hernia repair. Hernia 14:71–77
Schug-Pass C, Sommerer F, Tannapfel A, Lippert H, Köckerling F (2009) The use of composite meshes in laparoscopic repair of abdominal wall hernias: are there differences in biocompatibily? Experimental results obtained in a laparoscopic porcine model. Surg Endosc 23:487–495
Bohmer RD, Byrne PD, Maddern GJ (2002) A peeling mesh. Hernia 6:86–87
Schreinemacher MH, Emans PJ, Gijbels MJ, Greve JW, Beets GL, Bouvy ND (2009) Degradation of mesh coatings and intraperitoneal adhesion formation in an experimental model. Br J Surg 96:305–313
Conze J, Junge K, Weiss C, Anurov M, Oettinger A, Klinge U, Schumpelick V (2008) New polymer for intraabdominal meshes–PVDF copolymer. J Biomed Mater Res B Appl Biomater 87:321–328
Fortelny RH, Petter-Puchner AH, Glaser KS, Offner F, Benesch T, Rohr M (2010) Adverse effects of polyvinylidene fluoride-coated polypropylene mesh used for laparoscopic intraperitoneal onlay repair of incisional hernia. Br J Surg 97:1140–1145
Berger D, Bientzle M (2009) Polyvinylidene fluoride: a suitable mesh material for laparoscopic incisional and parastomal hernia repair! A prospective, observational study with 344 patients. Hernia 13:167–172
Anderson JM, Rodriguez A, Chang DT (2008) Foreign body reaction to biomaterials. Semin Immunol 20:86–100
Acknowledgments
This study was funded by Výzkumný ústav pletařský, a.s., Brno, Czech Republic.
Disclosures
Tomáš Novotný, Jiří Jeřábek, Karel Veselý, Robert Staffa, Martin Dvořák, and Jan Cagaš have no conflict of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Novotný, T., Jeřábek, J., Veselý, K. et al. Evaluation of a knitted polytetrafluoroethylene mesh placed intraperitoneally in a New Zealand white rabbit model. Surg Endosc 26, 1884–1891 (2012). https://doi.org/10.1007/s00464-011-2120-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-2120-4