Abstract
Background
Minimally invasive techniques have become an integral part of general surgery, with recent investigation into single-incision laparoscopic cholecystectomy (SILC). This study presents a prospective, randomized, multicenter, single-blind trial of SILC compared with four-port cholecystectomy (4PLC) with the goal of assessing safety, feasibility, and factors predicting outcomes.
Methods
Patients with biliary colic and documented gallstones or polyps or with biliary dyskinesia were randomized to SILC or 4PLC. Data measures included operative details, adverse events, and conversion to 4PLC or laparotomy. Pain, cosmesis, and quality-of-life scores were documented. Patients were followed for 12 months.
Results
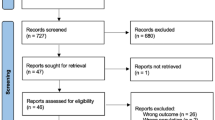
Two hundred patients were randomized to SILC (n = 117) or 4PLC (n = 80) (3 patients chose not to participate after randomization). Patients were similar except for body mass index (BMI), which was lower in the SILC patients (28.9 vs. 31.0, p = 0.011). One SILC patient required conversion to 4PLC. Operative time was longer for SILC (57 vs. 45 min, p < 0.0001), but outcomes, including total adverse events, were similar (34% vs. 38%, p = 0.55). Cosmesis scores favored SILC (p < 0.002), but pain scores were lower for 4PLC (1 point difference in 10-point scale, p < 0.028) despite equal analgesia use. Wound complications were greater after SILC (10% vs. 3%, p = 0.047), but hernia recurrence was equivalent for both procedures (1.3% vs. 3.4%, p = 0.65). Univariate analysis showed female gender, SILC, and younger age to be predictors for increased pain scores, while SILC was associated with improved cosmesis scores.
Conclusions
In this multicenter randomized controlled trial of SILC versus 4PLC, SILC appears to be safe with a similar biliary complication profile. Pain scores and wound complication rates are higher for SILC; however, cosmesis scores favored SILC. For patients preferring a better cosmetic outcome and willing to accept possible increased postoperative pain, SILC offers a safe alternative to the standard 4PLC. Further follow-up is needed to detail the long-term risk of wound morbidities, including hernia recurrence.

Similar content being viewed by others
References
Reynolds W (2001) The first laparoscopic cholecystectomy. JSLS 5(1):89–94
National Institutes of Health Consensus Development Conference (1992) Gallstones and laparoscopic cholecystectomy. NIH Consens Statement 10(3):1–28
Schirmer BD, Edge SB, Dix J, Hyser MJ, Hanks JB, Jones RS (1991) Laparoscopic cholecystectomy. Treatment of choice for symptomatic cholelithiasis. Ann Surg 213:665–676; discussion 677
Soper NJ, Stockmann PT, Dunnegan DL, Ashley SW (1992) Laparoscopic cholecystectomy. The new ‘gold standard’? Arch Surg 127:917–921; discussion 921–923
Johansson M, Thune A, Nelvin L, Stiernstam M, Westman B, Lundell L (2005) Randomized clinical trial of open versus laparoscopic cholecystectomy in the treatment of acute cholecystitis. Br J Surg 92:44–49
Ponsky TA, Diluciano J, Chwals W, Parry R, Boulanger S (2009) Early experience with single port laparoscopic surgery in children. J Laparoendosc Adv Surg Tech A 19(4):551–553
Saber AA, El-Ghazaly TH, Dewoolkar AV (2010) Single-incision laparoscopic bariatric surgery: a comprehensive review. Surg Obes Relat Dis 6(5):575–582
Targarona EM, Balague C, Martinez C, Pallares L, Estalella L, Trias M (2009) Single-port access: a feasible alternative to conventional laparoscopic splenectomy. Surg Innov 16(4):348–352
Chow AG, Purkayastha S, Zacharakis E, Paraskeva P (2011) Single-incision laparoscopic surgery for right hemicolectomy. Arch Surg 146(2):183–186
Navarra G, Pozza E, Occhionorelli S (1997) Short note: one wound laparoscopic cholecystectomy. Br J Surg 84(5):695–697
Podolsky ER, Rottman SJ, Curcillo PG (2009) Single port access (SPA) cholecystectomy: two year follow-up. JSLS 13(4):528–535
Marks J, Tacchino R, Roberts K, Onders R, Denoto G, Paraskeva P, Rivas H, Soper N, Rosemurgy A, Shah S (2011) Prospective randomized controlled trial of traditional laparoscopic cholecystectomy versus single-incision laparoscopic cholecystectomy: report of preliminary data. Am J Surg 201(3):369–373
Chang SK, Tay CW, Bicol RA, Lee YY, Madhavan K (2011) A case-control study of single-incision versus standard laparoscopic cholecystectomy. World J Surg 35(2):289–293
Prasad A, Mukherjee KA, Kaul S, Kaur M (2011) Postoperative pain after cholecystectomy: conventional laparoscopy versus single-incision laparoscopic surgery. J Minim Access Surg 7(1):24–27
Hernandez JM, Morton CA, Ross S, Albrink M, Rosemurgy AS (2009) Laparoendoscopic single site cholecystectomy: the first 100 patients. Am Surg 75(8):681–685
McGregor CG, Sodergren MH, Aslanyan A, Wright VJ, Purkayastha S, Darzi A, Paraskeva P (2011) Evaluating systemic stress response in single port vs. multi-port laparoscopic cholecystectomy. J Gastrointest Surg 15(4):614–622
Love KM, Durham CA, Meara MP, Mays AC, Bower CE (2010) Single-incision laparoscopic cholecystectomy: a cost comparison. Surg Endosc 25(5):1553–1558
Antoniou SA, Pointner R, Granderath FA (2011) Single-incision laparoscopic cholecystectomy: a systematic review. Surg Endosc 25(2):367–377
Phillipp S, Miedema B, Thaler K (2009) Single incision laproscopic cholecystectomy using conventional instruments: early experience in comparison with the gold standard. J Am Coll Surg 209(5):632–637
Chiruvella A, Sarmiento JM, Sweeney JF, Lin E, Davis SS (2010) Iatrogenic combined bile duct and right hepatic artery injury during single incision laparoscopic cholecystectomy. JSLS 14(2):268–271
Acknowledgments
This study was sponsored by Covidien (Mansfield, MA).
Disclosures
Dr. Phillips is a consultant for W. L. Gore & Associates and Cook Biotech. Dr. Marks is a consultant/researcher for Covidien, Olympus, and W. L. Gore & Associates and is on the advisory board for Apollo Endosurgery. Dr. Tacchino is teacher/consultant for Covidien. Dr. DeNoto is a speaker for Olympus and a consultant/speaker for LifeCell, Covidien, and Intuitive. Dr. Rivas works as an educator for Covidien. Dr. Soper is on the advisory board for Transeneterix, Terumo, Endogastric Solutions, and Miret Surgical Inc. and has received educational support from Covidien and Ethicon Endo-Surgery and research support from Karl Storz Endoscopy. Dr. Gecelter is a consultant on the advisory board for Covidien. Drs. Roberts, Onders, Islam, Rubach, Paraskeva, and Shah have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Phillips, M.S., Marks, J.M., Roberts, K. et al. Intermediate results of a prospective randomized controlled trial of traditional four-port laparoscopic cholecystectomy versus single-incision laparoscopic cholecystectomy. Surg Endosc 26, 1296–1303 (2012). https://doi.org/10.1007/s00464-011-2028-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-2028-z