Abstract
Objective
To investigate the feasibility of laparoscopic total mesorectal excision (TME) in mid and lower rectal cancers following neoadjuvant chemoradiation (nCRT).
Background
The laparoscopic approach for colon cancer has been widely accepted. A few studies have shown that there are advantages of laparoscopic over open TME surgery for rectal cancer. However, the role of laparoscopy has not been clearly defined specifically in cases following nCRT.
Methods
All patients with rectal cancer who underwent nCRT were identified; no operations for rectal carcinoma were performed laparoscopically between 1997 and 2005. The laparoscopic cases were matched to open cases based on gender, procedure, age, and body mass index (BMI). The medical records were reviewed and short-term outcome was compared between these two groups. Statistical analysis was performed using SPSS© 15 software.
Results
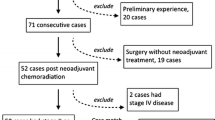
Between 2002 and 2008, 64 patients were identified, including 32 patients who underwent laparoscopic surgery and 32 who had a laparotomy. There was no difference between the two groups based on gender, procedure, age, BMI or American Society of Anesthesiologists (ASA) classification. The procedures performed within each group included 8 abdominoperineal resections and 24 anterior resections, which included 20 colonic J-pouch-anal anastomoses and 4 straight coloanal anastomoses. In the laparoscopic group, 12 patients underwent totally laparoscopic operations, 12 were either laparoscopic-assisted or hand-assisted procedures, and 8 were converted to laparotomy. The reasons for conversion included bleeding, splenic injury, and difficult anatomy. There were no differences in comorbidities, tumor location, tumor size, tumor stage or radiation dose between the two groups. Operative time was longer in the laparoscopic group (267 ± 76 versus 205 ± 49 min, p < 0.001). Operative blood loss, complication rate, and mortality rate were all similar between the two groups. However, the laparoscopic group benefited from shorter length of stay (6.1 ± 2.4 versus 7.6 ± 2.3 days, p = 0.012), earlier first bowel movement (1.9 ± 1 versus 3.3 ± 2.4 days, p = 0.006), and shorter time to regular diet (3.9 ± 2.1 versus 5.8 ± 2.5 days, p = 0.003). There was no difference in lymph node harvest (both positive node harvest and total lymph node harvest), distal margin or radial margin.
Conclusions
In our experience, laparoscopic TME for mid and lower rectal cancer is feasible and safe. Patients benefit from the short-term advantages of laparoscopy, including shorter length of hospital stay, time to tolerating a regular diet, and time to first bowel movement or stoma function. Although there were no short-term differences in oncologic parameters, the long-term oncologic outcome requires further investigation.
Similar content being viewed by others
References
Corman ML (1980) Classic articles in colonic and rectal surgery. A method of performing abdominoperineal excision for carcinoma of the rectum and of the terminal portion of the pelvic colon: by W. Ernest Miles, 1869–1947. Dis Colon Rectum 23:202–205
Heald RJ (1980) Towards fewer colostomies—the impact of circular stapling devices on the surgery of rectal cancer in a district hospital. Br J Surg 67:198–200
Heald RJ, Leicester RJ (1981) The low stapled anastomosis. Dis Colon Rectum 24:437–444
Sugarbaker PH, Corlew S (1982) Influence of surgical techniques on survival in patients with colorectal cancer. Dis Colon Rectum 25:545–557
Heald RJ (1979) A new approach to rectal cancer. Br J Hosp Med 22:277–281
Heald RJ, Husband EM, Ryall RD (1982) The mesorectum in rectal cancer surgery—the clue to pelvic recurrence? Br J Surg 69:613–616
Sauer R, Becker H, Hohenberger W, Rodel C, Wittekind C, Fietkau R et al (2004) Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med 351:1731–1740
Ceelen WP (2007) Use of laparoscopy for rectal cancer: a word of caution. J Clin Oncol 25:5040 (author reply-1)
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM et al (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 365:1718–1726
Clinical Outcomes of Surgical Therapy Study Group (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 350:2050–2059
Fleshman J, Sargent DJ, Green E, Anvari M, Stryker SJ, Beart RW et al (2007) Laparoscopic colectomy for cancer is not inferior to open surgery based on 5-year data from the COST Study Group trial. Ann Surg 246:655–662 (discussion 62–64)
Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ et al (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6:477–484
Marijnen CA, Kapiteijn E, van de Velde CJ, Martijn H, Steup WH, Wiggers T et al (2002) Acute side effects and complications after short-term preoperative radiotherapy combined with total mesorectal excision in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol 20:817–825
Tilney HS, Lovegrove RE, Purkayastha S, Heriot AG, Darzi AW, Tekkis PP (2006) Laparoscopic vs open subtotal colectomy for benign and malignant disease. Colorectal Dis 8:441–450
Tjandra JJ, Chan MK (2006) Systematic review on the short-term outcome of laparoscopic resection for colon and rectosigmoid cancer. Colorectal Dis 8:375–388
Pugliese R, Di Lernia S, Sansonna F, Scandroglio I, Maggioni D, Ferrari GC et al (2008) Results of laparoscopic anterior resection for rectal adenocarcinoma: retrospective analysis of 157 cases. Am J Surg 195:233–238
Bianchi PP, Rosati R, Bona S, Rottoli M, Elmore U, Ceriani C et al (2007) Laparoscopic surgery in rectal cancer: a prospective analysis of patient survival and outcomes. Dis Colon Rectum 50:2047–2053
Hartley JE, Mehigan BJ, Qureshi AE, Duthie GS, Lee PWR, Monson JRT (2001) Total mesorectal excision: assessment of the laparoscopic approach. Dis Colon Rectum 44:315–321. doi:10.1007/BF02234726
Palanivelu C, Sendhilkumar K, Jani K, Rajan PS, Maheshkumar GS, Shetty R et al (2007) Laparoscopic anterior resection and total mesorectal excision for rectal cancer: a prospective nonrandomized study. Int J Colorectal Dis 22:367–372
Liang JT, Lai HS, Lee PH (2007) Laparoscopic pelvic autonomic nerve-preserving surgery for patients with lower rectal cancer after chemoradiation therapy. Ann Surg Oncol 14:1285–1287
Braga M, Frasson M, Vignali A, Zuliani W, Capretti G, Di Carlo V (2007) Laparoscopic resection in rectal cancer patients: outcome and cost-benefit analysis. Dis Colon Rectum 50:464–471
Veenhof AA, Engel AF, Craanen ME, Meijer S, de Lange-de Klerk ES, van der Peet DL et al (2007) Laparoscopic versus open total mesorectal excision: a comparative study on short-term outcomes. A single-institution experience regarding anterior resections and abdominoperineal resections. Dig Surg 24:367–374
Pechlivanides G, Gouvas N, Tsiaoussis J, Tzortzinis A, Tzardi M, Moutafidis M et al (2007) Lymph node clearance after total mesorectal excision for rectal cancer: laparoscopic versus open approach. Dig Dis 25:94–99
Akiyoshi T, Kuroyanagi H, Oya M, Konishi T, Fukuda M, Fujimoto Y et al (2009) Safety of laparoscopic total mesorectal excision for low rectal cancer with preoperative chemoradiation therapy. J Gastrointest Surg 13:521–525
Disclosures
Dr. Wexner is a consultant for and has the right to receive inventor’s share royalties from Power Medical Interventions and from Karl Storz Endoscopy and has received inventors share royalties from Covidien. Dr. Sands received honoraria for speaking for Richard Wolf Medical Instruments Corporation. Drs. Denoya, Wang, Nogueras, and Weiss have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Denoya, P., Wang, H., Sands, D. et al. Short-term outcomes of laparoscopic total mesorectal excision following neoadjuvant chemoradiotherapy. Surg Endosc 24, 933–938 (2010). https://doi.org/10.1007/s00464-009-0702-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-009-0702-1