Abstract
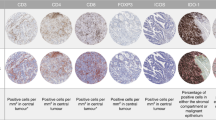
Anti-PD-1 treatment increases anti-tumour immune responses in animal models of hepatocellular carcinoma (HCC). Sorafenib, the mainstay of treatment of HCC patients, however, leads to tumour hypoxia and thereby abrogates the efficacy of anti-PD-1 treatment. This served as a rationale to implement CXCR4 inhibition as adjunct to sorafenib and anti-PD-1 treatment in murine HCC models. We studied the relationship between tumour hypoxia, PD-L1 and CXCL12 expression in human HCC, aiming to test the rationale for triple therapy combining sorafenib, PD-1 immune checkpoint inhibitors and CXCR4 inhibitors. Expression of CXCL12, PD-L1 and of surrogate markers for tumour hypoxia was evaluated at messenger RNA (mRNA) level in a cohort of HCC patients from The Cancer Genome Atlas and immunohistochemically in an independent cohort from the University Hospital of Bonn. Retrospective survival analyses were conducted. CXCL12 mRNA level significantly correlated with markers indicating tumour hypoxia in HCC (HIF1-α ρ = 0.104, p = 0.047). PD-L1 expression was significantly increased in tumours with a high number of tumour-infiltrating lymphocytes (ρ = 0.533, p < 0.001). In Cox proportional hazard analyses, high PD-L1 expression and loss of nuclear CXCL12 expression showed significant prognostic value in terms of overall survival (hazard ratio (HR) = 3.35 [95%CI 1.33–8.46], p = 0.011 for PD-L1; HR = 2.64 [95%CI 1.18–5.88], p = 0.018 for CXCL12, respectively). This study supports the rationale to combine CXCR4 inhibitors and PD-1 immune checkpoint inhibitors in patients with HCC, as sorafenib-induced tumour hypoxia leads to upregulation of PD-L1 and CXCL12.



Similar content being viewed by others
References
Bruix J, Sherman M, American Association for the Study of Liver D (2011) Management of hepatocellular carcinoma: an update. Hepatology 53:1020–1022. doi:10.1002/hep.24199
Chen J, Jiang CC, Jin L, Zhang XD (2016) Regulation of PD-L1: a novel role of pro-survival signalling in cancer. Ann Oncol 27:409–416. doi:10.1093/annonc/mdv615
Chen RX, Song HY, Dong YY, Hu C, Zheng QD, Xue TC, Liu XH, Zhang Y, Chen J, Ren ZG, Liu YK, Cui JF (2014) Dynamic expression patterns of differential proteins during early invasion of hepatocellular carcinoma. PLoS One 9:e88543. doi:10.1371/journal.pone.0088543
Chen Y, Ramjiawan RR, Reiberger T, Ng MR, Hato T, Huang Y, Ochiai H, Kitahara S, Unan EC, Reddy TP, Fan C, Huang P, Bardeesy N, Zhu AX, Jain RK, Duda DG (2015) CXCR4 inhibition in tumor microenvironment facilitates anti-programmed death receptor-1 immunotherapy in sorafenib-treated hepatocellular carcinoma in mice. Hepatology 61:1591–1602. doi:10.1002/hep.27665
Ehling J, Tacke F (2015) Role of chemokine pathways in hepatobiliary cancer. Cancer Lett. doi:10.1016/j.canlet.2015.06.017
Francisco LM, Sage PT, Sharpe AH (2010) The PD-1 pathway in tolerance and autoimmunity. Immunol Rev 236:219–242. doi:10.1111/j.1600-065X.2010.00923.x
Freeman GJ, Long AJ, Iwai Y, Bourque K, Chernova T, Nishimura H, Fitz LJ, Malenkovich N, Okazaki T, Byrne MC, Horton HF, Fouser L, Carter L, Ling V, Bowman MR, Carreno BM, Collins M, Wood CR, Honjo T (2000) Engagement of the PD-1 immunoinhibitory receptor by a novel B7 family member leads to negative regulation of lymphocyte activation. J Exp Med 192:1027–1034
Fujita Y, Yagishita S, Hagiwara K, Yoshioka Y, Kosaka N, Takeshita F, Fujiwara T, Tsuta K, Nokihara H, Tamura T, Asamura H, Kawaishi M, Kuwano K, Ochiya T (2015) The clinical relevance of the miR-197/CKS1B/STAT3-mediated PD-L1 network in chemoresistant non-small-cell lung cancer. Mol Ther 23:717–727. doi:10.1038/mt.2015.10
Gao Q, Wang XY, Qiu SJ, Yamato I, Sho M, Nakajima Y, Zhou J, Li BZ, Shi YH, Xiao YS, Xu Y, Fan J (2009) Overexpression of PD-L1 significantly associates with tumor aggressiveness and postoperative recurrence in human hepatocellular carcinoma. Clin Cancer Res 15:971–979. doi:10.1158/1078-0432.CCR-08-1608
Gevensleben H, Dietrich D, Golletz C, Steiner S, Jung M, Thiesler T, Majores M, Stein J, Uhl B, Mueller S, Ellinger J, Stephan C, Jung K, Brossart P, Kristiansen G (2015) The immune checkpoint regulator PD-L1 is highly expressed in aggressive primary prostate cancer. Clin Cancer Res. doi:10.1158/1078-0432.CCR-15-2042
Ghanem I, Riveiro ME, Paradis V, Faivre S, de Parga PM, Raymond E (2014) Insights on the CXCL12-CXCR4 axis in hepatocellular carcinoma carcinogenesis. Am J Transl Res 6:340–352
Goltz D, Montani M, Braun M, Perner S, Wernert N, Jung K, Dietel M, Stephan C, Kristiansen G (2015) Prognostic relevance of proliferation markers (Ki-67, PHH3) within the cross-relation of ERG translocation and androgen receptor expression in prostate cancer. Pathology 47:629–636. doi:10.1097/PAT.0000000000000320
Hato T, Goyal L, Greten TF, Duda DG, Zhu AX (2014) Immune checkpoint blockade in hepatocellular carcinoma: current progress and future directions. Hepatology 60:1776–1782. doi:10.1002/hep.27246
Hoskin PJ, Sibtain A, Daley FM, Wilson GD (2003) GLUT1 and CAIX as intrinsic markers of hypoxia in bladder cancer: relationship with vascularity and proliferation as predictors of outcome of ARCON. Br J Cancer 89:1290–1297. doi:10.1038/sj.bjc.6601260
Hu F, Miao L, Zhao Y, Xiao YY, Xu Q (2015) A meta-analysis for C-X-C chemokine receptor type 4 as a prognostic marker and potential drug target in hepatocellular carcinoma. Drug Des Devel Ther 9:3625–3633. doi:10.2147/DDDT.S86032
Ishida Y, Agata Y, Shibahara K, Honjo T (1992) Induced expression of PD-1, a novel member of the immunoglobulin gene superfamily, upon programmed cell death. EMBO J 11:3887–3895
Jung HI, Jeong D, Ji S, Ahn TS, Bae SH, Chin S, Chung JC, Kim HC, Lee MS, Baek MJ (2016) Overexpression of PD-L1 and PD-L2 is associated with poor prognosis in patients with hepatocellular carcinoma. Cancer Res Treat. doi:10.4143/crt.2016.066
Kan G, Dong W (2015) The expression of PD-L1 APE1 and P53 in hepatocellular carcinoma and its relationship to clinical pathology. Eur Rev Med Pharmacol Sci 19:3063–3071
Kuang DM, Zhao Q, Peng C, Xu J, Zhang JP, Wu C, Zheng L (2009) Activated monocytes in peritumoral stroma of hepatocellular carcinoma foster immune privilege and disease progression through PD-L1. J Exp Med 206:1327–1337. doi:10.1084/jem.20082173
Liu H, Liu Y, Liu W, Zhang W, Xu J (2015) EZH2-mediated loss of miR-622 determines CXCR4 activation in hepatocellular carcinoma. Nat Commun 6:8494. doi:10.1038/ncomms9494
Liu H, Pan Z, Li A, Fu S, Lei Y, Sun H, Wu M, Zhou W (2008) Roles of chemokine receptor 4 (CXCR4) and chemokine ligand 12 (CXCL12) in metastasis of hepatocellular carcinoma cells. Cell Mol Immunol 5:373–378. doi:10.1038/cmi.2008.46
Loncaster JA, Harris AL, Davidson SE, Logue JP, Hunter RD, Wycoff CC, Pastorek J, Ratcliffe PJ, Stratford IJ, West CM (2001) Carbonic anhydrase (CA IX) expression, a potential new intrinsic marker of hypoxia: correlations with tumor oxygen measurements and prognosis in locally advanced carcinoma of the cervix. Cancer Res 61:6394–6399
Marra F, Bertolani C (2009) Adipokines in liver diseases. Hepatology 50:957–969. doi:10.1002/hep.23046
Marra F, Tacke F (2014) Roles for chemokines in liver disease. Gastroenterology 147:577–594 . doi:10.1053/j.gastro.2014.06.043e571
Muller A, Homey B, Soto H, Ge N, Catron D, Buchanan ME, McClanahan T, Murphy E, Yuan W, Wagner SN, Barrera JL, Mohar A, Verastegui E, Zlotnik A (2001) Involvement of chemokine receptors in breast cancer metastasis. Nature 410:50–56. doi:10.1038/35065016
Nikkhoo B, Jalili A, Fakhari S, Sheikhesmaili F, Fathi F, Rooshani D, Hoseinpour Feizi MA, Nikzaban M (2014) Nuclear pattern of CXCR4 expression is associated with a better overall survival in patients with gastric cancer. J Oncol 2014:808012. doi:10.1155/2014/808012
Noman MZ, Desantis G, Janji B, Hasmim M, Karray S, Dessen P, Bronte V, Chouaib S (2014) PD-L1 is a novel direct target of HIF-1alpha, and its blockade under hypoxia enhanced MDSC-mediated T cell activation. J Exp Med 211:781–790. doi:10.1084/jem.20131916
Quagliata L, Schlageter M, Quintavalle C, Tornillo L, Terracciano LM (2014) Identification of new players in hepatocarcinogenesis: limits and opportunities of using tissue microarray (TMA). Microarrays (Basel) 3:91–102. doi:10.3390/microarrays3020091
Seki E, Schwabe RF (2015) Hepatic inflammation and fibrosis: functional links and key pathways. Hepatology 61:1066–1079. doi:10.1002/hep.27332
Shi F, Shi M, Zeng Z, Qi RZ, Liu ZW, Zhang JY, Yang YP, Tien P, Wang FS (2011) PD-1 and PD-L1 upregulation promotes CD8(+) T-cell apoptosis and postoperative recurrence in hepatocellular carcinoma patients. Int J Cancer 128:887–896. doi:10.1002/ijc.25397
Siegel R, Ma J, Zou Z, Jemal A (2014) Cancer statistics, 2014. CA Cancer J Clin 64:9–29. doi:10.3322/caac.21208
Tamas K, Domanska UM, van Dijk TH, Timmer-Bosscha H, Havenga K, Karrenbeld A, Sluiter WJ, Beukema JC, van Vugt MA, de Vries EG, Hospers GA, Walenkamp AM (2015) CXCR4 and CXCL12 expression in rectal tumors of stage IV patients before and after local radiotherapy and systemic neoadjuvant treatment. Curr Pharm Des 21:2276–2283
Tlsty TD, Coussens LM (2006) Tumor stroma and regulation of cancer development. Annu Rev Pathol 1:119–150. doi:10.1146/annurev.pathol.1.110304.100224
Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, Powderly JD, Carvajal RD, Sosman JA, Atkins MB, Leming PD, Spigel DR, Antonia SJ, Horn L, Drake CG, Pardoll DM, Chen L, Sharfman WH, Anders RA, Taube JM, McMiller TL, Xu H, Korman AJ, Jure-Kunkel M, Agrawal S, McDonald D, Kollia GD, Gupta A, Wigginton JM, Sznol M (2012) Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 366:2443–2454. doi:10.1056/NEJMoa1200690
Topalian SL, Taube JM, Anders RA, Pardoll DM (2016) Mechanism-driven biomarkers to guide immune checkpoint blockade in cancer therapy. Nat Rev Cancer 16:275–287. doi:10.1038/nrc.2016.36
Wendt MK, Cooper AN, Dwinell MB (2008) Epigenetic silencing of CXCL12 increases the metastatic potential of mammary carcinoma cells. Oncogene 27:1461–1471. doi:10.1038/sj.onc.1210751
Wendt MK, Johanesen PA, Kang-Decker N, Binion DG, Shah V, Dwinell MB (2006) Silencing of epithelial CXCL12 expression by DNA hypermethylation promotes colonic carcinoma metastasis. Oncogene 25:4986–4997. doi:10.1038/sj.onc.1209505
Wolchok JD, Kluger H, Callahan MK, Postow MA, Rizvi NA, Lesokhin AM, Segal NH, Ariyan CE, Gordon RA, Reed K, Burke MM, Caldwell A, Kronenberg SA, Agunwamba BU, Zhang X, Lowy I, Inzunza HD, Feely W, Horak CE, Hong Q, Korman AJ, Wigginton JM, Gupta A, Sznol M (2013) Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med 369:122–133. doi:10.1056/NEJMoa1302369
Wong CC, Tse AP, Huang YP, Zhu YT, Chiu DK, Lai RK, Au SL, Kai AK, Lee JM, Wei LL, Tsang FH, Lo RC, Shi J, Zheng YP, Wong CM, Ng IO (2014) Lysyl oxidase-like 2 is critical to tumor microenvironment and metastatic niche formation in hepatocellular carcinoma. Hepatology 60:1645–1658. doi:10.1002/hep.27320
Zeng Z, Shi F, Zhou L, Zhang MN, Chen Y, Chang XJ, Lu YY, Bai WL, Qu JH, Wang CP, Wang H, Lou M, Wang FS, Lv JY, Yang YP (2011) Upregulation of circulating PD-L1/PD-1 is associated with poor post-cryoablation prognosis in patients with HBV-related hepatocellular carcinoma. PLoS One 6:e23621. doi:10.1371/journal.pone.0023621
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study has been approved by the Institutional Review Board (IRB) of the University Hospital of Bonn (No. 167/16). Informed consent has been obtained from all patients that were included in the TCGA cohort in accordance with the Helsinki Declaration of 1975.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Alexander Semaan, Dimo Dietrich, Hans-Peter Fischer and Diane Goltz have equal contribution.
Rights and permissions
About this article
Cite this article
Semaan, A., Dietrich, D., Bergheim, D. et al. CXCL12 expression and PD-L1 expression serve as prognostic biomarkers in HCC and are induced by hypoxia. Virchows Arch 470, 185–196 (2017). https://doi.org/10.1007/s00428-016-2051-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-016-2051-5