Abstract
Purpose
During pancreatoduodenectomy (PD), two techniques have been described to dissect the head of pancreas, viz. the superior mesenteric artery (SMA) approach by dissecting the uncinate process and the uncinate process first approach.
Methods
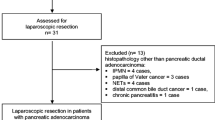
Forty-four consecutive patients, who underwent PD between June 2009 and April 2010, were analyzed. Thirty patients underwent the SMA first approach along with uncinate dissection (group 1), while 14 patients underwent the uncinate process first approach (group 2).
Results
There were 30 male and 14 female patients. The median age was 51 years (range 19–76 years). Median intraoperative blood loss in group 1 was 800 ml, while that in group 2 was 600 ml. A mean of 0.52 units of blood were transfused in group 1 (range 0–3) compared to 0.2 units in group 2 (range 0–1). The median operative time in group 1 was 457.5 min and the median operative time was 450 min in group 2. Complication rate was 40% and 14.3% in groups 1 and 2, respectively. Median duration of hospital stay was 14 days in group 1 and 12.5 days in group 2. Median nodes resected in group 1 were 8 (range 0–26), while in group 2 they were 9 (range 2–14). Resection margins were positive in two cases (one in each group). There were two mortalities in group 1 and no mortalities in group 2. None of the above differences were significant.
Conclusions
SMA first is a safe technique. It compares well with the uncinate first approach in terms of operative time, blood loss, number of lymph nodes retrieved, margin positivity and operative morbidity. Both techniques may be useful in situations such as a large uncinate process tumor or when superior mesenteric vein/portal vein/superior mesenteric artery involvement is suspected or present. Further studies, evaluating data related to specific predefined uncinate tumors, would be the next logical step in further defining the precise role of these techniques.


Similar content being viewed by others
References
Hackert T, Hinz U, Fritz S, Strobel O, Schneider L, Hartwig W, Büchler MW, Werner J. (2011) Enucleation in pancreatic surgery: indications, technique, and outcome compared to standard pancreatic resections. Langenbecks Arch Surg (in press)
Schnelldorfer T, Ware AL, Sarr MG, Smyrk TC, Zhang L, Qin R et al (2008) Long-term survival after pancreatoduodenectomy for pancreatic adenocarcinoma: is cure possible? Ann Surg 247:456–462
Seiler CA, Wagner M, Bachmann T, Redaelli CA, Schmied B, Uhl W et al (2005) Randomized clinical trial of pylorus-preserving duodenopancreatectomy versus classical Whipple resection-long term results. Br J Surg 92:547–556
Wagner M, Redaelli C, Lietz M, Seiler CA, Friess H, Buchler MW (2004) Curative resection is the single most important factor determining outcome in patients with pancreatic adenocarcinoma. Br J Surg 91:586–594. doi:10.1002/bjs.4484
Das K (1912) Carcinom der Papilla duodeni und seine radikale Entfernung. Beitr Klin Chir 78:439–486
Whipple A, Parsons W, Mullins C (1935) Treatment of carcinoma of the ampulla of Vater. Ann Surg 102:763–79. doi:10.1097/00000658-193510000-00023
Traverso LW, Longmire WP Jr (1978) Preservation of the pylorus in pancreaticoduodenectomy. Surg Gynecol Obstet 146:959–962. doi:10.1007/978-3-540-28656-1_44
Pessaux P, Regenet N, Arnaud JP (2003) Resection of the retroportal pancreatic lamina during a cephalic pancreaticoduodenectomy: first dissection of the superior mesenteric artery. Ann Chir 128:633–636
Pessaux P, Varma D, Arnaud JP (2006) Pancreaticoduodenectomy: superior mesenteric artery first approach. J Gastrointest Surg 10:607–611. doi:10.1016/j.gassur.2005.05.001
Popescu I, David L, Dumitra AM, Dorobantu B (2007) The posterior approach in pancreaticoduodenectomy: preliminary results. Hepatogastroenterology 54:921–926
Hackert T, Werner J, Weitz J, Schmidt J, Buchler MW (2010) Uncinate process first—a novel approach for pancreatic head resection. Langenbecks Arch Surg 395(8):1161–1164
Shukla PJ, Barreto G, Pandey D, Kanitkar G, Nadkarni MS, Neve R et al (2007) Modification in the technique of pancreaticoduodenectomy: supracolic division of jejunum to facilitate uncinate process dissection. Hepatogastroenterology 54:1728–1730
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J et al (2005) Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138:8–13
Wente MN, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR et al (2007) Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142:761–768. doi:10.1016/j.surg.2007.05.005
Wente MN, Veit JA, Bassi C, Dervenis C, Fingerhut A, Gouma DJ et al (2007) Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery 142:20–25. doi:10.1016/j.surg.2007.02.001
Barreto G, D'Souza MA, Shukla PJ, Shrikhande SV (2008) The gray zone between postpancreaticoduodenectomy collections and pancreatic fistula. Pancreas 37:422–425. doi:10.1097/MPA.0b013e318175ddd0
Shrikhande SV, Barreto G, Shukla PJ (2008) Pancreatic fistula after pancreaticoduodenectomy: the impact of a standardized technique of pancreaticojejunostomy. Langenbecks Arch Surg 393:87–91. doi:10.1007/s00423-007-0221-2
Welsch T, Eisele H, Zschäbitz S, Hinz U, Büchler MW, Wente MN (2011) Critical appraisal of the International Study Group of Pancreatic Surgery (ISGPS) consensus definition of postoperative hemorrhage after pancreatoduodenectomy. Langenbecks Arch Surg (in press)
Shukla P, Barreto S, Mohandas K, Shrikhande S (2009) Defining the role of surgery for complications after pancreatoduodenectomy. ANZ J Surg 79:33–37. doi:10.1111/j.1445-2197.2008.04794.x
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
D'souza MA, Singh K, Hawaldar RV, Shukla PJ, Shrikhande SV (2010) The vascular stapler in uncinate process division during pancreaticoduodenectomy: technical considerations and results. Dig Surg 27:175–181. doi:10.1159/000264674
Shukla PJ, Barreto SG, Kulkarni A, Nagarajan G, Fingerhut A (2009) Vascular anomalies encountered during pancreatoduodenectomy: do they influence outcomes? Ann Surg Oncol 17:186–193
Leach SD, Davidson BS, Ames FC, Evans DB (1996) Alternative method for exposure of the retropancreatic mesenteric vasculature during total pancreatectomy. J Surg Oncol 61:163–165. doi:10.1002/(SICI)1096-9098(199602)61:2<163::AID-JSO14>3.0.CO;2-A
Machado MC, Penteado S, Cunha JE, Jukemura J, Herman P, Bacchella T et al (2001) Pancreatic head tumors with portal vein involvement: an alternative surgical approach. Hepatogastroenterology 48:1486–1487
Varty PP, Yamamoto H, Farges O, Belghiti J, Sauvanet A (2005) Early retropancreatic dissection during pancreaticoduodenectomy. Am J Surg 189:488–491. doi:10.1016/j.amjsurg.2005.01.007
Weitz J, Kienle P, Schmidt J, Friess H, Buchler MW (2007) Portal vein resection for advanced pancreatic head cancer. J Am Coll Surg 204:712–716. doi:10.1016/j.jamcollsurg.2007.01.004
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shrikhande, S.V., Barreto, S.G., Bodhankar, Y.D. et al. Superior mesenteric artery first combined with uncinate process approach versus uncinate process first approach in pancreatoduodenectomy: a comparative study evaluating perioperative outcomes. Langenbecks Arch Surg 396, 1205–1212 (2011). https://doi.org/10.1007/s00423-011-0824-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-011-0824-5