Abstract
Background
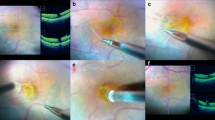
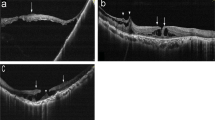
The aim of this study is to present functional and anatomical results of pars plana vitrectomy without gas tamponade in lamellar macular holes. Additionally, the study determines factors influencing final outcome.
Methods
Twenty-six eyes of 26 patients with lamellar macular hole were diagnosed using spectral domain optical coherence tomography (SD- OCT). The diameters of the lamellar defects were measured. Pars plana vitrectomy with epiretinal membrane (ERM) removal and internal limiting membrane (ILM) peeling without endotamponade followed. Follow-up examinations were conducted with SD- OCT for a period of 12 months after surgery. The following factors were examined: maximum and minimum diameter of the lamellar defect, maximum diameter of the disruption of the photoreceptors, representing the photoreceptor layer, central macular thickness, paracentral macular thickness 1000 µm from the centre of the fovea, and maximum paracentral retinal thickness. Retina thickness was measured manually from the inner retina surface to the upper line of retinal pigment epithelium.
Results
Prior to surgery, mean visual acuity was 0.2. Twelve months after surgery, the mean visual acuity was 0.51. Lower visual acuity was observed in patients with photoreceptor layer defects localized under the fovea. Epiretinal membranes and complete or partial posterior hyaloid detachment were observed in all cases. The size of the lamellar defect had no influence on final visual acuity.
Discussion
The results obtained show that intraocular gas tamponade is not a crucial step in achieving closure and visual improvement in lamellar macular holes.





Similar content being viewed by others
References
Gass JD (1975) Lamellar macular hole: a complication of cystoid macular edema after cataract extraction: a clinicopathologic case report. Trans Am Ophthalmol Soc 73:230–250
Witkin AJ, Ko TH, Fujimoto JG, Schuman JS, Baumal CR, Rogers AH, Reichel E, Duker JS (2006) Redefining lamellar holes and the vitreomacular interface: an ultrahigh-resolution optical coherence tomography study. Ophthalmology 113:388–397
Nawrocki J, Michalewska Z (2010) Spectral Domain Optical Coherence Tomography for Macular Holes. In: Holz F, Spaide R (eds.) Medical Retina: Focus on Retinal Imaging. Springer, Heidelberg, pp 141–154
Theodossiadis PG, Grigoropoulos VG, Emfietzoglou I, Nikolaidis P, Vergados I, Apostolopoulos M, Theodossiadis GP (2009) Evolution of lamellar macular hole studied by optical coherence tomography. Graefes Arch Clin Exp Ophthalmol 247:13–20
Hirakawa M, Uemura A, Nakano T, Sakamoto T (2005) Pars plana vitrectomy with gas tamponade for lamellar macular holes. Am J Ophthalmol 140:1154–1155
Kokame GT, Tokuhara KG (2007) Surgical management of inner lamellar macular hole. Ophthalmic Surg Lasers Imaging 38:61–63
Engler C, Schaal KB, Höh AE, Dithmar S (2008) Surgical treatment of lamellar macular hole. Ophthalmologe 105:836–839
Garretson BR, Pollack JS, Ruby AJ, Drenser KA, Williams GA, Sarrafizadeh R (2008) Vitrectomy for a symptomatic lamellar macular hole. Ophthalmology 115:884–886
Wolf-Schnurrbusch UE, Ceklic L, Brinkmann CK, Iliev ME, Frey M, Rothenbuehler SP, Enzmann V, Wolf-Schnurrbusch WS, UE CL, Brinkmann CK, Iliev ME, Frey M, Rothenbuehler SP, Enzmann V, Wolf S (2009) Macular thickness measurements in healthy eyes using six different optical coherence tomography instruments. Invest Ophthalmol Vis Sci 50:3432–3437
Haouchine B, Massin P, Tadayoni R, Erignay A, Gaudric A (2004) Diagnosis of macular pseudoholes and lamellar macular holes by use of optical coherence tomography. Am J Ophthalmol 138:732–739
Sandberg MA, Berson E (1983) Visual acuity and cone spatial density in retinitis pigmentosa. Invest Ophthalmol Vis Sci 24:1511–1513
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have no financial interest in this study. This study was presented at the Annual Meeting of the German Ophthalmological Society (DOG, Leipzig 2009).
Rights and permissions
About this article
Cite this article
Michalewska, Z., Michalewski, J., Odrobina, D. et al. Surgical treatment of lamellar macular holes. Graefes Arch Clin Exp Ophthalmol 248, 1395–1400 (2010). https://doi.org/10.1007/s00417-010-1400-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-010-1400-3