Abstract
Purpose
This review aims to sum up current knowledge on the sensitivity and specificity of ultrasound features suggestive of acute pelvic inflammatory disease (PID).
Methods
A PubMed database search was undertaken, using the MeSH terms “(pelvic inflammatory disease or salpingitis or adnexitis) and ultrasonography”. We included original articles evaluating the performance of vaginal ultrasound in detecting acute PID.
Results
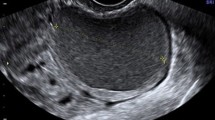
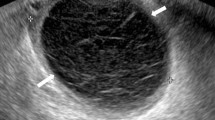
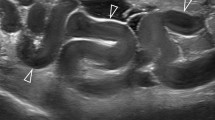
Seven articles were selected, including between 18 and 77 patients each. The golden standard used was laparoscopy/endometrial biopsy in six studies and mostly clinical evaluation in one. “Thick tubal walls” proved to be a specific and sensitive ultrasound sign of acute PID, provided that the walls of the tubes can be evaluated, i.e., when fluid is present in the tubal lumen (100 % sensitivity). The cogwheel sign is also a specific sign of PID (95–99 % specificity), but it seems to be less sensitive (0–86 % sensitivity). Bilateral adnexal masses appearing either as small solid masses or as cystic masses with thick walls and possibly manifesting the cogwheel sign also seems to be a reasonably reliable sign (82 % sensitivity, 83 %specificity). Doppler results overlap too much between women with and without acute PID for them to be useful in the diagnosis of acute PID, even though acutely inflamed tubes are richly vascularized at color Doppler.
Conclusions
Even though the results of our review suggest that transvaginal ultrasound has limited ability to diagnose acute PID, it is likely to be helpful when managing women with symptoms of acute PID, because in some cases the typical ultrasound signs of acute PID can be detected.





Similar content being viewed by others
References
Jacobson L, Westrom L (1969) Objectivized diagnosis of acute pelvic inflammatory disease. Diagnostic and prognostic value of routine laparoscopy. Am J Obstet Gynecol 105(7):1088–1098. doi:0002-9378(69)90132-X
Sellors J, Mahony J, Goldsmith C, Rath D, Mander R, Hunter B, Taylor C, Groves D, Richardson H, Chernesky M (1991) The accuracy of clinical findings and laparoscopy in pelvic inflammatory disease. Am J Obstet Gynecol 164(1 Pt 1):113–120
Centers for Disease Control and Prevention (2010) Sexually transmitted diseases treatment guidelines. MMWR 59(RR-12):63–67
Timor-Tritsch IE, Lerner JP, Monteagudo A, Murphy KE, Heller DS (1998) Transvaginal sonographic markers of tubal inflammatory disease. Ultrasound Obstet Gynecol 12(1):56–66. doi:10.1046/j.1469-0705.1998.12010056.x
Romosan G, Bjartling C, Skoog L, Valentin L (2013) Ultrasound for diagnosing acute salpingitis: a prospective observational diagnostic study. Hum Reprod 28(6):1569–1579. doi:10.1093/humrep/det065
Molander P, Sjoberg J, Paavonen J, Cacciatore B (2001) Transvaginal power Doppler findings in laparoscopically proven acute pelvic inflammatory disease. Ultrasound Obstet Gynecol 17(3):233–238. doi:10.1046/j.1469-0705.2001.00353.x
Patten RM, Vincent LM, Wolner-Hanssen P, Thorpe E Jr (1990) Pelvic inflammatory disease. Endovaginal sonography with laparoscopic correlation. J Ultrasound Med 9(12):681–689
Cacciatore B, Leminen A, Ingman-Friberg S, Ylostalo P, Paavonen J (1992) Transvaginal sonographic findings in ambulatory patients with suspected pelvic inflammatory disease. Obstet Gynecol 80(6):912–916
Tukeva TA, Aronen HJ, Karjalainen PT, Molander P, Paavonen T, Paavonen J (1999) MR imaging in pelvic inflammatory disease: comparison with laparoscopy and US. Radiology 210(1):209–216
Adams J, Polson DW, Franks S (1986) Prevalence of polycystic ovaries in women with anovulation and idiopathic hirsutism. Br Med J (Clin Res Ed) 293(6543):355–359
Boardman LA, Peipert JF, Brody JM, Cooper AS, Sung J (1997) Endovaginal sonography for the diagnosis of upper genital tract infection. Obstet Gynecol 90(1):54–57. doi:10.1016/S0029-7844(97)00241-X
Timmerman D, Valentin L, Bourne TH, Collins WP, Verrelst H, Vergote I (2000) Terms, definitions and measurements to describe the sonographic features of adnexal tumors: a consensus opinion from the International Ovarian Tumor Analysis (IOTA) group. Ultrasound Obstet Gynecol 16(5):500–505. doi:10.1046/j.1469-0705.2000.00287
Grieb G, Steffens G, Pallua N, Bernhagen J, Bucala R (2011) Circulating fibrocytes––biology and mechanisms in wound healing and scar formation. Int Rev Cell Mol Biol 291:1–19. doi:10.1016/B978-0-12-386035-4.00001-X
Ozbay K, Deveci S (2011) Relationships between transvaginal colour Doppler findings, infectious parameters and visual analogue scale scores in patients with mild acute pelvic inflammatory disease. Eur J Obstet Gynecol Reprod Biol 156(1):105–108. doi:10.1016/j.ejogrb.2010.12.030
Alatas C, Aksoy E, Akarsu C, Yakin K, Bahceci M (1996) Hemodynamic assessment in pelvic inflammatory disease by transvaginal color Doppler ultrasonography. Eur J Obstet Gynecol Reprod Biol 70(1):75–78 pii: S0301211596025432
Tepper R, Aviram R, Cohen N, Cohen I, Holtzinger M, Beyth Y (1998) Doppler flow characteristics in patients with pelvic inflammatory disease: responders versus nonresponders to therapy. J Clin Ultrasound 26(5):247–249
Davis JA, Gosink BB (1986) Fluid in the female pelvis: cyclic patterns. J Ultrasound Med 5(2):75–79
Molander P, Cacciatore B, Sjoberg J, Paavonen J (2000) Laparoscopic management of suspected acute pelvic inflammatory disease. J Am Assoc Gynecol Laparosc 7(1):107–110
Acknowledgments
We thank Dr. Povilas Sladkevicius for providing us with ultrasound images.
Conflict of interest
The authors have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Romosan, G., Valentin, L. The sensitivity and specificity of transvaginal ultrasound with regard to acute pelvic inflammatory disease: a review of the literature. Arch Gynecol Obstet 289, 705–714 (2014). https://doi.org/10.1007/s00404-013-3091-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-013-3091-6