Abstract
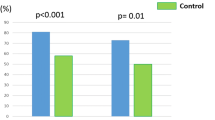
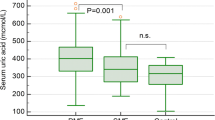
We retrospectively investigated a cohort of 176 myelofibrosis patients (128 primary-PMF; 48 secondary-SMF) from five hematology centers. The presence of chronic kidney disease (CKD) was determined in addition to other clinical characteristics. CKD was present in 26.1% of MF patients and was significantly associated with older age (P < 0.001), higher WBC (P = 0.015), and its subsets (neutrophil, monocyte, and basophil counts), higher platelets (P = 0.001), lower albumin (P = 0.018), higher serum uric acid (P = 0.001), higher LDH (P = 0.022), and the presence of CV risk factors (P = 0.011). There was no significant association with driver mutations, degree of bone marrow fibrosis, PMF/SMF, or DIPSS risk categories (P > 0.05 for all analyses). The presence of CKD was significantly associated with shorter time to arterial (HR = 3.49; P = 0.041) and venous thrombosis (HR = 7.08; P = 0.030) as well as with shorter overall survival (HR 2.08; P = 0.009). In multivariate analyses, CKD (HR = 1.8; P = 0.014) was associated with shorter survival independently of the DIPSS (HR = 2.7; P < 0.001); its effect being more pronounced in lower (HR = 3.56; P = 0.036) than higher DIPSS categories (HR = 2.07; P = 0.023). MF patients with CKD should be candidates for active management aimed at the improvement of renal function. Prospective studies defining the optimal therapeutic approach are highly needed.


Similar content being viewed by others
References
Arber DA, Orazi A, Hasserjian R, Thiele J, Borowitz MJ, Le Beau MM, Bloomfield CD, Cazzola M, Vardiman JW (2016) The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 127(20):2391–2405. https://doi.org/10.1182/blood-2016-03-643544
Hasselbalch HC, Bjørn ME (2015) MPNs as inflammatory diseases: the evidence, consequences, and perspectives. Mediat Inflamm 2015:102476–102416. https://doi.org/10.1155/2015/102476
Hultcrantz M, Kristinsson SY, Andersson TM, Landgren O, Eloranta S, Derolf AR, Dickman PW, Bjorkholm M (2012) Patterns of survival among patients with myeloproliferative neoplasms diagnosed in Sweden from 1973 to 2008: a population-based study. J Clin Oncol 30(24):2995–3001. https://doi.org/10.1200/JCO.2012.42.1925
Passamonti F, Cervantes F, Vannucchi AM, Morra E, Rumi E, Pereira A, Guglielmelli P, Pungolino E, Caramella M, Maffioli M, Pascutto C, Lazzarino M, Cazzola M, Tefferi A (2010) A dynamic prognostic model to predict survival in primary myelofibrosis: a study by the IWG-MRT (International Working Group for Myeloproliferative Neoplasms Research and Treatment). Blood 115(9):1703–1708. https://doi.org/10.1182/blood-2009-09-245837
Passamonti F, Giorgino T, Mora B, Guglielmelli P, Rumi E, Maffioli M, Rambaldi A, Caramella M, Komrokji R, Gotlib J, Kiladjian JJ, Cervantes F, Devos T, Palandri F, De Stefano V, Ruggeri M, Silver RT, Benevolo G, Albano F, Caramazza D, Merli M, Pietra D, Casalone R, Rotunno G, Barbui T, Cazzola M, Vannucchi AM (2017) A clinical-molecular prognostic model to predict survival in patients with post polycythemia vera and post essential thrombocythemia myelofibrosis. Leukemia 31(12):2726–2731. https://doi.org/10.1038/leu.2017.169
Lekovic D, Gotic M, Perunicic-Jovanovic M, Vidovic A, Bogdanovic A, Jankovic G, Cokic V, Milic N (2014) Contribution of comorbidities and grade of bone marrow fibrosis to the prognosis of survival in patients with primary myelofibrosis. Med Oncol 31(3):869. https://doi.org/10.1007/s12032-014-0869-8
Newberry KJ, Naqvi K, Nguyen KT, Cardenas-Turanzas M, Florencia Tanaka M, Pierce S, Verstovsek S (2014) Comorbidities predict worse prognosis in patients with primary myelofibrosis. Cancer 120(19):2996–3002. https://doi.org/10.1002/cncr.28857
Kc D, Falchi L, Verstovsek S (2017) The underappreciated risk of thrombosis and bleeding in patients with myelofibrosis: a review. Ann Hematol 96(10):1595–1604. https://doi.org/10.1007/s00277-017-3099-2
Guglielmelli P, Carobbio A, Rumi E, De Stefano V, Mannelli L, Mannelli F, Rotunno G, Coltro G, Betti S, Cavalloni C, Finazzi MC, Thiele J, Cazzola M, Vannucchi AM, Barbui T (2020) Validation of the IPSET score for thrombosis in patients with prefibrotic myelofibrosis. Blood Cancer J 10(2):21. https://doi.org/10.1038/s41408-020-0289-2
Barbui T, Carobbio A, Cervantes F, Vannucchi AM, Guglielmelli P, Antonioli E, Alvarez-Larran A, Rambaldi A, Finazzi G, Barosi G (2010) Thrombosis in primary myelofibrosis: incidence and risk factors. Blood 115(4):778–782. https://doi.org/10.1182/blood-2009-08-238956
Christensen AS, Moller JB, Hasselbalch HC (2014) Chronic kidney disease in patients with the Philadelphia-negative chronic myeloproliferative neoplasms. Leuk Res 38(4):490–495. https://doi.org/10.1016/j.leukres.2014.01.014
Krečak I, Holik H, Martina MP, Zekanović I, Coha B, Gverić-Krečak V (2020) Chronic kidney disease could be a risk factor for thrombosis in essential thrombocythemia and polycythemia vera. Int J Hematol. https://doi.org/10.1007/s12185-020-02898-7
Said SM, Leung N, Sethi S, Cornell LD, Fidler ME, Grande JP, Herrmann S, Tefferi A, D’Agati VD, Nasr SH (2011) Myeloproliferative neoplasms cause glomerulopathy. Kidney Int 80(7):753–759. https://doi.org/10.1038/ki.2011.147
Alexander MP, Nasr SH, Kurtin PJ, Casey ET, Hernandez LP, Fidler ME, Sethi S, Cornell LD (2015) Renal extramedullary hematopoiesis: interstitial and glomerular pathology. Mod Pathol 28(12):1574–1583. https://doi.org/10.1038/modpathol.2015.117
Strati P, Glass WF, Abdelrahim M, Selamet U, Tchakarov A, Workeneh BT, Verstovsek S, Abudayyeh A (2019) Renal complications of primary myelofibrosis. Leuk Lymphoma 60(2):507–510. https://doi.org/10.1080/10428194.2018.1474525
Fukuda Y, Araki M, Yamamoto K, Morishita S, Inano T, Misawa K, Ochiai T, Edahiro Y, Imai M, Yasuda H, Gotoh A, Ohsaka A, Komatsu N (2019) Evidence for prevention of renal dysfunction associated with primary myelofibrosis by cytoreductive therapy. Haematologica 104(11):e506–e509. https://doi.org/10.3324/haematol.2018.208876
Strati P, Abdelrahim M, Selamet U, Page VD, Pierce SA, Verstovsek S, Abudayyeh A (2019) Ruxolitinib therapy is associated with improved renal function in patients with primary myelofibrosis. Ann Hematol 98(7):1611–1616. https://doi.org/10.1007/s00277-019-03708-9
Barosi G, Mesa RA, Thiele J, Cervantes F, Campbell PJ, Verstovsek S, Dupriez B, Levine RL, Passamonti F, Gotlib J, Reilly JT, Vannucchi AM, Hanson CA, Solberg LA, Orazi A, Tefferi A, International Working Group for Myelofibrosis R, Treatment (2008) Proposed criteria for the diagnosis of post-polycythemia vera and post-essential thrombocythemia myelofibrosis: a consensus statement from the International Working Group for Myelofibrosis Research and Treatment. Leukemia 22(2):437–438. https://doi.org/10.1038/sj.leu.2404914
Thiele J, Kvasnicka HM, Facchetti F, Franco V, van der Walt J, Orazi A (2005) European consensus on grading bone marrow fibrosis and assessment of cellularity. Haematologica 90(8):1128–1132
Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130(6):461–470
Levin A, Stevens PE (2014) Summary of KDIGO 2012 CKD guideline: behind the scenes, need for guidance, and a framework for moving forward. Kidney Int 85(1):49–61. https://doi.org/10.1038/ki.2013.444
Lucijanic M, Skelin M, Lucijanic T (2017) Survival analysis, more than meets the eye. Biochem Med 27(1):14–18
Lucijanic M (2016) Survival analysis in clinical practice: analyze your own data using an Excel workbook. Croat Med J 57(1):77–79. https://doi.org/10.3325/cmj.2016.57.77
Baek SW, Moon JY, Ryu H, Choi YS, Song IC, Lee HJ, Yun HJ, Kim S, Jo DY (2018) Chronic kidney disease in the BCR-ABL1-negative myeloproliferative neoplasm: a single-center retrospective study. Korean J Intern Med 33(4):790–797. https://doi.org/10.3904/kjim.2016.263
Maruyama K, Nakagawa N, Suzuki A, Kabara M, Matsuki M, Shindo M, Iwasaki S, Ogawa Y, Hasebe N (2019) Novel detection of CALR-mutated cells in myeloproliferative neoplasm-related glomerulopathy with interstitial extramedullary hematopoiesis: a case report. Am J Kidney Dis 74(6):844–848. https://doi.org/10.1053/j.ajkd.2019.05.016
Afzali B, Goldsmith DJA (2004) Beneficial effects of statins on the kidney. J Clin Pathol 57(7):673–674. https://doi.org/10.1136/jcp.2003.014282
Orth S, Nowicki M, Wiecek A, Ritz E (1993) Nephroprotective effect of ACE inhibitors. Drugs 46(Suppl 2):189–195; discussion 195-186. https://doi.org/10.2165/00003495-199300462-00029
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All patients provided written informed consent for molecular analyses. The study was approved by the Institutional review boards. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lucijanic, M., Galusic, D., Krecak, I. et al. Reduced renal function strongly affects survival and thrombosis in patients with myelofibrosis. Ann Hematol 99, 2779–2785 (2020). https://doi.org/10.1007/s00277-020-04239-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-020-04239-4