Abstract
Introduction and hypothesis
Vaginal pessaries, pelvic floor exercises and surgery are treatment options for women with symptomatic pelvic organ prolapse (POP). The aim of this study was to compare the outcomes of pessaries and surgery in women with symptomatic POP using the validated International Consultation on Incontinence Questionnaire-Vaginal Symptoms (ICIQ-VS) and Urinary Incontinence (ICIQ-UI) Short Form (SF).
Methods
Women attending the Urogynecology clinics with symptomatic POP were recruited. All women were treated using either a vaginal pessary or surgery. Outcomes were evaluated and then compared at 1 year using the validated ICIQ-VS and ICIQ-UI (SF) questionnaires.
Results
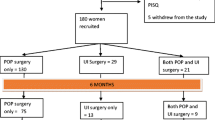
A total of 287 women with symptomatic prolapse were recruited. 269 women completed the questionnaires at baseline and 183 at 1 year. At 1 year, improvement was noted in quality of life (QOL), frequency of urinary leak and vaginal symptoms in both groups except for the symptom of vaginal soreness in the pessary group and the symptom of a tight vagina in the surgery group. However, both these symptoms were not bothersome. Women who underwent surgery demonstrated an improvement in faecal evacuation and sex life. There was an overall statistically significant improvement in vaginal, sex, QOL and urinary symptom scores in both groups. No statistically significant difference was noted between the surgery and the pessary groups.
Conclusions
Using validated questionnaires 1 year after treatment, women with symptomatic POP report improvement in vaginal, bowel, urinary and quality of life scores when treated with either pessary use or surgery. No statistically significant difference was noted in the two groups.


Similar content being viewed by others
References
Hagen S, Stark D, Maher C, Adams E (2005) Conservative management of pelvic organ prolapse in women. Cochrane Database Syst Rev 4:CD003882
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89:501–506
Digesu GA, Chaliha C, Salvatore S, Hutchings A, Khullar V (2005) The relationship of vaginal prolapse severity to symptoms and quality of life. BJOG 112:971–976
Braekken IH, Majida M, Engh ME, Bo K (2010) Can pelvic floor muscle training reverse pelvic organ prolapse and reduce prolapse symptoms? An assessor-blinded, randomized, controlled trial. Am J Obstet Gynecol 203(2):170.e1–170.e7
Wilson PD, Berghmans B, Hagen S, Hay-Smith J, Moore K, Nygaard I et al (2005) Adult conservative management. In: Abrams P, Cardozo L, Khoury S, Wein A (eds) Incontinence, 3rd edn. Health Publications, Plymouth, pp 936–943
Powers K, Lazarou G, Wang A, La Combe J, Besinger G, Greston WM et al (2006) Pessary use in advanced pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 17:160–164
Thakar R, Stanton S (2002) Management of genital prolapse. BMJ 324(7348):1258–1262
Jelovsek JE, Maher C, Barber MD (2007) Pelvic organ prolapse. Lancet 369(9566):1027–1038
Bash KL (2000) Review of vaginal pessaries. Obstet Gynecol Surv 55:455–460
Kapoor DS, Thakar R, Sultan AH, Oliver R (2009) Conservative versus surgical management of prolapse: what dictates patient choice? Int Urogynecol J Pelvic Floor Dysfunct 20(10):1157–1161
Kuhn A, Bapst D, Stadlmayr W, Vits K, Mueller MD (2009) Sexual and organ function in patients with symptomatic prolapse: are pessaries helpful? Fertil Steril 91(5):1914–1918
Fernando RJ, Thakar R, Sultan AH, Shah SM, Jones PW (2006) Effect of vaginal pessaries on symptoms associated with pelvic organ prolapse. Obstet Gynaecol 108(1):93–99
Komesu YM, Rogers RG, Rode MA, Craig EC, Gallegos KA, Montoya AR et al (2007) Pelvic floor symptom changes in pessary users. Am J Obstet Gynecol 197:620e1–620e6
Clemons JL, Aguilar VC, Tillinghast TA, Jackson ND, Myers DL (2004) Patient satisfaction and changes in prolapse and urinary symptoms in women who are fitted successfully with a pessary for pelvic organ prolapse. Am J Obstet Gynecol 190(4):1025–1029
Abdool Z, Thakar R, Sultan AH, Oliver R (2011) Prospective evaluation of outcome of vaginal pessaries versus surgery in women with symptomatic pelvic organ prolapse. Int Urogynecol J 22:273–278
Bradshaw HD, Hiller L, Farkas AG, Radley S, Radley SC (2006) Development and psychometric testing of a symptom index for pelvic organ prolapse. J Obstet Gynaecol 26:241–252
Price N, Jackson SR, Avery K, Brookes ST, Abrams P (2006) Development and psychometric evaluation of the ICIQ Vaginal Symptoms Questionnaire: the ICIQ-VS. BJOG 113(6):700–712
Avery K, Donovan J, Peters T, Shaw C, Gotoh M, Abrams P (2004) ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn 23(4):322–330
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO, Klarskov P et al (1996) The standardization of terminology of female pelvic organ Prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1):10–17
Adams EJ, Thomson AJM, Maher C, Hagen S (2004) Mechanical devices for pelvic organ prolapse in women. Cochrane Database Syst Rev 2:CD004010
Maher C, Baessler K, Glazener CMA, Adams EJ, Hagen S (2007) Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 3:CD004014. doi:10.1002/14651858.CD004014
Lone F, Thakar R, Sultan AH, Karamalis G (2011) A 5-year prospective study of vaginal pessary use for pelvic organ prolapse. Int J Gynecol Obstet 114:56–59
Barber MD, Walters MD, Cundiff GW, PESSRI Trial Group (2006) Responsiveness of the Pelvic Floor Distress Inventory (PFDI) and Pelvic Floor Impact Questionnaire (PFIQ) in women undergoing vaginal surgery and pessary treatment for pelvic organ prolapse. Am J Obstet Gynecol 194(5):1492–1498
Hullfish KL, Bovbjerg VE, Gurka MJ, Steers WD (2008) Surgical versus nonsurgical treatment of women with pelvic floor dysfunction: patient centered goals at 1 year. J Urol 179:2280–2285
Kelleher CJ, Cardozo LD, Khullar V, Salvatore S (1997) King’s Health Questionnaire (KHQ). A new questionnaire to assess the quality of life of urinary incontinent women. Br J Obstet Gynaecol 104:1374–1379
Schaffer J, Cundiff GW, Amundsen CL, Bent A, Coates KW, Strohbehn K et al (2006) Do pessaries improve lower urinary tract symptoms? J Pelvic Med Surg 12:72–73
Moore KN, Dumoulin C, Bradley C, Burgio K, Chambers T, Hagen S, Hunter KF, Imamura M, Thakar R, Williams K (2013) Adult conservative management. In: Abrams PH, Cardozo L, Khoury AE, Wein A (eds) Fifth International Consultation on Incontinence, 5th edn. Health Publications, Plymbridge, pp 1101–1227
Lambrou NC, Buller JL, Thompson JR, Cundiff GW, Chou B, Montz FJ (2000) Prevalence of perioperative complications among women undergoing reconstructive pelvic surgery. Am J Obstet Gynecol 183:1355–1358
Financial disclaimer/conflict of interest
Farah Lone: none; Ranee Thakar: Secretary IUGA, Honorarium and Astellas speaker; Abdul H. Sultan: Pfizer and Astellas speaker.
Authors’ contributions
F. Lone: project development, data collection, data analysis, manuscript writing; R. Thakar: project development, manuscript editing; A.H. Sultan: project development, manuscript editing.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lone, F., Thakar, R. & Sultan, A.H. One-year prospective comparison of vaginal pessaries and surgery for pelvic organ prolapse using the validated ICIQ-VS and ICIQ-UI (SF) questionnaires. Int Urogynecol J 26, 1305–1312 (2015). https://doi.org/10.1007/s00192-015-2686-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2686-9