Abstract
Purpose
To develop and validate the IPREA (Inconforts des Patients de REAnimation) questionnaire for the assessment of discomfort perceived by patients related to their intensive care unit (ICU) stay.
Methods
This was a two step-study comprising a phase of item generation conducted in one ICU and a phase of psychometric evaluation during a multicenter prospective cohort study in 14 ICUs. Patients were unselected consecutive adult surviving ICU patients. On the day of ICU discharge, a nurse asked patients to rate the severity of 16 discomfort sources, from 0 to 100. Ten percent of patients were randomly chosen to be questioned again to assess the reproducibility.
Results
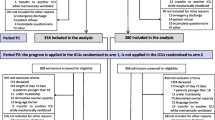
Of 1,380 eligible patients, 1,113 survived and 868 patients could be questioned. The highest scores were for sleep deprivation (35 ± 33), being restrained by tubing, wires, and cables (33 ± 30), pain (32 ± 30), and thirst (32 ± 34). No multidimensional structure was identified. The mean overall score of discomfort was 22 ± 14. Internal consistency was satisfactory using Cronbach’s alpha coefficient (0.78). The test–retest reliability study found average measure intraclass correlations ranging from 0.70 to 0.92. The mean duration of the questionnaire administration was 10 ± 7 min.
Conclusion
The psychometric properties and acceptability of the IPREA questionnaire make it a potential instrument for measuring discomfort perceived by unselected ICU patients.

Similar content being viewed by others
References
Jones C, Griffiths RD, Humphris G, Skirrow PM (2001) Memory, delusions, and the development of acute posttraumatic stress disorder-related symptoms after intensive care. Crit Care Med 29:573–580
Capuzzo M, Valpondi V, Cingolani E, Gianstefani G, De Luca S, Grassi L, Alvisi R (2005) Post-traumatic stress disorder-related symptoms after intensive care. Minerva Anestesiol 71:167–179
Jackson JC, Hart RP, Gordon SM, Hopkins RO, Girard TD, Ely EW (2007) Post-traumatic stress disorder and post-traumatic stress symptoms following critical illness in medical intensive care unit patients: assessing the magnitude of the problem. Crit Care 11:R27
Ballard KS (1981) Identification of environmental stressors for patients in a surgical intensive care unit. Issues Ment Health Nurs 3:89–108
Turner JS, Briggs SJ, Springhorn HE, Potgieter PD (1990) Patients’ recollection of intensive care unit experience. Crit Care Med 18:966–968
Soehren P (1995) Stressors perceived by cardiac surgical patients in the intensive care unit. Am J Crit Care 4:71–76
Novaes MA, Aronovich A, Ferraz MB, Knobel E (1997) Stressors in ICU: patients’ evaluation. Intensive Care Med 23:1282–1285
Simini B (1999) Patients’ perceptions of intensive care. Lancet 354:571–572
Nelson JE, Meier DE, Oei EJ, Nierman DM, Senzel RS, Manfredi PL, Davis SM, Morrison RS (2001) Self-reported symptom experience of critically ill cancer patients receiving intensive care. Crit Care Med 29:277–282
Rotondi AJ, Chelluri L, Sirio C, Mendelsohn A, Schulz R, Belle S, Im K, Donahoe M, Pinsky MR (2002) Patients’ recollections of stressful experiences while receiving prolonged mechanical ventilation in an intensive care unit. Crit Care Med 30:746–752
Parthasarathy S, Tobin MJ (2004) Sleep in the intensive care unit. Intensive Care Med 30:197–206
van de Leur JP, van der Schans CP, Loef BG, Deelman BG, Geertzen JH, Zwaveling JH (2004) Discomfort and factual recollection in intensive care unit patients. Crit Care 8:R467–R473
Granja C, Lopes A, Moreira S, Dias C, Costa-Pereira A, Carneiro A (2005) Patients’ recollections of experiences in the intensive care unit may affect their quality of life. Crit Care 9:R96–R109
Sukantarat KT, Williamson RC, Brett SJ (2007) Psychological assessment of ICU survivors: a comparison between the Hospital Anxiety and Depression scale and the Depression, Anxiety and Stress scale. Anaesthesia 62:239–243
Li D, Puntillo K, Miaskowski C (2008) A review of objective pain measures for use with critical care adult patients unable to self-report. J Pain 9:2–10
Figueroa-Ramos MI, Arroyo-Novoa CM, Lee KA, Padilla G, Puntillo KA (2009) Sleep and delirium in ICU patients: a review of mechanisms and manifestations. Intensive Care Med 35:781–795
Bosma KJ, Ranieri VM (2009) Filtering out the noise: evaluating the impact of noise and sound reduction strategies on sleep quality for ICU patients. Crit Care 13:151
Fung D, Cohen MM (1998) Measuring patient satisfaction with anesthesia care: a review of current methodology. Anesth Analg 87:1089–1098
Juniper EF, Guyatt GH, Jaeschke R (1996) How to develop and validate a new health related quality of life instrument. Lippincott-Raven, Philadelphia
Nunnally JC, Bernstein IH (1994) Statistical foundations. McGraw-Hill, New York
Auquier P, Pernoud N, Bruder N, Simeoni MC, Auffray JP, Colavolpe C, François G, Gouin F, Manelli JC, Martin C, Sapin C, Blache JL (2005) Development and validation of a perioperative satisfaction questionnaire. Anesthesiology 102:1116–1123
Simeoni M, Auquier P, Fernandez O, Flachenecker P, Stecchi S, Constantinescu C, Idiman E, Boyko A, Beiske A, Vollmer T, Triantafyllou N, O’Connor P, Barak Y, Biermann L, Cristiano E, Atweh S, Patrick D, Robitail S, Ammoury N, Beresniak A, Pelletier J, MusiQol study group (2008) Validation of the Multiple Sclerosis International Quality of Life questionnaire. Mult Scler 14:219–230
Simeoni MC, Auquier P, Antoniotti S, Sapin C, San Marco JL (2000) Validation of a French health-related quality of life instrument for adolescents: the VSP-A. Qual Life Res 9:393–403
Cornock MA (1998) Stress and the intensive care patient: perceptions of patients and nurses. J Adv Nurs 27:518–527
Honkus VL (2003) Sleep deprivation in critical care units. Crit Care Nurs Q 26:179–189; 190–191
Bergbom-Engberg I, Haljamae H (1989) Assessment of patients’ experience of discomforts during respirator therapy. Crit Care Med 17:1068–1072
Baker CF (1993) Annoyance to ICU noise: a model of patient discomfort. Crit Care Nurs Q 16:83–90
Bruera E, Kuehn N, Miller MJ, Selmser P, Macmillan K (1991) The Edmonton Symptom Assessment System (ESAS): a simple method for the assessment of palliative care patients. J Palliat Care 7:6–9
Puntillo KA, White C, Morris AB, Perdue ST, Stanik-Hutt J, Thompson CL, Wild LR (2001) Patients’ perceptions and responses to procedural pain: results from Thunder Project II. Am J Crit Care 10:238–251
Revill SI, Robinson JO, Rosen M, Hogg MI (1976) The reliability of a linear analogue for evaluating pain. Anaesthesia 31:1191–1198
Le Gall JR, Lemeshow S, Saulnier F (1993) A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study. JAMA 270:2957–2963
Linacre MJ, Wright BD (1998) A user’s guide to WinSteps, Rasch-model computer programs. MESA Press, Chicago
Wright BD, Stone MH (1979) Best test design: Rasch measurement. MESA Press, Chicago
Angoff WH (1993) Perspectives on differential item functioning methodology. Lawrence Erlbaum, Hillsdale
Ware JE, Harris WJ, Gandek B, Reese PR (1997) MAP-R for Windows: Multitrait/multiitem analysis program-revised user’s guide. Health Assessment Lab, Boston
Leonard KL (2008) Is patient satisfaction sensitive to changes in the quality of care? An exploitation of the Hawthorne effect. J Health Econ 27:444–459
Leonard K, Masatu MC (2006) Outpatient process quality evaluation and the Hawthorne effect. Soc Sci Med 63:2330–2340
Arroyo-Novoa CM, Figueroa-Ramos MI, Puntillo KA, Stanik-Hutt J, Thompson CL, White C, Wild LR (2008) Pain related to tracheal suctioning in awake acutely and critically ill adults: a descriptive study. Intensive Crit Care Nurs 24:20–27
Dudgeon DJ, Harlos M, Clinch JJ (1999) The Edmonton Symptom Assessment Scale (ESAS) as an audit tool. J Palliat Care 15:14–19
Rusinova K, Pochard F, Kentish-Barnes N, Chaize M, Azoulay E (2009) Qualitative research: adding drive and dimension to clinical research. Crit Care Med 37(1 Suppl):S140–S146
Acknowledgments
We thank all members of the nursing staff of each participating ICU for their strong involvement and motivation in the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
On behalf of the Comité Réanimation (Critical Care Committee) de la Société Française d’Anesthésie et de Réanimation.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
Hospital investigators of the IPREA group and trial centers
Phase 1 of item generation: ICU A and Critical Care Medicine Committee of the Société Française d’Anesthésie Réanimation (SFAR)
ICU A: Pierre Kalfon, MD (from October 1996 to December 2002); Hélène Schenk, RN, Virginie Lagueny, RN; Nadine Archambaud, RN, and the whole nursing staff, Frank Thomas, MD; Hervé Clavier, MD and Lilia Soufir, MD, Service de réanimation polyvalente, Hôpital des Diaconesses, Paris.
Comité Réanimation (Critical Care Medicine Committee) of the Société Française d’Anesthésie Réanimation (SFAR) (January 2003): Yannick Mallédant, MD, PhD, Département d’Anesthésie-Réanimation, CHU Pontchaillou, Rennes; Jean Mantz, MD, PhD, Service d’Anesthésie Réanimation, CHU Beaujon, Clichy; Claude Martin, MD, PhD, Département d’Anesthésie-Réanimation, CHU Nord, Marseille; Olivier Mimoz, MD, PhD, Département d’Anesthésie-Réanimation, CHU La Miletrie, Poitiers; Thierry Pottecher, MD, PHD, Service de réanimation polyvalente, CHU Hautepierre, Strasbourg; Benoit Vallet, Clinique d’Anesthésie et de Réanimation, Hôpital Claude Huriez, CHU de Lille; Pierre Courant, MD, Service de réanimation polyvalente, Centre Hospitalier, Avignon; Hervé Dupont, MD, PhD, Service d’Anesthésie-Réanimation, CHU Hôpital Nord, Amiens; Bernard Garrigues, Service de Réanimation médico-chirurgicale, Centre Hospitalier du pays d’Aix, Aix-en-Provence; Rémy Gauzit, MD, Département d’Anesthésie-Réanimation, Unité de Réanimation chirurgicale, CHU Hôtel-Dieu, Assistance Publique-Hôpitaux de Paris; Laurent Jacob, MD, PhD, Département d’Anesthésie-Réanimation, Unité de réanimation chirurgicale, CHU Saint-Louis, Assistance Publique-Hôpitaux de Paris; Jean Laurens, MD, Service de réanimation polyvalente, Polyclinique des Cèdres, Mérignac; Jacques Kienlen, MD, Département d’Anesthésie-Réanimation, Hôpital Gui de Chauliac, CHU de Montpellier; Alain Lepape, MD, Département d’Anesthésie-Réanimation, Unité de Réanimation chirurgicale, CHU de Lyon Sud, Pierre-Bénite; Benoit Weber, MD, PhD, Département d’Anesthésie-Réanimation, Unité de réanimation chirurgicale, CHU Charles Nicolle, Rouen; Nicolas Bruder, MD, PhD, Département d’Anesthésie-Réanimation, Unité de Soins Intensifs Neurochirurgicaux, CHU La Timone, Marseille; Jacques Durand-Gasselin, MD, Service de réanimation polyvalente, Centre Hospitalier Intercommunal Font-Pré, Toulon; Didier Journois, Département d’Anesthésie-Réanimation, Unité de réanimation chirurgicale, Hôpital Européen Georges Pompidou, Assistance Publique-Hôpitaux de Paris; Didier Payen de la Garanderie, Département d’Anesthésie-Réanimation, Unité de réanimation chirurgicale, CHU Lariboisière, Assistance Publique-Hôpitaux de Paris; Jean-François Poussel, Service de réanimation polyvalente, Hôpital Bon Secours, Metz, Pierre Kalfon, Service de réanimation polyvalente, Hôpital des Diaconesses, Paris.
Phase 2 of psychometric validation (ICU 1 to 14)
Yannick Mallédant, MD, PhD, Thomas Signouret, MD, Département d’Anesthésie-Réanimation, CHU Pontchaillou, Rennes; Jean Mantz, MD, PhD, Service d’Anesthésie Réanimation, CHU Beaujon, Clichy; Claude Martin, MD, PhD, Département d’Anesthésie-Réanimation, CHU Nord, Marseille; Olivier Mimoz, MD, PhD, Département d’Anesthésie-Réanimation, Unité de réanimation chirurgicale, CHU La Miletrie, Poitiers; Thierry Pottecher, MD, PHD, Service de réanimation polyvalente, CHU Hautepierre, Strasbourg; Pierre Courant, MD, Service de réanimation polyvalente, Centre Hospitalier, Avignon; Hervé Dupont, MD, PhD, Service d’Anesthésie-Réanimation, CHU Hôpital Nord, Amiens; Patrick Arnodo, MD, Bernard Garrigues, Service de Réanimation médico-chirurgicale, Centre Hospitalier du pays d’Aix, Aix-en-Provence; Rémy Gauzit, MD, Département d’Anesthésie-Réanimation, Unité de Réanimation chirurgicale, CHU Hôtel-Dieu, Assistance Publique-Hôpitaux de Paris; Laurent Jacob, MD, PhD, Département d’Anesthésie-Réanimation, Unité de réanimation chirurgicale, CHU Saint-Louis, Paris; Jean Laurens, MD, Service de réanimation polyvalente, Polyclinique des Cèdres, Mérignac; Alain Lepape, MD, Département d’Anesthésie-Réanimation, Unité de Réanimation chirurgicale, CHU de Lyon Sud, Pierre-Bénite; Jacques Durand-Gasselin, MD, Service de réanimation polyvalente, Centre Hospitalier Intercommunal Font-Pré, Toulon; Annabelle Tessiau, RN, Martine Perdereau, RN, Thomas Sauzeau, RN, Mouldi Hamrouni, MD, Pierre Kalfon, MD (from September 2003), Guy Monchamps, MD, and Abdelkhader Ouchenir, MD, Service de réanimation polyvalente, Hôpitaux de Chartres, Chartres; and the entire nursing staff of each participating center, all in France.
Rights and permissions
About this article
Cite this article
Kalfon, P., Mimoz, O., Auquier, P. et al. Development and validation of a questionnaire for quantitative assessment of perceived discomforts in critically ill patients. Intensive Care Med 36, 1751–1758 (2010). https://doi.org/10.1007/s00134-010-1902-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-010-1902-9